 |
 |
 |
| |
Ledipasvir/Sofosbuvir is Safe and Effective as a Single-Tablet-Regimen for Treatment of Patients with Genotype 1 Chronic Hepatitis C Virus, Including those with Compensated Cirrhosis
|
| |
| |
Reported by Jules Levin
20th International AIDS Conference, Melbourne, Australia, 20-25 July 2014
Mark S. Sulkowski, MD1, Kris Kowdley, MD2, Peter J. Ruane, MD3, Trevor Hawkins, MD4, Richard Elion, MD5, Kimberly Workowski, MD6, Anthony Mills, MD7, Mani Subramanian, MD, PhD8, Xiao Ding, PhD8, Star Seyedkazemi, PharmD8, Robert H. Hyland, D.Phil8, Jenny C. Yang, PharmD8, Phillip S. Pang, MD, PhD8, John G. Mchutchison, MD8, Nezam Afdhal, MD9 and David Wyles, MD10
1Johns Hopkins University School of Medicine, Baltimore, MD, 2Virginia Mason Medical Center, Seattle, WA, 3Peter J. Ruane, MD, Inc, Los Angeles, CA, 4Southwest Care Center, Santa Fe, NM, 5Whitman Walker Clin., Washington, DC, 6Infectious Diseases, Emory University School of Medicine, Atlanta, GA, 7Anthony Mills MD, Inc., Los Angeles, CA, 8Gilead Sciences, Inc., Foster City, CA, 8Gilead Sciences, Foster City, CA, 9Beth Israel Deaconess Medical Center, Harvard University School of Medicine, Boston, MA, 10Medicine, University of California San Diego, La Jolla, CA
this poster at IAC is a pooled analysis, that is a review/summary of the 3 phase studies ION-1, ION-2, ION-3 which were all reported at EASL, in April, the European Liver Meeting in London, UK. This summary captures the data but here are links to the original presentations at EASL, which provide a little more information, and also immediately below is the program abstract:
EASL: All Oral Fixed-Dose Combination Ledipasvir/Sofosbuvir With Or Without Ribavirin for 12 or 24 Weeks in Treatment-Naive Genotype 1 HCV-Infected Patients: the Phase 3 ION-1 Study - (04/14/14)
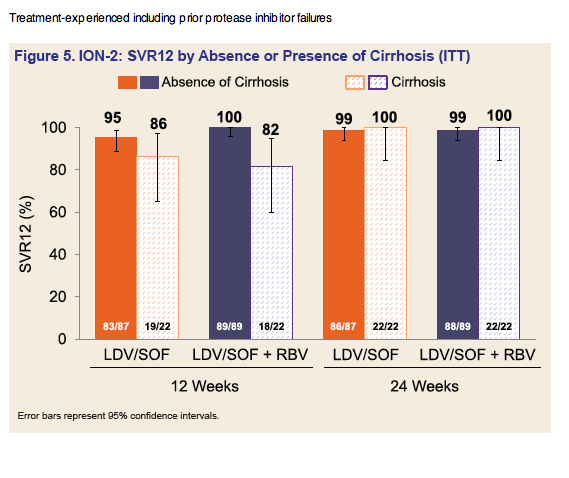
EASL: All Oral Fixed-Dose Combination Ledipasvir/Sofosbuvir With or Without Ribavirin for 12 or 24 Weeks in Treatment-Experienced Genotype 1 HCV-Infected Patients: The Phase 3 ION-2 Study - (04/14/14)
EASL: Ledipasvir/Sofosbuvir With and Without Ribavirin for 8 Weeks Compared to Ledipasvir/Sofosbuvir for 12 Weeks in Treatment-Naïve Noncirrhotic Genotype-1 HCV-Infected Patients: The Phase 3 ION-3 Study - (04/11/14)
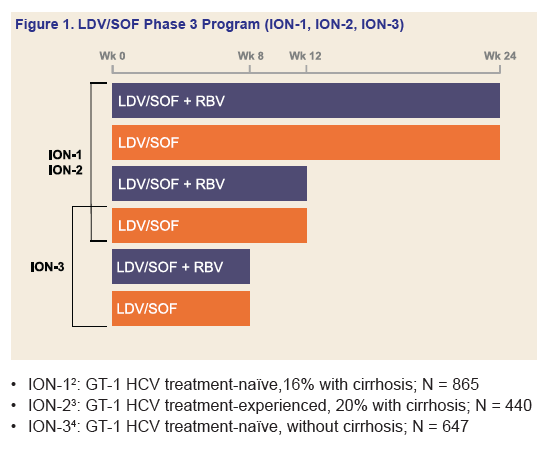
Program Abstract - Methods: Three open-label phase 3 clinical trials evaluated the safety and efficacy of LDV/SOF administered with or without (±) RBV for treatment of GT 1 chronic HCV. There was no upper limit to age or body mass index (BMI). Treatment-naïve patients, including those with compensated cirrhosis, were randomized to 12 and 24 weeks of LDV/SOF ± RBV in the ION-1 study, while patients without cirrhosis were randomized to 8 weeks of LDV/SOF ± RBV or 12 weeks of LDV/SOF in the ION-3 study. HCV treatment-experienced patients, including those with compensated cirrhosis and prior HCV protease-inhibitor (PI) failure, were randomized to 12 and 24 weeks of LDV/SOF ± RBV in the ION-2 study. The primary endpoint was SVR at 12 weeks after the end of therapy (SVR12).
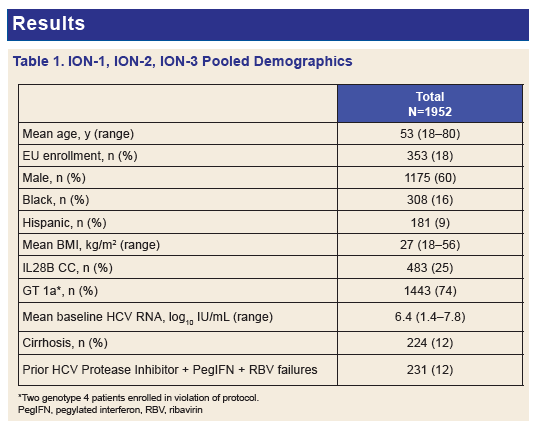
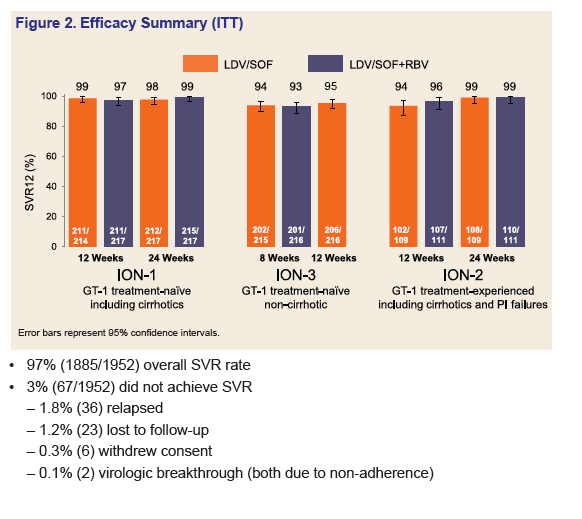
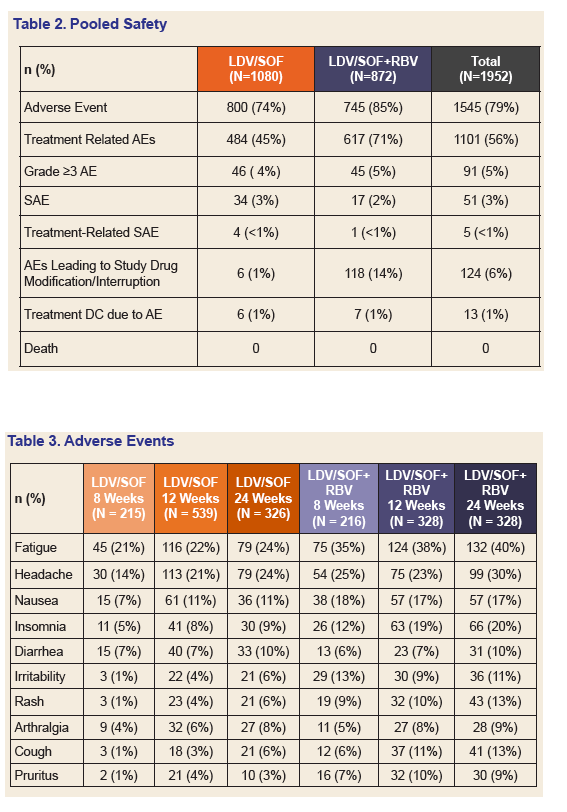
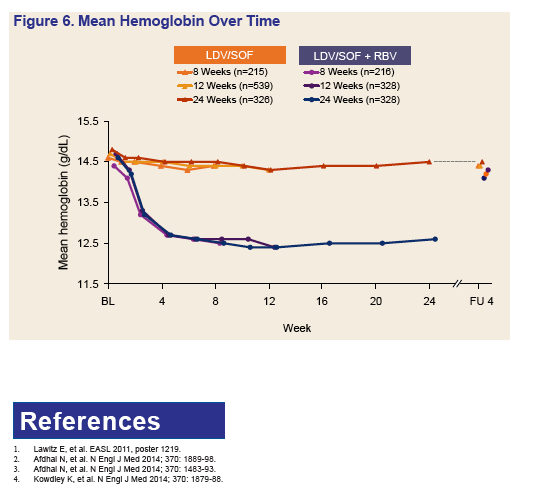
Results: Of the 1952 patients randomized and treated in these three phase 3 studies, 308 (16%) were African American, 224 (12%) had compensated cirrhosis, 591 (26%) had a BMI ≥ 30 kg/m2, 1597 (82%) had a high HCV viral load ≥ 800,000 IU/mL, and 440 (23%) were treatment-experienced. Of these 440 treatment-experienced subjects, 231 (53%) were prior HCV protease-inhibitor (PI) + PegIFN + RBV treatment failures. Overall, 97% of all patients achieved SVR12. The intent-to-treat SVR12 rates in all treatment arms are show in Figure 2 below. The most common adverse events (AEs) included fatigue, headache, nausea, and insomnia. Majority of AEs occurred more frequently in the RBV-containing arms of the studies.
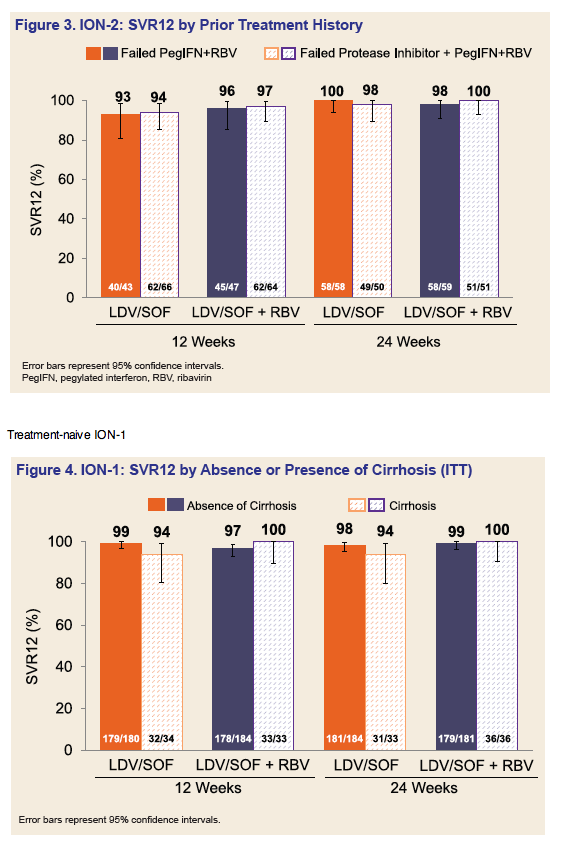
Conclusions: A single-tablet-regimen of LDV/SOF, given once-daily, was highly effective in patients with genotype 1 HCV infection, including those with compensated cirrhosis and those who had previously failed triple therapy with a PI + PegIFN + RBV. The addition of RBV did not increase SVR rates but lead to higher rates of AEs.




|
| |
|
 |
 |
|
|