 |
 |
 |
| |
Maraviroc (MVC) Once Daily With Darunavir/Ritonavir(DRV/r) Compared to Tenofovir/Emtricitabine (TDF/FTC) With DRV/r: 48-Week Results From MODERN (Study A4001095)
|
| |
| |
Reported by Jules Levin
20th International AIDS Conference, July 20-25, 2014, Melbourne
H.-J. Stellbrink,1P. Pulik,2J. Szlavik,3D. Murphy,4A. Lazzarin,5J. Portilla,6A. Rinehart,7E. Le Fevre,8A. Fang,9S. Valluri,9G. Mukwaya,10J. Heera111ICH-Study Center, Hamburg, Germany; 2SPZOZ Wojewodzki Szpital Zakazny, Warsaw, Poland; 3Egyesittet Szent Istvan es Szent Laszio Korhaz-Rendelointezet, Budapest, Hungary; 4Clinique Medicale L'Actuel, Montreal, Canada; 5Ospedale San Raffaele, Divisione di Malattie Infettive, Milan, Italy; 6Hospital General Universitario de Alicante, Unidad de VIH, Alicante, Spain; 7-8ViiV Healthcare, 7Research Triangle Park, NC, USA; 8Brentford, United Kingdom; 9-11Pfizer Inc., 9New York, NY, USA; 10Medicines Development Group, New York, NY, USA; 11Groton, CT, USA

---------------------------
Program Abstract
Background: Maraviroc, a CCR5 receptor antagonist, has shown durable antiviral response with a favorable safety profile. Nucleos(t)ide-sparing, 2-drug regimens containing ritonavir-boosted protease inhibitors have not been extensively studied in antiretroviral-naïve subjects. Such regimens may decrease pill burden, toxicities, costs and drug-drug interactions.
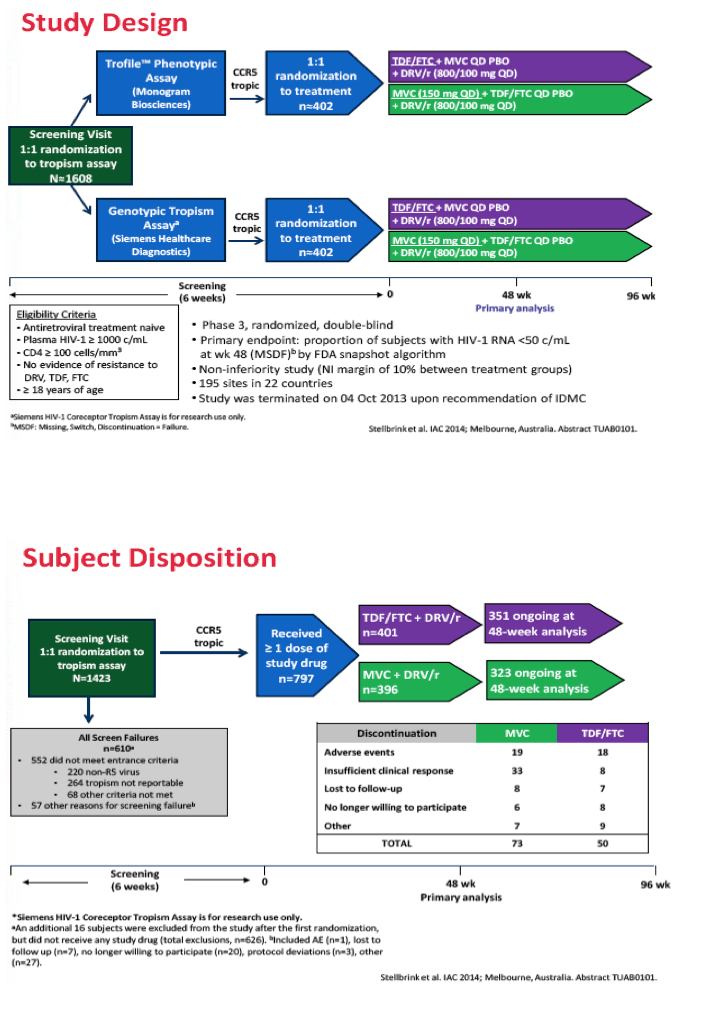
Methods: In this multicenter, double-blind, Phase III study, HIV-1 infected antiretroviral-naïve adults with HIV-1 RNA >1000 copies/mL, without reported viral resistance, underwent 2-stage randomization. At screening, subjects were first randomized 1:1 to either genotype (Siemens) or Enhanced Sensitivity Trofile Assay (ESTA, Monogram BioSciences) to identify CCR5-tropic HIV-1 infection. Subjects with CCR5-tropic HIV-1 were then randomized 1:1 to receive MVC 150 mg QD or TDF/FTC 200/300 mg QD each with DRV/r 800/100 mg QD for up to 96 weeks. The primary endpoint was proportion of subjects with HIV-1 RNA < 50 copies/mL at Week 48 (FDA "snapshot" algorithm).
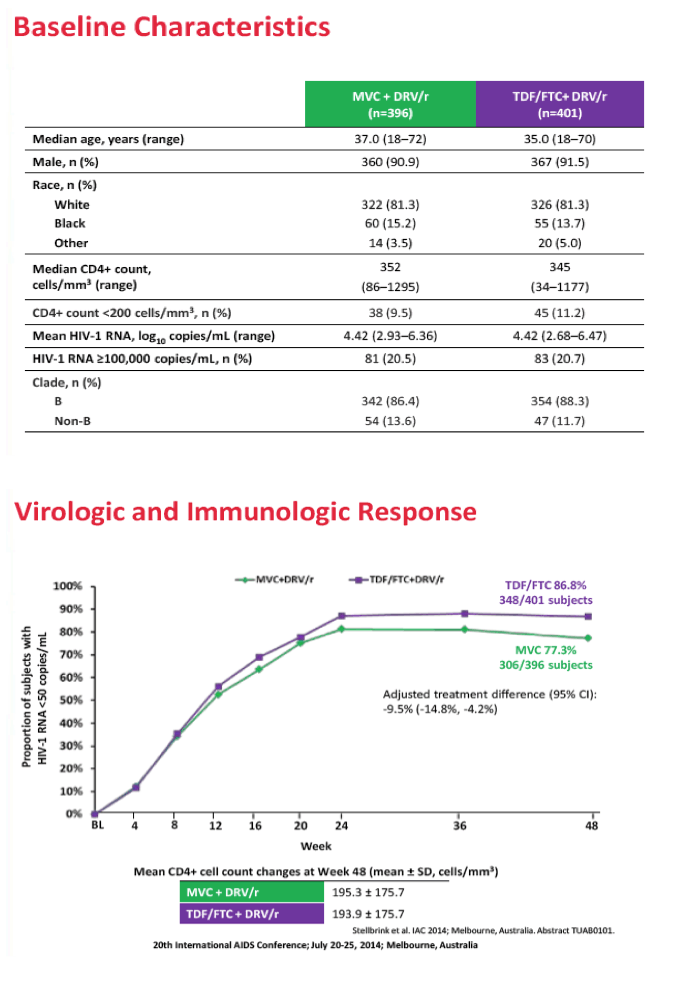
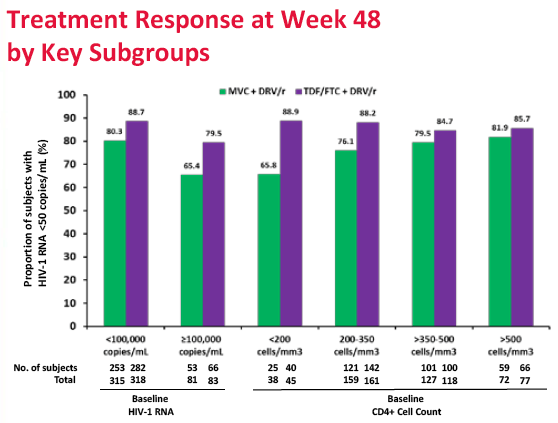
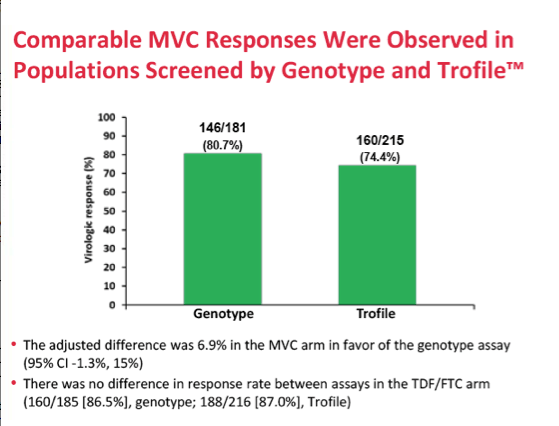
Results: 797 subjects were dosed (MVC n=396, TDF/FTC n=401). At baseline: median age 37.1 years, 8.8% female, 18.7% non-white, 20.6% HIV-1 RNA >100,000 copies/mL. Proportion of subjects meeting the primary endpoint was 77.3% for MVC and 87.0% for TDF/FTC (difference -9.73%; 95% CI; -15.0% to -4.4%). MVC did not meet the -10% non-inferiority criteria. The difference in the proportion of subjects meeting the primary endpoint between the tropism assays (genotype or ESTA) was not statistically significant (MVC: difference 6.86% in favor of genotyping, 95% CI -1.28% to 15.0%; TDF/FTC: difference 0.3%, 95% CI: -6.4% to 6.9%). More MVC subjects discontinued for lack of efficacy (8.3% vs 2.0%). Protocol defined treatment failure (PDTFs) were 10.1% for MVC and 3.2% for TDF/FTC.
Discontinuations due to AEs were 4.8% for MVC and 4.5% for TDF/FTC. Category C events, grade 3/4 AEs and laboratory abnormalities were similar between the treatment arms. This study was prematurely stopped for inferior efficacy following a recommendation by the data monitoring committee.
Conclusions: At Week 48, MVC dosed once daily with DRV/r in a 2 drug-regimen showed inferior efficacy to TDF/FTC + DRV/r in antiretroviral-naïve subjects. The two CCR5-tropism assays (genotype or ESTA) were similar in predicting a positive treatment outcome. There were no new or unique safety findings.
--------------------------


|
| |
|
 |
 |
|
|