 |
 |
 |
| |
Single Dose Tenofovir Disoproxil Fumarate (TDF) with and without Emtricitabine (FTC) in HIV-1 Infected Pregnant Women and Their Infants: Pharmacokinetics (PK) and Safety
|
| |
| |
Reported by Jules Levin
CROI 2009 Feb 8-12 Montreal
Patricia Flynn*1, Mark Mirochnick2, David Shapiro3, Arlene Bardeguez4, Sharon Huang3, Susan Fiscus5, Koen VanRompay6, James Rooney7, Brian Kearney7, Lynne Mofenson8, Heather Watts8, Patrick Jean-Philippe9, and PACTG 394 Study Team
1St. Jude Children's Research Hosp, Memphis TN USA; 2Boston University School of Medicine, Boston, MA; 3Harvard School Public Health and Statistical Data Analysis Center, Boston, MA USA; 4Univ Medicine Dentistry of NJ, Newark, NJ, USA; 5Univ North Carolina School of Medicine, Chapel Hill, NC USA;
6University of California, Davis CA USA; 7Gilead Sciences, Foster City, CA USA; 8PAMA Branch, NICHD, NIH, Rockville, MD USA; and 9DAIDS, NIAID, NIH, Bethesda, MD
AUTHOR CONCLUSIONS
No significant maternal or infant adverse events were observed with the administration of 900 mg of TFV to HIV-infected pregnant women and 4 mg/kg TDF oral suspension to their infants.
Single dose TDF administration results in CB/M ratios of approximately 65% regardless of maternal dose.
There was a trend to lower AUC (↓38%) and Cmax (↓62%) in women delivering by VD (n=9) compared to CS (n=6) but sample size was small resulting in limited power.
TFV Cmax increased by 83% compared to 600 mg dosing but AUC was similar.
TFV exposures were lower in infants suggesting either altered absorption or more rapid clearance.
Single dose TDF did not result in detection of the K65R mutation in the 8 women who were assessed for resistance. However, the remaining 8 women and all of the infants had undetectable levels of viremia that precluded resistance testing.
ABSTRACT
Background: Tenofovir (TFV) is effective for prevention of SIV transmission in a macaque model and is available as an oral agent (TDF). We conducted a Phase I trial of TDF and TDF/FTC in HIV-infected pregnant women and their infants. PK and safety of 600 mg oral TDF has been reported by this group (CROI, 2006, #708). We now report the PK and safety of 900 mg TDF alone plus 600 mg FTC (given as Truvada) in mothers and 4 mg/kg TDF alone and plus 3 mg/kg FTC administered to their newborns.
Methods: TDF (n=7) or TDF/FTC (n=8) was given during active labor for patients with vaginal delivery (VD) or 4 hrs prior to scheduled C-section (CS). Infants received the same regimen as their mothers and were dosed as soon as possible after birth. All women received HAART during pregnancy and women and infants received the ACTG 076 zidovudine regimen peripartum. Maternal (M) blood samples at 7 intervals over 24 hrs post-dosing, a cord blood (CB) sample, and infant (IN) samples at 5 intervals over 36 hrs post-dosing were obtained and assayed for TFV by LC/MS-MS. FTC PK is pending.
Results: TDF and TDF/FTC were safe and well tolerated in 15 mothers and
16 infants. Among the mothers, median (range) age and HIV-RNA viral load at entry were 26 years (19-37) and 1.53 log10 copies/mL (0.95-3.17). Median (range) time from TDF dose to delivery was 7 hr (1.5-21) and from birth to TDF dose in infants was 5.5 hr (1.8-11). PK findings from the TDF and TDF/FTC groups were similar and combined; median and ranges are presented in the table.

M TFV at delivery was 108.5 ng/mL (n=15, 0-381) and CB TFV was 68.3 ng/mL (n=15, 0-224.2). CB TFV exceeded the target of 50 ng/mL in 10 of 15. CB/M was 66.5% (n=14). Women delivering by VD (n=9) had lower AUC (↓38%) and Cmax (↓62%) compared to CS (n=6) but these differences were not statistically significant. TFV Cmax increased by 83% compared to 600 mg dosing but AUC was similar. No infant was HIV infected and no mother demonstrated a new K65R resistance mutation by week 12.
Conclusions: TDF is safe and demonstrated an acceptable absorption profile. M TFV AUC and TFV placental transfer is sufficient to achieve CB concentrations with antiretroviral activity. TFV exposures were lower in infants suggesting either altered absorption or more rapid clearance. The appropriate dosing schedule in infants to maintain effective concentrations over the first days of life remains to be determined.
STUDY AIM
To evaluate the pharmacokinetics, safety, and tolerance of a single dose of oral tenofovir disoproxil fumarate (TDF) alone and in combination with single dose emtricitabine in HIV-1 infected pregnant women and their infants, when administered at the onset of active labor or prior to delivery by elective C-section.
BACKGROUND
A two dose nevirapine (NVP) regimen is currently the standard for PMTC in resource limited settings but there are concerns about development of resistance.
Tenofovir (TFV) has demonstrated significant prophylactic efficacy against Simian Immunodeficiency Virus (SIV) infection in macaques in multiple studies including a perinatal transmission model.
In cohort 1, HIV-infected pregnant women received a single dose of TDF of 600 mg orally during labor or prior to elective C-section to the mother and no drug dosing for the infant (CROI, 2006, #708) with the following findings.
- Median TFV cord blood concentration was 76 ng/ml, consistent with values expected to provide antiretroviral activity.
- At 12 hours of age, no infant had a TFV concentration above the lower limit of detection for the assay
To more consistently achieve TFV concentrations likely to be effective in preventing maternal to child HIV-1 transmission in cord blood and in the infants, we opened cohort 2 to study the safety, tolerance and pharmacokinetics of a single dose of 900 mg TDF.
PACTG 394 was amended during enrollment into cohort 2 to add emtricitabine (FTC) using co-formulated Truvada.
METHODS
Population:
· HIV-infected pregnant women greater than or equal to 34 weeks gestation.
· Any maternal background ART regimen, excluding those containing TFV, was allowed.
· Women with serious underlying medical condition or obstetrical complication, chronic diarrhea, or creatinine clearance less than 70 mL/min/1.73 m2 were excluded.
· Maternal and infant prophylaxis for prevention of maternal to child transmission was given consistent with current PHS perinatal guidelines.
Drug Administration: HIV-infected pregnant women received a single maternal dose of TDF, 900mg alone (3 TDF tablets), or coformulated with FTC, 600 mg (3 Truvada tablets), during active labor or 4 hours prior to a scheduled C-section. Infants received 4 mg/kg TDF suspension alone or with 3 mg/kg FTC suspension, orally as soon as possible after birth. All women received additional ARVs and all infants received zidovudine for prophylaxis of perinatal prevention.
Pharmacokinetic Design:
Maternal: Blood samples predose, 1, 2, 4, 8, 12, and 24 hours post dose and at the time of delivery.
Cord Blood: A minimum of 5 ml of cord blood obtained at delivery.
Infant: Blood samples predose, 4, 12, 24, and 36 hours post dose.
Assay: Tenofovir measured by LC/MS (LOQ=25 ng/ml).
Data Analysis: AUC determined using trapezoidal rule. Estimates of maternal tenofovir plasma concentration at the time of delivery and measured cord blood concentrations of tenofovir were used to determine a cord blood/maternal tenofovir ratio as a measure of placental transfer. Unpaired t-test was used for comparison of pharmacokinetic parameters by group.
RESULTS
Eighteen mother-infant pairs were enrolled; 9 pairs in the TDF alone group and 9 in the combination TDF/FTC group. The demographics and PK characteristics of the women and their infants in these two groups were similar and are combined. Safety criteria are presented by study group. Sixteen women and their infants received study agents and provided safety data; 15 women and 16 infants had evaluable pharmacokinetic information as determined by pre-established study criteria. Two mothers and their infants did not receive study drug: one mother received study drug and was in false labor; and one infant in the TDF/FTC group only received TDF.
Patient Demographics:
Mothers (n=15)
· Race:
- Black: 9 (60%)
- Hispanic: 4 (27%)
- White 2 (13%)
· Median age: 26 years (range, 19-37)
· Undetectable viral load (< 50 copies/mL) at entry: 10 (67%)
· Undetectable viral load (< 50 copies/mL) at delivery: 14 (93%)
· Median maternal weight: 84.9 kg (range, 66.6-111.4)
· Background ART:
- 2 NRTIs + PI: 13 (87%)
- NRTIs only: 2 (13%)
· Median time from dose to delivery in mothers: 6:58 hrs (range, 1.3-21)
Infants (n=16)
· Mode of Delivery: 9 spontaneous vaginal and 7 Cesarean section (1 specifically to interrupt HIV transmission)
· Median birthweight: 3.32 kg (range, 2.81-4.06)
· Median gestational age: 39.5 weeks (range, 37-42)
· Median Apgar at 5 minutes: 9 (range, 8-10)
· Median time from birth to dose in infants: 5:30 hr (1:5-11:02)
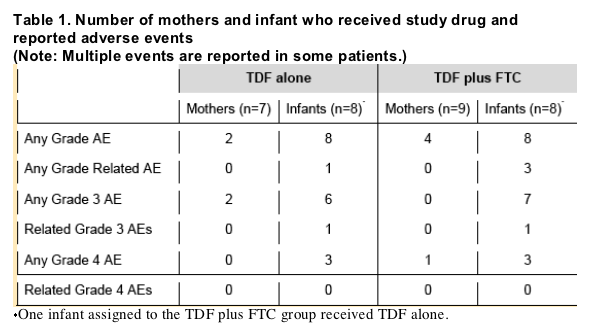
Safety and Tolerance:
Both mothers and infants tolerated study drug well.
Among women all events were low glucose values and none were thought related to study agents (Table 1).
Adverse events were common in infants and consisted mainly of laboratory abnormalities considered unrelated to study agents (Table 1).
Eight grade 4 events occurred in 6 infants and included 5 increased potassium values that were likely related to obtaining blood; 1 decreased hemoglobin; 1 decreased glucose; and 1 increased calcium value. There were no grade 4 events thought related to study agents.
Eight grade 3 events occurred in 5 infants receiving TDF including 3 decreased hemoglobin; 2 decreased glucose; 2 decreased ANC; and 1 elevated CPK. Of these, one Grade 3 hemoglobin value was thought to be possibly treatment related.
There were 12 Grade 3 events in 8 infants who received TDF/FTC, including 2 decreased ANC events; 3 elevated potassium; 3 decreased hemoglobin; 1 decreased glucose; 1 decreased platelet; and 2 elevated bilirubin. Of these, only one patient with a Grade 3 hemoglobin value was thought to be possibly treatment related.
No infant developed HIV infection.
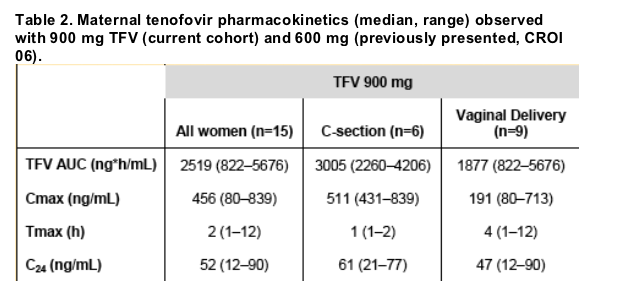
Maternal Tenofovir Pharmacokinetics:
Maternal TFV pharmacokinetic parameters are presented below. Data is shown for all evaluable participants and separately for women delivering via spontaneous vaginal delivery (n=9) and C-section (n=6). AUC was greatest in women delivering by C-section but this difference was not statistically significant (p=0.7, 95%CI: -1016.6 to 2001.6).
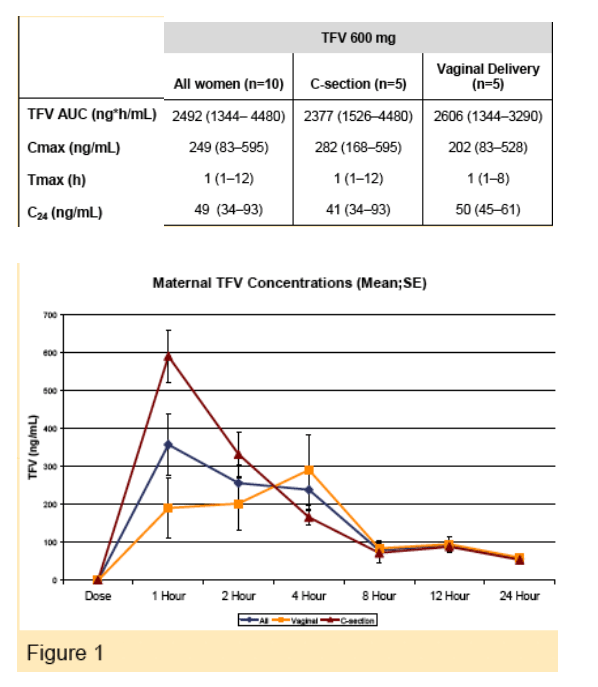
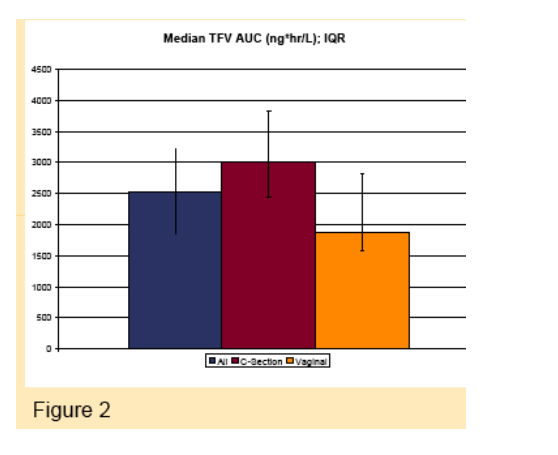
Cord Blood Tenofovir Pharmacokinetics:
The median TFV concentration was 68.3 ng/mL (range, 0-224.2, n=15) . Five values fell below the targeted concentration of 50 ng/mL (0, 15.8, 33.2, 45.8 48.7). Neither time between maternal dose and delivery nor maternal weight was different between the groups with cord blood concentrations above vs. below 50 ng.mL (p=0.6, 95%CI: -4.8-2.8 and p=0.6, 95%CI: -12.3-20.6).
Maternal TFV concentrations from within 1 hour of delivery were available for 13 of the 15 infants with cord blood samples. After excluding the infant with no detectable TFV in cord blood and his mother who also had no detectable TFV at the time of delivery, the median cord blood to maternal ratio was 66.5% (range, 25.6-83.5%). This value was similar to that obtained in the 600 mg TDF group previously reported (65%, range 35-100%).
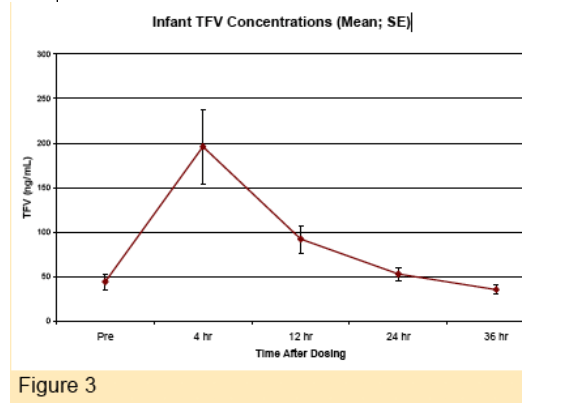
Infant Tenofovir Pharmacokinetics:
Infant TFV pharmacokinetics are shown below. At the time of TDF dosing, the mean TFV concentration in the infant was 44 ng/mL, below the targeted minimum concentration for infants of 50 ng/mL but substantial interpatient variability was observed. Cmax was observed in 15 of the 16 infants at the 4 hour time point (one infant had Cmax at 12 hr). By 24 hours after dosing, the mean concentration was approximately 50 ng/mL.
TVF Resistance:
Maternal specimens for viral load were collected at labor and delivery, 24-48 hours post delivery and weeks 1, 6-8, and 12 weeks post delivery and assayed using the Roche Ultrasensitive test kit. Twelve viral samples from 8 women obtained post TDF dosing demonstrated viral load values greater than 1,000 viral copies/mL and had high sensitivity resistance testing performed. None of these 8 women demonstrated a new K65R mutation through 12 weeks of the study. The remaining women did not have sufficient virus present to assess the development of resistance.
Acknowledgements
We thank the many families that agreed to participate in this study. Overall support for the International Maternal Pediatric Adolescent
AIDS Clinical Trials Group IMPAACT) was provided by the National Institute of Allergy and Infectious Diseases [U01 AI068632] and by the Eunice Kennedy Shriver National Institute of Child Health and Human Development [HHSN267200800001C]. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institute of Allergy and Infectious Diseases or the National Institutes of Health. This work was supported by the Statistical and Data Analysis Center at Harvard School of
Public Health, under the National Institute of Allergy and Infectious Diseases cooperative agreement #5 U01 AI41110 with the Pediatric AIDS Clinical Trials Group (PACTG) and #1 U01 AI068616 with the IMPAACT Group.
|
| |
|
 |
 |
|
|