 |
 |
 |
| |
Safety, Acceptability and Pharmacokinetic Assessment (Adherence) of Monthly Dapivirine Vaginal Microbicide Rings (Ring-004) for HIV Prevention
|
| |
| |
Reported by Jules Levin
CROI 2012
Annalene Nel1, Mercy Kamupira1, Cynthia Woodsong1, Ariane van der Straten2, Elizabeth Montgomery2, Neli‘tte van Niekerk1, Jeremy Nuttall1 1 International Partnership for Microbicides, Silver Spring, MD, USA2 WomenŐs Global Health Imperative, RTI International, San Francisco, CA, USA
ABSTRACT
Background:
Dapivirine (TMC 120) is a non-nucleoside reverse transcriptase inhibitor in development as a microbicide for prevention of male to female HIV-transmission. Formulation of dapivirine in vaginal rings for monthly use represents a potential means of increasing microbicide product adherence, acceptability and efficacy.
Methods:
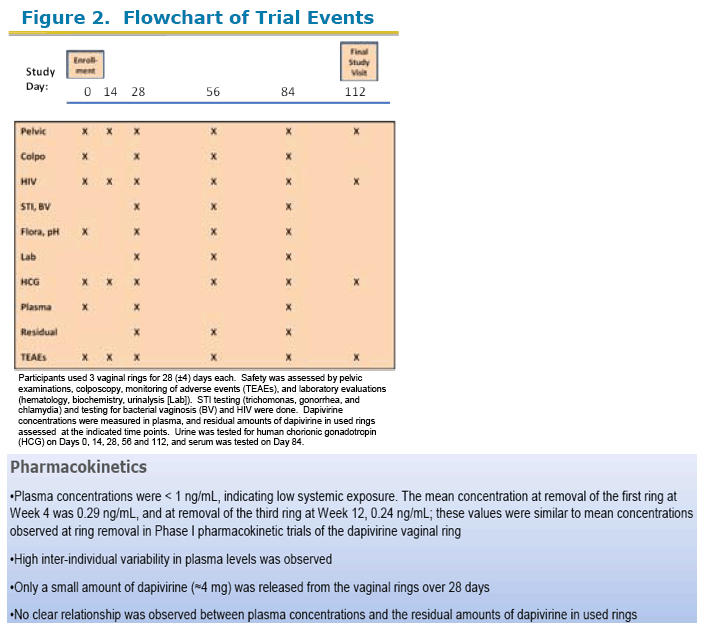
Dapivirine (25 mg) was dispersed in platinum-catalyzed silicone matrix vaginal rings. A double-blind, randomized (1:1) placebo-controlled trial was conducted in 280 healthy, sexually active, HIV-negative African women to evaluate the safety and acceptability of the rings, and assess plasma dapivirine concentrations. Vaginal rings were inserted once every 28 days over a 12-week period. Dapivirine levels were measured in plasma at Weeks 4 and 12, upon removal of the first and third rings. Safety was evaluated by colposcopy, adverse events and laboratory assessments over 16 weeks, and ring acceptability and adherence were assessed by questionnaires.
Results:
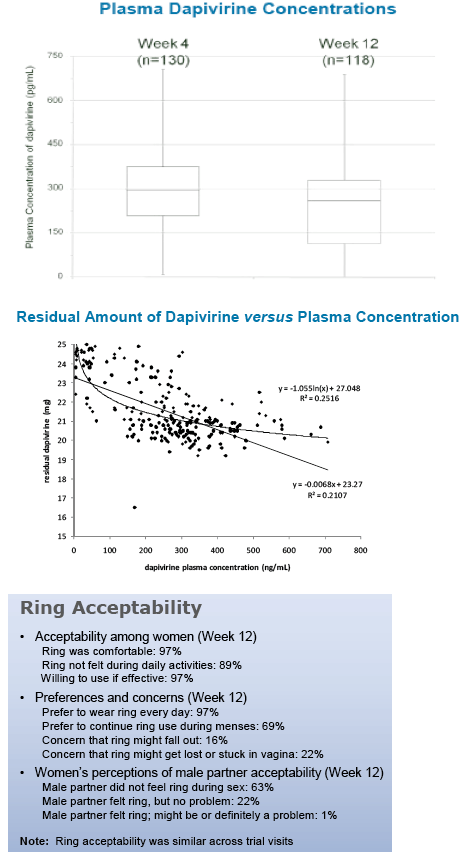
Of 280 women, 265 completed the trial. Systemic exposure to dapivirine was low, with a maximum observed plasma concentration of 708 pg/mL. Mean plasma concentrations were similar at Weeks 4 and 12, at 293 and 239 pg/mL, respectively. Five serious AEs were reported, of which one (tonsillitis; not product-related) occurred in the dapivirine arm. One death (placebo arm; hemopneumothorax, secondary to physical assault) was unrelated to ring use. No AEs were considered to be definitely related to treatment and no non-serious AEs resulted in ring discontinuation. Three HIV seroconversions occurred in the placebo arm. Six pregnancies were reported, two of which occurred in the dapivirine group. Findings probably or possibly related to ring use were similar for dapivirine and placebo. 92% of participants reported no ring removals for the duration of the trial and 97% of women reported that the ring was comfortable to wear. 97% of questionnaire responders were willing to use the vaginal ring in future if it is shown to be safe and effective for HIV prevention.
Conclusions:
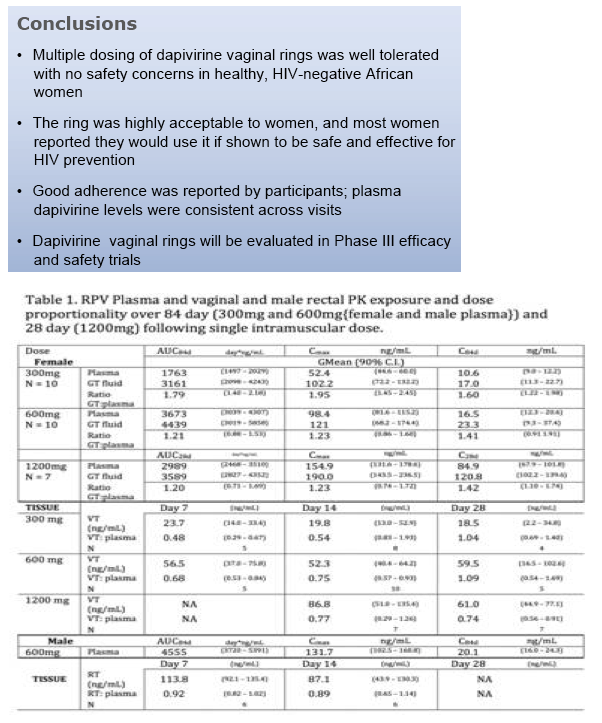
Multiple dosing of monthly dapivirine vaginal rings was well tolerated with no safety concerns in healthy, sexually active HIV-negative African women. Pharmacokinetic and questionnaire data indicated good adherence to ring use. Most participants found the ring acceptable and would use it if shown to be effective for HIV prevention. Dapivirine Ring-004 will be evaluated in expanded safety and Phase III efficacy trials.


|
| |
|
 |
 |
|
|