 |
 |
 |
| |
A Pilot Study of Abacavir/Lamivudine and Raltegravir in Antiretroviral-Naïve HIV-1 Infected Subjects: 48 Week Results
|
| |
| |
Reported by Jules Levin
18th Intl AIDS Conf Vienna July 18-23 2010
B Young1, T Vanig2, E DeJesus3, T Hawkins4, L Yau5, B Ha5 and the SHIELD Study Team. 1Rocky Mountain CARES, Denver, CO and Health Connections International, Amsterdam; 2Spectrum Medical Group, Phoenix, AZ; 3Orlando Immunology Center, Orlando, FL; 4Southwest CARE Center, Santa Fe, NM; 5GlaxoSmithKline, RTP, NC


ABSTRACT
Background - RAL is an HIV-1 integrase strand-transfer inhibitor with potent in
vitro activity that has not been evaluated with ABC/3TC in antiretroviral-naïve,
HIV-1 infected individuals. The objective of the SHIELD study was to evaluate
the efficacy and safety of ABC/3TC+RAL as initial therapy.
Methods - This is a 96-week, open-label, pilot, prospective, multi-center study
evaluating ABC/3TC (600 mg/300 mg once daily) + RAL (400 mg twice daily) in
subjects with entry viral load (VL) >1,000 c/mL. Subjects were excluded if they
were HLA-B*5701 positive or had RAL, ABC, or 3TC resistance mutations.
Virologic failure (VF) was defined as failure to achieve VL <400 c/mL by Wk 24
or confirmed rebound ≥400 c/mL or confirmed 1 log10 c/mL increase above
nadir. The planned Week 48 interim analysis is reported.
Results - SHIELD enrolled 35 subjects. Baseline (BL) characteristics were:
median HIV-1 RNA 4.8 log10 c/mL (34% ≥100,000 c/mL), median CD4 301
cells/mm3 (20% <200 cells/mm3). Two subjects (6%) prematurely discontinued
study by Week 48: adverse event (1) and lost-to-follow-up (1).
At Week 48, the proportion of subjects with HIV-1 RNA <400 and <50 c/mL were both 91% (32/35) by ITT M=F. Median CD4 change from BL was 247 cells/mm3. One subject met VF criteria. Five subjects (14%) had drug-related grade 2-4 adverse events. No drug-related SAEs were reported.
Week 48 fasting lipid changes [median (95% confidence intervals)] were not different from BL for total/HDL cholesterol ratio [0.01 (-0.23, 0.46)] and triglycerides [-1 (-11.5, 58.5) mg/dL], and increased for LDL cholesterol [9 (3.5, 17) mg/dL], HDL cholesterol [5.5 (2-8) mg/dL], and total cholesterol [16.5 (11-29.5) mg/dL].
Conclusions In this pilot study, RAL+ABC/3TC achieved sustained virologic
suppression and exhibited potent antiretroviral activity through Week 48, with
limited impact on fasting lipids.
INTRODUCTION
The December 2009 DHHS Guidelines1 recommend initiating HAART in treatment-naïve patients with 2 NRTIs and either a NNRTI, a boosted PI, or a integrase strand-transfer inhibitor. The Guidelines specifically identify the need for additional data on the combination of the NRTIs abacavir sulfate (ABC) and lamivudine (3TC) with the integrase inhibitor raltegravir (RAL).
While all combinations of antiretroviral agents must be individually evaluated for potency, safety/tolerability, and treatment-emergent resistance patterns, the myriad of available choices make it increasingly possible to focus on long-term safety. In previous studies RAL has been shown to have a minimal impact
on the serum levels of total cholesterol, LDL cholesterol, and triglycerides, with modest increases in HDL cholesterol.2,3 ABC/3TC has been associated with moderate increases in lipids,4,5 although the total to HDL cholesterol ratio remained largely unchanged.
This objective of this study was to evaluate the efficacy and safety
of ABC/3TC + RAL, with a particular emphasis on lipid levels.
METHODS
The SHIELD study (COL111429) is an ongoing 96-week, open-label, prospective, multicenter trial evaluating ABC/3TC 600 mg/300 mg once daily (EPZICOM, GlaxoSmithKline, RTP, NC) and RAL 400 mg twice daily (Isentress, Merck & Co., Inc., Whitehouse Station, NJ) in antiretroviral-naïve HLA-B*5701-negative adults with screening HIV-1 RNA >1,000 c/mL.
Patients were excluded if they had an active or acute CDC Clinical Category C event (AIDS-defining illness) within 30 days of screening, had chronic hepatitis B infection (HBsAg+), or if their screening viral genotype indicated the presence of key mutation(s) to any study drug. For ABC and 3TC, key mutations were: K65R;
L74V; Y115F; and two or more thymidine analog mutations (M41L, D67N, K70R, K219Q or E) that included changes at either L210 or T215. For RAL, key mutations were Q148H/R/K and N155H. There were no restrictions on screening CD4 cell count.
Virologic failure was defined as having either confirmed virologic non-response (HIV-1 RNA >400 c/mL at Week 24 [W24]) or confirmed virologic rebound (HIV-1 RNA ≥400 c/mL after an initial response of HIV-1 RNA <400 c/mL or >1 log10 c/mL increase above nadir). In the case of clinically suspected hypersensitivity to
ABC, subjects were permitted to substitute ABC/3TC with zidovudine 300 mg/lamivudine 150 mg twice daily (ZDV/3TC [COMBIVIR], GlaxoSmithKline, RTP, NC) and were not discontinued from the study.
The primary efficacy endpoint of this study is the percentage of subjects with HIV-1 RNA <50 c/mL at W48. The primary safety endpoint is the percentage of subjects with treatment-related grade 3 or 4 adverse events (AEs) and laboratory abnormalities.
RESULTS
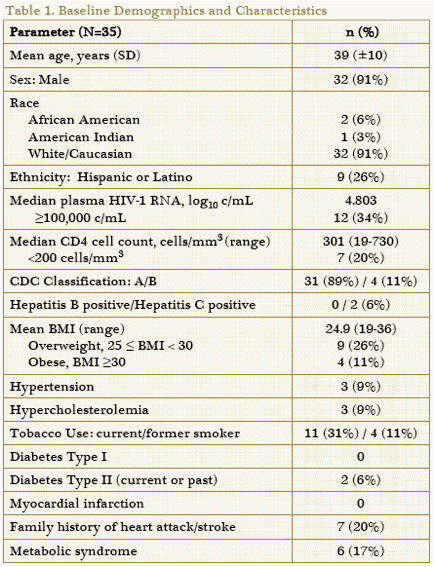
Thirty-five subjects with a mean age of 39 years enrolled in the study (Table 1). At baseline, 34% had HIV-1 RNA ≥100,000 c/mL, and 20% had CD4 cell counts <200 cells/mm3. While 37% of patients were overweight or obese and 43% were current or former tobacco smokers, the incidence of hypertension (9%) and hypercholesterolemia (9%) were low.
Subject Accountability
Thirty four (34) of 35 subjects completed W48. One patient discontinued the study due to AEs (affect lability and depression).
Efficacy Results
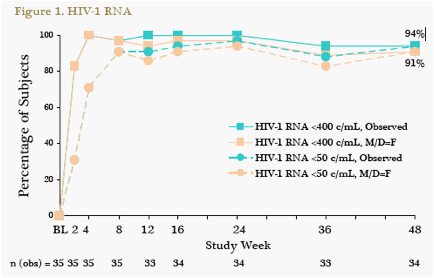
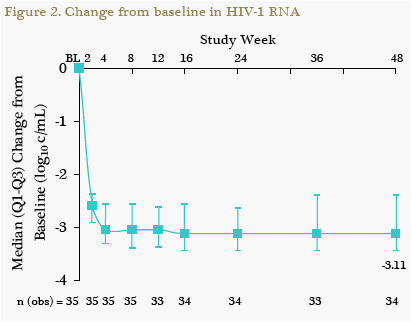
At W48, 91% (32/35) of patients achieved the primary endpoint of HIV-1 RNA <50 c/mL using a MD=F analysis and 94% (32/34) using an observed analysis (Figure 1). The results were the same for HIV-1 RNA <400 c/mL. Virologic suppression was rapid and sustained (Figure 2).
One patient experienced virologic failure and discontinued from the study after W48. Retrospective genotypic analyses indicated multiple RT, PRO, and integrase mutations at baseline.
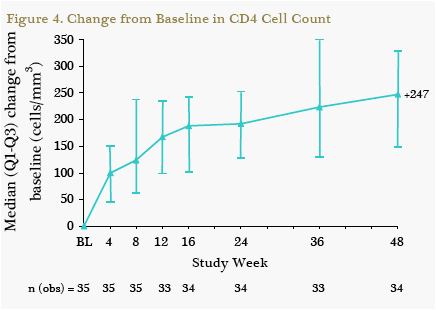
All 12 patients with baseline viral loads ≥100,000 c/mL had HIV-1 RNA <50 c/mL at W48 (Figure 3). For patients with low baseline viral loads, 87% (20/23) had HIV-1 RNA <50 c/mL at W48 using the MD=F analysis and 91% (20/22) using an observed analysis. Overall, the median increase in CD4 cell count from baseline to W48 was 247 cells/mm3 (Figure 4).
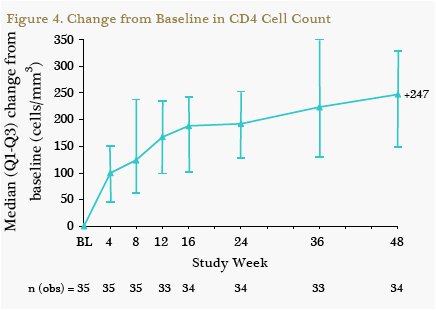
Safety Results
Through W48, 15% (5/35) of patients experienced treatment-related grade 2 to 4 AEs (Table 2); only fatigue (n=2) occurred in >1 patient. No patient experienced treatment-related serious AEs. There were no suspected hypersensitivity reactions to abacavir.
Over 48 weeks, statistically significant increases were observed in median fasting total, HDL, and LDL cholesterol, while triglyceride levels remained stable (Figure 5). Total:HDL cholesterol ratio also remained stable.
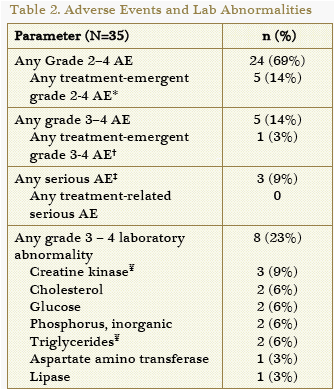
*Only fatigue (n=2) affected >1 patient in this study
Patient withdrew from the study due to affect lability and depression
Small intestinal perforation, cytomegalovirus , deep vein thrombosis
Treatment-emergent grade 4 toxicities were creatinine kinase (2 patients) and
triglycerides (1 patient)
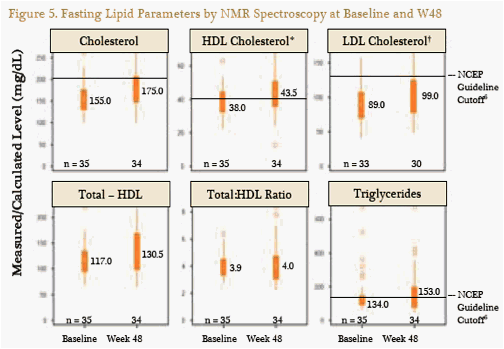
*Direct measurement
Calculated
In each panel, the solid orange bar spans quartile 1 to quartile 3, the lighter
circle within the solid bar is the median, the lines indicate the minimum and
maximum, and the circles are outliers in the data.
Inflammatory Biomarkers
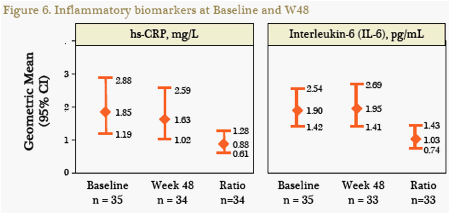
Median hs-CRP decreased by 12% and median levels of interleukin-6 increased
by 3% (Figure 6), but these changes were not statistically significant.

|
| |
|
 |
 |
|
|