 |
 |
 |
| |
CDC Figures Annual US Mortality in People With HCV Could Top 80,000: HCV Mortality Under-reported, Mortality Rate 12 Times Higher than General Population, HCV+ Die 15 Years Younger than General Population
|
| |
| |
IDWeek, October 2-6, 2013, San Francisco
Mark Mascolini
As many as 80,000 people with hepatitis C virus (HCV) infection could die yearly in the United States, according to results of a multicohort analysis from 2006 through 2010 [1]. People with HCV died at an average age 15 years younger than people in the general population.
From 2.7 to 3.9 million people in the United States have chronic HCV infection. To estimate all-cause and liver-related mortality among HCV-positive US residents, the Centers for Disease Control and Prevention (CDC) examined electronic medical records of adults who had at least one health system encounter from January 2006 through December 2010 in four integrated healthcare systems. In the resulting Chronic Hepatitis Cohort Study (CHeCS), the investigators identified those who died from 2006 through 2010. They compared CHeCS mortality findings with data from the national Multiple Cause of Death (MCOD) study in the same period.
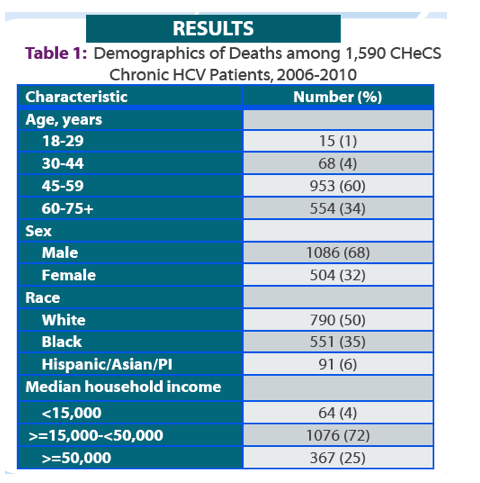
From 2006 through 2010, the CDC team considered 11,703 people with chronic HCV representing 0.5% of patients in the 2.1-million person CHeCS cohort. Among people with HCV, 1590 (14%) died during the study period. Most people who died were 45 to 59 years old (60%), followed by the group 60 and older (34%). Men accounted for two thirds of the deaths (68%), whites for 50%, and blacks for 35%. Almost three quarters of those who died (72%) had a median household income between $15,000 and $50,000, while 25% had a higher income.
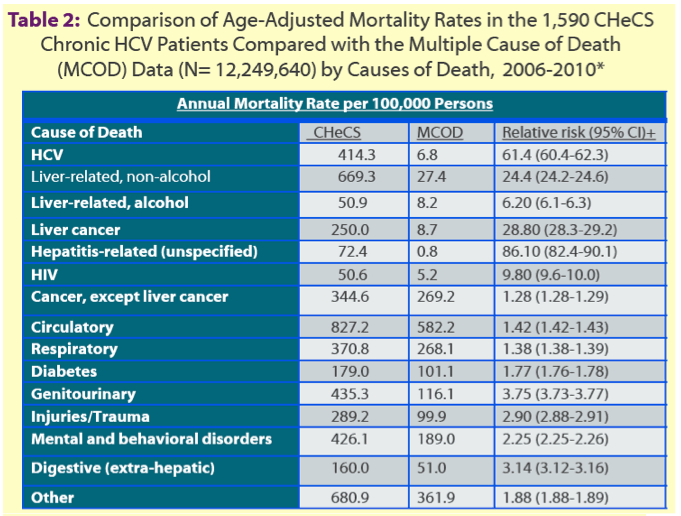
Compared with MCOD data, mortality was 12 times higher in CHeCS. Age-adjusted mortality in CHeCS compared with MCOD was 61 times higher for HCV infection (relative risk [RR] 61.4), 29 times higher for liver cancer (RR 28.8), 24 times higher for nonalcohol-related liver disease (RR 24.4), 10 times higher for HIV infection (RR 9.8), 6 times higher for alcohol-related liver disease (RR 6.2), and 86 times higher for unspecified hepatitis-related disease (RR 86.1) (P < 0.0001 for all).
Age averaged 59 years in CHeCS members who died, 15 years younger than the all-cause death age in US national data.
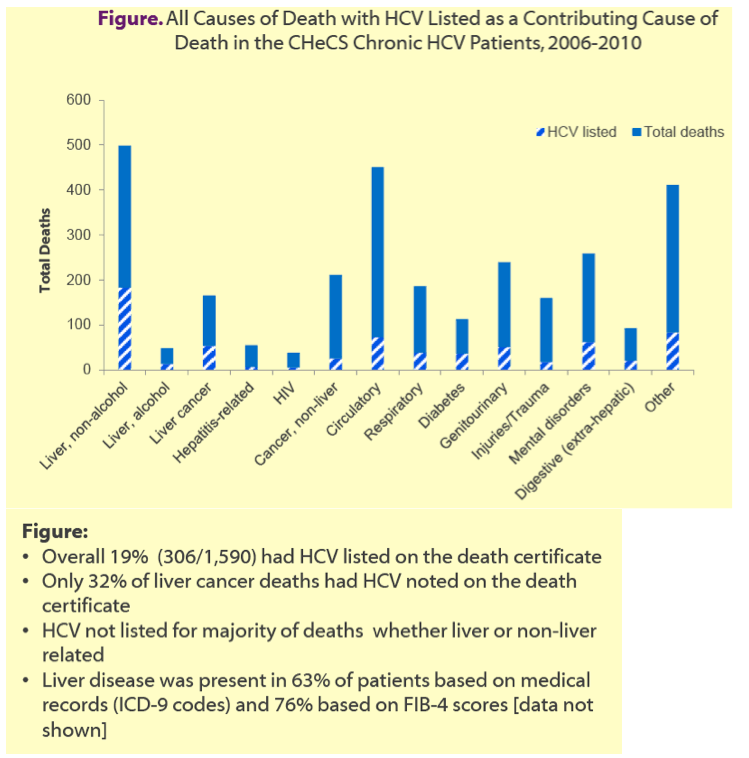
Among the 1590 CHeCS members who died, only 306 (19%) had HCV infection listed as an underlying cause on their death certificate. Among people who died of liver cancer, only 32% had HCV listed as an underlying cause. Death certificates did not list HCV for most deaths regardless of whether the deaths were liver-related or not. Among CHeCS members who died, medical records (ICD-9 codes) noted liver disease in 63%, and FIB-4 scores indicated liver disease in 76%.
"Even in these well-characterized HCV patients," the CDC team concluded, "HCV was noted in only 19% of death certificates." Based on this finding, the researchers estimated that more than 80,000 US residents with HCV died in 2010. They noted that chronic liver disease recorded in two thirds of CHeCS members who died "suggests that 53,000 patients are dying not only with, but possibly from HCV."
Reference
1. Mahajan R, Xing J, Liu S, et al. Rates and causes of mortality among people in care with hepatitis C virus infection--Chronic Hepatitis Cohort Study (CHeCS), 2006-2010. IDWeek 2013. October 2-6, 2013. San Francisco. Abstract 1774.
----------------------------
Reported by Jules Levin
Mortality among Persons in Care with Hepatitis C Virus Infection-Chronic Hepatitis Cohort Study (CHeCS), 2006 -2010
Reena Mahajan,1 Jian Xing,1 Stephen Liu,1Kathleen Ly,1 Anne C. Moorman,1Lora Rupp,2 Fujie Xu,1Scott Holmberg,1 for the Chronic Hepatitis Cohort Study (CHeCS) Investigators*
(1)Centers for Disease Control and Prevention, Atlanta, GA (2)Center for Health Services Research, Henry Ford Health System, Detroit, MI


Program Abstract
Background: To examine the association of hepatitis C virus (HCV) infection with all-cause and liver-related mortality, we analyzed data from a prospective observational cohort study in four health care systems in the United States.
Methods: We examined electronic health records of adults with at least one health system encounter from January 2006 through December 2010 from four integrated health care systems, and created a cohort of confirmed HCV-infected patients [Chronic Hepatitis Cohort Study (CHeCS)]. Cohort patients who died during 2006-2010 were analyzed. All-cause and disease-specific death rates were calculated based upon US census data from 2006-2010. Total number of deaths came from Multiple Cause of Death (MCOD) data based on 12 million death certificates for U.S. residents for the same time period.
Results: Of 2,143,369 adult patients with an encounter with the four CHeCS sites during 2006-2010, 11,703 (0.5%) had diagnosed chronic HCV infection. Of these, 1,590 (14%) died during 2006-2010; 75% of whom were born between 1945-1965, 50% were white, and 68% were men. Primary cause of death (498 of 1590) was liver disease unrelated to alcohol. Despite confirmed chronic HCV infection in those who died, only 19%had HCV infection listed as an underlying cause of death, and only 32% among those who died of primary liver cancer. Mean age of death for HCV patients (59 years) was 15 years younger than in those without HCV infection from national data. The age-adjusted mortality rate for liver disease in CHeCS was twelve times higher than the MCOD rate.
Conclusion: HCV infection was not listed as a cause of mortality in approximately 80% of confirmed HCV-infected persons; currently only 15,000 deaths have HCV infection listed on the death certificate. Our data suggests that the national mortality rate of those with HCV could be as high as 75,000 persons per year, with over 60% of current deaths in our HCV-infected cohort directly attributable to liver disease. Whether ascribed to liver-related causes or not, mortality in HCV-infected persons was 15 years younger compared with the national average in non-HCV infected persons.

* The CHeCS Investigators include Scott D. Holmberg, Eyasu H.Teshale, Philip R. Spradling, and Anne C. Moorman, CDC, Atlanta, Georgia; Stuart C. Gordon, David R. Nerenz, Mei Lu, Lois Lamerato, Loralee B. Rupp, Nonna Akkerman, Nancy Oja-Tebbe, Chad M. Cogan, and Dana Larkin, Henry Ford Health System, Detroit, Michigan; Joseph A. Boscarino, Zahra S. Daar, Joe B. Leader, and Robert E. Smith, Geisinger Health System, Danville, Pennsylvania; Vinutha Vijayadeva, Kelly E. Sylva, John V. Parker, and Mark M. Schmidt, Kaiser Permanente- Hawaii, Honolulu, Hawaii; Mark A. Schmidt, Judy L. Donald, and Erin M. Keast, Kaiser Permanente- Northwest, Portland, OR.
The findings and conclusions in this report are those of the authors and do not necessarily represent the official position of the Centers for Disease Control and Prevention.

|
| |
|
 |
 |
|
|