 |
 |
 |
| |
Cardiovascular-related Deaths in HIV-infected Patients between 2000 and 2010 - The ANRS EN20 Mortalite 2010 Survey
|
| |
| |
Reported by Jules Levin
CROI 2013
Sandrine HENARD 1, Caroline ROUSSILLON 2,3, Fabrice BONNET 2,4, Audrey TAIEB 2,3, Patrice CACOUB 5, Dominique SALMON 6, Eric ROSENTHAL 7, Philippe MORLAT 2,4, Genevieve CHENE 2, 3,4, Thierry MAY 1 and the ANRS EN20 Mortality 2010 Study Group
1 CHU Nancy Brabois, Nancy; 2 Univ. Bordeaux, Bordeaux; 3 INSERM U897, Bordeaux; 4 CHU de Bordeaux, Bordeaux; 5 Hopital La Pitie-Salpetriere, Universite Paris 6, Paris; 6 Hopital Cochin, Universite Paris 5, Paris; 7 CHU de Nice, Universite de Nice-Sophia Antipolis
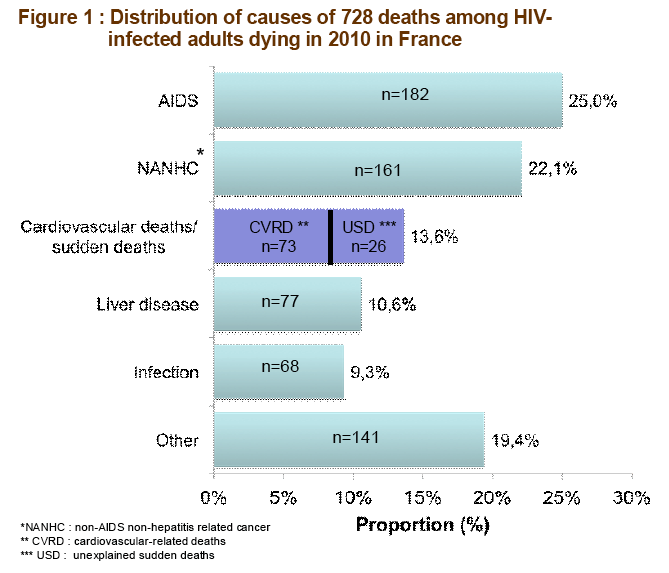
from Jules: deaths - AIDS 25%, nonAIDS nonHepatitis cancers 22%, liver disease 10.6%, infection 9.3%, other 19.4%
DISCUSSION AND CONCLUSION
The proportion of CVRD increased regularly between 2000 (8%) and 2010 (14%), and became the third most frequent cause of
mortality among HIV-infected patients. This increase is partially explained by the inclusion of the unexplained sudden deaths.
The frequency of traditional cardiovascular risk factors (smoking, diabetes, hyperlipidemia, high blood pressure, age > 50 years)
among HIV patients may contribute deeply to this evolution. Additionally, duration of antiretroviral treatment could help to explain
this trend.
This result emphasized the need to improve management of HIV-infected patients receiving antiretroviral treatment, especially
reinforcing prevention initiatives against cardiovascular risk factors.
ABSTRACT
Background: The objective of this study was to describe cardiovascular-related deaths (CVRD) that occurred in France in 2010 among HIV-infected adults, to compare them to other causes of deaths notified in HIV-infected patients and to evaluate their evolution since 2000 in the three French national surveys describing the causes of death in HIV-infected patients in 2000, 2005 and 2010.
Method: A national sample of clinical sites involved in the management of HIV infection in France notified HIV-infected patientŐs deaths. The causes of death were documented using a standardized questionnaire similar to the one used in the two previous national surveys.
Results: In 2010, the 90 participating sites notified 728 deaths; AIDS events (25%) and non-AIDS malignancies (22%) were the two
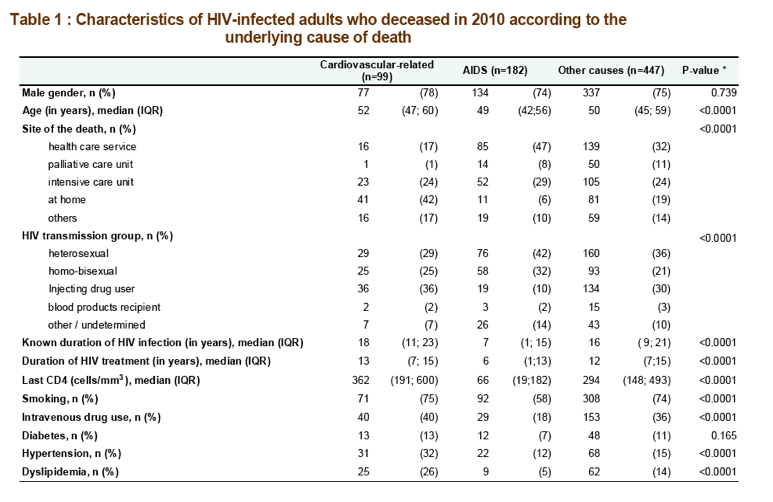
leading causes, followed by CVRD (14 %; n=99). Median age of patients with CVRD was 52 years (vs 50 for other causes, p=0.02), 78% were men (vs 75%; p=0.53), 46% died at hospital (vs 72%, p<0.0001). Median duration of HIV infection in patients with CVRD was 18 years (vs 14, p<0.0001), and median duration of antiretroviral (ART) treatment was 13 years (vs 11, p=0.007). Last CD4 cell count was >500/mm3 in 30% (vs 18%, p=0.004) and last plasma HIV-RNA was <500 copies/mL in 82% (vs 64%, p=0.004). Seventy two percent of CVRD were smokers (vs 64%, p=0.26); 31% had hypertension (vs 14%, p<0.0001), 25% dyslipidemia (vs 11%, p=0.0001) and 13%
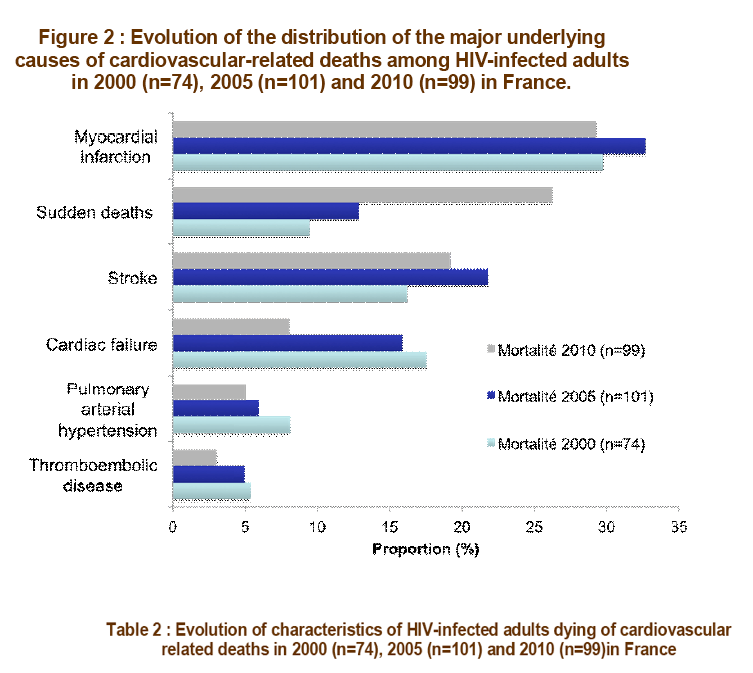
diabetes (vs 9%, p=0.27). Among the 99 CVRD, 29 (29%) were due to heart attack infarction, 26 (26%) were sudden deaths, 19 (19%)
were due to stroke, 8 (8%) to cardiac failure , 5 (5%) to pulmonary arterial hypertension, 5 (5%) to arterial or deep venous thrombosis.
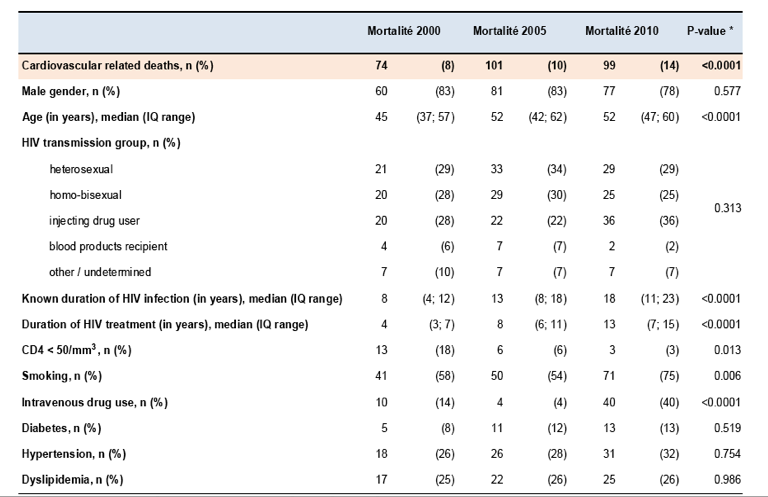
Proportion of CVRD increased from 8 % [2000], 10% [2005] to 14% [2010] (p<0.0001).
From 2000 to 2010, median age (45 years vs 52 for other causes, p<0.0001), proportion of patients with a last available CD4 cell count >500/mm3 (19% vs 22%, p=0.70), median duration of HIV infection (8 years vs 17, p<0.0001), median duration of ART treatment (4 years vs 12 p<0.0001) and proportion of smokers (58% vs 75%, p=0.03) regularly increased.
Conclusion: In 2010, cardiovascular diseases became the third most frequent cause of mortality among HIV-infected patients. Ageing of the HIV population, increasing exposition to high blood pressure and dyslipidemia, and the duration of ART may explain this trend. Prevention initiatives, particularly in patients on long-term therapy, have to be reinforced.

|
| |
|
 |
 |
|
|