| |
Vegetarian diet linked to longer life, less CVD
|
| |
| |
Download the PDF here
Download the PDF here
from Jules: the Editorial below says "The study by Orlich and colleagues1 provides additional evidence that vegetarian diets are associated with improved health outcomes, including all-cause mortality. The study is a well-done, prospective cohort study of more 70 000 Seventh-Day Adventists demonstrating a 12% reduction in all-cause mortality in vegetarians. Vegetarian diets also were associated with reductions in cardiovascular mortality and several other categories of cause-specific mortality.", but then goes on to discuss the limitations of the study. However we have seen many other diet study like that with the Mediterranean Diet and how that has been helpful in delaying disease & death. So particularly in HIV+ individuals who face challenges of increased rates of comorbidities and particularly for older/aging HIV+ individuals over 50 and even moreso for those over 55 & 60, diet and exercise remain a major intervention & preventative step individuals can take.
from paper below ...."These results demonstrate an overall association of vegetarian dietary patterns with lower mortality compared with the nonvegetarian dietary pattern. They also demonstrate some associations with lower mortality of the pesco-vegetarian, vegan, and lacto-ovo-vegetarian diets specifically compared with the nonvegetarian diet.
Some associations of vegetarian diets with lower cardiovascular mortality and lower noncardiovascular, noncancer mortality were observed. Vegetarian diets have been associated with more favorable levels of cardiovascular risk factors,17,22- 25,36- 37 and nutrient profiles of the vegetarian dietary patterns suggest possible reasons for reduced cardiovascular risk, such as lower saturated fat and higher fiber consumption.38 Analysis within the non-CVD, noncancer category revealed notable reductions in mortality with underlying cause classified as endocrine or renal (diabetes mellitus and renal failure, in particular). These apparent protective associations seem consistent with previously published findings showing an association of vegetarian diets with reduced risk of incident diabetes25 and of prevalent diabetes, hypertension, and metabolic syndrome.21,23- 24"
June 11 2013, the heart.org
Loma Linda, CA - In a large observational study of generally middle-aged American Seventh-day Adventists, the vegetarians in the group-ranging from vegans to those who ate meat once a week-were 12% less likely to die within six years than their meat-eating peers [1]. Does this mean everyone should forgo eating meat? Not so fast, experts caution, pointing to study limitations. But it does add support for following a "heart-healthy" diet.
The Adventist Health Study 2 was published online June 3, 2013 in JAMA Internal Medicine.
According to lead author Dr Michael J Orlich (Loma Linda University, CA), "This research gives more support to the idea that certain vegetarian dietary patterns may be associated with reduced mortality and increased longevity" and can be used to guide food choices.
However, in an accompanying editorial [2], Dr Robert B Baron (University of California, San Francisco) points out since it was a observational study, cause-and-effect conclusions cannot be drawn from it, and it was based on a one-time questionnaire. He urges clinicians counseling patients to be less focused on a vegetarian vs nonvegetarian diet and rather to look to the broader goal of improving the diet.
Asked to comment, Dr Robert H Eckel (University of Colorado Anschutz Medical Campus, Aurora) concurs. "We need to put this study into perspective. Is a vegetarian diet heart healthy? Probably yes. Should people convert to a vegetarian diet based on this study? Absolutely not. I think they need to look at their overall diet and make sure it is consistent with what we know about diet and heart disease," he told heartwire.
Cut out meat and live longer?
Previous studies found that eating nuts, fruit, salads, fiber, and polyunsaturated fats or following a "healthy" or vegetarian or Mediterranean diet was linked with longer life, whereas eating red or processed meat upped mortality, the authors report. The first Adventist Health Study of about 30 000 Seventh-day Adventists living in California in the 1970s found a link between vegetarianism and lower all-cause mortality. But the European Prospective Investigation into Cancer and Nutrition-Oxford (EPIC-Oxford) cohort study did not find this association.
To investigate this, the researchers examined data from 73 308 Seventh-day Adventist men and women over age 25 who were living in the US from 2002 to 2007. The study participants had a mean age of around 57 years, and about 66% were women.
Based on their replies to questions about their consumption of 200 foods over the past year, the participants were classed into the following dietary patterns:
· Vegan: Ate eggs, dairy products, fish, and meat less than once a month (n=5548; 7.6%).
· Lacto-ovo-vegetarian: Ate eggs and dairy products once a month or more; ate fish and meat less often (n=21 177; 28.9%).
· Pescovegetarian: Ate fish once a month or more; ate meat less often (n=7194; 9.8%).
· Semivegetarians: Ate meat once a month or more; ate fish or meat no more than once a week (n=4031; 5.5%).
· Nonvegetarians: Ate fish or meat more than once a week (35 359; 48.2%).
Over a follow-up of a mean of 5.79 years, 2570 participants died.
Compared with nonvegetarians, the hazard ratio (HR) for all-cause mortality for all vegetarians combined was significant: 0.88 (95% CI 0.80-0.97). The HR for all-cause mortality ranged from 0.81 to 0.92 in the different vegetarian types and was significant only for lacto-ovo-vegetarians and pescovegetarians.
Some vegetarian diets were significantly associated with lower mortality from CVD, ischemic heart disease, renal disease, and endocrine disease (diabetes), but not from cancer. The associations were larger and more likely to be significant in men than in women.
The effect of a vegetarian diet in this study was "pretty modest," Eckel said. The more extreme diet-the vegan diet-did not appear to add additional benefits.
Most nutritional experts "agree that diets should limit added sugars and sugary drinks, refined grains, and large amounts of saturated and trans fats, [and healthy diets should include] substantial amounts of fruits and vegetables [and] whole grains, legumes, and nuts," Baran writes. "Achieving these goals trumps the more narrow goals of whether to include moderate amounts of dairy, eggs, fish, or even meat."
Eckel agrees. "We need to get away from this 'good food/bad food' " concept, he said. The overall diet is what is important. "Is some red meat or saturated fat in a diet appropriate? I think so. It's just a matter of how much."
-------------------------------
JAMA Intern Med. June 2013
Vegetarian Dietary Patterns and Mortality in Adventist Health Study 2 ONLINE FIRST
Michael J. Orlich, MD; Pramil N Singh, DrPH; Joan Sabate, MD, DrPH; Karen Jaceldo-Siegl, DrPH; Jing Fan, MS; Synnove Knutsen, MD, PhD; W. Lawrence Beeson, DrPH; Gary E. Fraser, MBchB, PhD
ABSTRACT
Importance Some evidence suggests vegetarian dietary patterns may be associated with reduced mortality, but the relationship is not well established.
Objective To evaluate the association between vegetarian dietary patterns and mortality.
Design Prospective cohort study; mortality analysis by Cox proportional hazards regression, controlling for important demographic and lifestyle confounders.
Setting Adventist Health Study 2 (AHS-2), a large North American cohort.
Participants A total of 96 469 Seventh-day Adventist men and women recruited between 2002 and 2007, from which an analytic sample of 73 308 participants remained after exclusions.
Exposures Diet was assessed at baseline by a quantitative food frequency questionnaire and categorized into 5 dietary patterns: nonvegetarian, semi-vegetarian, pesco-vegetarian, lacto-ovo-vegetarian, and vegan.
Main Outcome and Measure The relationship between vegetarian dietary patterns and all-cause and cause-specific mortality; deaths through 2009 were identified from the National Death Index.
Results There were 2570 deaths among 73 308 participants during a mean follow-up time of 5.79 years. The mortality rate was 6.05 (95% CI, 5.82-6.29) deaths per 1000 person-years. The adjusted hazard ratio (HR) for all-cause mortality in all vegetarians combined vs nonvegetarians was 0.88 (95% CI, 0.80-0.97). The adjusted HR for all-cause mortality in vegans was 0.85 (95% CI, 0.73-1.01); in lacto-ovo-vegetarians, 0.91 (95% CI, 0.82-1.00); in pesco-vegetarians, 0.81 (95% CI, 0.69-0.94); and in semi-vegetarians, 0.92 (95% CI, 0.75-1.13) compared with nonvegetarians. Significant associations with vegetarian diets were detected for cardiovascular mortality, noncardiovascular noncancer mortality, renal mortality, and endocrine mortality. Associations in men were larger and more often significant than were those in women.
Conclusions and Relevance Vegetarian diets are associated with lower all-cause mortality and with some reductions in cause-specific mortality. Results appeared to be more robust in males. These favorable associations should be considered carefully by those offering dietary guidance.
The possible relationship between diet and mortality remains an important area of investigation. Previous studies have identified dietary factors associated with mortality. Those found to correlate with reduced mortality include nuts,1- 4 fruit,5- 6 cereal fiber,2 polyunsaturated fatty acids (PUFAs),2 ω-3PUFAs,3 green salad,7 Mediterranean dietary patterns,8- 11 "healthy" or "prudent" dietary patterns,10,12- 13 plant-based diet scores,14 plant-based low-carbohydrate diets,15 and vegetarian diets.4,16- 17 Associations with increased mortality have been found for a high glycemic load,2 meat,6- 7 red meat,18- 19 processed meat,18- 19 eggs,7 potatoes,5 increased energy intake,20 and animal-based low-carbohydrate diets.15
Vegetarian dietary patterns may contain many of the above-listed foods and nutrients associated with reduced mortality while having reduced intakes of some foods associated with increased mortality. Vegetarian dietary patterns have been associated with reductions in risk for several chronic diseases, such as hypertension,21- 22 metabolic syndrome,23 diabetes mellitus,24- 25 and ischemic heart disease (IHD),17,26 which might be expected to result in lower mortality.
Vegetarian diets represent common, real-world dietary patterns and are thus attractive targets for study.
Previous studies of the relationship between vegetarian dietary patterns and mortality have yielded mixed results. In the first Adventist Health Study, a study of 34 198 California Seventh-day Adventists,27 vegetarian dietary patterns were associated with reduced all-cause mortality and increased longevity.4,17 In contrast, the European Prospective Investigation into Cancer and Nutrition-Oxford (EPIC-Oxford) cohort study did not show an all-cause mortality advantage for British vegetarians (among 47 254 vegetarian and nonvegetarian participants),28 and pooled results have shown reductions only for IHD mortality.16
Our objective, in light of the potential benefits of vegetarian diets and the existing uncertainty in the literature, was to evaluate the possible association of vegetarian dietary patterns with reduced mortality in a large American cohort including many vegetarians.
METHODS
STUDY POPULATION
Adventist Health Study 2 (AHS-2) is a cohort of 96 469 Seventh-day Adventist men and women recruited at churches in the United States and Canada between 2002 and 2007.29 Butler et al29 provided a detailed explanation of the cohort formation and characteristics. Written informed consent was obtained from all participants upon enrollment. The study was approved by the institutional review board of Loma Linda University.
Exclusions were applied in the following order: missing data for questionnaire return date, birth date, sex, or race (n = 1702); age younger than 25 years (n = 434); estimated energy intake (not including write-in items) less than 500 kcal/d or more than 4500 kcal/d; improbable response patterns (eg, identical responses to all questions on a page) or more than 69 missing values in dietary data (n = 4961); non-US residents (n = 4108); or history of a specific prior cancer diagnosis (except nonmelanoma skin cancers) or of cardiovascular disease (CVD) (coronary bypass, angioplasty/stent, carotid artery surgery, myocardial infarction, or stroke; or angina pectoris or congestive heart failure treated in the past 12 months) (n = 11 956). After exclusions, there remained an analytic sample of 73 308.
MORTALITY DATA
Mortality data through December 31, 2009, were obtained from the National Death Index. International Statistical Classification of Diseases, 10th Revision (ICD-10) codes for the underlying cause of death were used for causal classification. Unnatural causes of death (ICD-10 letters U, V, W, X, and Y) were considered as censoring events. Deaths associated with IHD were identified as ICD-10 I20-25; CVD deaths, as those starting with the letter I; and cancer deaths, as those starting with the letter C. Noncardiovascular, noncancer deaths were identified as all natural deaths not classified as CVD or cancer deaths. Infectious disease deaths were identified as those starting with the letters A or B; neurologic deaths, the letter G; respiratory deaths, the letter J; renal deaths, the letter N; and endocrine deaths, the letter E. Stroke deaths were identified using the code I60-69; diabetes mellitus deaths, E10-14; and renal failure deaths, N17-19.
DIETARY DATA
Usual dietary intake during the previous year was assessed at baseline by a self-administered quantitative food frequency questionnaire of more than 200 food items. Dietary patterns were determined according to the reported intake of foods of animal origin.
Thus, vegans consumed eggs/dairy, fish, and all other meats less than 1 time/mo;
lacto-ovo-vegetarians consumed eggs/dairy 1 time/mo or more but fish and all other meats less than 1 time/mo;
pesco-vegetarians consumed fish 1 time/mo or more but all other meats less than 1 time/mo;
semi-vegetarians consumed nonfish meats 1 time/mo or more and all meats combined (fish included) 1 time/mo or more but no more than 1 time/wk; and last,
nonvegetarians consumed nonfish meats 1 time/mo or more and all meats combined (fish included) more than 1 time/wk.
For some analyses, the 4 vegetarian categories (vegan, lacto-ovo-vegetarian, pesco-vegetarian, and semi-vegetarian) were combined as "vegetarian."
The food frequency questionnaire was previously validated against six 24-hour dietary recalls for intake of nutrients30 and selected foods/food groups.31 Validity correlations for red meat, poultry, fish, dairy, and eggs were 0.76, 0.76, 0.53, 0.86, and 0.64, respectively, in whites and 0.72, 0.77, 0.57, 0.82, and 0.52, respectively, in blacks.31 Mean duration of adherence to dietary patterns was calculated for respondents to a follow-up questionnaire in which participants were asked to characterize their consumption of meat and dairy products at that time and in previous decades.
COVARIATES
Other variables, all measured at baseline, were as follows (Table 1 footnotes for category specification): sex (dichotomous), race (dichotomous), geographic region (6 levels), personal income (4 levels), educational level (4 levels), marital status (dichotomous), smoking (8 levels), alcohol use (5 levels), exercise (ie, "vigorous activities, such as brisk walking, jogging, bicycling, etc, long enough or with enough intensity to work up a sweat, get your heart thumping, or get out of breath") (5 levels), sleep (3 levels), menopausal status of women (dichotomous), hormone therapy in postmenopausal women (dichotomous), dietary energy (7 levels: <1000 kcal, 1000-1499 kcal,1500-1999 kcal, 2000-2499 kcal, 2500-2999 kcal, 3000-3999 kcal, and ≥4000 kcal), body mass index (calculated as weight in kilograms divided by height in meters squared) (9 levels: <18, 18 to <20, 20 to <23, 23 to <25, 25 to <27, 27 to <30, 30 to <35, 35 to <40, and ≥40). Race was included as a potentially important covariate. Participants self-identified their race/ethnicity in 1 or more of 21 categories. Those self-identifying as black/African American, West Indian/Caribbean, African, or other black were categorized as black for this analysis and all others were categorized as nonblack.
STATISTICAL ANALYSIS
Baseline descriptive statistics were calculated according to the 5 dietary-pattern categories. Means and percentages were adjusted for age, sex, and race by direct standardization using the entire analytic sample as the standard distribution. Age-sex-race standardized mortality rates were computed by dietary pattern. Analyses of mortality were performed using Cox proportional hazards regression with attained age as the time variable and left truncation by age at study entry. Covariates were selected on an a priori basis as likely confounders based on prior studies and suspected relationships. Menopausal status and hormone therapy were represented in models as nested covariates (ie, sex + [sex x menopause] + [sex x menopause x hormone therapy]). Covariates were tested for possible interaction with the diet variable and for suspected interactions between selected covariates. The Cox proportional hazards assumption was evaluated using Schonfeld residuals, log(-log) plots, and attained-age interaction terms. Significant nonproportionality of hazards was present for race and marital status, so attained-age interaction terms for these variables were retained in the models. Residual methods were used to evaluate possible outliers and influential data points; no data points required removal. Multiple imputation of missing values was done for the small amount of missing data in the dietary variables used to calculate vegetarian status and for all covariates; a guided multiple-imputation approach was used when possible,32 as we have evidence that many of the missing dietary data are true zeroes.33 Analyses were performed using commercial software (SAS, version 9.3; SAS Institute, Inc). Guided multiple imputation was performed using R, version 2.13.1 software34 and the Hmisc package.35
DISCUSSION (results follow)
These results demonstrate an overall association of vegetarian dietary patterns with lower mortality compared with the nonvegetarian dietary pattern. They also demonstrate some associations with lower mortality of the pesco-vegetarian, vegan, and lacto-ovo-vegetarian diets specifically compared with the nonvegetarian diet.
Some associations of vegetarian diets with lower cardiovascular mortality and lower noncardiovascular, noncancer mortality were observed. Vegetarian diets have been associated with more favorable levels of cardiovascular risk factors,17,22- 25,36- 37 and nutrient profiles of the vegetarian dietary patterns suggest possible reasons for reduced cardiovascular risk, such as lower saturated fat and higher fiber consumption.38 Analysis within the non-CVD, noncancer category revealed notable reductions in mortality with underlying cause classified as endocrine or renal (diabetes mellitus and renal failure, in particular). These apparent protective associations seem consistent with previously published findings showing an association of vegetarian diets with reduced risk of incident diabetes25 and of prevalent diabetes, hypertension, and metabolic syndrome.21,23- 24
No significant associations with reduced cancer mortality were detected. The heterogeneous nature of cancer may obscure specific diet-cancer associations in analyses of combined cancer mortality, and lack of significance may reflect insufficient power to detect weaker associations at early follow-up. Early analyses of vegetarian dietary patterns and cancer incidence in AHS-2 demonstrated significantly reduced risks of female-specific and gastrointestinal cancers.39
Effects were generally stronger and more significant in men than women. Previous studies40- 42 among Adventists have demonstrated effect modification by sex of the association of vegetarian diets with reduced ischemic heart disease mortality. It is possible that within dietary groups the diets of men and women differ in important ways; however, a recent evaluation38 of the nutrient profile of the dietary patterns in this cohort did not reveal striking differences.
Alternatively, the biological effect of dietary factors on mortality may be different in men and women. Future analysis will evaluate possible effect modification by sex for particular foods or nutrients, which may suggest sex-specific mechanisms.
Strengths of this study include the large number of participants consuming various vegetarian diets; the diverse nature of this cohort in terms of sex, race, geography, and socioeconomic status, enhancing generalizability; the low use of tobacco and alcohol, making residual confounding from these unlikely; the shared religious affiliation of the cohort, which may lead to greater homogeneity across several possible unmeasured confounders, enhancing internal validity; and precise dietary pattern definitions based on measured food intake rather than self-identification of dietary patterns.
This analysis is limited by relatively early follow-up. If dietary patterns affect mortality, they may do so with moderate effect sizes, via complex pathways, and with long latency periods. Early follow-up analysis may thus have bias toward the null, and true associations may remain undetected. Observed mortality benefits may be affected by factors related to the conscious lifestyle choice of a vegetarian diet other than dietary components. Potential for uncontrolled confounding remains. Dietary patterns may change over time, whereas the analysis relies on a single measurement of diet at baseline. Caution must be used in generalizing results to other populations in which attitudes, motivations, and applications of vegetarian dietary patterns may differ; dietary pattern definitions used may not reflect some common uses of these terms.
Further study of the possible association with mortality of specific foods and nutrients that characterize the different diet-pattern groups is a major future goal of the AHS-2 study. Later follow-up may yield more statistically robust results; allow direct comparisons between vegetarian groups and enable subgroup analysis, particularly by race/ethnicity; and allow for analysis by more specific causes of mortality.
The lack of similar findings in British vegetarians28 remains interesting, and this difference deserves careful study. In both cohorts, the nonvegetarians are a relatively healthy reference group. In both studies, the nutrient profiles of vegetarians differ in important ways from those of nonvegetarians, with vegetarians (especially vegans) consuming less saturated fat and more fiber.38,43 It appears that British vegetarians and US Adventist vegetarians eat somewhat differently.44 For instance, the vegetarians in our study consume more fiber and vitamin C than those of the EPIC-Oxford cohort: mean dietary fiber in EPIC-Oxford vegans was 27.7 g/d in men and 26.4 g/d in women compared with 45.6 g/d in men and 47.3 g/d in women in AHS-2 vegans; mean vitamin C in EPIC-Oxford vegans was 125 mg/d in men and 143 mg/d in women compared with 224 mg/d in men and 250 mg/d in women in AHS-2 vegans.38,43 Individuals electing vegetarian diets for ethical or environmental reasons may eat differently from those who choose vegetarian diets primarily for reasons of perceived superiority for health promotion. We believe that perceived healthfulness of vegetarian diets may be a major motivator of Adventist vegetarians. More important, other large cohort studies have linked increased red and processed meat consumption to higher mortality,18- 19,45 and our findings build on this work by demonstrating reduced mortality in those consuming low-meat dietary patterns. Notably, the findings of the present study are similar to those of prior North American Adventist cohorts, demonstrating a consistent association over several decades and replicating prior results in a population with greater geographic and ethnic diversity.46
In conclusion, in a large American cohort, we found that vegetarian dietary patterns were associated with lower mortality. The evidence that vegetarian diets, or similar diets with reduced meat consumption, may be associated with a lower risk of death should be considered carefully by individuals as they make dietary choices and by those offering dietary guidance.
RESULTS
BASELINE CHARACTERISTICS
Among the 73 308 individuals in our analytic sample, 5548 (7.6%) were vegans, 21 177 (28.9%) were lacto-ovo-vegetarians, 7194 (9.8%) were pesco-vegetarians, 4031 (5.5%) were semi-vegetarians, and 35 359 (48.2%) were nonvegetarians. Table 2 presents characteristics of the participants at baseline according to the 5 dietary patterns. Percentages and means were age-sex-race standardized as appropriate. Vegetarian groups tended to be older, more highly educated, and more likely to be married, to drink less alcohol, to smoke less, to exercise more, and to be thinner. The proportion of blacks was highest among pesco-vegetarians and lowest in lacto-ovo-vegetarians. Of postmenopausal women, far fewer vegans were receiving hormone therapy. Mean reported duration of adherence to current dietary pattern (not included in Table 2) was 21 years for vegans, 39 years for lacto-ovo-vegetarians, 19 years for pesco-vegetarians, 24 years for semi-vegetarians, and 48 years for nonvegetarians.
MORTALITY
The mean (SD) follow-up time was 5.79 (1.31) years. During this time, there were 2570 deaths among 73 308 participants, and the overall mortality rate was 6.05 (95% CI, 5.82-6.29) deaths per 1000 person-years. Table 3 gives the age-sex-race standardized mortality rates by dietary pattern. Vegans, lacto-ovo-vegetarians, and pesco-vegetarians had significantly lower mortality rates compared with nonvegetarians.
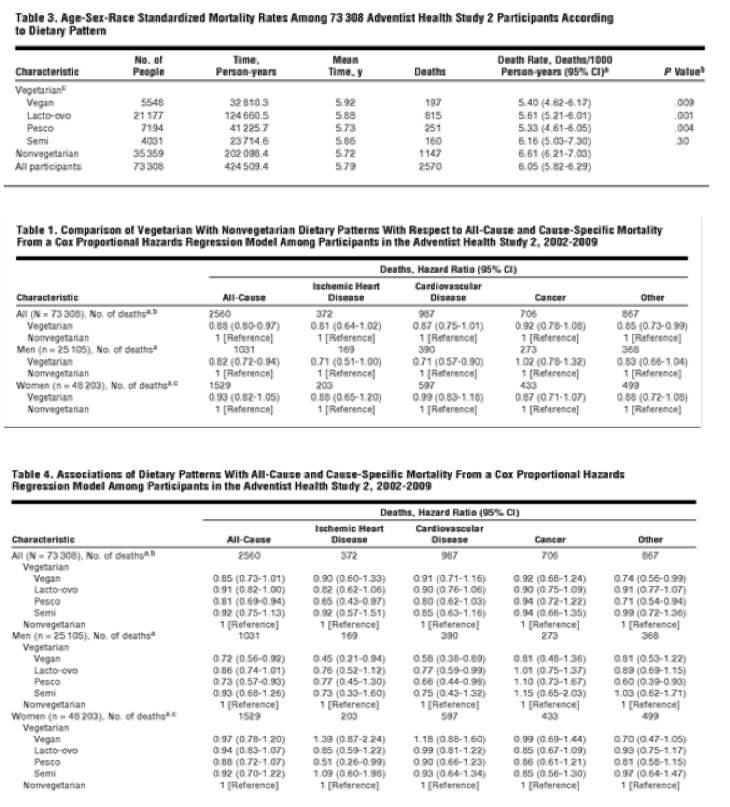
Table 1 reports the comparison of multivariate-adjusted risk of death for all vegetarians combined with that for nonvegetarians. Vegetarians had 0.88 (95% CI, 0.80-0.97) times the risk of all-cause mortality of nonvegetarians. In men, the hazard ratio (HR) was 0.82 (95% CI, 0.72-0.94) and in women, 0.93 (0.82-1.05).
Significantly reduced risk in both sexes combined was also seen for other mortality (ie, non-CVD, noncancer) (HR, 0.85; 95% CI, 0.73-0.99) but not clearly for IHD mortality (0.81; 0.64-1.02), CVD mortality (0.87; 0.75-1.01), or cancer mortality (0.92; 0.78-1.08). For men, CVD mortality (0.71; 0.57-0.90) and IHD mortality (0.71; 0.51-1.00) achieved significance, and other mortality had a notable but nonsignificant reduction (0.83; 0.66-1.04). In women, there were no significant reductions in these causal categories of mortality, although the effect estimates for IHD mortality, cancer mortality, and other mortality were moderately less than 1.0. Results (not included in table) for stroke were, for both sexes combined, HR, 1.10 (95% CI, 0.82-1.47); for men, 0.83 (0.52-1.31); and for women, 1.27 (0.89-1.80).
Table 4 reports the comparison of the multivariate-adjusted risk of death for 4 categories of vegetarians compared with nonvegetarians. Pesco-vegetarians had significantly reduced risk in both sexes combined for all-cause mortality (HR, 0.81; 95% CI, 0.69-0.94), IHD mortality (0.65; 0.43-0.97), and other mortality (0.71; 0.54-0.94); in men for all-cause mortality (0.73; 0.57-0.93), CVD mortality (0.66; 0.44-0.98), and other mortality (0.60; 0.39-0.93); and in women for IHD mortality (0.51; 0.26-0.99). Lacto-ovo-vegetarians had significantly reduced risk in both sexes combined for all-cause mortality (HR, 0.91; 95% CI, 0.82-1.00) and in men for CVD mortality (0.77; 0.59-0.99). Vegans had significantly reduced risk in both sexes combined for other mortality (HR, 0.74; 95% CI, 0.56-0.99) and in men for all-cause mortality (0.72; 0.56-0.92), IHD mortality (0.45; 0.21-0.94), and CVD mortality (0.58;0.38-0.89).
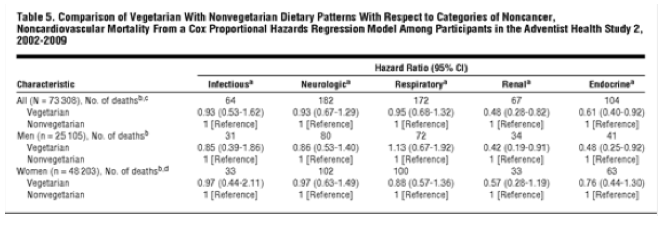
Table 5 presents the results of multivariate-adjusted Cox analyses for several more-specific categories of mortality within the broad "other" mortality of Table 1 (ie, non-CVD, noncancer mortality), comparing all vegetarians with nonvegetarians. In men and women combined, vegetarians had a significantly reduced risk of renal mortality (HR, 0.48; 95% CI, 0.28-0.82) and endocrine mortality (0.61; 0.40-0.92); in men, vegetarians had reduced risk of renal mortality (0.42; 0.19-0.91) and endocrine mortality (0.48; 0.25-0.92); and in women, nonsignificant reductions for both renal mortality (0.57; 0.28-1.19) and endocrine mortality (0.76; 0.44-1.30). Forty of 67 renal deaths were associated with renal failure (for both sexes combined, HR, 0.26; 95% CI, 0.12-0.57; for women, 0.39; 0.13-1.17; and for men, 0.21; 0.07-0.63). Sixty-seven of 104 endocrine deaths were associated with diabetes mellitus (for both sexes combined, HR, 0.53; 95% CI, 0.32-0.89; for women, 0.78; 0.41-1.48; and for men, 0.27; 0.11-0.66).
A sensitivity analysis in which body mass index was added to the model generally had only a modest effect on the results. Overall HRs for vegetarians were then 0.90 (95% CI, 0.82-0.98) for both sexes combined, 0.83 (0.72-0.96) for men, and 0.95 (0.84-1.06) for women. The adjustment for body mass index did not consistently move results toward the null. Mortality results adjusted for body mass index affected statistical significance in the following instances. For all vegetarians combined compared with nonvegetarians: IHD mortality in men (HR, 0.77; 95% CI, 0.54-1.10), endocrine mortality in both sexes combined (HR, 0.71; 95% CI, 0.46-1.09), and diabetes mortality in both sexes combined (HR, 0.65; 95% CI, 0.38-1.11). For specific vegetarian dietary patterns compared with nonvegetarians: vegans, all-cause mortality in both sexes combined (HR, 0.84; 95% CI, 0.72-1.00) and IHD mortality in men (0.50; 0.24-1.06); lacto-ovo-vegetarians, all-cause mortality in both sexes combined (0.92; 0.84-1.02) and CVD mortality in men (0.81; 0.63-1.05); pesco-vegetarians, IHD mortality in both sexes combined (0.69; 0.45-1.05), other mortality in both sexes combined (0.77; 0.60-1.00), CVD mortality in men (0.68; 0.45-1.04), and other mortality in men (0.65; 0.43-1.00). Additional adjustment by dietary energy intake resulted in negligible changes. Formal tests for interaction of the diet variable (vegetarian vs nonvegetarian) with sex revealed significant interaction for CVD mortality (P = .01), but no significant interaction for all-cause mortality or other categories of mortality.
--------------------------------------
Invited Commentary | ONLINE FIRST
Should We All Be Vegetarians?Comment on "Vegetarian Dietary Patterns and Mortality in Adventist Health Study 2"
Robert B. Baron, MD, MS
As a graduate student studying nutrition in the early 1970s, I became a vegetarian (a lacto-ovo vegetarian, to be exact). Early observational studies had already pointed to better health outcomes on meat-free diets. Similarly, early reports suggested that meat production was wasteful and had adverse environmental impacts. The mainstream nutrition community, though, strongly resisted the growing vegetarian movement, often raising concerns about nutritional deficiencies with the most extreme types of vegetarian diets. By the time I was a third-year medical student, I had returned to eating meat, given the lack of vegetarian options in hospital cafeterias. As my clinical training and experience increased, though, I became convinced that patients in any phase of life, and with virtually any medical condition, could safely follow a meat-free diet.
Today, millions of US citizens describe themselves as vegetarians, and hundreds of millions of people around the globe eat meat-free diets. Vegetarian options are increasingly available in US hospitals, restaurants, and social events. But the question remains: Can vegetarian diets improve health outcomes?
The study by Orlich and colleagues1 provides additional evidence that vegetarian diets are associated with improved health outcomes, including all-cause mortality. The study is a well-done, prospective cohort study of more 70 000 Seventh-Day Adventists demonstrating a 12% reduction in all-cause mortality in vegetarians. Vegetarian diets also were associated with reductions in cardiovascular mortality and several other categories of cause-specific mortality.
The study, however, illustrates several challenges in trying to answer the core question of whether vegetarian diets improve health outcomes. Like all observational studies, this one provides associations, not cause-and-effect evidence. Although the authors use state-of-the-art approaches to adjustment for potential confounders, one can never be sure that there are not other factors influencing the association between vegetarian diets and mortality. Recent publication of large randomized trials of different diets and dietary approaches may end reliance on observational studies, which, no matter how well done, have limitations resulting from confounding.2- 3
Another weakness of the study is that it relies on a single measurement of dietary intake at baseline and, as the authors (and my personal anecdote) point out, dietary patterns may change over time. The study also is limited by the great variety of diets consumed by those identified as vegetarians. In addition to vegans and lacto-ovo vegetarians, the study includes as vegetarians those who eat fish (pesco vegetarian) and those who eat fish and nonfish meats monthly but not more than once per week (semivegetarian). Stricter definitions would exclude both of the latter 2 groups as vegetarian.
This variety of dietary intake labeled as vegetarian reflects the challenges of clinical practice. That is, patients who self-identify as vegetarian have not yet provided much information about what they eat. Clinicians need to ask additional questions to identify average intakes of dairy products, eggs, fish, and meat. Moreover, grouping patients into these 4 vegetarian categories provides little information about the quality or quantity of the overall dietary intake. Clinicians, either alone or in conjunction with dietitians, also need to assess intake of total calories, added sugars and sugary drinks, refined grains, salt, saturated and trans fats, alcohol, vegetables, fruits, whole grains, legumes, nuts, and oils. In short, vegetarian diets can represent a wide spectrum of nutrient intake, and it is the clinician's responsibility to help the patient determine the potential health benefits or harms of a particular diet.
For many, the decision about eating a meat-free diet has more to do with religious or ethical beliefs than achievement of beneficial health outcomes. In these settings, clinicians must work within the patient's predefined belief framework to maximize dietary composition, without contradicting the patient's beliefs.
Environmental concerns also have become a significant force in the conversation about dietary choices. A growing body of literature points to the negative environmental impact of meat, particularly meat produced from industrial farm animals. As opposed to animals grazing in pastures, industrial farm animals consume extremely large amounts of feed, water, land, and fossil fuels and are estimated to contribute substantially to water shortages; soil, water, and air pollution; and climate change.4 This may turn out to be a stronger motivation to decreasing meat intake for many than even the potential health benefits.
How then should clinicians advise patients about what to eat? First and foremost, dietary advice needs to be given to patients based on their own dietary history and preferences, their motivation to change their diet, and their clinical circumstances. In each instance, diets with or without meat can be designed to meet clinical goals. For patients with chronic illness, diets become another tool (along with medications and other nonpharmacologic interventions) in the patients' and clinicians' "toolbox" to prevent and treat chronic disease.
For most patients, controlling calories remains the primary nutritional goal. In a society in which weight gain is the norm as we age, preventing weight gain (and improving fitness) remains the primary goal. Although nutrition authorities may disagree about the optimal balance of macronutrients in an ideal diet, and the amount of meat and other specific foods that should be ingested, virtually all agree that diets should limit added sugars and sugary drinks, refined grains, and large amounts of saturated and trans fats. Similarly, virtually all diet recommendations include eating substantial amounts of fruits and vegetables. Most authorities will also agree that diets should include whole grains, legumes, and nuts.
Achieving these goals trumps the more narrow goals of whether to include moderate amounts of dairy, eggs, fish, or even meat. Similarly, debates about how much whole grain or vegetable oil should be included may pale compared with the basic tenets described above. In fact, in much the same way that clinicians learn to master a short list of generic medications that can be used in most common clinical circumstances, clinicians can also learn to develop a "generic" diet that meets nutritional requirements. With minor case-by-case adjustments, the generic diet will serve most patients who seek (or could benefit from) dietary advice. More extreme diets, though, also may confer benefit for specific clinical conditions, including short-term weight loss and as alternatives (or adjuncts) to medications to treat specific conditions.
Our debates about the superiority of one diet over another have not served the public well. It is time to acknowledge the common features of diets associated with good clinical outcomes and to focus our attention on helping patients avoid the intense commercial pressures to eat otherwise.
| |
| |
| |
|
|
|