 |
 |
 |
| |
Independent Predictors of Patient-Reported Outcomes (PROs) and Quality of Life (QOL) in Chronic Hepatitis C Patients Receiving Interferon (IFN) -Free versus IFN-Containing Regimens with Sofosbuvir (SOF)
|
| |
| |
Reported by Jules Levin
EASL 2014 April 9-13 London, UK
Zobair M. Younossi, Maria Stepanova, Fatema H. Nader, David Nelson, Eric Lawitz, Ira M. Jacobson, Edward Gane, Sharon L. Hunt
1.Center for Liver Diseases, Department of Medicine, Inova Fairfax Medical Campus, Falls Church VA, United States.
2.Betty and Guy Beatty Center for Integrated Research, Inova Health System, Falls Church VA, United States.
3.University of Florida, Gainesville, FL, United States.
4. Texas Liver Institute, University of Texas Health Science Center, San Antonio, TX, United States.
5. Weill Cornell Medical College, New York, NY, United States.
6. Auckland City Hospital, Auckland, New Zealand.

Program abstract-
Background and aims: IFN causes substantial impairment of QoL. We compared PROs and QoL between IFN-free and IFN-containing-SOF regimens.
Methods: 525 patients receiving IFN+RBV+SOF (NEUTRINO) or RBV+SOF (FUSION) completed PRO questionnaires: CLDQ-HCV (QoL), FACIT-F (Fatigue) and WPAI-SHP (work productivity and activity). Subjects were blinded to virologic data.
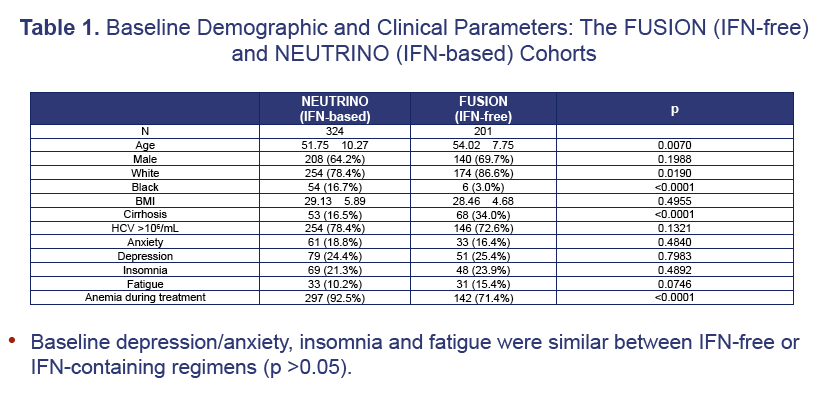
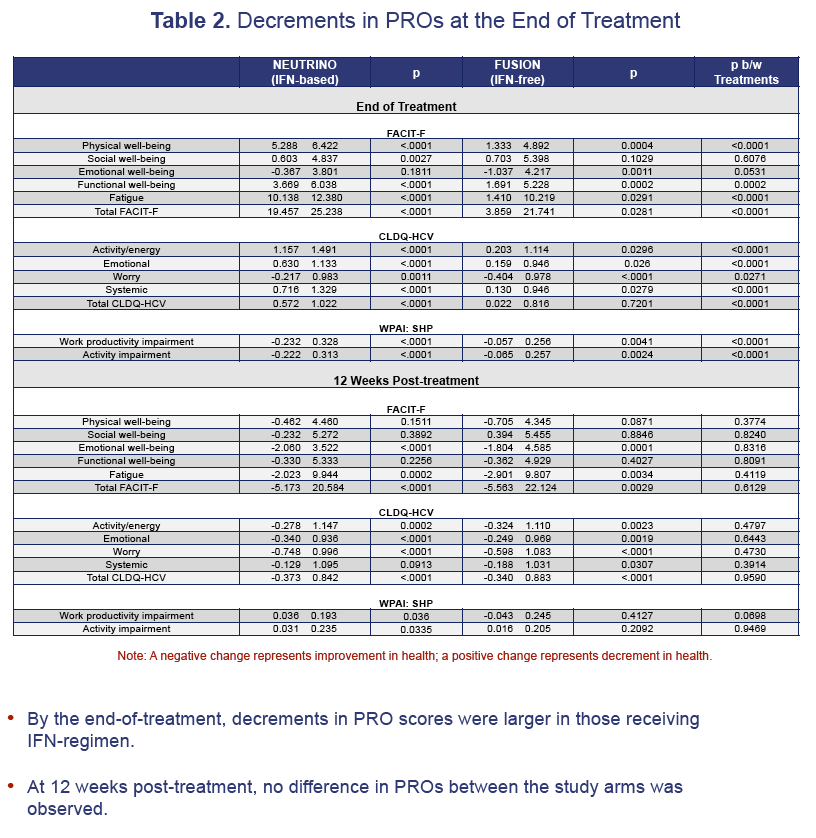
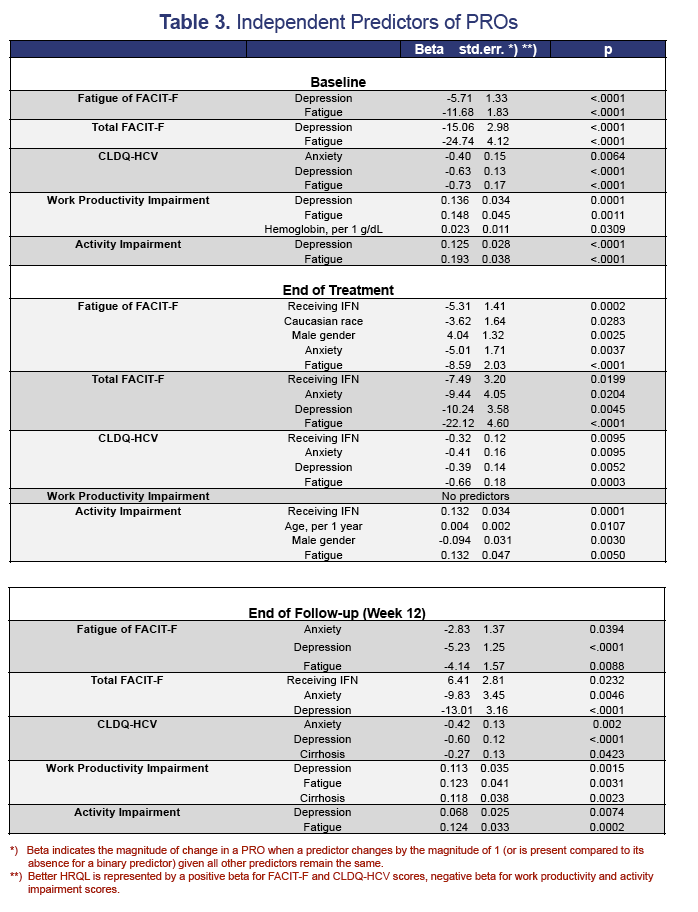
Results: Baseline depression/anxiety, insomnia and fatigue were similar between IFN-free or IFN-containing regimens (p>0.05). By the end-of-treatment, decrements in PRO scores were higher in those receiving IFN-regimen: physical well-being (decrement=18.9% IFN-based vs. 4.6% IFN-free, p< 0.0001), functional well-being (13.2% vs. 6.1%, p=0.0002), fatigue (19.4% vs. 2.7%, p< 0.0001), total-FACIT-F (12.2% vs. 2.4%, p< 0.0001), all domains of CLDQ-HCV (9.5% to 19.3% vs. 0.3% to -3.3%, p< 0.05), work productivity (23.2% vs. 5.7%, p=0.004) and activity impairment (22.2% vs. 6.5%, p=0.002). In multivariate analysis, predictors of poor PROs at baseline were depression (beta=-9.4 to -13.6%, p< 0.05) and fatigue (beta=-12.2 to -22.5%, p< 0.05). At the end-of-treatment, predictors of poor PROs included receiving IFN (beta=-4.7 to -13.2%, p< 0.05), depression (beta=-6.4 to -6.5%, p< 0.05), fatigue (beta=-10.9 to -16.5%, p< 0.05) and female gender (beta=-7.8 to -9.4%, p< 0.05). By follow-up week 12, predictors of poor PROs included depression, anxiety, fatigue and cirrhosis (p-values< 0.05). In subjects with SVR-12, predictors of residual PRO impairment included anxiety (beta=-5.4 to -7.0%, p< 0.05), depression (beta=-6.8 to -11.3%, p< 0.05), fatigue (beta=-8.0 to -12.4%, p< 0.05) and cirrhosis (beta=-4.4 to -11.8%, p< 0.05).
Conclusions: Fatigue and depression are the main drivers of PRO impairment. During treatment, IFN is another predictor of poor PROs.


|
| |
|
 |
 |
|
|