 |
 |
 |
| |
Metabolic Syndrome (MS) [glucose/diabetes] Is a Negative Predictor of Treatment Outcome in Patients With Chronic Hepatitis C: Results From the IDEAL Study
|
| |
| |
Reported by Jules Levin
EASL Apr 14-18 2010 Vienna Austria
M. S. Sulkowski,1 J. W. King,2 S. A. Harrison,3 L. Rossaro,4 K.-Q. Hu,5 E. J. Lawitz,6 M. L. Shiffman,7 A. J. Muir,8 G. W. Galler,9 J. McCone,10 L. M. Nyberg,11 W. M. Lee,12 R. Ghalib,13 J. G. McHutchison,8 S. Noviello,14 V. S. Goteti,14 J. K. Albrecht,14 C. A. Brass14
1Johns Hopkins University School of Medicine, Baltimore, Maryland, USA; 2Louisiana State University Health Sciences Center, Shreveport, Louisiana, USA; 3Brooke Army Medical Center, Fort Sam Houston, Texas, USA; 4University of California Davis Medical Center, Sacramento, California, USA;
5University of California-Irvine Medical Center, Irvine, California, USA; 6Alamo Medical Research, San Antonio, Texas, USA; 7Liver Institute of Virginia, Bon Secours Health System, Newport News, Virginia, USA; 8Duke Clinical Research Institute, Durham, North Carolina, USA; 9Kelsey-Seybold Research
Foundation, Houston, Texas, USA; 10Mount Vernon Endoscopy Center, Alexandria, Virginia, USA; 11Kaiser Permanente, San Diego Medical Center, San Diego, California, USA; 12University of Texas Southwestern Medical Center at Dallas, Dallas, Texas, USA;
13The Liver Institute at Methodist Dallas, Dallas, Texas, USA; 14Schering-Plough Corporation, now Merck & Co., Inc., Whitehouse Station, New Jersey, USA
"Patients with elevated glucose and HDL-C (18%; 557/3070) had a very low probability of SVR (OR = 1.97)"
Author Summary
· Baseline MS, particularly elevated glucose level (glucose intolerance), is a negative predictor of SVR in patients with chronic hepatitis C genotype 1 infection receiving PEG-IFN alfa plus RBV therapy
· Low HDL-C was associated with improved SVR rate
Author Conclusions
· While MS is a predictor of response to PEG-IFN/RBV therapy in patients with chronic hepatitis C genotype 1 infection, the current definition of MS may not present the ideal framework to investigate HCV treatment response because 3 components are strong independent "negative" predictors of SVR (elevated fasting glucose, hypertension, elevated triglycerides), whereas 1 component of MS (low HDL) is a strong "positive" predictor of SVR
Abstract
Background/Aims: Small studies have suggested that metabolic syndrome and its various components are associated with poor response to HCV therapy, or may normalize with HCV eradication. We retrospectively interrogated the IDEAL database to examine the role of MS in HCV therapy.
Methods: 3070 treatment-naive, HCV genotype-1 infected adults received peginterferon (PEG) alfa-2b 1.5 or 1 µg/kg/wk plus ribavirin (RBV) 800-1400 mg/d or PEG alfa-2a 180 µg/wk plus RBV 1000-1200 mg/d. Metabolic syndrome was defined by the IDF/AHA criteria requiring 3/5 of: 1) fasting glucose ≥5.6 mmol/L or use of diabetes medications, 2) elevated blood pressure (≥130/85) or use of antihypertensive medications, 3) triglycerides ≥150 mg/dL, 4) HDL-C<40 mg/dL (males) or <50 mg/dL (females), 5) central obesity with waist circumference >102cm (males) or 88cm (females).
Results: 30.3% of patients had MS at baseline, with lower sustained virologic response (SVR) in those with MS (34.9% vs 41.6%, p<0.001). This difference was greater in women (34.7% vs 43.2%, p=0.006) than men (35.0% vs 40.5%, p=0.024). MS was a negative predictor for response (OR=1.3) in nearly all subgroups, with a higher odds ratio in those with advanced fibrosis (OR=1.7). SVR was lower with each additional component of the MS definition present, with the largest decrease from 2 criterion (SVR=40.0%) to 3 criterion (SVR=35.5%), which is consistent with the MS definition. Multivariate regression including MS and each of its components shows that elevated glucose has the best negative predictive value (OR=1.72) but 'high' HDL is a negative predictor of SVR
(OR=1.50); waist circumference and MS are no longer significant predictors of SVR. Patients with both high glucose and HDL (18.1%; 557/3070) had a low probability of SVR (OR= 1.97). Removing central obesity from the MS criteria (not measured in FU), 48% of those with baseline MS no longer met diagnostic criteria six months after completion of therapy due to normalization of one or more of the other factors.
Conclusions: MS is a negative predictor of response to PEG/RBV therapy. Surprisingly, 'high' HDL was also a negative predictor of SVR. Normalization of MS was common.
Abstract updated since submission.
Background
· Metabolic syndrome (MS) is defined by a cluster of abnormalities: insulin resistance, obesity, dyslipidemia, and hypertension.1 Several consensus definitions have been created over the last decade, with most recent refinements substituting hyperglycemia for insulin resistance
· Components of MS have been associated with worsening hepatitis C infection, as well as with poor response to hepatitis C treatment
- I nsulin resistance is more prevalent among patients with hepatitis C than in the general population and increases with higher rates of fibrosis progression2,3
- Furthermore, insulin resistance is known to impair sustained virologic response (SVR) among patients receiving pegylated interferon (PEG-IFN) alfa plus ribavirin (RBV) combination therapy4
- However, the relationship between MS, some of its components, and treatment response are not known
· The Individualized Dosing Efficacy vs Flat Dosing to Assess Optimal Pegylated Interferon Therapy (IDEAL) study was a prospective, randomized study conducted in patients with chronic hepatitis C genotype 1 infection in the United States5
Aim
· To examine the relationship between MS and response to hepatitis C virus (HCV) therapy in the IDEAL study
Patients and Methods
Patients
· Chronic hepatitis C, genotype 1
· Treatment naive
· Age, 18 to 70 years
· Weight, 40 to 125 kg
· Compensated liver disease
· Relevant exclusion criterion:
- Patients weighing >105 to 125 kg with a BMI >30 and 3 or more of the risk factors below:
·· Strong family history of coronary heart disease
·· Uncontrolled hypercholesterolemia
·· Diabetes mellitus
·· Hypertension
·· Smoking
· MS was defined using the International Diabetes Federation/American Heart Association (IDF/AHA) criteria6,7 as patients having ≥3 of the
following 5 criteria:
- Fasting glucose ≥100 mg/dL (≥5.6 mmol/L) or use of diabetes medications
- Blood pressure: systolic (SBP) ≥130 mm Hg or diastolic (DBP) ≥85 mm Hg or use of antihypertensive medications
-Triglycerides (TG) ≥150 mg/dL
--- High-density lipoprotein cholesterol (HDL-C) <40 mg/dL (males) or <50 mg/dL (females)
--- Central obesity with waist circumference >102 cm (males) or >88 cm (females)
Study Design
· IDEAL was a phase 3b, randomized, parallel-arm trial conducted at 118 academic and community centers in the United States (Figure 1)
Figure 1. IDEAL study design. HCV = hepatitis C virus; PEG-IFN = peginterferon; RBV = ribavirin
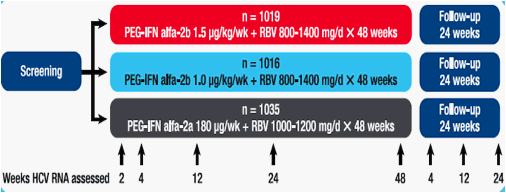
Assessments
· Fasting glucose, blood pressure, TG levels, and HDL-C levels were measured at baseline (screening visit 2) and follow-up week 24
· Waist circumference was measured at baseline (screening visit 2) only
· HCV RNA levels were assessed at baseline (screening visit 2), at treatment weeks 2, 4, 12, 24, and 48, and at follow-up weeks 4, 12, and 24
· SVR was defined as undetectable HCV RNA at the end of follow-up (week 24 or, if missing, week 12)
--- HCV RNA was measured using COBAS TaqMan (Roche; lower limit of quantitation, 27 IU/mL)
Results
Patients
· 30% (929/3070) of patients demonstrated MS at baseline (≥3 of the 5 criteria below):
- 61% (565/929) of patients had baseline fasting glucose ≥5.6 mmol/L or were receiving diabetes medications
- 85% (787/929) of patients had SBP ≥130 mm Hg or DBP ≥85 mm Hg or were receiving antihypertensive medications
- 57% (529/929) of patients had TG ≥150 mg/dL
- 68% (631/929) of patients had HDL-C levels <40 mg/dL (males) or <50 mg/dL (females)
- 77% (716/929) of patients had waist circumference >102 cm in males or >88 cm in females
· Patient characteristics are shown in Table 1
--- Patients with baseline MS were older and heavier, and more had advanced fibrosis/cirrhosis and steatosis compared with those without baseline MS
Table 1. Baseline Patient Characteristics
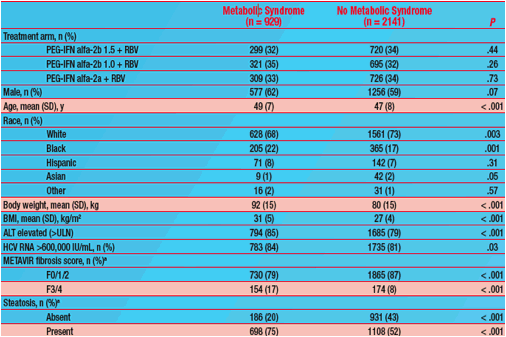
a147 missing.
ALT = alanine aminotransferase; BMI = body mass index; HCV = hepatitis C virus;
PEG-IFN = peginterferon; RBV = ribavirin; SD = standard deviation; ULN = upper limit of normal.
Virologic Response
· SVR was lower in patients with MS at baseline than those without MS (Figure 2A)
· Among patients with MS, those with elevated fasting glucose or on diabetes medications attained the lowest rate of SVR, and those with decreased HDL-C levels had the highest rate of SVR (Figure 2B)
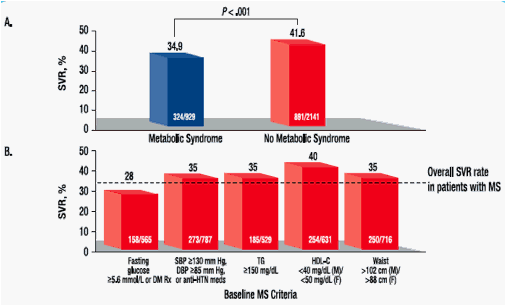
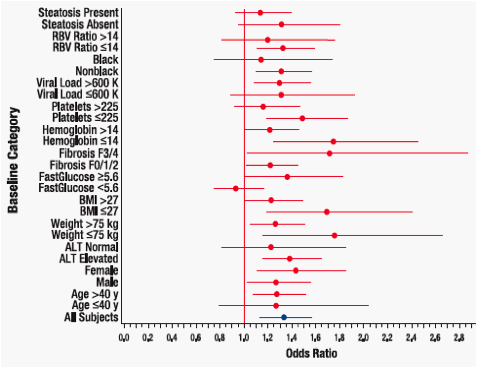
· MS was a negative predictor of SVR (odds ratio [OR] = 1.3) (Figure 3)
- Most patient demographic subgroups with baseline MS had lower SVR rates compared with those without MS
- This observation was apparent in all but one baseline subgroup (fasting glucose <5.6 mmol/L), particularly in patients with advanced fibrosis (OR = 1.7)
--- The effect of baseline MS on SVR was more pronounced in women (35% [122/352] vs 43% [382/885]) than men (35% [202/577] vs 41% [509/1256])
Figure 3. Forest plot of odds ratios (95% confidence intervals) for sustained virologic response rates according to baseline characteristics comparing patients without metabolic syndrome to those with metabolic syndrome. ALT = alanine aminotransferase; BMI = body mass index; RBV = ribavirin. RBV ratio = assigned RBV dose (mg/kg/day).
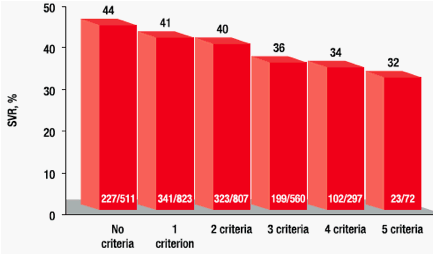
· SVR decreased with each additional component of the MS definition (Figure 4)
--- The largest reduction in SVR occurred between the patients with 2 criteria compared with 3 criteria that define MS
Figure 4. Sustained virologic response (SVR) according to presence of metabolic syndrome criteria
· Multivariate regression analysis including MS and each of its components revealed that elevated glucose or being on diabetes
medications (OR = 1.72) and "high" HDL-C (OR = 1.49) were strong negative predictors of SVR (Table 2)
· Patients with elevated glucose and HDL-C (18%; 557/3070) had a very low probability of SVR (OR = 1.97)
--- Waist circumference and MS were not significant predictors of SVR
Table 2. Multivariate Logistic Regression Analysis for Sustained Virologic Response Using Stepwise Selection Method

aHDL-C ≥40 mg/dL (M) or ≥50 mg/dL (F) vs <40 mg/dL (M) or <50 mg/dL (F) has OR = 0.67 (95% confidence interval 0.57-0.79).
bCalculated using multivariate logistic regression model without stepwise selection method.
Anti-HTN meds = antihypertensive medications; DM Rx = treatment for diabetes mellitus; F = female; HDL-C = high-density lipoprotein cholesterol;
M = male; MS = metabolic syndrome
Normalization of MS at End of Follow-up
· 48% (220/454) of patients with baseline MS (defined as ≥3 of 4 of the MS criteria, excluding waist circumference) no longer met MS
criteria at the end of the 24-week follow-up due to normalization of 1 or more of the MS diagnostic criteria
· Among the patients with baseline MS but no MS at the end of the 24-week follow-up:
- 63% (93/148) had glucose values <100 mg/dL (<5.6 mmol/L) and no diabetes medications
- 42% (84/201) had SBP <130 mm Hg and DBP <85 mm Hg and no antihypertensive medications
- 71% (119/167) had TG <150 mg/dL
- 61% (108/178) had HDL-C levels ≥40 mg/dL (males) and ≥50 mg/dL (females)
--- Central obesity was removed from the MS diagnostic criteria because it was not measured after completion of therapy
References
1. Huang PL. Dis Model Mech. 2009;2(5-6):231-237.
2. Zein CO et al. Am J Gastroenterol. 2005;100(1):48-55.
3. Hui JM et al. Gastroenterology. 2003;125(6):1695-1704.
4. Kawaguchi T et al. Am J Gastroenterol. 2007;102(3):570-576.
5. McHutchison JG et al. N Engl J Med. 2009;361(6):580-593.
6. International Diabetes Federation.
http://www.idf.org/webdata/docs/IDF_Metasyndrome_definition.pdf.
7. Grundy SM et al. Circulation. 2005;112(17):2735-2751.
|
| |
|
 |
 |
|
|