 |
 |
 |
| |
Barriers to Effective Prevention: Applying a PrEP Care Continuum to a US Cohort of Black and White MSM
|
| |
| |
Reported by Jules Levin
CROI 2015 Feb 23-26, Seattle, WA
Colleen F. Kelley MD, MPH; Erin Kahle PhD; Aaron Siegler PhD; Carlos del Rio MD; Travis S. Sanchez DVM, MPH; Patrick S. Sullivan DVM, PhD; and Eli S. Rosenberg PhD Center for AIDS Research at Emory University, Atlanta, GA, USA


program abstract-
Background: Reductions in HIV incidence with pre-exposure prophylaxis (PrEP) for men who have sex with men (MSM) will require significant coverage of those at risk. We propose a simplified framework, similar to the HIV Care Continuum, to achieve protection from HIV with PrEP as follows: 1. At-risk MSM; 2. Aware of and willing to take PrEP; 2. Access to healthcare; 3. Receiving a PrEP prescription; and 4. Adhering to PrEP. We evaluated the PrEP Care Continuum on a cohort of Southern MSM and projected how many MSM might achieve protection from HIV.
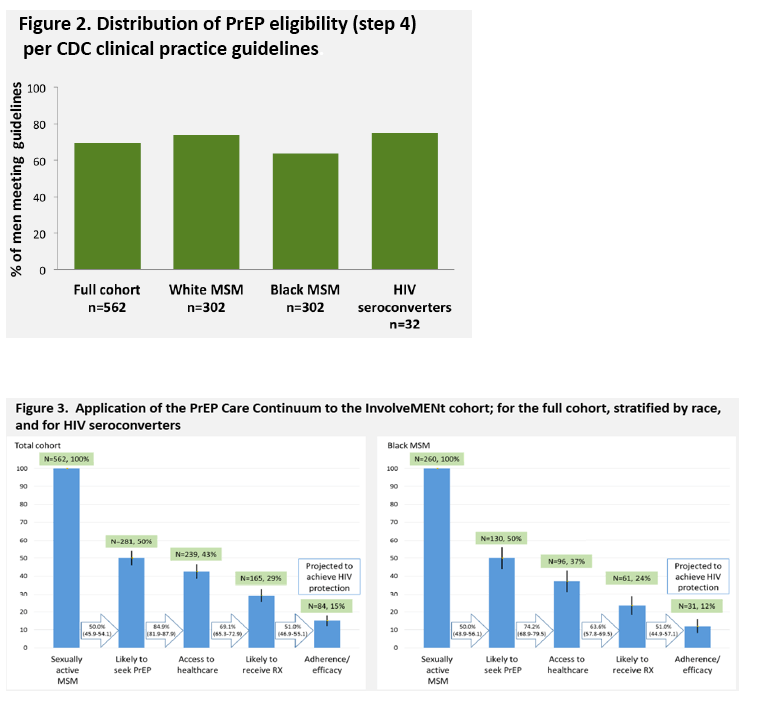
Methods: InvolveMENt was an HIV incidence cohort of 562 black and white sexually active, non-monogamous, HIV-negative MSM in Atlanta, Georgia conducted from 2010-2014 with 32 observed HIV seroconversions, and which was used to apply the PrEP Care Continuum under optimistic estimates. Step 1 included all MSM in this at-risk cohort. Step 2 used awareness/willingness estimates. Step 3 used the percent of cohort men with health insurance or ACA eligibility in GA. Step 4 used the percent of cohort men meeting CDC PrEP eligibility guidelines. Step 5 applied the 51% adherence/efficacy estimate from the iPrex OLE study. Proportions with 95% confidence intervals (CI) of MSM in the total cohort and seroconverters projected to reach each step were calculated. We performed sensitivity analyses for a 20% increase at each continuum step individually and for all steps.
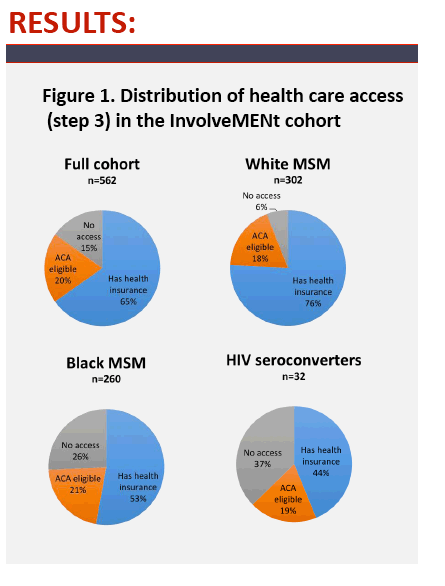
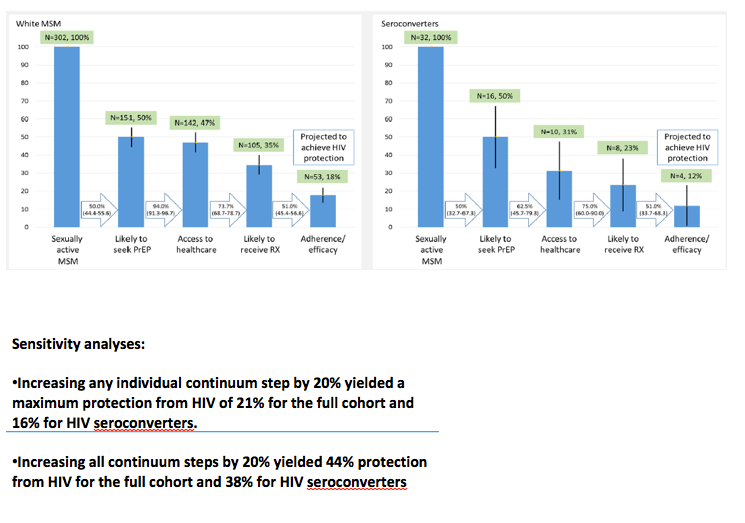
Results: Awareness/willingness was estimated at 50% for both analyses. Sixty-five percent of MSM in the total cohort, and 43% of seroconverters had health insurance; an additional 20% were ACA eligible in both groups. Sixty-nine percent of MSM in the total cohort and 75% of seroconverters met PrEP eligibility guidelines. The PrEP Care Continuum (figure) resulted in 15% (84/562; CI 12, 18%) of the cohort and 13% (4/32; CI 1, 23%) of seroconverters achieving theoretical protection from HIV. Increases in each step individually by 20% yielded a maximum protection of 21% for the cohort and 16% for seroconverters, while increasing all steps by 20% yielded 44% and 38% protection respectively.
Conclusions: Even with generous, 'best-case scenario' estimates, few Atlanta MSM will achieve protection from HIV with PrEP given the significant barriers described in the PrEP Care Continuum. Each step of the proposed continuum represents a critical intervention point. Novel strategies for PrEP delivery are needed to achieve the necessary effectiveness for MSM at risk of HIV.
|
| |
|
 |
 |
|
|