 |
 |
 |
| |
Prevalence of Chronic Kidney Disease Among HIV-infected Adults in Care in the United States Medical Monitoring Project, 2009
|
| |
| |
Reported by Jules Levin
CROI 2013
Shikha Garg; Carolyn Furlow-Parmley; Emma Frazier; Jacek Skarbinski for the Medical Monitoring Project; Centers for Disease Control and Prevention, Atlanta, GA
I asked the author Garg why HIV+ individuals >60 were showing less CKD compared to the general population in this study while among HIV+ <60 CKD was more prevalent compared to the general population and this was the response:
"One possible explanation is that we may be seeing a cohort effect: people with HIV who live past 60 years may be healthier than similarly aged people in the general population (NHANES). Sicker HIV-infected people with renal disease and other comorbidities may die earlier than their HIV-uninfected counterparts. As a result, in this study, we would be comparing healthier older HIV-infected persons to sicker older HIV-uninfected persons."

ABSTRACT
Background: Chronic kidney disease (CKD) is an important non-infectious cause of morbidity/mortality among the aging U.S. HIV-infected population, but disease burden estimates are lacking.
Methods: We used 2009 data from the Medical Monitoring Project to determine CKD prevalence among a nationally representative cross-sectional sample of HIV-infected adults in care in the U.S. CKD was defined as an estimated glomerular filtration rate (GFR) <60 ml/min/1.73m2 using the Modification of Diet in Renal Disease equation. NHANES data from 2001-2008 were used to compare CKD prevalence among HIV-infected adults to the general U.S. population. Bivariate analyses and multivariate logistic regression were used to examine factors associated with CKD among HIV-infected adults. All analyses accounted for clustering, unequal selection probabilities, and non-response.
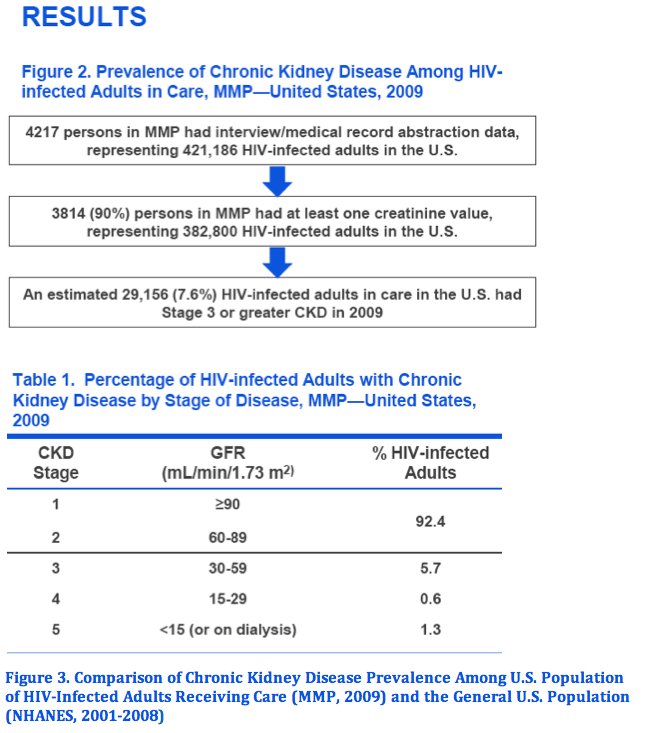
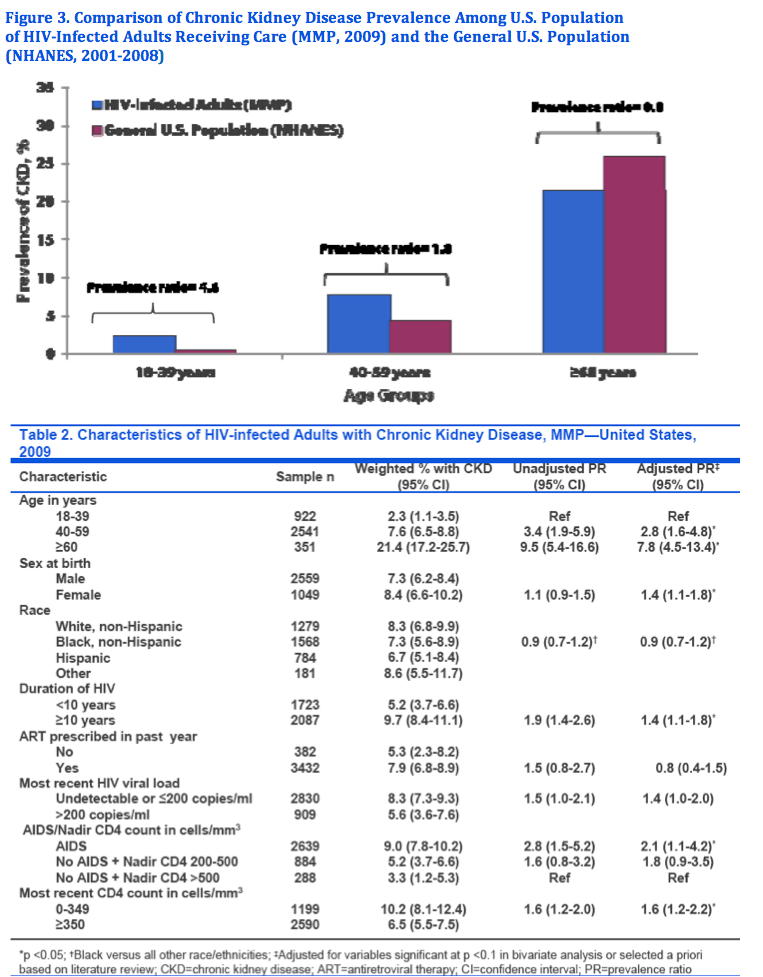
Results: Among 4217 adults, 3814 (90%) had at least one creatinine. The mean population GFR was 93.3 ml/min/1.73m2. An estimated 32,080 persons or 7.6% [95% confidence interval: 6.6%- 8.6%] of HIV-infected adults in care had CKD [5.7% had Stage 3 CKD (GFR 30-59 ml/min/1.73m2), 0.6% had Stage 4 CKD (GFR 15-29 ml/min/1.73m2), and 1.3% had Stage 5 CKD (GFR <15 ml/min/1.73m2)]. Among adults aged ≥60 years, 21% had CKD. Compared to the general U.S. population, the relative prevalence of CKD among HIV-infected adults was substantially higher in adults aged 20-39 years [prevalence ratio (PR) 4.6] and those aged 40-59 years (PR 1.8), but lower in adults aged ≥60 years (PR 0.8). Among HIV-infected adults, factors associated with CKD included older age, female sex, duration of HIV ≥10 years, AIDS diagnosis, and recent CD4 count <350 cells/mm3.
Conclusions: Approximately 1 in 13 HIV-infected adults in care in the U.S. has CKD. While the absolute burden of CKD falls predominantly among those aged ≥60 years, younger HIV-infected adults are substantially more likely to have CKD than the general U.S. population. As the HIV- infected population ages, healthcare providers should minimize the morbidity and mortality associated with CKD by implementing routine CKD screening, aggressively managing comorbid conditions, and among persons with CKD, avoiding nephrotoxic agents and referring early to a nephrologist
Background/Objectives

|
| |
|
 |
 |
|
|