 |
 |
 |
| |
Effects of aging and antiretroviral therapy on B Cell phenotypes in HIV infected subjects
|
| |
| |
Reported by Jules Levin
IDSA Oct 2-6 2013 San Francisco, CA
Puja Van Epps1,5, Katherine Tassiopoulos2, Roy Matining2, Donald Anthony1, Alan Landay3, Robert Kalayjian4, David H. Canaday1,5
(1)University Hospitals Case Medical Center, Cleveland, OH (2)Harvard School of Public Health, Boston, MA (3)Rush Medical Center, Chicago IL.
(4)Metrohealth Medical Center, Cleveland, OH (5)Geriatric Research Center Clinical Core (GRECC), Cleveland VA


Program Abstract
Background:
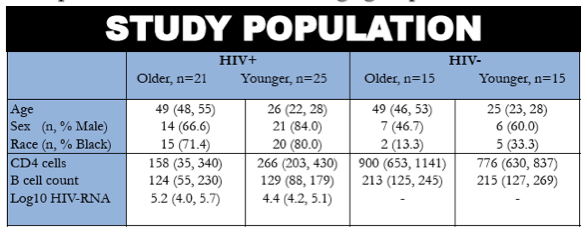
Older HIV infected subjects had significant B cell expansion, in a prospective study that examined immune differences to initial antiretroviral therapy (ART) between older and younger (≥45 vs. ≤30 years) through the AIDS Clinical Trials Group (ACTG Study 5015). Herein we examined age-group differences in B cell phenotypes, and their associations with antibody responses to vaccination.
Methods:
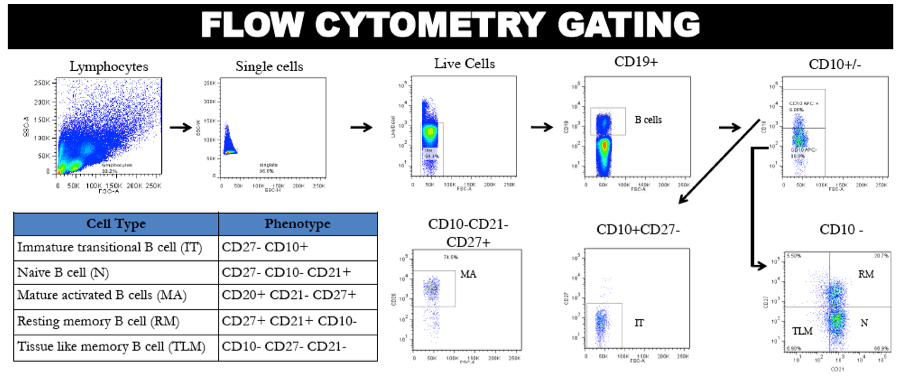
Age group differences in B cell phenotypes, as counts and % of naive, resting memory (RM), immature transitional (IT), tissue like memory (TLM) and mature activated (MA) B cells from cryopreserved PBMCs (at weeks 0, 48, 96, 192 for A5015; at week 0 for healthy controls (A5113)) were compared within A5015 and to age-matched healthy controls using exact Wilcoxon Rank Sum test. 46 subjects were analysed in the HIV infected group (21 older, 25 younger) and 30 in the control group (15 per age group). Multivariable linear regression explored associations between each phenotype and the 12 week change in log10 antibody concentration after tetanus and hepatitis A vaccination at week 0.
Results:
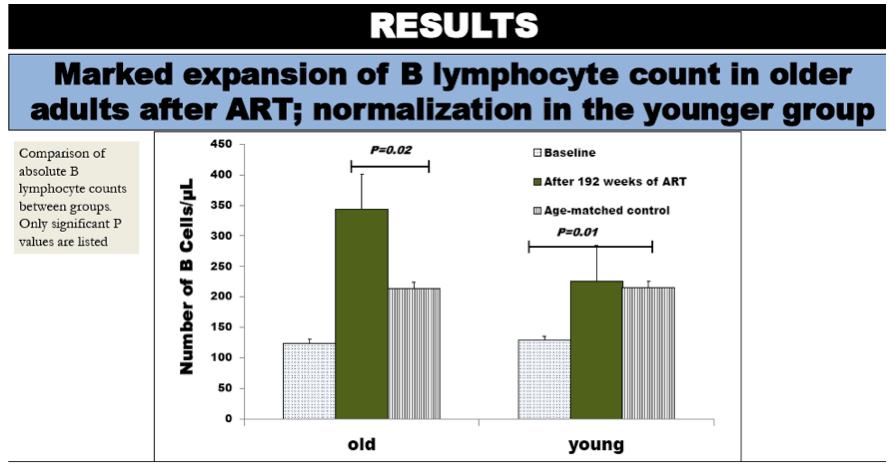
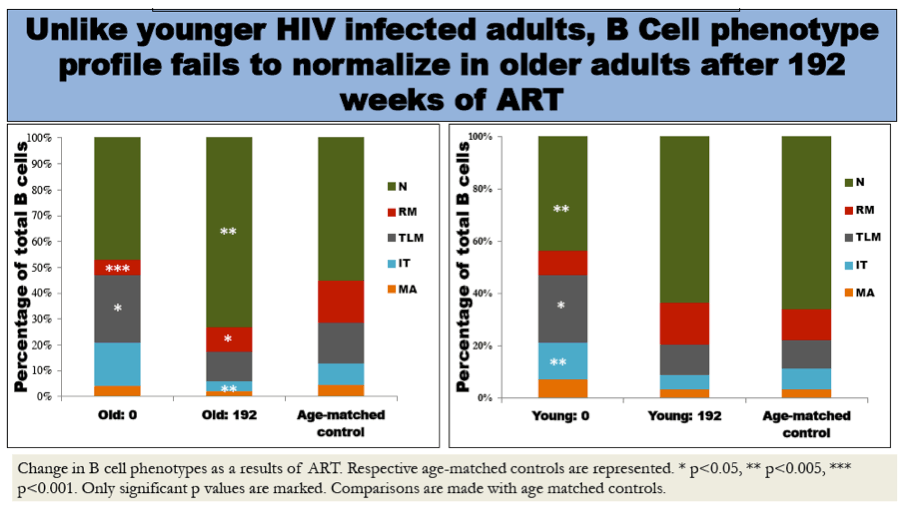
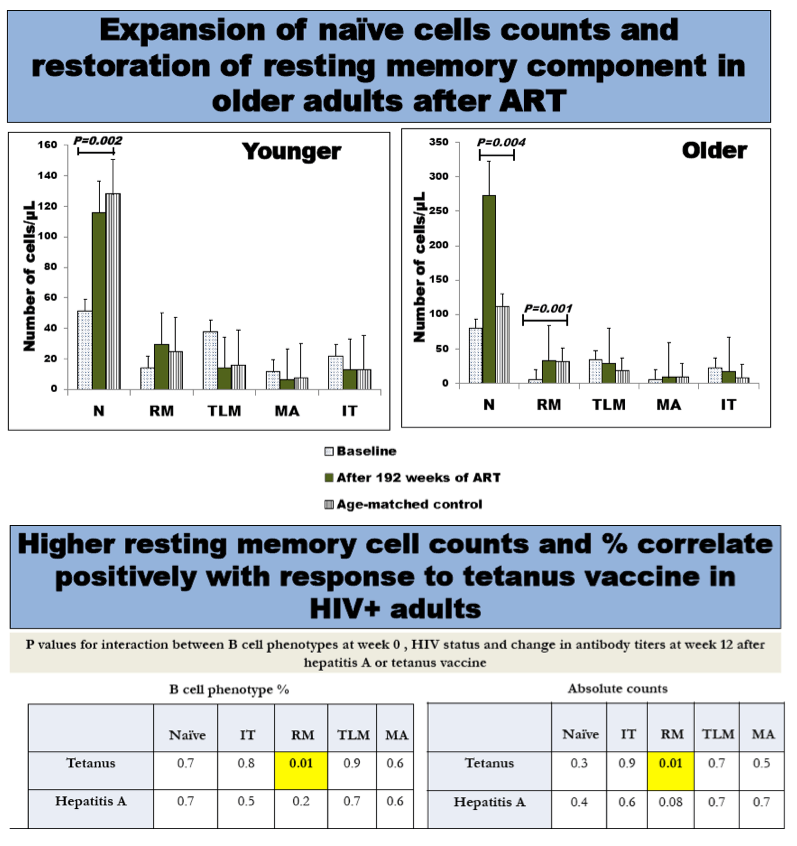
Naive counts and the % naive cells increased significantly from baseline to week 192 in older (by median 161cells/µL & 25.6% respectively; both p<0.03) and younger (by 51cells/µL & 17.6%, p<0.04) subjects, however, older HIV infected subjects had significantly higher naive counts and % at week 192 than controls (p<0.05). RM counts and % increased in both age groups (older: 9cells/mL, p=0.006 & 2.3%, p=0.08; younger: 11cells/mL & 4.5%, both p<0.04) but the median %RM cells remained lower than controls among older subjects (p=0.01). There were no significant age-group differences in changes of IT, TLM and MA cells. Higher baseline RM cell counts and % were significantly associated with higher tetanus antibody increases after vaccination, but this was evident only among HIV infected subjects (p=0.01 for interaction between HIV-infection status and RM counts or %) and was not age related.
Conclusion:
Older HIV infected subjects had naive B cell expansion with ART and incomplete restoration of % RM cells. Relationship between RM cells at baseline and tetanus responses may lead to insights about the effects of HIV infection on B cell memory function and vaccine responses.
|
| |
|
 |
 |
|
|