 |
 |
 |
| |
Summary of Antiretroviral Treatment Naïve Studies from CROI:
Still Looking for a Consensus on When to Start
|
| |
| |
Susan J. Little, M.D.
Associate Professor of Medicine
University of California San Diego, USA
Treatment guidelines for much of the developed world recommend that antiretroviral treatment (ART) should be started among asymptomatic individuals with a CD4 cell count of around 350 cells/mm3, although in certain populations, such as those with high plasma viral loads (pVL), HIV-associated nephropathy, HCV or HBV co-infection, pregnancy or breast-feeding, or those with more rapid CD4 cell decline, consideration should be given to earlier initiation of treatment [1-3]. These recommendations are based upon relatively few randomized controlled trials (RCT) [4], but rather multiple observational studies [5, 6]. Several large observational studies were presented at the 16th Conference on Retroviruses and Opportunistic Infections that may further push the pendulum that seems to be swinging with greater force toward earlier initiation of ART among antiretroviral therapy-naïve individuals.
When to Start ART?
Two large observational studies addressed the question of when to start ART among antiretroviral naïve patients. Mari Kitahata (CROI Abst 71) and her colleagues from the North American AIDS Cohort Collaboration on Research and Design (NA-NACCORD) Study performed an analysis as part of a prospective ongoing collaborative study of 22 HIV research cohorts in the United States and Canada established in 2006 [7]. Previous observational data from this group suggested a significant improvement in survival for patients who initiated HAART at CD4 cell counts between 351-500 cells/mm3 rather than defer treatment [5]. The current study from the NA-ACCORD group used observational data designed to mimic that of a clinical trial of asymptomatic HIV-infected individuals with CD4 cell counts of >500 cells/mm3, to evaluate the hypothesis that starting HAART at higher CD4 cell counts improves survival.
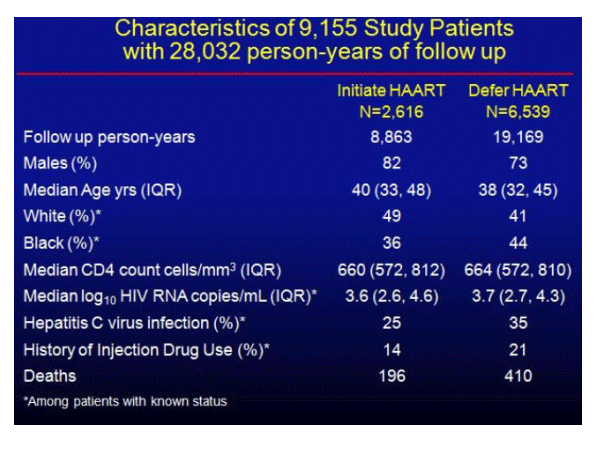
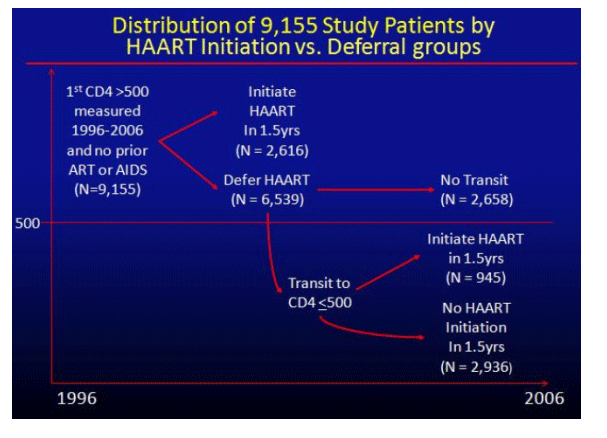
ART naïve patients with CD4 cell counts >500 cells/mm3 in active follow-up between 1996 and 2006 were evaluated (Table 1). Patients with prior ART or AIDS-defining illness were excluded. Participants were randomized to immediate or deferred HAART, beginning at the first CD4 cell count >500 cells/mm3 and using an intention to treat analysis. Patients in the immediate treatment group were required to initiate HAART within 1.5 years of study entry or they were censored and considered protocol "failures". Those in the deferred arm were required to initiate ART within 1.5 years of the time that their CD4 cell count fell below 500 cells/mm3, otherwise, they were similarly considered in violation of the protocol and were censored. The primary study outcome was all-cause mortality.
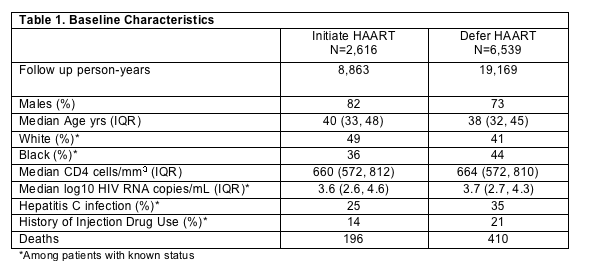
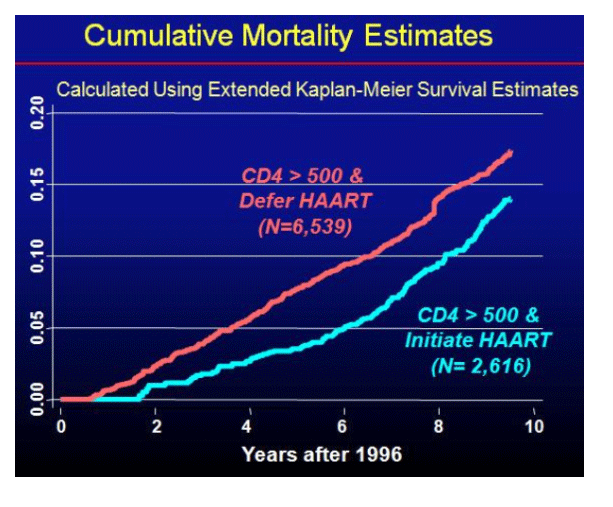
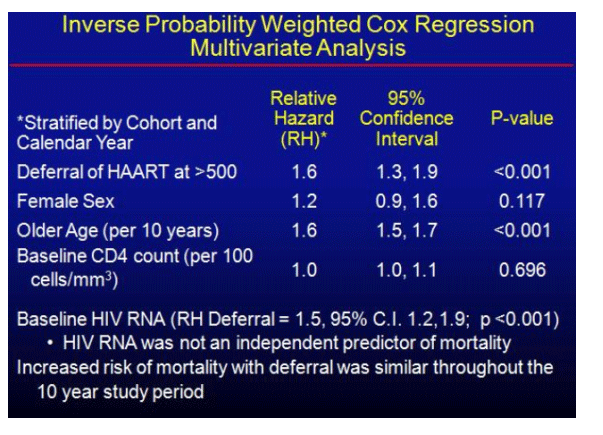
The absolute, all cause mortality for patients who deferred ART was 60% higher and relatively stable for the entire 10 year study period compared to those who initiated immediate ART (p<0.001). In the multivariate analysis, although older age was significantly associated with an increased risk of mortality, gender and baseline CD4 cell count were not associated with an increased risk of mortality. While race did not affect the study outcome, a history of either IDU or HCV infection were independent predictors of mortality. The median CD4 cell count just prior to initiation of ART was 674 for the immediate HAART group and 390 for the deferred HAART group, with a nearly identical viral load response following 12 months of HAART in the immediate and deferred groups (% with VL <500, 79 vs. 73, respectively).
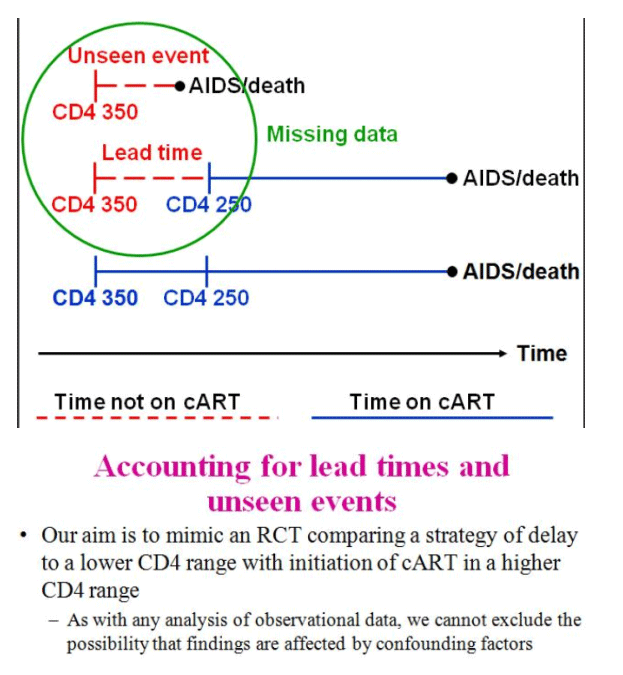
Kitahata and colleagues acknowledge the multiple methodological challenges in analyzing such observational data. By including patients prior to the initiation of HAART, not just at the initiation of HAART, the lead-time during which therapy is deferred is included. Inclusion of this lead-time allows for a direct measurement of AIDS events and deaths that may occur during period of deferred treatment rather than an imputation of such events as is typically performed for observational studies that include patients only at the start of their HAART regimen. The observational design of this study may still be subject to residual confounding due to unmeasured factors that only a large randomized trial can balance. Study investigators attempted to estimate the size of such potential unmeasured confounders and suggested that the effect size of these unmeasured confounders would have to be extremely large to obviate the results of the current study.
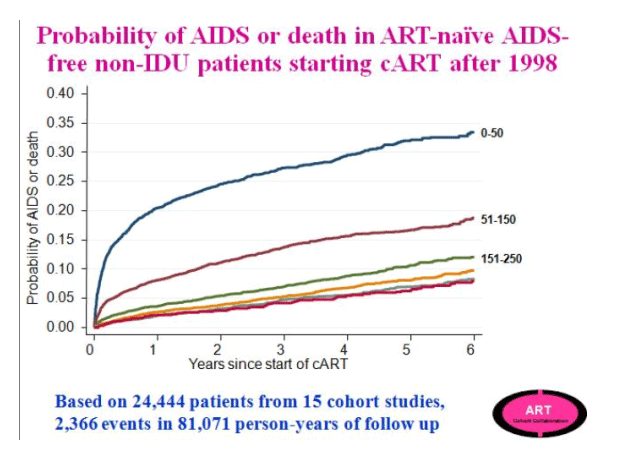
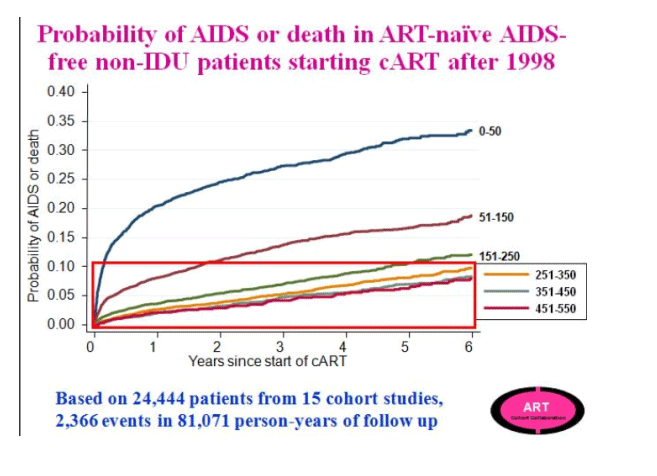
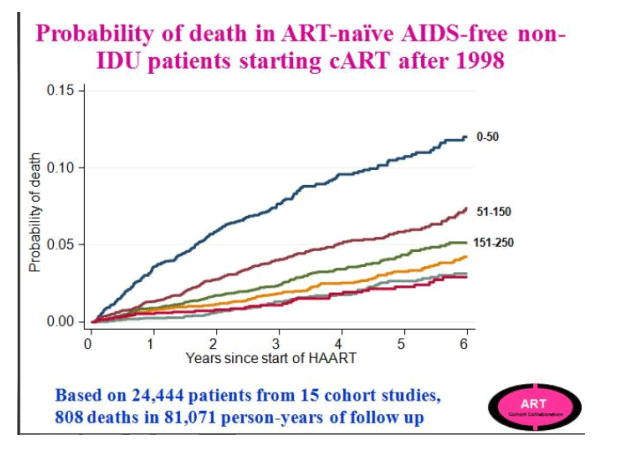
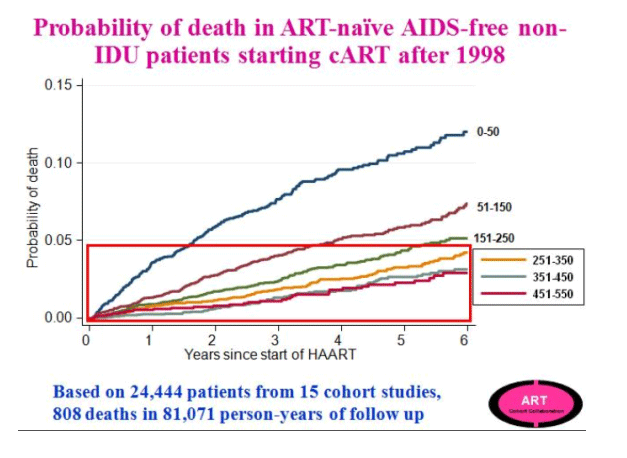
Jonathan Sterne presented a prospective cohort analysis from the Antiretroviral Therapy Cohort Collaboration (ART-CC), a collaboration of 15 HIV cohorts from North America and Europe (CROI 72b). Similar to the NA-ACCORD study, the investigators aimed to mimic a RCT using observational data to compare the strategy of immediate vs. delayed ART among treatment-naïve patients identified after 1998. Analysis of over 24,444 patients starting cART after 1998 from the study cohort demonstrate a graded association with increasing probability of death for patients who initiate combination ART (cART) with lower baseline CD4 cell counts, especially below 200 cells/mm3. A smaller absolute difference in prognosis, however, was observed within the group who started cART with CD4 cell counts greater than 250 cells/mm3. Subjects were categorized as deferred ART or immediate ART and stratified by CD4 at the time of study entry. Thus, unlike the NA-ACCORD analysis, patients in two study arms did not begin the study at comparable CD4 cell counts, but rather the deferred group started at a lower CD4 cell count and statistical methods were used to estimate the number of unseen events (AIDS events and deaths) as well as the variable lead times that are not directly observed in this group such that a direct comparison could be made to the immediate treatment group. To better estimate the missing data, study investigators used data from 7 pre-cART HIV cohorts (1989 - 1995) totaling 21,247 patients and excluding participants whose HIV transmission risk was IDU.
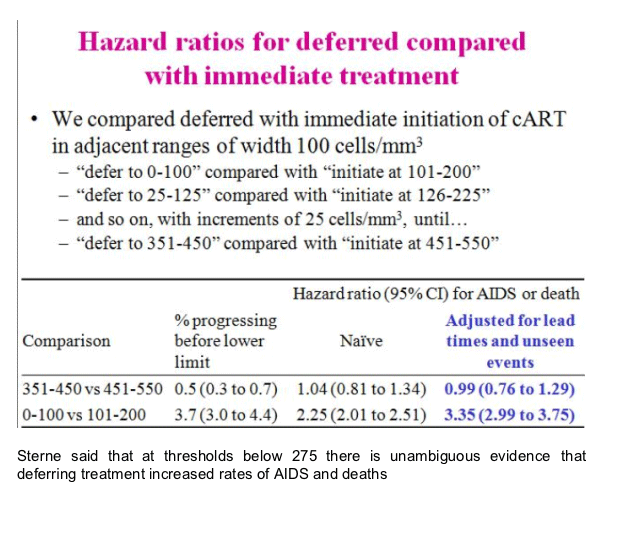
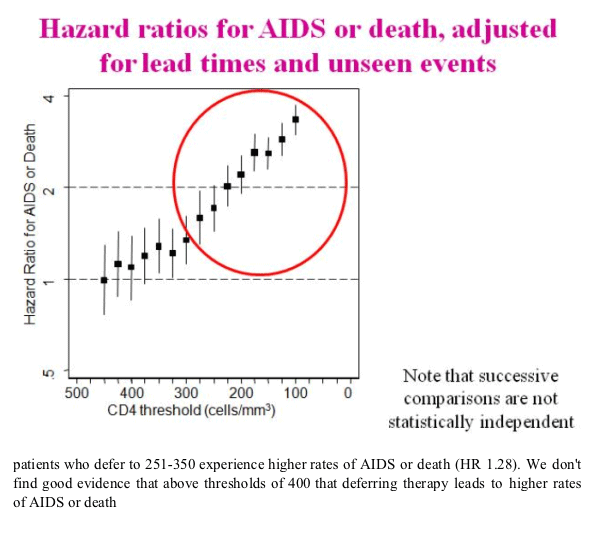
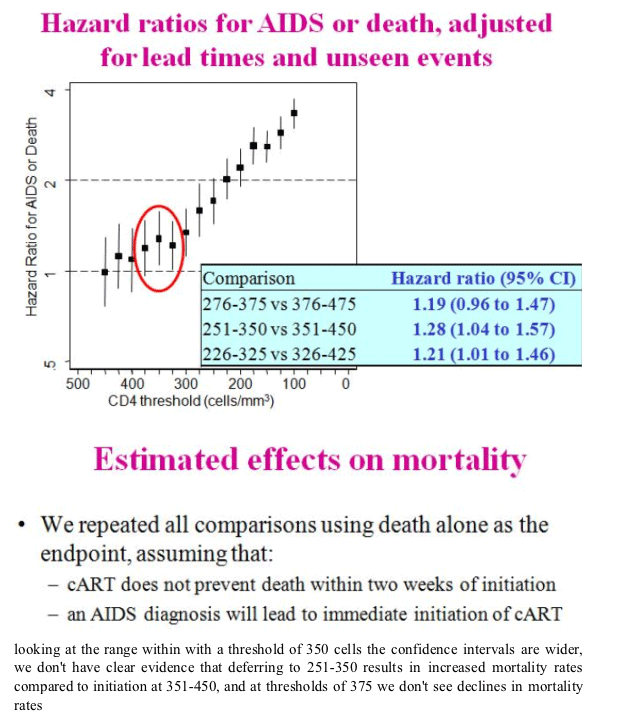
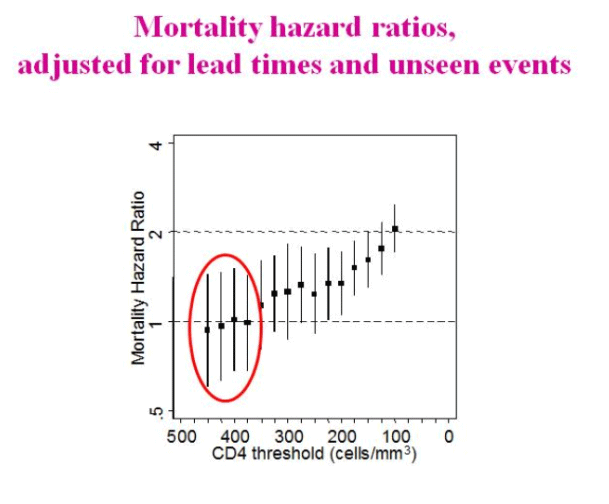
The ART-CC compared the strategy of cART initiated at higher vs. lower CD4 cell count across a range of CD4 counts among ART naïve patients (using the pre-cART data to impute missing data). Delaying treatment to below 350 cells/mm3 was associated with an increased risk of AIDS and death (HR 1.28, 95% CI 1.04 to 1.57), though there was no significant increased risk of mortality alone observed for patients who delayed treatment to a CD4 <350 cells/mm3. At CD4 thresholds >400 cells/mm3, there was not a significantly increased risk of AIDS and death associated with delaying ART. These analyses were restricted to non-IDU, AIDS-free participants, but did not otherwise control for confounding factors and found that adjusting for age, gender, and HIV risk group did not significantly alter the outcome. Investigators were not able to examine the effects of serious non-AIDS events.
An open question period allowed questions to be directed to both of the presenters: 1) Differences between the two studies. While both studies relied upon prospective analyses of observational clinical data, the NA-ACCORD study entered patients into study at the time of their first CD4>500 cells/mm3, thus generally starting the entire cohort from the same CD4 count at entry. The ART-CC study started patients from a HAART era cohort at a specified CD4 and then compared this group to a historical pre-HAART era (pre-cART) cohort at a lower target CD4 range and used the latter group to impute unseen events and estimate lead times for the first group. There were uncertainties about whether such a comparison group for the ART-CC study was likely to result in similar estimates for the missing data as would be directly measured in a HAART-era cohort. 2) Possible confounding - are patients who choose to defer therapy inherently different from those who choose to initiate earlier ART therapy? For instance, could providers elect to defer therapy among those patients they expect to be non-adherent to ART? Kitahata observed that potential unmeasured confounders would have to be associated with both deferral of ART and mortality to be associated with unmeasured confounding and that the effect size of these unmeasured confounders would have to be extremely large to mitigate the results of the NA-ACCORD study. In an effort to address potential differences between the two NA-ACCORD study arms, a comparison of median follow-up and lost to follow-up was performed with comparable results. Further analyses were performed removing all patients with HCV infection and all patients with IDU as a possible transmission risk. Neither sensitivity analysis affected the primary NA-ACCORD study outcome. 3) What were the causes of death associated with the higher cumulative death rate observed in the NA-ACCORD study compared to the ART-CC study? In preliminary analyses, the cause of death for the majority of participants was non-AIDS related death. Further analyses are planned. 4) Given the potential challenges of RCT to definitively resolve the question of when to start ART among treatment naïve patients, should such a study be attempted given the anticipated cost and duration?
From Jules: during the Q&A Doug Richman said this at the microphone: Doug Richman- "I'm really compelled by Mary's data.....the argument that a randomized trial makes any sense bothers me for several reasons, it would take many many years, hundreds of millions of dollars, and wouldn't it make more sense, since most of the patients who present even in the developed world have low CD4 counts, to identify people who need access to care, use all that money and energy to treat people of higher risk"
Current plans are underway to begin the International Network for Strategic Initiatives in Global HIV Trials (INSIGHT) network START trial, a randomized, international multicenter trial that will aim to de-termine whether the immediate initiation of ART in treatment-naïve persons with CD4+ counts >500 cells/mm3 is superior, in terms of morbidity and mortality, to deferral of treatment until the CD4+ count declines to <350 cells/mm3. In its pilot phase, START will enroll 900 participants followed by expansion to include approximately 4,000 participants if the initial phase is successful. The entire study is expected to take about 6 years. Another RCT trial is already underway that will address the issue of when to start ART as a secondary objective, the HPTN 052/ACTG5245 study. While these trials will certainly provide valuable data and potential insights to the relative risks and benefits to earlier treatment, given the multitude of questions in this chronic disease that remain unanswered across the range of HIV disease stages and potential ART start options (secondary transmission risk, acquired resistance, morbidity and mortality risk, etc - from Jules: aging questions), one has to also question whether it might be better to use the large body observational data currently available to structure flexible consensus guidelines that include rationale support for ART for nearly all HIV infected patients. With multiple, more tolerable ART drugs available for use among newly HIV identified individuals, durable virological suppression has become an expectation for the majority of treated patients within populations that have access to pVL monitoring. There will likely always be individuals who are suboptimal candidates for ART at higher CD4 cell counts and in whom treatment should be deferred for a variety of reasons (those who are non-adherent or are at very low risk of disease progression, etc). ART should be fully integrated into the combined prevention-treatment research agenda and as such, studies that assess the secondary transmission risk associated with suboptimal monitoring and earlier initiation of ART should also be considered part of the critical assessment of an optimally delivered ART management program as we consider future directions.
Is Treatment for Primary HIV Infection Beneficial?
Radjin Steingrover presented an evaluation of transient HAART during primary HIV infection (PHI) from the Dutch Primo-SHM Cohort (CROI 70LB). Eligible patients had a negative or indeterminate western blot and detectable plasma HIV RNA or historical documentation of negative HIV screening tests within the past 180 days, now with positive HIV tests. All patients initiated an Efavirenz-based regimen, followed by treatment interruption if pVL was undetectable at time of interruption. "Most" patients with PHI in Dutch treatment centers were offered randomization to either no ART, 24 weeks ART, or 60 weeks ART, though provider and patient preference did dictate assignment to no ART or early HAART in a significant number of patients. A previous study from this group suggested that treatment of PHI had a beneficial effect upon the steady-state viral load [8], thus, the primary study endpoint was duration of time without ART. Following ART interruption, patients were advised to restart ART upon documentation of a CD4 cell count <350 cells/mm3 (verified by repeat documentation), development of symptomatic HIV disease or CDC category B or C events.
A total of 141 patients were identified, 136 were enrolled, and 32 chose to begin early HAART prior to randomization. One hundred and two patients were included in the final analysis, of which only 51 were randomized and 51 received self/provider-selected treatment-assignment. Thus the final analysis of 102 participants included 47 untreated and 55 who received transient HAART. The baseline characteristics of the patients were well matched (Table 2) with baseline CD4 cell counts >500 cells/mm3.
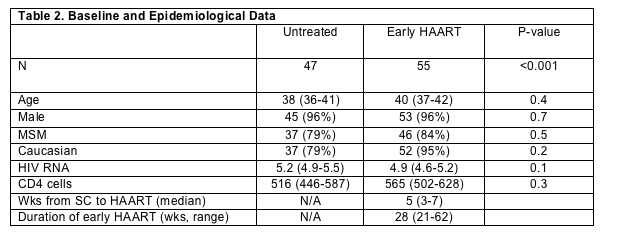
Among the 33 patients who started (n=23) or restarted (n=10) ART, 31 of 33 (94%) did so for low CD4 cell counts with no significant difference in CD4 cell count between the untreated and transient HAART arms at the time of ART initiation.
A corrected Kaplan Meier survival analysis was presented which adjusted the follow-up time in the early-treated patients to correct for the duration of time on early HAART (follow-up time reduced by subtracting the time that patients spent on initial therapy) and demonstrated that after 2 years, approximately 50% of patients in the untreated arm had initiated ART compared to approximately 15% of those who had received transient HAART had restarted ART (p=0.001).
Independent predictors of the time patients remained untreated were age, baseline CD4 cell count, and early HAART. The treated patients gained an average of 60 weeks without treatment by receiving a short course of early HAART (median duration of transient HAART was 28 weeks).
Several limitations to the study were addressed during the question period. 1) The partial randomization structure of the study allowed fully 50% of the study participants to self-select their treatment or lack of treatment assignment. Thus, patients who presented with more severe acute infection syndromes may have selected early HAART and/or patients more likely to be non-adherent may have chosen to defer ART. The potential for confounding in a non-randomized study as previously addressed is significant. Sensitivity analyses were not presented to evaluate factors that might have affected the primary study outcome. Dr. Steingrover did state that while a formal subgroup analysis of the 51 randomized and 51 self/provider-assigned groups was not performed, there did not appear to be any major trend differences in outcome between these two groups. 2) The key question for this study will be whether a short course of ART reduces the total exposure to ART over a defined period of time (3-5 years) rather than simply reducing the time to initiation or re-initiation of HAART. Since any course of HAART will increase the CD4 cell count, it seems predictable that the time to re-initiation of ART in this group after a treatment interruption (now with a new higher CD4 cell count) will be longer than in a comparable group that did not receive HAART and thus has a lower starting CD4 cell count. The alternative question (not answered for this study) is whether a short course of HAART delivered during PHI will effectively reduce the number of individuals receiving ART at year 5 compared to a group of patients who do not receive transient HAART during PHI? Ongoing RCTs are in progress (Primo-SHM, SPARTAC, ACTG), which should help to resolve many of these issues. 3) No resistance evaluations were performed as part of the treatment interruption arm to evaluate the risk of drug resistance after stopping an EFV-based regimen. This is yet another concern, though perhaps more manageable with proper ART stopping protocols, for this patient population without clear indications for ART and a need for vigilant monitoring for adverse outcomes related to ART at this early stage.
Mortality Risk and HAART Use Among Naïve Patients in the Developing World
Stephen Lawn and his colleagues outlined the challenges associated with ART scale up in the developing world including high early mortality (8-26% in the first year of ART[9]), retention, a high burden of tuberculosis, and challenges related to programmatic sustainability of scale-up programs. In follow-up to work evaluating early mortality among nearly 40,000 patients from Gugulethu township in Cape Town, South Africa associated with their National ART service, this group evaluated the question of how mortality risk changes during CD4 cell count recovery during continued ART in the same observational cohort [10]. All patients were treated according to National ART criteria, which included treatment for WHO Stage 4 disease or a CD4<200 cells/mm3 with an NNRTI-based first line regimen. Participants were provided routine CD4 and pVL monitoring every 3 months and co-trimoxazole prophylaxis. Current study results were provided for 2,434 patients (67% women) starting ART between 2002 and 2007 with a median age 33, median CD4 101 cells/mm3, with 23% having WHO Stage 4 and 53% having WHO Stage 3 disease. The median follow-up period of observation was 1.3 years during which 192 deaths occurred during ART.
During the first 12 months, the cumulative mortality during continued ART was 8.5% followed by a continued, but less steep increase in cumulative mortality to 13.2% following a continued duration of ART of 48 months. When stratified by baseline CD4 cell count, patients with a CD4<100 cells/mm3 had nearly twice the mortality at 1 year (11.6% vs. 5.2%) and 4 (16.7% vs. 9.5%) years as patients with a CD4>100 cells/mm3. The magnitude of the 4-year Gugulethu cumulative mortality figures are 3-fold higher for both AIDS-related and non-AIDS related mortality compared to the 5 year cumulative mortality for a non-developing world ART cohort (ATHENA cohort[11]) for similarly stratified patients.
Although rates of pVL suppression (<400) were very high (typically >90% for the entire cohort), and CD4 cell counts rose appropriately, Lawn and colleagues wanted to assess the relationship between CD4 cell count recovery and mortality risk. By categorizing the time of follow-up relative to the quarterly CD4 cell count, they calculated the total person time accrued within different CD4 cell count strata for the whole cohort and used this to evaluate mortality rate (deaths/100 person-years, PYs) stratified by regularly updated CD4 cell counts. Using this approach, mortality rates for patients with CD4<50 cells/mm3 were approximately 38 deaths/100PYs with rates declining sharply thereafter to 5.4 deaths/100PYs for patients with CD4<200 cells/mm3. There appeared to be a relative plateau effect in mortality rates for patients with CD4>200 cells/mm3 to CD4≥500 cells/mm3 with mortality rates ranging from 1.2-2.7 deaths/100PYs. In the multivariate analysis, the updated CD4 cell count was the strongest predictor of mortality with those in the lowest CD4 cell count range (0-49) having a nearly 12 fold higher risk of death (P<0.001) compared to those in the highest CD4 cell range (≥500). The same threshold effect was demonstrated with a significantly increased risk of death for patients wtih a CD4<100 cells/mm3 and a trend for increased risk of death for those with a CD4<200 cells/mm3. These data suggest mortality risk will depend most significantly upon the amount of time spent with persistently low CD4 cell counts while on ART, especially below 200 cells/mm3.
Lawn suggested that by initiating ART at higher CD4 cell counts, one could reduce the amount of time spent in the lower CD4 strata with the highest associated risk of mortality among patients receiving ART. During the question period, Dr. Lawn strongly urged that early diagnosis and treatment was the key to improved patient survival, rather than crisis management of opportunistic infections and their associated morbidity and mortality in patients with more advanced disease, particularly in sites with more limited resources. He further stressed that viral load monitoring was clearly indicated for this patient population, though suggested that while the vast majority of the viral load measures were below the limit of detection, the field would welcome the application of a binary pVL assay platform for more cost effective screening in conjunction with traditional quantitative assays.
Martin Brinkhof (CROI Abs 141) and his colleagues from the ART in Lower Income Countries Collaboration (ART-LINC) of the International epidemiological Databases to Evaluate AIDS (IeDEA) presented an evaluation of mortality among patients receiving their first course of ART and attempted to compare these rates to general population mortality rates in sub-Suharan Africa. The method of standardizing patient mortality relative to the mortality in the general population was expressed as the standardized mortality ratio (SMR) = Observed number of deaths (on ART)/Expected number of deaths (based on age- and gender-specific, HIV-unrelated mortality rate in the general population). Patient data from 5 ART programs in 4 sub-Saharan African countries were evaluated for the present study. A total of 13,249 ART-naïve adult (≥16 yrs) patients (67% women) were evaluated comprising 14,695 PYs of follow-up and including 1,177 deaths in the first 2 years. The median age was 34 years and median baseline CD4 107 cells/mm3, with 85% of participants having advance disease (WHO stage 3 or 4) and an overall cumulative mortality at 2 years of 11.7% (95% CI: 11.1%-12.3%). In order to calculate expected mortality estimates for general population, the investigators collaborated with the World Health Organization (WHO) who provided data from death registries and life table data.
The SMRs for the first 3 months of ART stratified by baseline CD4 demonstrated that the relative mortality was increased by over 500-fold for patients initiating ART with a baseline CD4<25 cells/mm3 and advanced disease (WHO stage 3 or 4) and approximately 200-fold for patients with the same low CD4 but less advanced disease compared to the HIV-unrelated background mortality. Even for patients starting ART with 200 cells/mm3, and less advanced disease, the relative mortality was nearly 30-times that of the HIV-unrelated background mortality during the first 3 months of treatment. SMRs dropped significantly in patients over time on ART, but remained increased for patients with lower baseline CD4 cell counts and more advance disease (Table 3).
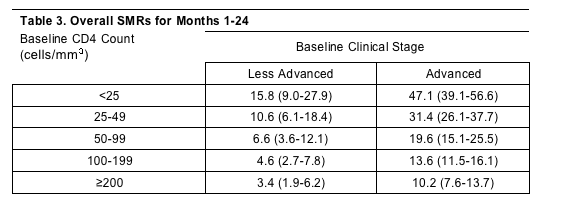
Although the risk of mortality for patients with less advanced clinical disease and the highest strata of baseline CD4 cell count (≥200) approached the mortality risk of the general population (3- to 4-fold higher), less than 10% of the entire cohort actually initiated ART at this stage of disease based upon available National ART guidelines. Dr. Brinkhof reached a similar conclusion to that of Dr. Lawn, that earlier initiation of ART is critical to improving patient outcomes in sub-Saharan Africa.
ART Outcomes Among Treatment-Naïve vs. Treatment-Experienced Women
Kimberly Struble (CROI Abs 987b) and her colleagues from the Food and Drug Administration evaluated datasets from 38 registrational RCTs from 2000-2008 in an effort to assess gender differences in ART efficacy as defined by pVL <400 copies and differences in treatment effect size at week 48. A total of 17,826 patients were evaluated and stratified by treatment history, as treatment naïve (TN, 54%) or treatment experienced (TE, 46%). Efficacy analyses by ARV class were also performed and included 14 ARV drugs. Overall there were no clinically or statistically significant gender differences in the week 48 efficacy outcomes in either TN or TE patient populations, regardless of ART drug class.
References:
1. Guidelines for the use of antiretroviral agents in HIV-1-infected adults and adolescents. In: Services DoHaH, ed. Vol. 2009, 2008:Developed by the DHHS Panel on Antiretroviral Guidelines for Adults and Adolescents - A Working Group of the Office of AIDS Research Advisory Council (OARAC)
2. Clumeck N, Pozniak A and Raffi F. European AIDS Clinical Society (EACS) guidelines for the clinical management and treatment of HIV-infected adults. HIV Med 2008;9:65-71
3. Gazzard BG. British HIV Association Guidelines for the treatment of HIV-1-infected adults with antiretroviral therapy 2008. HIV Med 2008;9:563-608
4. Emery S, Neuhaus JA, Phillips AN, et al. Major clinical outcomes in antiretroviral therapy (ART)-naive participants and in those not receiving ART at baseline in the SMART study. J Infect Dis 2008;197:1133-44
5. Kitahata MM, Gange SJ and Moore RD. Initiating rather than deferring HAART at a CD4+ count between 351-500 cells/mm3 is associated with improved survival. 48th International Conference on Antimicrobial Agents and Chemotherapy (ICAAC). Washington, DC. , 2008
6. May M, Sterne JA, Sabin C, et al. Prognosis of HIV-1-infected patients up to 5 years after initiation of HAART: collaborative analysis of prospective studies. Aids 2007;21:1185-97
7. Gange SJ, Kitahata MM, Saag MS, et al. Cohort profile: the North American AIDS Cohort Collaboration on Research and Design (NA-ACCORD). Int J Epidemiol 2007;36:294-301
8. Steingrover R, Schellens I, Verbon A, et al. Temporary ART during Primary HIV-1 Infection Lowers the Viral Set-point: The Prospective, Randomized Primo-SHM Study. 15th Conference on Retroviruses and Opportunistic Infections. Boston, Massachusetts, 2008
9. Lawn SD, Harries AD, Anglaret X, Myer L and Wood R. Early mortality among adults accessing antiretroviral treatment programmes in sub-Saharan Africa. Aids 2008;22:1897-908
10. Lawn SD, Little F, Bekker LG, et al. Changing mortality risk associated with CD4 cell response to antiretroviral therapy in South Africa. Aids 2009;23:335-42
11. van Sighem AI, van de Wiel MA, Ghani AC, et al. Mortality and progression to AIDS after starting highly active antiretroviral therapy. Aids 2003;17:2227-36
















|
| |
|
 |
 |
|
|