 |
 |
 |
| |
Outcomes Differ for HIV-Infected Patients Receiving Care at Hospital vs. Community-Based Clinics
|
| |
| |
Reported by Jules Levin
IDWeek/IDSA Oct 2-6 2013, San Francisco, CA
Asher Schranz1, Kathleen Brady2,3, Sara Keller4, Florence Momplaisir5, Joshua Metlay6, and Baligh Yehia3
1New York University, 2Philadelphia Department of Public Health, 3University of Pennsylvania, 4Johns Hopkins University, 5Temple University, 6Harvard University
In conclusion...We found that patients at community-based HIV clinics are predominantly low-income and have public insurance or are uninsured. This is consistent with the mission of many community health centers, which aim to provide a safety net for the underserved.
Our analysis showed that community clinics have significantly higher rates of retention in care. We hypothesize that this stems from the mission, structure and activities of many community health centers, which are targeted towards specific patient populations. Additionally, hospital-based primary care clinics have been shown to have more delays in care due to administrative and logistical issues, and we think that this may contribute to their lower rate of retention.
We also found that patients seen in hospital clinics are more likely to be virally suppressed, despite similar rates of ART.
In part, this may be due to improved access and coordination with specialty care services, specifically mental health and substance abuse. Enhanced coordination of care may allow for better treatment of comorbid diseases and improved adherence to HAART.

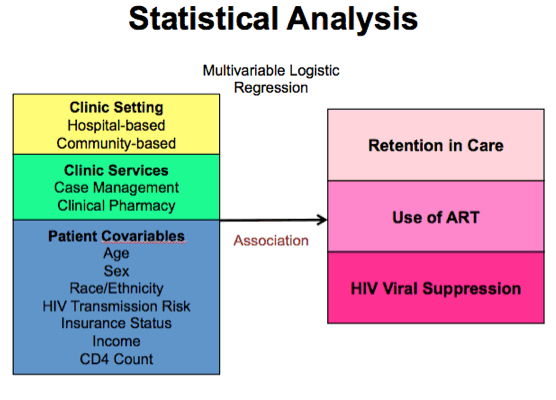
Successful care for people living with HIV is determined by numerous factors, including "patient" factors, such as sociodemographics and clinical status, as well as "environmental" ones including where patients receive care, where patients live and services offered by clinics. These factors influence health behaviors, such as adherence to ART, and ultimately translates into biologic outcomes, as seen on the right, - such as viral load suppression and mortality - as well as public health outcomes - including transmission to uninfected individuals.
Much has been studied about various patient-level factors, but less has been is known about which environmental and clinic-level factors influence outcomes.
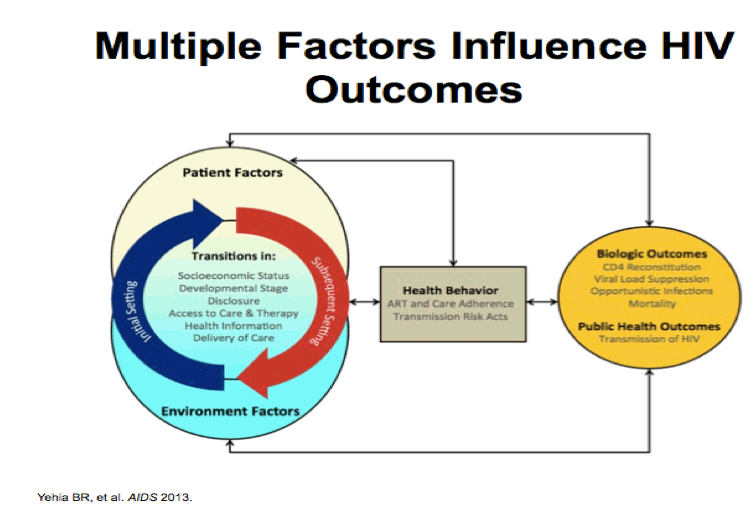
Outpatient care for people living with HIV is delivered in different settings, including large hospital clinics and community-based practices.
Little is known about how these different settings influence patient outcomes in HIV. Patient outcomes may be influenced by the type of clinic in which care is delivered.
We know already from research in the primary care literature that hospital-based clinics have higher rates of vaccinations among their patients than other clinic settings, and also that patients in community health centers are more likely to have had visits to a general provider within the past year, compared with the general population.


We assessed 3 clinical outcomes:
First, retention in care. For this, we used the definition provided by the Health Resources and Services Administration, which is two or more visits with an HIV provider in a calendar year, separated by at least 90 days.
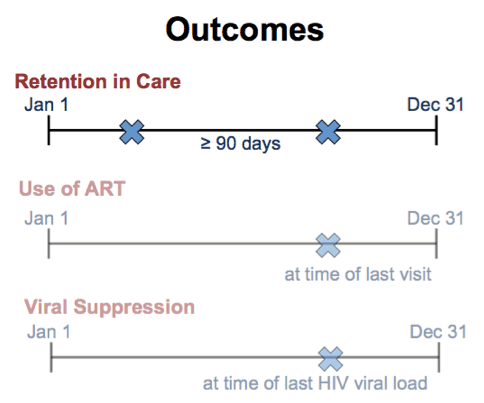
Second, use of antiretroviral therapy. This was defined as the patient being documented to be taking at least three antiretroviral drugs at the last clinic visit in the calendar year.
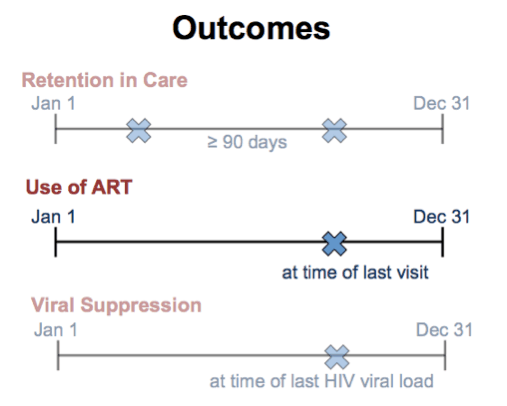
Third is viral suppression, defined as viral RNA less than 200 during the last viral load measurement in the year.
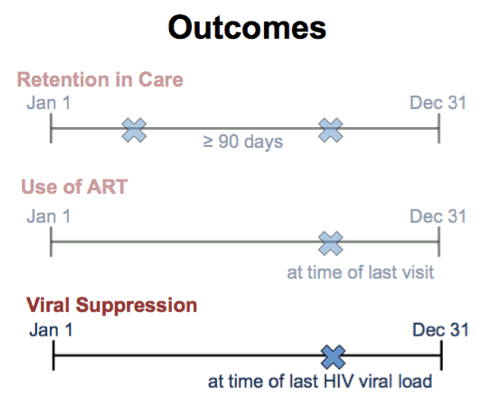
In our analysis, we built three multivariate logistic regression models to assess for associations between clinic setting - that is, hospital or community based clinic - and each of our individual outcomes: retention in care, use of antiretroviral therapy and viral suppression. Our analysis took into account onsite clinic services, specifically case management and clinical pharmacy, and patient variables, such as age, sex, race/ethnicity, transmission risk, insurance status, income and CD4 count.
This slide displays the characteristics of our patient sample across the four-year study period.
--
Overall we had ___ people in the study, increasing from 6,434 patients to 10,037 in 2011.
The sample aged over time, with patients 50 years and older increasing to 37% of the sample.
The majority of patients were male .
--
Black patients comprised the majority.
Heterosexual transmission remained the primary risk factor and there were no large variations in the transmission risk of patients.
Patients with household income under ten thousand dollars decreased.
And the proportion of patients with a CD4 count less than 350 decreased over the period.
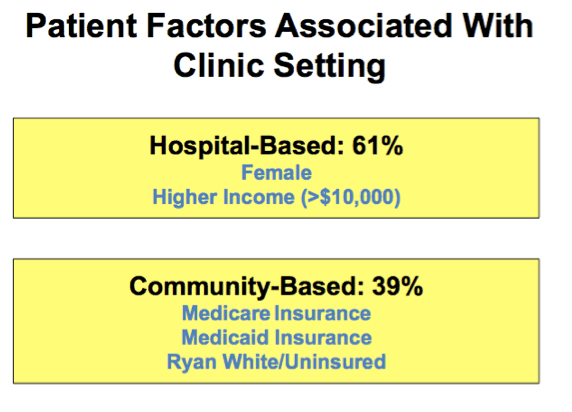
Overall, patients attended hospital-based clinics in 61% of patient-years; and community-based clinics saw the remaining 39% of patient-years.
In multivariate analysis we found that patients seen in hospital clinics were significantly more likely to be female and have higher income.
Significant associations with visiting community clinics included being on Medicare or Medicaid for insurance or being uninsured or covered by the Ryan White program.
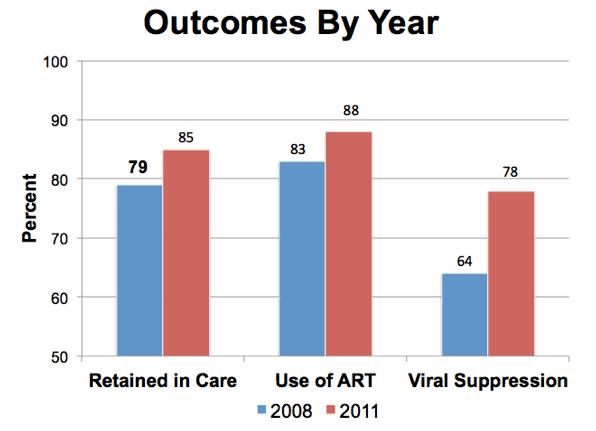
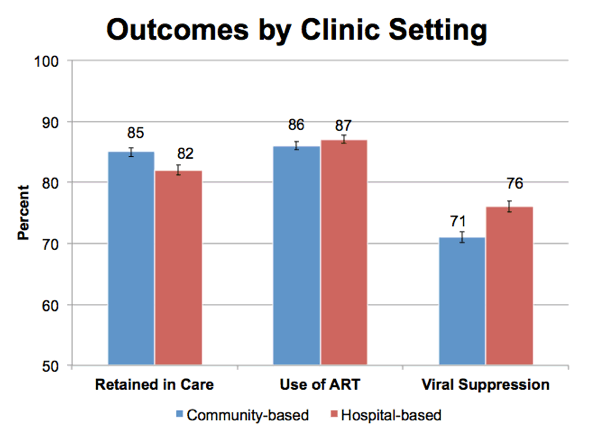
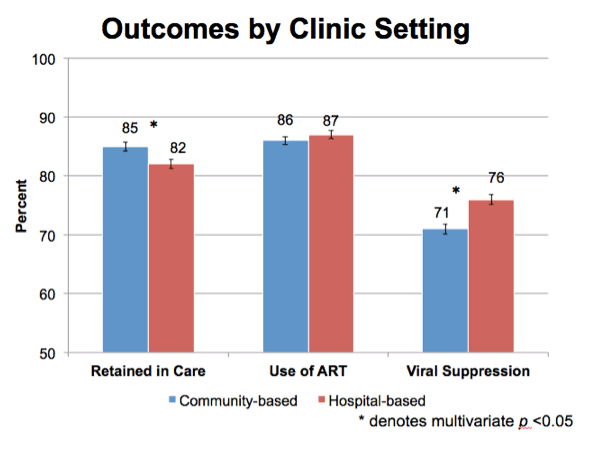
This slide shows the unadjusted proportion of patients in each clinic type meeting our outcomes.
Overall we found that community clinics had significantly higher retention in care, retaining 85% of their patients, compared with 82% in hospital-based clinics
Use of ART was similar between clinic types at 86 to 87%.
And, on the right, we show that patients seen in hospital based clinics had higher rates of viral suppression. 76% patients in hospital clinics were suppressed, compared with 71% in community clinics.
In multivariate analyses, adjusting for clinic and patient factors, we found that:
Retention in care and viral suppression significantly differed by clinic setting.
No statistically significant difference was observed in ART use.
|
| |
|
 |
 |
|
|