 |
 |
 |
| |
Mechanisms of isolated unconjugated hyperbilirubinaemia
induced by the HCV NS3/4A protease inhibitor BI 201335
|
| |
| |
Reported by Jules Levin EASL 2011 Berlin Germany March 30-Apr 2
Rucha Sane,1 Lalitha Podila,1 Arti Mathur,1 Kirsten Mease,1 Mitchell Taub,1 Donald Tweedie,1 Quihong Huang,1 Mabrouk Elgadi,2 Gerhard Nehmiz,3 Gerd Steinmann3
1Boehringer Ingelheim Pharma Inc., Ridgefield, CT, USA; 2Boehringer Ingelheim Canada Ltd, Burlington, Canada; 3Boehringer Ingelheim Pharma GmbH & Co-KG, Biberach, Germany
AUTHOR CONCLUSIONS
· BI 201335 for the treatment of chronic HCV GT-1 infection causes dose-dependent increases in predominantly unconjugated bilirubin without inducing haemolysis or liver injury in animals and humans. Thus, interactions of BI 201335 with bilirubin metabolism and excretion are the most likely reasons for this effect
· BI 201335 does perturb a number of processes involved in bilirubin disposition in vitro, including uptake into hepatocytes (OATP1B1), inhibition of metabolism (UGT1A1), and inhibition of efflux into bile (MRP2). Based on the strong inhibitory effect of BI 201335, at relevant drug concentrations, and the close correlation of hyperbilirubinaemia with UGT1A1 genotype in humans, UGT1A1 inhibition may be responsible for the observed hyperbilirubinaemia; this mechanism has been proposed for other drugs, such as atazanavir. However the other mechanisms (OATP1B1 and MRP2 inhibition) may also contribute to the elevation of bilirubin
· Most importantly, isolated unconjugated hyperbilirubinaemia associated with BI 201335 intake was rapidly reversible and not associated with liver injury, haemolysis or clinical symptoms other than usually mild jaundice in healthy volunteers and chronic HCV patients
ABSTRACT
Background: Reversible asymptomatic unconjugated hyperbilirubinaemia was observed on treatment of animals and humans with the hepatitis C virus (HCV) NS3/4A protease inhibitor BI 201335. In absence of liver injury and haemolysis, hyperbilirubinaemia can be caused by interference with bilirubin disposition.
Methods: Liver histology and safety laboratory tests were assessed in rhesus monkeys. The effect of BI 201335 on [3H]bilirubin uptake was studied using primary rat hepatocytes. OATP1B1 inhibition was evaluated in HEK293 cells expressing OATP1B1 and estradiol-17ß-D-glucuronide (EBG) as a substrate. UGT1A1 inhibition was assessed using human liver microsomes and estradiol as a substrate. Multidrug resistance-associated protein 2 (MRP2) inhibition was evaluated using inverted membrane vesicles expressing MRP2 and EBG as a substrate. The effect on biliary excretion of [3H]bilirubin/conjugated bilirubin was evaluated using sandwich-cultured rat and human hepatocytes. UGT1A1 polymorphisms, safety and tolerability were monitored in clinical phase I and II trials.
Results: In monkeys, unconjugated hyperbilirubinaemia was not associated with haemolysis, alanine aminotransferase elevations or histopathological liver injury. In vitro, BI 201335 inhibited several enzymes and transporters that play a role in bilirubin disposition: BI 201335 (20 μM) decreased the uptake of [3H]bilirubin into rat hepatocytes by ~40%; OATP1B1, a transporter implicated in hepatic uptake of bilirubin, was inhibited with an IC50 of 0.5 μM; UGT1A1 was inhibited with a Ki of 0.2 μM; and MRP2-mediated transport was inhibited with an IC50 of 6.2 μM. In sandwich-cultured hepatocytes, BI 201335 (12.5 μM) reduced the biliary excretion index of [3H]bilirubin by ~56%. In a phase I trial of healthy volunteers with or without Gilbert's syndrome, incidence of hyperbilirubinaemia and peak levels correlated with UGT1A1 polymorphisms. Phase II trials SILEN-C1 and two in chronic HCV patients demonstrated that hyperbilirubinaemia was dose dependent, predominantly unconjugated and not associated with liver injury or haemolysis. Bilirubin elevation was not associated with clinical adverse events, in particular skin and gastrointestinal reactions, and levels normalised rapidly after cessation of BI 201335 in all patients.
Conclusions: BI 201335 for treatment of chronic HCV genotype-1 infection causes dose-dependent increases of predominantly unconjugated bilirubin, which were not associated with liver injury or haemolysis. Thus, hyperbilirubinaemia seen during BI 201335 administration is primarily due to its effect on inhibition of hepatic uptake and UGT1A1.
INTRODUCTION
BI 201335 is a highly potent and specific hepatitis C virus (HCV) NS3/4A protease inhibitor
Phase I and II clinical investigations demonstrate that BI 201335 once daily (QD) is well tolerated and induces robust antiviral responses in HCV genotype-1 (GT-1) patients1-3
Reversible isolated unconjugated hyperbilirubinaemia was observed on-treatment with BI 201335 in animals and humans
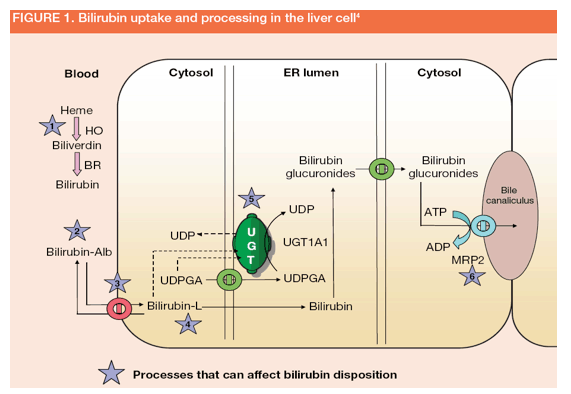
Different drugs such as indinavir, atazanavir, rifampicin, rifamycin and probenecid have been shown to induce hyperbilirubinaemia by perturbing one or more of the hepatocellular processes involved in bilirubin metabolism and excretion (Figure 1)
In the absence of liver injury and haemolysis, hyperbilirubinaemia associated with BI 201335 treatment is likely caused by interference with bilirubin metabolism
METHODS
· Liver histology and safety laboratory tests were assessed in rhesus monkeys treated with BI 201335
· The effect of BI 201335 on [3H]bilirubin uptake was studied using primary rat hepatocytes
· HEK293 cells, transiently expressing a single transporter, were utilised to study the interaction of BI 201335 with the organic anion transporting polypeptide 1B1 (OATP1B1) using estradiol-17ß-D-glucuronide (EBG) as a substrate
-- transfection ready OATP1B1 cDNA in a pCMV6 XL4 vector was obtained from Origene. Prior to transfection, all cDNAs were amplified and characterised for purity, concentration, identification, sequence accuracy, and functional expression of the transporter of interest
-- HEK293 cells were seeded in 12-well plates coated with poly-D-lysine at a density of 400,000 cells/mL. At 16-20 hours post seeding, cells were transfected with cDNA vectors using FuGENE 6. At 48 hours post transfection, cells were incubated with radiolabelled drug or probe substrate. The assay was stopped by washing the cells with ice-cold OptiMEM and then the cells were lysed with 1% sodium dodecyl sulfate
-- samples were analysed using a Wallac Microbeta scintillation counter. Microsoft® Excel and GraphPad Prism version 5.03 were utilised for data analysis
· UGT1A1 inhibition was assessed by incubation of human liver microsomes with the UGT1A1 probe substrate, estradiol, at its apparent Km value, i.e. 20 μM
-- the microsomes were activated by the addition of alamethicin (50 μg/mg protein) with incubation on ice for 15 minutes
-- the reaction was initiated by the addition of UDPGA (5 mM) after a 5 minute preincubation in 37°C water bath with activated enzyme, substrate and BI 201335 at various concentrations
-- the reactions were terminated at desired timepoints and the formation of estradiol 3-glucuronide was monitored using LC/MS/MS
· Multidrug resistance-associated protein 2 (MRP2) inhibition was evaluated using inverted membrane vesicles expressing MRP2 with EBG as substrate. MK 571 was used as a positive control, as it is a known inhibitor of MRP2
· The effect on biliary excretion of [3H]bilirubin/conjugated bilirubin was evaluated using sandwich-cultured rat and human hepatocytes
· UGT1A1 polymorphisms, as well as safety and tolerability of BI 201335, were monitored in clinical phase I and II trials

Preclinical toxicology studies
· In the repeat dose studies in rhesus monkeys of various duration (4, 26 and 39 weeks), a reversible and dose-dependent increase in bilirubin concentration was observed at ≥20 mg/kg/day, as measured by standard clinical pathology laboratory methods
· Bilirubin elevations tended to increase and peak approximately 2 weeks after dosing was initiated and then declined towards baseline levels by the end of the study, but, depending on the dose, were still increased relative to the controls
· The transient increases in bilirubin levels suggest an adaptive response
· Increased total bilirubin was predominantly due to high unconjugated (indirect) bilirubin as confirmed in a 4-week study by a specific, comprehensive high-performance liquid chromatography assay
· Increased indirect bilirubin is not considered a result of liver damage as it was not associated with an elevation of liver enzymes nor histopathological evidence of hepatotoxicity
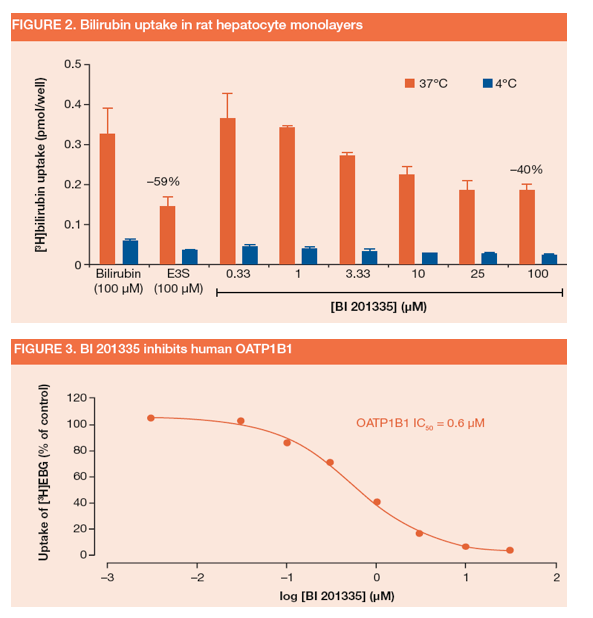
· Experiments were conducted at 37°C and 4°C to separate active and passive uptake of bilirubin into cultured rat hepatocytes, respectively. Estrone-3-sulfate (E3S) was used as a control inhibitor, since it is a substrate of multiple OATPs in human and OATPs in rat
· An in vitro test for potential haemolysis demonstrated no drug-related effects on haemolysis up to the highest concentration tested (100 μg/mL) indicating that hyperbilirubinaemia was not the result of haemolysis
In vitro studies on interference with bilirubin disposition
· In vitro, BI 201335 inhibited several enzymes and transporters that play a role in bilirubin disposition:
-- BI 201335 (20 μM) decreased the uptake of [3H]bilirubin into rat hepatocytes by ~40% (Figure 2)
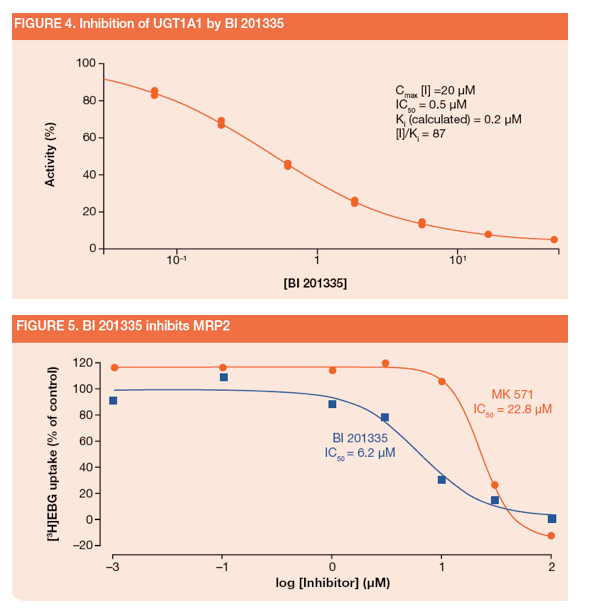
-- OATP1B1, a transporter implicated in hepatic uptake of bilirubin, was inhibited with an IC50 of 0.6 μM (Figure 3)
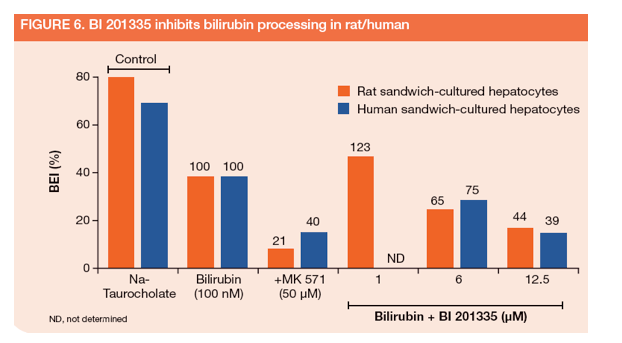
-- UGT1A1 was inhibited with a Ki of 0.2 μM (Figure 4)
-- MRP2 was inhibited with an IC50 of 6.2 μM (Figure 5)
-- in sandwich-cultured hepatocytes, BI 201335 (12.5 μM) reduced the biliary excretion index (BEI) of [3H]bilirubin by ~56% (Figure 6)
Clinical studies in healthy volunteers and patients with chronic HCV infection
· In a phase I trial (1220.6) of healthy volunteers without or with Gilbert's syndrome (GS) over 3 or 4 weeks, respectively, incidence of hyperbilirubinaemia and peak levels of unconjugated bilirubin correlated with UGT1A1 polymorphisms5
· Of the 9 subjects with GS, 5 were homozygous for A(TA7)TAA allele (*28/*28) and the remaining four were heterozygous *1/*28
· As expected, 3 of the 5 subjects who were homozygous for GS had elevated total bilirubin at baseline
· While on treatment, all homozygous subjects had total bilirubin elevations up to 4.6 x upper limit of normal (ULN), reaching a maximum approximately 3 weeks after the start of treatment (Figure 7)
· In contrast, only 2/7 subjects without *28 polymorphisms, and none of the three heterozygous subjects, developed hyperbilirubinaemia. Peak bilirubin levels in the 2 subjects without this polymorphism were lower than in homozygous subjects, peaking at approximately 40 μM
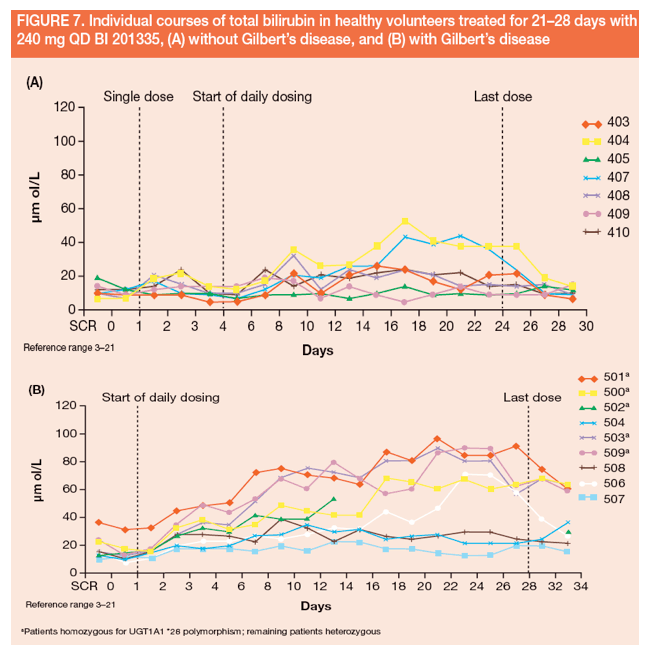
· In conclusion, subjects homozygous for the UGT1A1 *28 polymorphism, which is associated with GS, had higher bilirubin peaks on treatment with 240 mg QD BI 201335 compared with heterozygous subjects or volunteers without this polymorphism
· Individual healthy volunteers with GS experienced scleral icterus at the 240 mg dose
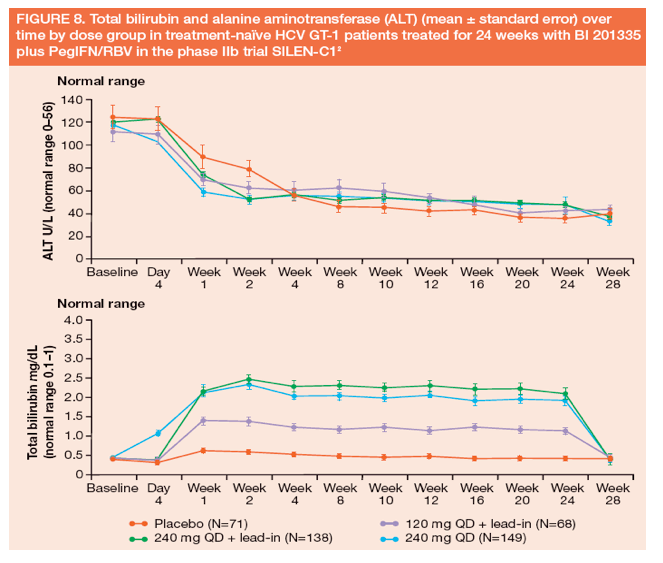
· Clinical phase II trials SILEN-C1, -C2 and -C3 in chronic HCV patients demonstrated that hyperbilirubinaemia was dose-dependent, predominantly unconjugated and not associated with liver injury or haemolysis (Figure 8)
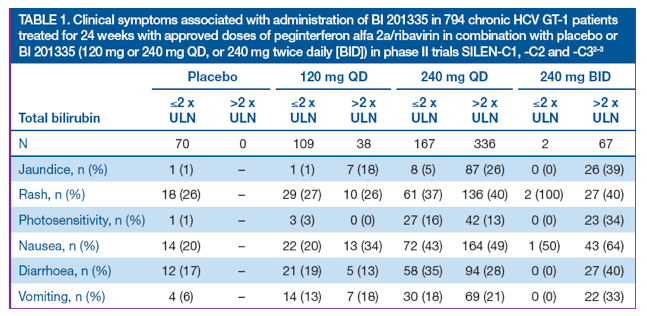
-- bilirubin elevation was associated with the occurrence of icterus in a dose-dependent fashion (18.7% of patients treated with 240 mg QD), but was not associated with any relevant clinical adverse events, in particular skin and gastrointestinal reactions (Table 1), and levels normalised rapidly after cessation of BI 201335 in all patients
References
1. Manns MP, et al. Potency, safety and pharmacokinetics of the NS3/4A protease inhibitor BI201335 in patients with chronic HCV genotype-1 infection. J Hepatol 2010 Nov 11 [Epub ahead of print].
2. Sulkowski MS, et al. SILEN-C1: Sustained Virologic Response (SVR) and safety of BI201335 combined with peginterferon alfa-2a and ribavirin (P/R) in treatment-naïve patients with chronic genotype 1 HCV infection. EASL 2011.
3. Sulkowski MS, et al. SILEN-C2: Sustained Virologic Response (SVR) and safety of BI201335 combined with peginterferon alfa-2a and ribavirin (P/R) in chronic HCV genotype-1 patients with non-response to P/R. EASL 2011.
4. Ah YM, et al. Drug-induced hyperbilirubinemia and the clinical influencing factors. Drug Metab Rev 2008;40(4):511-537.
5. Boehringer Ingelheim data on file.
|
| |
|
 |
 |
|
|