 |
 |
 |
| |
Tipranavir & Darunavir, Prevalences of mutations in patients with discordant phenotypic resistance from Monogram Biosciences database of routine clinical samples from 2006 - 2008
|
| |
| |
Richard Bethell1, Joseph Scherer2, Myriam Witvrouw1, Agnes Paquet3, Eoin Coakley3, David Hall4
1Boehringer Ingelheim (Canada) Ltd, Quebec, Canada; 2Boehringer Ingelheim Germany, Ingelheim, Germany; 3Monogram Biosciences, California, USA; 4Boehringer Ingelheim Pharmaceuticals, Connecticut, USA

ABSTRACT
Background: Current guidelines recommend that resistance testing should be performed when considering a change to the treatment regimens of protease experienced patients. To explore their available options, the database of clinical isolates at Monogram Biosciences with Phenosense GT results, both genotypic and phenotypic test results, was queried for the years 2006-2008.
Phenotypic GT results were analyzed to see how many patients could consider the second generation protease inhibitors (PIs), darunavir (DRV) and tipranavir (TPV) treatment, based on phenotypic results.
Identifying key mutations that predict discordant response between the two drugs could prove helpful in deciding which to use.
Methods: Specimens collected 2006-2008 and assayed with Monogram Biosciences PhenoSense GT were queried. Results were categorized according to their upper and lower clinical cut-offs as resistant (R), partially susceptible (PS), or susceptible (S) to ritonavir-boosted TPV, DRV, lopinavir (LPV), saquinavir (SQV), atazanavir (ATV), and fosamprenavir (fAPV). Patients with a discordancy in phenotypic resistance to DRV/r and TPV/r were investigated to observe which mutations were more prevalent in each set of patients.
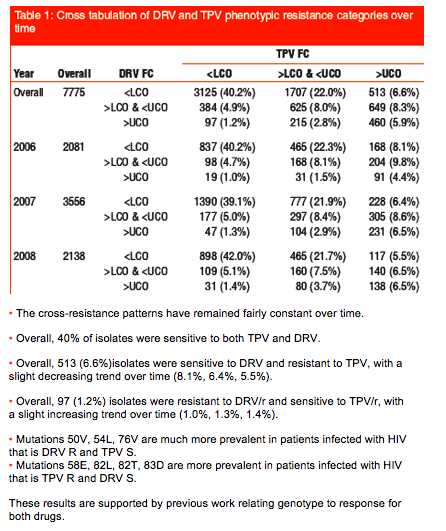
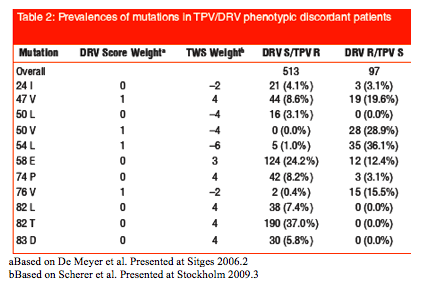
Results: There were 513 (6.6%) isolates that were S to DRV and R to TPV (DRV-S/TPV-R) and 97 (1.2%) that were S to TPV and R to DRV (DRV-R/TPV-S). Amino acid substitutions that showed higher prevalence in patients with DRV-S/TPV-R virus were 82L/T (44.4% vs. 0% of patients with DRV-S/TPV-R vs DRV-R/TPV-S had the mutation) and 83D (5.8% vs. 0%). In contrast substitutions that showed higher prevalence in patients with DRV-R/TPV-S virus were 50V (0.0% vs. 28.9%), 54L (1.0% vs. 36.1%) and 76V (0.4% vs. 15.5%).
Conclusions: Common DRV-associated resistance mutations 50V, 54L and 76V that are associated with an improved clinical response to TPV/r were more prevalent in patients with phenotypic resistance to DRV and susceptibility to TPV. In contrast 82L/T and 83D, mutations associated with resistance to TPV but not to DRV, were more prevalent in patients with resistance to TPV and susceptibility to DRV
INTRODUCTION
Decisions about the next regimen to use for an antiretroviral therapy experienced HIV-1 infected patient are based on an assessment of resistance, which may involve genotypic sequencing of the viral population circulating in the peripheral blood or in vitro testing of the phenotypic resistance to candidate drugs or an assesment of both genotype and phenotype. A database of test results for clinical isolates sent for both genotypic and phenotypic testing can be examined to see what resistance patterns are being observed and how those patterns are
changing over time.
Monogram Biosciences offers a PhenoSense GT assay conducting both phenotype and genotype resistance testing. The database of results from this testing offers the opportunity to look at what drugs are available for patients considering a change in therapy.
Evaluations based on phenotypic testing are attractive when considering the choice of protease inhibitor in a PI-experienced patient because the complex patterns of mutations in treatment-experienced patients makes interpretations based on genotype alone extremely difficult, even with the development of a number of competing interpretative algorithms. The objectives of the present study were to identify recent patterns of phenotypic susceptibility to tipranavir and darunavir in the Monogram Biosciences database and to identify amino acid substitutions associated with samples with differential phenotypic susceptibility to
these two agents.
METHODS
Population: Patients with clinical isolates tested for phenotype and genotype 2006-2008.
· Sent to Monogram Biosciences and successfully producing results for
both tests.
· Not participating in a clinical trial.
· Having a phenotypic result above the lower clinical cut-off (LCO) for at
least one of atazanavir, darunavir, fosamprenavir, lopinavir, and
saquinavir.
The population was interrogated to look at patterns of resistance to four widely used protease inhibitors: atazanavir, fosamprenavir, lopinavir, and saquinavir, along with patterns of resistance and cross-resistance with the two most recently introduced second generation protease inhibitors: darunavir and tipranavir.
Phenotypic outcomes were categorized according to the LCO and the upper clinical cut-off (UCO) established by Monogram Biosciences on the basis of clinical data.1
· Below the LCO indicates a fully responsive susceptible (S) virus.
· Between the LCO and the UCO indicates a partially responsive, partially susceptible (PS) virus.
· Above the UCO indicates a non-responsive resistant (R) virus.
To further investigate apparent hypersusceptibility with tipranavir as observed in other investigations, a FC less than 0.5 was considered hypersusceptible (HS).
Patients were identified that had discordant phenotypic resistance for TPV/r and DRV/r, described in the results sections as DRV S/TPV R (i.e. virus predicted susceptible to DRV/r and resistant to TPV/r based on phenotype) and DRV R/TPV S. Prevalences of mutations that play key roles in the respective genotypic resistance algorithms2,3 were tabulated for both sets of patients. The mutations identified in both tipranavir and darunavir algorithms included L24I, I50V, I50L, I54L, Q58E, L76V, I47V, T74P, V82L, V82T, N83D.
Results are reported descriptively as rates and proportions.
RESULTS
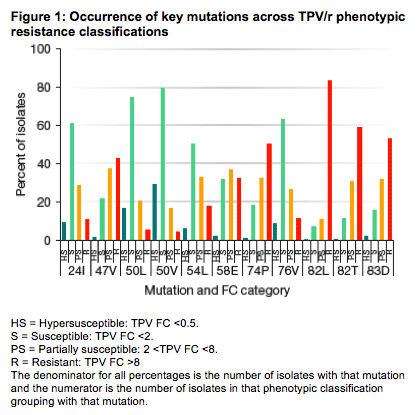
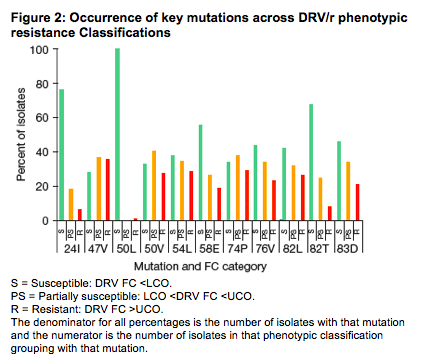
Figures 1 and 2 provide an assessment of the association of these mutations with phenotypic resistance to TPV/r and DRV/r. Some key results:
· For TPV/r, over 80% of isolates with the 82L mutation were resistant, followed by 82T (58.6%), 83D (52.6%), 74P (49.9%) and 47V (42.1%).
· In contrast, the mutations 50V (79.7% of isolates with that mutation were S to TPV), 50L (74.9%), 76V (63.1%), 24I (61.0%) and 54L (50.4%) are much more likely to be seen in patients infected with HIV that was susceptible to TPV/r.
· These results are consistent with what has been shown in the TPV weighted score development.2
· For DRV, the mutations shown to be associated with resistance to DRV all appear at about the same rate across the phenotypic resistance categories.
· Isolates with mutations 58E, 82T and 83D (major TPV/r resistance associated mutations) appear more often in patients predicted S to DRV/r.
· An interesting result is that 53/54 occurrences of the mutation 50L are in patients infected with HIV that was S to DRV/r. Also, 24I is much more prevalent in DRV-S isolates.
REFERENCES
1. Defining the Upper and Lower Phenotypic Clinical Cut-offs for Darunavir/Ritonavir by the PhenoSense Assay. Coakley E, Chappey C, Benhamida J, Picchio G, de Bethune MP. 14th Conference on Retroviruses and Opportunistic Infections. 2007.
2. De Meyer, S., I. Dierynck, E. Lathouwers, B. Van Baelen, T. Vangeneugden, S. Spinosa-Guzman, M. Peeters, G. Picchio, and M. de Bethune. 2008a. Phenotypic and genotypic determinants of resistance to darunavir: analysis of data from treatment experienced patients in POWER 1, 2, 3 and DUET-1 and 2 [abstract 33]. Antivir Ther 13: Suppl 3:A33
3. J Scherer, JM Schapiro, F Maggiolo, Cf Perno, C Boucher, J Baxter, H Gellermann, C Tilke, MM Santoro, DB Hall. Improving the prediction of virologic response to tipranavir: the development of a tipranavir weighted mutation score. 7th European HIV Drug Resistance Workshop, 25 - 27 March, 2009, Stockholm, Sweden (Poster # 94).
4. Mutations 24I, 50L/V, 54L and 76V, selected by other protease inhibitors, predict durable response to tipranavir in treatment experienced patients when two or more are present. Hall DB, Baxter J, Schapiro J, Boucher CAB, Tilke C, Scherer J. 2008. XVII International HIV Drug Resistance Workshop. Sitges, Spain.
Acknowledgement
Supported by Boehringer Ingelheim Pharmaceuticals
|
| |
|
 |
 |
|
|