 |
 |
 |
| |
HIV Controllers Have Inflammation & ART Should Be "Considered", study investigators say
|
| |
| |
Reported by Jules Levin
CROI 2013
Link to webcast:
http://webcasts.retroconference.org/console/player/19424?mediaType=podiumVideo
"HIV replication persists in controllers & contributes to a chronic inflammatory state which may have downstream clinical consequences such as accelerated arthreosclerosis, so Antiretroviral therapy should be considered for controllers."
Of note in the presentation just before Dr Hatano's Dr Joyce Sanchez presented "Persistent Abnormalities of Lymphoid Structures in HIV Viremic Controllers.... Background: Chronic inflammation causes collagen deposition and fibrosis in lymphoid tissues, including gut associated lymphoid tissue (GALT) and this process is mediated by HIV replication. It is not known if immunologic or therapeutic control of HIV replication prevents or reverses this process. The investigators hypothesized Elite Controllers would have significantly less collagen deposition in lymphatic structure than other groups of HIV infected persons, but they found "Elite controllers had significantly increased levels of collagen compared to HIV-uninfected, and as well viremic controllers also had higher levels, this came as a surprise Dr Sanchez said and was in contrast to their hypothesis. Not surprisingly they saw high levels of collagen in untreated viremic HIV+ but this was expected & seen before in studies. And they saw high levels of collagen in patients on ART with viral suppression with <350 CD4s or >500 CD4s. Dr Sanchez it was also surprising that all these HIV+ groups whether controllers or suppressed o ART or viremic untreated, all had about the same levels of collagen. And Dr Sanchez suggested ongoing innune activation & low level replication may be responsible.
Methods: We examined GALT tissues from 5 different groups: HIV- (n = 10), untreated HIV controllers (viral load <2000 copies/mL, n = 25, including 14 "elite" controllers with viral load <75 copies/mL), untreated HIV non-controllers (n = 10, viral load >2000 copies/mL), immunologic non-responders (viral load <75 copies/mL on effective ART, CD4 cell count <350 cells/μL, n = 34), immunologic responders (viral load <75 copies/mL on effective ART, CD4 cell count >500 cells/μL, n = 11). Histologic methods were used to measure the level of collagen in lymphoid aggregates (LA) and the size of the CD4 T cell populations. We also used in situ hybridization to quantify cells expressing HIV RNA in the rectal tissues.
Results: The amount of collagen in LA (lymph tissue) of rectum was higher in all groups of HIV+ subjects compared to uninfected subjects (p = 0.0013 for controllers [p = 0.0090 for the elite subgroup], p = 0.0044 for the non-controllers, and p = 0.0155 for those on ART). Importantly, we found evidence for ongoing virus production by in situ hybridization in 4% controllers, 25% of immunologic non-responders, and 44% of responders. The single individual with normal lymphoid architecture was the patient thought to be cured of HIV infection, i.e., the "Berlin Patient," who had no lymph node or GALT HIV RNA, normal levels of collagen and normal CD4 T cell levels.
Conclusions: Tissue fibrosis in GALT is persistent despite long-term control of HIV by immunologic or therapeutic means. The observation that HIV RNA expression is often detected in these tissues even among controllers and among ART suppressed patients suggests that persistent virus production may contribute to inflammation and immune activation that ultimately leads to tissue fibrosis. The one case of completely normal lymphoid architecture in the individual thought to be cured of HIV is consistent with this conceptual model. Strategies to fully suppress virus replication in tissues may result in reversal of inflammatory damage and more complete reconstitution of immunity.
SLIDE CONCLUSIONS: "Elite and viremic controllers have surprisingly high levels of collagen deposition in GALT lymphoid tissues. The presence of ongoing low-level virus production & increased immune activation suggests that even this amount of virus production is sufficient to sustain fibrotic damage to lymphatic structures"
---------------------------------------
Prospective ART of Asymptomatic HIV+ Controllers
Hiroyu Hatano from the Univ of Calif SF presented
CONCLUSIONS
In this first prospective study of ART initiation in HIV-infected controllers, 24 weeks of ART was safe & well-tolerated. Despite being able to maintain very low plasma HIV RNA levels in the absence of ART, controllers had readily measurable levels of HIV RNA and DNA in GALT. ART initiation in controller led to significant decreases: ultrasensitive plasma RNA, rectal cell-associated RNA and immune activation (blood & rectum)
FUTURE DIRECTIONS
This was a small pilot study with a hteerogenous group of controllers, but even in the 4/16 controllers with pre-ART plasma RNA <40 copies/ml there was a significant decrease in ultrasensitive plasma RNA & similar reductions in immune activation. Since immune activation (%CD38+HLA-DR+ CD* T cells) is less predictive of morbidity/mortality than plasma biomarkers we will be looking at biomarkers in this group (d-dimer, IL-6, sCD14) and flow-mediated vasodilation (FMD), which is a predictor of CVD.
CONCLUSIONS
HIV replication persists in controllers & contributes to a chronic inflammatory state which may have downstream clinical consequences such as accelerated arthreosclerosis, so Antiretroviral therapy should be considered for controllers.
HIV-infected Controllers
· HIV-infected "controllers" are individuals who are able to maintain low levels of plasma RNA in the absence of ART
· Controllers have
- Stable low-level viremia (Hatano, JVI 09, Pereya JID 09, Learmont, NEJM 09)
- Elevated levels of T-cell activation (Hunt, JID 08 and PloS One 11)
- Increased artherosclerosis (Hsue, AIDS 09, Pereya, AIDS 12)
· However, the degree to which viral replication contributes to these outcomes is not known
· Controllers have higher levels of immune activation compared to ART-suppressed indivuduals (Hunt, JID 08)
· Approximately 10% of controllers appear to progress immunologically despite maintaining low plasma RNA levels (Hunt, JID 08)
- In one retrospective study, controllers who initiated ART for clinical reasons had blunted CD4 recovery (Okulicz, CID 10)
Study Objectives
In a prospective, open-label pilot study:
- To treat controllers with ART for 24 weeks
- To examine the effects of ART on HIV RNA/DNA and host immune responses in controllers
Study Design
16 asymptomatic controllers were enrolled, HIV+, had not been on HAART, and had a viral load <1,000 copies/ml for >1 year.
They received open-label raltegravir+TDF/FTC (Truvada) for 24 weeks.
Blood was collected about every 4 weeks. 13/16 subjects also underwent colorectal biopsy at weeks -2, week 6, and week 22.
Study Measurements
Primary Endpoints
· Ultrasensitive plasma RNA (TMA and SCA)
· HIV antibody (detuned EIA, LS-VITROS)
· Cell-associated RNA (blood & rectum)
· HIV DNA (blood & rectum)
· Immune activation (blood & rectum)
- % CD38+HLA-DR+ CD+ and CD8+ T cells
· HIV-specific responses (blood & rectum)
- % Gag-specific IFNg+IL-2+ CD4+ and CD8+ T cells

RESULTS
- CD4 T-cell Counts Did Not Increase Significantly with ART
- Controllers had Significant Decrease in Ultrasensitive Plasma RNA with ART (p<0.001 at weeks 4, 12 & 24)
- Controllers had Significant Decrease in HIV antibody Levels with ART starting at week 12 sustained at week 24 (week 4 p=0.90, wk 12 p<0.001, week 24 p<0.001)
- No Significant Decrease in Cell-Associaed RNA or Proviral DNA with ART (blood)
- Controllers had Significant Decrease in Rectal RNA with ART, but no decrease in rectal DNA except perhaps a trend towards a decrease at week 22. Decrease in rectal RNA at week 22: -0.61 log10 CD4+ (p=0.01)
HOW DID IMMUNOLOGICAL PARAMETERS CHANGE WITH ART?
As you can see from previous research (Hunt et al, PLoS One 2011), HIV controllers had higher immune activation than HIV-negs. As well as previously mentioned, controllers have accelerated atherosclerosis (Huse et a, AIDS 2009; Pereya et a, AIDS 2009)
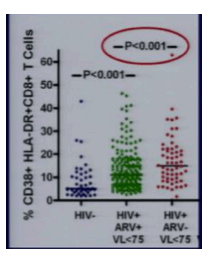
Controller had Significant Decrease in Immune Activation with ART (blood), both CD4 & CD8 (% CD38+HLA-DR+ CD4+ T cells, % CD38+HLA-DR+ T cells (blood)
Decrease in T cell activation at week 24:
CD4 activation: -1.9% (p<0.001)
CD8 activation: -9.0% (p<0.001)
Controllers had Significant Decrease in Markers of Immune Dysfunction with ART (blood)
Decrease in % PD1 at week 24:
%PD1+CD4: -1.6% (p=0.04)
%PD1+: -4.5% (p<0.001)
Controllers Did Not note Significant Decrease in CD4 Activation in the gut (%CD38+HLA-DR+ CD4 T cells (GALT), But did see in Controllers Significant Decrease in Rectal CD8+ T Cell Activation with ART when gut biopsies were done at week 6 (p=0.0004) and at week 22 (p=0.01)
%CD38+HLA-DR+ CD8+ T cells (GALT: Decrease in Rectal T cell activation at week 22: rectal CD8 activation: -12.2% (p=0.01)
No Significant Decrease in HIV-specific T cell Responses with ART (blood)
Log10 % Gag-specific IFNg+IL-2+ CD+ & CD8+ T cells (blood)
No Significant Decrease in Rectal HIV-specific T cell Responses with ART
Log10 % Gag-specific T Total CD4+ & CD8 T cells (GALT)
What about the 4/16 "Elite Controllers who had VL<40 c/ml at baseline??
"Elite" Controllers had Significant Decrease in Ultrasensitive Plasma RNA with ART
If you look at slide you will see the subjects with detectable RNA had declines but those with undetectable RN remained about the same.
"Elite" Controllers had Significant Decrease in HIV Antibody Levels with ART
"Elite" Controllers had Trends Towards Decrease in Immune Activation with ART in both blood and the rectum
Decrease in T cell activation at week 22:
CD8 activation (blood): -6.0% (p=0.091)
CD8 activation (rectum: -24.0% P=0.11)
|
| |
|
 |
 |
|
|