 |
 |
 |
| |
Disparities in HIV viral load suppression among MSM, the HIV Outpatient Study, 2013
|
| |
| |
Reported by jules Levin
CROI 2015 Feb 23-26, Seattle, WA
Kate Buchacz1, Carl Armon2, Ellen Tedaldi3, Frank J. Palella, Jr.4, Richard Novak5, Douglas Ward6, Rachel Hart2, Marcus Durham1, John T. Brooks1
1 U.S. Centers for Disease Control and Prevention, Atlanta, GA; 2Cerner Corporation, Vienna, VA; 3Temple University School of Medicine, Philadelphia, PA; 4Feinberg School of Medicine, Northwestern University, Chicago, IL; 5University of Illinois, Chicago, IL; 6Dupont Circle Physicians Group, Washington, DC


program abstract
Background: The National HIV/AIDS Strategy has prioritized reducing disparities in virologic suppression (VS) by race/ethnicity among gay, bisexual and other men who have sex with men (collectivey referred to as MSM). Improving VS for black MSM may decrease HIV morbidity and sexual transmission of HIV.
Methods: We analyzed data from the HIV Outpatient Study (HOPS) MSM participants in care at 9 HIV specialty clinics in the United States. We limited analyses to MSM with ł 2 HOPS visits since HOPS inception in 1993, of which at least one occurred in 2013, and who were of non-Hispanic white (NHW), non-Hispanic black (NHB) or Hispanic/Latino race/ethnicity (Hispanic). We assessed the frequency of VS, defined as an HIV RNA (viral load, VL)
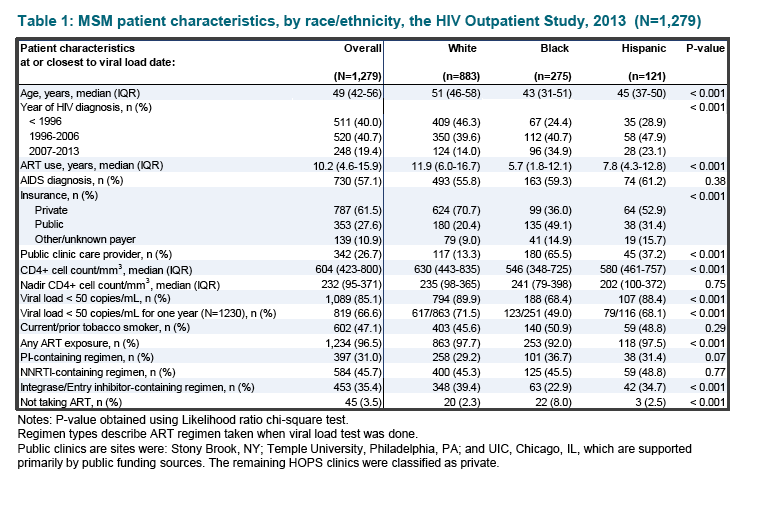
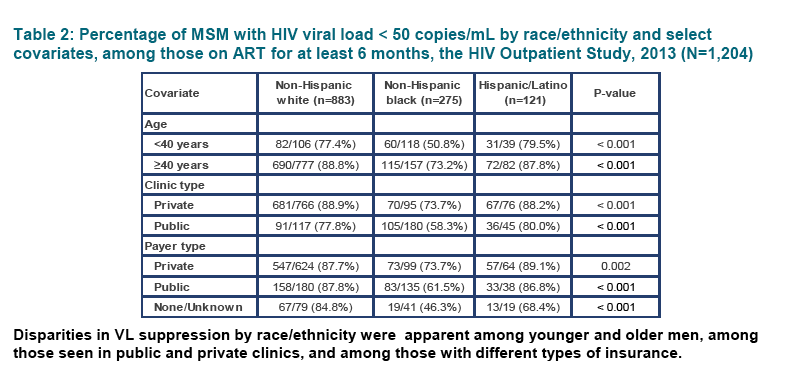
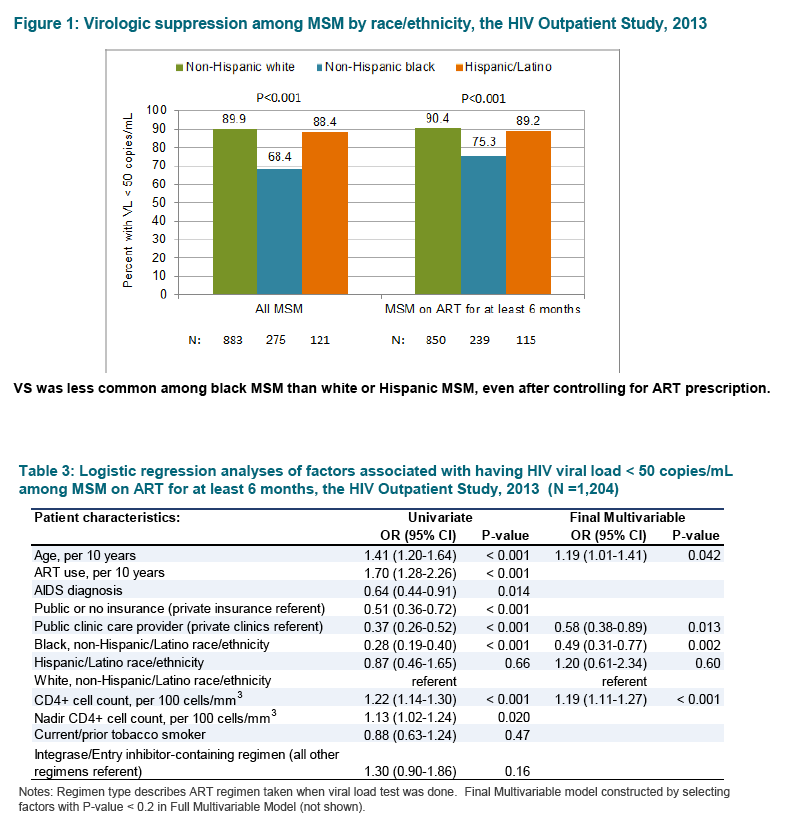
Results: Among 1,239 MSM studied, 266 (21%) were NHB, and 117 (9%) were Hispanic. NHB MSM were younger than NHW and Hispanic MSM (median age 43 vs. 51 and 45 years, respectively), more frequently HIV-diagnosed after 2006 (35% vs. 14% and 23%), less frequently privately insured (36% vs. 71% and 53%) and more frequently cared for at public rather than private clinics (66% vs. 14% and 39%) all p 3) were: for NHB, 242 and 532; for NHW, 235 and 628; and for Hispanics, 207 and 576. Fewer NHB MSM were prescribed ART at the time of VL measurement (92% vs. 98% and 97%) and VS was less common among NHB than NHW and Hispanic MSM, p 3, 95% CI: 1.11-1.27); insurance type was not independently associated with VS.
Conclusions: In our large heterogeneous HIV cohort, NHB MSM had significantly lower rates of VS than NHW and Hispanic MSM. The associations of race/ethnicity and clinic type with VS suggest that interventions to improve HIV care outcomes for all MSM may need to address structural factors and social disparities.
|
| |
|
 |
 |
|
|