| |
Silibinin monotherapy prevents graft infection after orthotopic liver transplantation in a patient with chronic hepatitis C
|
| |
| |
from Jules: many studies in the past few years conducted by Peter Ferenci have shown IV silibin to have significant antiviral efficacy against HCV (see link below). So for patients who are peg/rbv nonresponders and for that matter responders as well IV silibin should be researched in combination with telaprevir and boceprevir as it might have a particular benefit for prior null responders and partial responders and perhaps most importantly for patients who are contraindicated for peg/rbv but could combine IV silibin with an HCV protease.
Jnl of Hepatology March 2011
Sandra Beinhardt1, Susanne Rasoul-Rockenschaub2, Thomas Matthias Scherzer1, Peter Ferenci1Corresponding Author Informationemail address
1 Internal Medicine III, Department of Gastroenterology and Hepatology, Medical University of Vienna, Austria
2 Division of Transplantation, Department of Surgery, Medical University of Vienna, Austria
To the Editor:
We read with great interest the letter by Neumann et al. [1] on the effect of Silibinin in preventing graft infection in a patient with cirrhosis due to chronic hepatitis C (HCV). We obtained the same result in a patient treated with intravenous (i.v.) Silibinin mono-therapy (Legalon SIL, Rottapharm-Madaus).
In 1994, the 46-year-old male patient with beta-thalassemia was first diagnosed for HCV with mixed genotype 1a/4. Both genotypes were also present upon starting silibinin treatment and on the day of OLTx. In 1998, he was treated with 5MU interferon three times a week and weight based ribavirin. Treatment was stopped due to failure to clear the virus after 24weeks of treatment.
In 2009, he presented with end stage liver failure (Child-Pugh stage C, MELD 20). In the mean time, he had developed insulin dependent diabetes mellitus which is treated with insulin aspartate (Novomix 30 100E/ml, Novo Nordisk Pharma GmbH; 16 IE-0-0/day). He was listed for orthotopic liver transplantation (OLT) on the 29th of October 2009. Based on our observation of the potent antiviral effects of Silibinin [2], [3] a feasibility study was discussed in the transplant setting.
Accordingly, a patient placed first on the waiting list for OLT should receive i.v. Silibinin. In this patient a donor liver became available on day 15 of Silibinin mono-therapy. The data on virus concentrations, obtained pre and after OLT, are shown in Fig. 1. Baseline virus load was low (28.800IU/ml) and decreased on intravenous Silibinin mono-therapy to 43IU/ml on the day of OLTx. Due to a miscommunication between our outpatient center and the OLT-team, treatment was interrupted for 2days after OLT and virus concentration increased to 115IU/ml. Nevertheless, HCV-RNA levels decreased after resuming Silibinin-infusions to 30IU/ml on day 6 and became unquantifiable (<15IU/ml) on day 10, and undetectable on day 22 after OLT. Silibinin was stopped 25days after OLT. During 5months of follow-up, HCV-RNA levels remained undetectable.
Fig. 1. HCV-kinetics during silibinin i.v. monotherapy. HCV RNA levels measured by real-time PCR (Cobas Taqman, Roche Diagnostics, Pleasanton, CA).
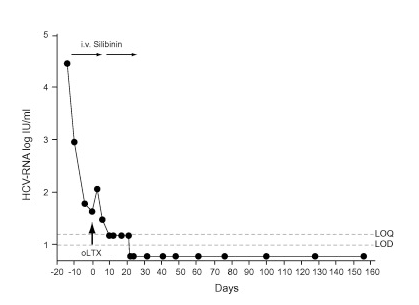
The surgical procedure and post-operative phase went ahead without any complications. Immunosuppressive therapy included prednisolone and cyclosporine A. Like in the patient of Neumann et al. [1] bilirubin levels increased during treatment with Silibinin to a maximum of 17.15mg/dl (on day 3 post OLT) but decreased continuously while the patient was still on Silibinin. The higher increase of bilirubin in our patient could be due to the longer administration of Silibinin combined with the post-operative phase. Aminotransferase levels reached nearly normal values (ASAT 39U/l, ALAT 32U/l) 4days after starting Silibinin-infusions but increased again after OLT and reached normal levels within 4weeks after OLT.
While the goal to prevent graft infection was reached in both patients, the approaches were different. Neumann et al. [1] started Silibinin application 8h after the anhepatic phase (while the viral load was 182IU/ml). Our patient was pretreated with Silibinin for 15days with an interruption of 2days in the post-operative period. Previously, we have shown in a non-responders cohort that the interruption of Silibinin treatment over the weekend results in an increase in viral load [4]. The doses of Silibinin were slightly different. While Neumann et al. used a fixed dose of 1400mg/day we applied 20mg/kg body weight/day. The low baseline viral load may be a condition favoring the action of Silibinin.
These encouraging observations should lead to a prospective evaluation of i.v. Silibinin in this group of patients, having no medical alternatives to prevent graft infection. Studies are needed to find the best way to apply this concept in future (timing, duration, and optimal dose).
Financial disclosures
PF is a member of the global advisory board and of the speaker bureau of ROCHE; he receives also an unrestricted research grant from ROCHE Austria. He is also member of the global advisory boards of Tibotec, Novartis/HGS and Rottapharm-Madaus.
Conflict of interest
All other authors have no financial disclosures to report.
--------------------------------
Successful prevention of hepatitis C virus (HCV) liver graft ...by Silibin
Successful prevention of hepatitis C virus (HCV) liver graft reinfection by silibinin mono-therapy. Articles in Press Jnl of Hepatology April 2010 U.P. ...
www.natap.org/2010/HCV/040710_01.htm
References
[1]. Neumann UP, Biermer M, Eurich D, Neuhaus P, Berg T. Successful prevention of hepatitis C virus (HCV) liver graft reinfection by silibinin monotherapy. J Hepatol. 2010;52:951-952.
[2]. Ferenci P, Scherzer TM, Kerschner H, Rutter K, Beinhardt S, Hofer H, et al. Silibinin is a potent antiviral agent in patients with chronic hepatitis C not responding to pegylated interferon/ribavirin therapy. Gastroenterology. 2008;135:1561-1567.
[3]. Ahmed-Belkacem A, Ahnou N, Barbotte L, Wychowski C, Pallier C, Brillet R, et al. Silibinin and related compounds are direct inhibitors of Hepatitis C virus RNA-dependent RNA polymerase. Gastroenterology. 2010;13:1112-1122.
[4]. Scherzer TM, Beinhardt S, Rutter K, Staettermayer A, Maieron A, Stauber RE et al. Silibinin for treatment of nonresponders to pegerinterferon/ribavirin - search for the optimal dosing schedule. Hepatology 2009; 50 (4 Suppl.) 701A [abstract #847].
------------------------------
Silibinin in hepatitis C related liver transplantation
Jnl of Hepatology March 2011
Thomas Berg, M. Biermer, UP. Neumann
Medizinische Klinik II, Sektion Hepatologie, Universitatsklinikum Leipzig, Liebigstr. 20, 04103 Leipzig, Germany
Reply to Beinhardt et al.;
We congratulate Beinhardt et al. for their interesting paper about successful prevention of hepatitis C virus (HCV) reinfection by short-term administration of high-dose silibinin infusions before and after OLT [1]. Preventing HCV reinfection has an enormous impact on the long term outcome of liver transplantation. Since interferon alpha based treatment regimens are not tolerated early after OLT and also in most instances in the pre-transplant setting, silibinin mono therapy seems to be a promising treatment option - supported by its reasonable safety profile, as documented by its use in amanita-induced acute liver failure.
Success or failure of preventing re-infection with a short term silibinin mono therapy seems to depend mainly on the level of hepatitis C viremia at the time of OLT. The breakdown of hepatitis C viremia, usually seen during the anhepatic phase, works synergistically with the direct antiviral effect of silibinin infusion to support the prevention of re-infection.
As an additional mode of action, a direct inhibitory effect of silymarin components towards the viral entry into hepatocytes has been proposed in vitro [2].
In both cases, in ours [3] and the one reported by Beinhardt et al. [1], HCV RNA levels were low at the time of OLT and particularly after the anhepatic phase (range of 102IU/ml). The approach reported here includes a silibinin treatment before OLT, hereby significantly lowering viremia in order to provide beneficial conditions for the successful prevention of re-infection. This might significantly enlarge the pool of patients benefiting from post-OLT silibinin infusions. However, since the exact timing of the transplantation is usually not feasible, a standardization of the reported procedure seems to be difficult and is probably only possible in the setting of living donor liver transplantation (LDLT).
Up to now little is known about the safety of high dose silibinin infusions in the setting of end stage chronic liver disease. In our hands patients with advanced cirrhosis showed a marked elevation of bilirubin (mainly indirect) in response to silibinin infusions - an observation that was not seen in patients with mild or moderate fibrosis. The clinical significance of this bilirubin elevation remains unclear. At the same time this finding is obviously affecting MELD-score depending organ allocation.
Clearly the potential of silibinin infusions in the peri-transplant period in HCV infected patients needs further evaluation. Studies should address several open questions as the optimal duration of treatment after OLT, the safety and effectiveness of silibinin infusions before OLT, and the potentially enhancing effect of adding ribavirin to silibinin infusions.
Conflict of Interest
The authors who have taken part in this study declared that they do not have anything to disclose regarding funding or conflict of interest with respect to this manuscript.
References
[1]. Beinhardt S, Rasoul-Rockenschaub S, Scherzer TM, Ferenci P. Silibinin monotherapy prevents graft infection after orthotopic liver transplantation in a patient with chronic hepatitis C. J Hepatol. 2011;54:591-592.
[2]. Wagoner J, Negash A, Kane OJ, Martinez LE, Nahmias Y, Bourne N, et al. Multiple effects of silymarin on the hepatitis C virus lifecycle. Hepatology. 2010 Jun;51(6):1912-1921.
[3]. Neumann UP, Biermer M, Eurich D, Neuhaus P, Berg T. Successful prevention of hepatitis C virus (HCV) liver graft reinfection by silibinin monotherapy. J Hepatol. 2010;52:951-952.
|
|
| |
| |
|
|
|