| |
As Hepatitis C Spreads, Scotland Steps In: HCV Action Plan by Scotland
|
| |
| |
(Wall St Jnl article published May 16 2013 follows this brief info & links to the Scottish govt HCV program)
-------------------------------------------------------
Hepatitis C Action Plan for Scotland: Phase II: May 2008 - March 2011, Scottish
Executive's first Hepatitis C Action Plan: "One of the other very strong messages that came out of the consultation was that without substantial new resources, it will not be possible to adequately address the Hepatitis C epidemic in Scotland. The Scottish Executive has heard this message, and as a first step, has allocated 4m to NHS boards over the two-year period of this Action Plan to support the actions described here."
http://www.scotland.gov.uk/Publications/2008/05/13103055/0
www.scotland.gov.uk
Publications
2008
May
Hepatitis C Action Plan for Scotland: Phase II: May 2008 - March 2011
Publications > 2008 > May
May 19, 2008 - the report on hepatitis c action plan phase ii. ... Hepatitis C Action Plan for Scotland: Phase II: May 2008 - March 2011
In 2004, the Scottish Government recognised that "Hepatitis C is one of the most serious and significant public health risks of our generation". 1 By December 2006, Health Protection Scotland ( HPS) estimated that 50,000 persons in Scotland had been infected with the Hepatitis C virus and that 38,000 were chronic carriers (Figure 1). 2,3
Following an extensive consultation in 2005, the Health Minister and Chief Medical Officer launched Scotland's Action Plan for Hepatitis C in September 2006. 10
Its aims are:
· To prevent the spread of Hepatitis C particularly among IDUs.
· To diagnose Hepatitis C infected persons, particularly those who would most benefit from treatment.
· To ensure that those infected receive optimal treatment, care and support.
Phase II covers the three years 2008/09, 2009/10 and 2010/11. For each of its actions the following have been identified: desired outcome(s), performance measures to gauge progress in achieving the desired outcome(s), timescales, the lead organisation(s) accountable for delivering the action and key network(s) to support the lead organisation(s) ( Appendix 7).
The actions are categorised into those for i) Testing, Treatment, Care and Support, ii) Prevention, iii) Information Generating and iv) Co-ordination activities
The Action Plan is designed to improve all services applicable to the prevention of, and diagnosis and care of persons with, Hepatitis C, ranging from those that provide education to young people in schools about the dangers of injecting drug use and Hepatitis C to the treatment of infected persons with antiviral drugs and the associated social support required to support them and their families through what, often, is a challenging journey.
In the context of Hepatitis C being a condition which affects, mainly, people who are vulnerable and marginalised, the Action Plan recognises the crucial role of the voluntary and local authority sectors in providing education, training and social support services and the huge opportunity for Hepatitis C-related prevention, diagnosis and treatment in Scotland's prisons.
--------------------------------------------
As Hepatitis C Spreads, Scotland Steps In
Wall St Jnl May 16 2013
By JEANNE WHALEN
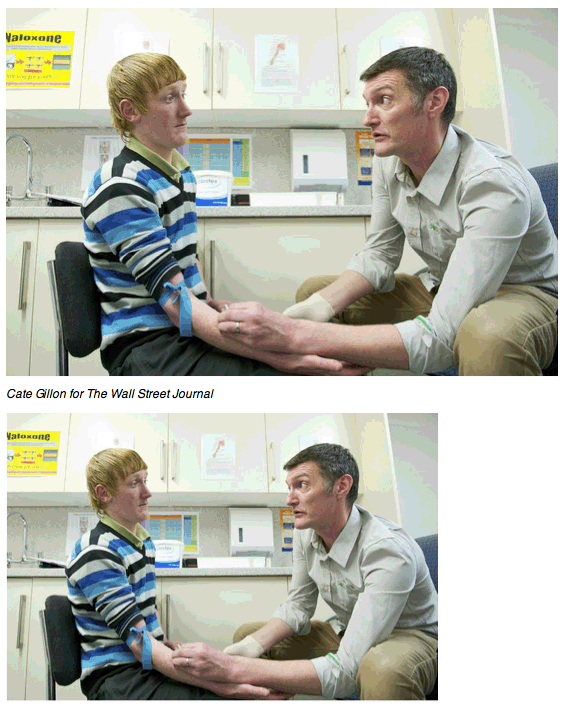
Brian Stephens, right, a nurse in Dundee, takes blood from a patient who did not develop hepatitis C.
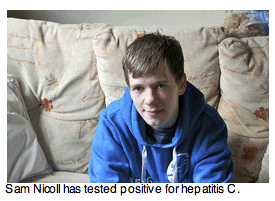
DUNDEE, Scotland-Sam Nicoll, an unemployed laborer with a history of heroin use in this down-and-out city, has recently been released from prison. He's just become a father. And on a recent morning, he ran out of injection needles.
But a nurse here, Brian Stephens, wants the 24-year-old to focus on a different problem: hepatitis C.
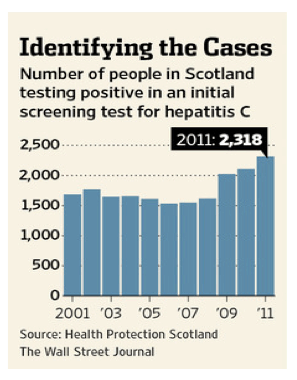
Mr. Nicoll recently took a blood test for the virus at a local needle exchange, and it came back positive. In most parts of the world, he wouldn't be diagnosed or considered for treatment. Few countries conduct widespread testing of injection drug users or offer them medication for hepatitis C, in part because they are considered too unreliable to turn up for appointments or to stick to the costly, monthslong treatment regimen.
Scotland, however, is ignoring conventional wisdom and making a bold push to control a virus that may be one of the biggest ticking time bombs in medicine. Hepatitis C kills about 350,000 people a year globally, and in many Western countries it infects far more people than HIV. The disease can lead to cirrhosis or cancer of the liver and is the leading cause of liver transplants in many countries.
Yet because the virus often strikes injection drug users, the homeless and other hard-up populations, efforts to tackle the problem have lagged behind, health experts say. While hepatitis C now kills more Americans each year than HIV does, the U.S. Centers for Disease Control and Prevention spends only about $30 million a year on prevention of viral hepatitis, compared with almost $800 million for HIV.
For its part, Scotland, with a population of only five million, has launched a 100 million (about $150 million) program, running from 2008 to 2015, to diagnose and treat hepatitis C, regardless of the patient's history. Medication alone can cost anywhere from $10,000 to $40,000 per patient.
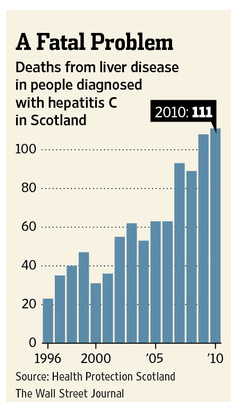
Because Scotland was hit with a wave of hepatitis C in the 1980s and it can take 20 years or more for infections to seriously damage the liver, the country is "just at the moment beginning to see this increase in end-stage liver disease," says David Goldberg, head of Health Protection Scotland's hepatitis C and HIV programs and professor of public health at University of Glasgow. "That clearly is going to have a major impact on demand for liver transplants over the next decade."
The country's taxpayer-funded health system is scrambling to find and treat infections in all hepatitis-prone communities, including Pakistani immigrants and people who received blood transfusions before the virus was discovered in 1989. But it is mostly focusing on current and former injection drug users, who account for about 90% of infections here.
Cities such as Dundee and Edinburgh-setting of the heroin-drenched 1996 film "Trainspotting"-have been particularly hard hit by injection drug use since an economic downturn in the 1980s. Within the European Union, Scotland has one of the highest reported prevalence levels of injection drug use, according to the European Monitoring Centre for Drugs and Drug Addiction.
Early results of the Scottish program are promising. About half of the 38,000 Scots estimated to have been chronically infected have now been diagnosed, compared with 39% in 2007. Of those, about 1,100 new patients a year are receiving treatment, nearly triple the number from 2007. Dr. Goldberg says the aim is to reach 2,000 new patients a year, which should help prevent up to 5,200 cases of cirrhosis by 2030.
Tackling hepatitis C is a difficult assignment. It typically is spread when an infected person's blood enters another person's body, as often happens when drug users share needles. According to the U.K.'s National Health Service, the virus can also be found in some other body fluids, including saliva and semen, but this is far less common, making sexual transmission more rare than it is with HIV.
Because symptoms often don't surface until decades after infection, many people don't know they are infected.
To find infections in current drug users, Scotland is blanketing needle exchanges with simple finger-prick diagnostic kits. After identifying people with infections, many parts of Scotland try to start weaning them off heroin before offering hepatitis C medication. The typical approach is to prescribe methadone, a synthetic opiate that can help reduce heroin cravings, and wait for the patient to gain some stability, says John Dillon, a doctor in Dundee who helps run the hepatitis C program, which is staffed with about 85 doctors and nurses.
But Dundee and other regions have started treating drug users without necessarily trying to stabilize them on methadone first. They are motivated by research from University of Bristol, London School of Hygiene and Tropical Medicine and other institutions suggesting that if just 20 out of 1,000 active injection drug users are treated each year, it could stop them infecting others and reduce the rate of hepatitis C prevalence by nearly 30% in 10 years.
Doing that requires a ton of support, says Mr. Stephens, 41, the nurse at the hepatitis C program in Dundee. But for many, it may be years before they are ready to quit their drug habit, he says. "And how many people will they have infected in that time?"
Much of the program involves sending nurses like him out into the field. A 16-year veteran in nursing, he is known for going to extremes to stay in touch with patients, sometimes phoning them many times to remind them to turn up for appointments. He gives them his cellphone number, answers their calls on weekends, helps them inject the weekly interferon shots they need to kill the virus and sometimes spends hours at needle exchanges and methadone clinics waiting in vain for them to appear.
On a recent morning, Mr. Stephens met with Mr. Nicoll, who had come to a needle exchange program for a new set of syringes. Mr. Stephens invited him into a private room to discuss the results of the blood test he had taken at the exchange about seven months previously, which indicated that he probably had the hepatitis C virus. Mr. Nicoll had missed several appointments to return for a second test needed to confirm the infection. "I've been quite scared to come back," he acknowledged.
Mr. Stephens seized the moment and drew the blood on the spot, explaining what treatment would involve. Clutching a small bag of syringes, Mr. Nicoll mentioned that his life was about to get more hectic: "I've got a baby daughter coming. She's due soon."
About two weeks before meeting Mr. Stephens, Mr. Nicoll had started taking methadone in an effort to tame his drug habit. But like many methadone recipients-particularly in the early stages of treatment-he was continuing to use heroin. Mr. Stephens said that wouldn't disqualify him from hepatitis C treatment. "If someone is continuing to use heroin and they continue to come to appointments, we don't really care. We'll go ahead and treat them anyway," he said. (In a subsequent interview, Mr. Nicoll said he had stopping using heroin, which Mr. Stephens said was confirmed in a urine test. The two are awaiting more blood test results before deciding on the next step in his hepatitis treatment.)
Mr. Stephens said he wound up specializing in hepatitis C after a London surgeon once told him: "Whatever you do, get into hepatitis, because it's going to be huge." The work takes its own form of patience: At a nearby methadone clinic that afternoon, Mr. Stephens met with George Nelson, a 44-year-old addict who was successfully cured of hepatitis C a few years ago, only to find recently that he had reinfected himself through risky drug use.
"I remember getting cleared last time and saying, 'I'll never do that again,'" Mr. Nelson told Mr. Stephens. "For 14 months I was clean. Then I put myself at risk again."
Many countries don't treat active drug users or patients taking methadone because of this risk: they fear the money and effort will be wasted if the person continues using illicit drugs and gets reinfected. "There's been an argument, if you have constrained resources, who would you treat first? Obviously not drug users. But actually there's an argument that you should treat them first," says Charles Gore, president of the World Hepatitis Alliance in London. In Scotland and many places, injection drug use is by far the biggest source of the virus's transmission. Stopping that transmission is "a way to turn off the tap, and then we can empty the pool," Mr. Gore says.
In a recent study, University of Dundee analyzed treatment results for 291 patients in the region, comparing outcomes for people who had never injected drugs to those of active and former users. They found that 61% of noninjection-drug-users achieved a sustained virological response, or SVR, the clinical term for a cure. About 55% of former users and 47% of active users obtained an SVR, the study showed. The authors concluded that active injection drug use "is not a barrier to treatment or a successful achievement of SVR."
In the U.S., few doctors offer hepatitis C treatment to people taking drugs or methadone, says Michael Ninburg, executive director of the Hepatitis Education Project in Seattle. There are also few needle exchanges or methadone clinics in many communities, and even those that do exist don't typically test people for hepatitis C. John Ward, director of the CDC's viral hepatitis division, says the disease is simply "underrecognized, undermanaged and undertreated."
Still, the Scottish approach is being tried in a few places.
Diana Sylvestre, an assistant clinical professor of medicine at University of California, San Francisco, runs a nonprofit clinic in Oakland that treats many people with drug addictions. When she started the clinic 15 years ago, "it became apparent hepatitis C was a huge problem," she says. She started out treating people who had achieved some stability in their lives while taking methadone, later branching out to addicts in more of a "state of disarray," she says. The clinic conducts blood tests and doles out medicine at weekly meetings that also include lunch and hepatitis C education sessions.
"We find that some people you would never predict are able to organize themselves around this schedule," she says, adding that "virtually 100%" of patients who start treatment complete it, and that 80% to 85% are cured.
The lack of medical insurance among many U.S. drug users makes it hard to tackle the hepatitis C problem in a comprehensive way, says Brian Edlin, an associate professor at Weill Cornell Medical College in New York who treats injection drug users for hepatitis C.
Indeed, in a recent study he led to evaluate hepatitis C treatment in active drug users, some of the patients didn't have health insurance, Dr. Edlin says. He provided free care to everyone in the study and helped eligible patients get enrolled in Medicaid to cover the cost of medication. For those who weren't eligible, he obtained free drugs from manufacturers. He also offered mental-health and substance-abuse treatment to anyone who wanted it. Overall, 72% of the patients were cured of hepatitis C, a result he called "very successful." Next he is aiming to recruit up to 200 injection drug users for a larger trial that will more rigorously test the benefits of treatment.
"Doctors raise legitimate uncertainties about treating this population that need to be addressed through research," Dr. Edlin said.
In Dundee, Mr. Stephens and his colleagues are also attempting to enroll injection drug users in a similar study. To encourage them to sign up, they are offering participants a regular supply of high-protein drinks and vouchers to buy food at supermarkets. That is an incentive because "heroin users don't eat very well," Mr. Stephens says. "They spend most of their money on drugs."
Still, recruitment so far has been tough. One young woman he was hoping to enroll didn't turn up for a meeting at the needle exchange. Later, he learned she was due in court on charges she had assaulted a shopkeeper after she had been caught stealing. He ultimately tracked her down and enrolled her in the study. If she goes to prison, he says, "we'll continue her treatment" there.
Meanwhile, Mr. Stephens says he has seen anecdotal evidence that current and recent heroin users can make it through treatment. One patient recently cured, 35-year-old Leanne Petrie, took heroin for 16 years before quitting in late 2011. In an interview, she said she tested positive for hepatitis C around the age of 25 but didn't seek treatment for years.
In 2010, while living in the Scottish county of Fife, she was taking methadone to try to withdraw from heroin, and attending hepatitis C support meetings to learn about treatment. But because she was drinking heavily, her substance-abuse counselor cut off her methadone, which she says prompted her to drink more-about a bottle of vodka a day. She was also still dabbling in heroin.
In 2011, she says she got involved with a violent man who also took heroin. In December 2011, he burned her hand with a cigarette and wrecked her apartment, she says. A few days later, she took an overdose of sleeping pills. "I felt I couldn't get out," she says.
She woke up in the hospital, and, at the encouragement of her family, decided to move to Dundee to say with her cousin. She stopped drinking and taking heroin, and in January 2012, sought treatment for hepatitis C. In the middle of her treatment, she had to leave her cousin's house and stay in a homeless shelter for three months, but she eventually got an apartment from social services. She completed her treatment in November.
Seeing progress with her hepatitis C treatment helped her cope with the instability in her life and stay off drugs, she says. "Since I moved to Dundee I've achieved a lot," she says. "When you see the treatment is working, it helps you keep going."
|
|
| |
| |
|
|
|