 |
 |
 |
| |
Impact of Specific Antiretroviral Drugs on
Non-AIDS Mortality; the D:A:D Study -
|
| |
| |
LPV, ATV, NVP--But Not EFV--Tied to Higher Non-AIDS Death Rate in D:A:D
CROI 2015, February 23-26, 2015, Seattle, Washington
Mark Mascolini
Analysis of the D:A:D cohort linked cumulative use of lopinavir, atazanavir, or nevirapine to small but significant increases in the non-AIDS death rate [1]. The same analysis tied recent efavirenz exposure to about a 15% lower non-AIDS death rate.
D:A:D is the large ongoing study of antiretroviral-treated people in Europe, the United States, and Australia. Noting previous research that linked protease inhibitor (PI) use to a higher risk of death and non-AIDS diagnoses, the D:A:D team conducted a fresh analysis of their cohort to determine whether individual antiretrovirals affect non-AIDS death risk.
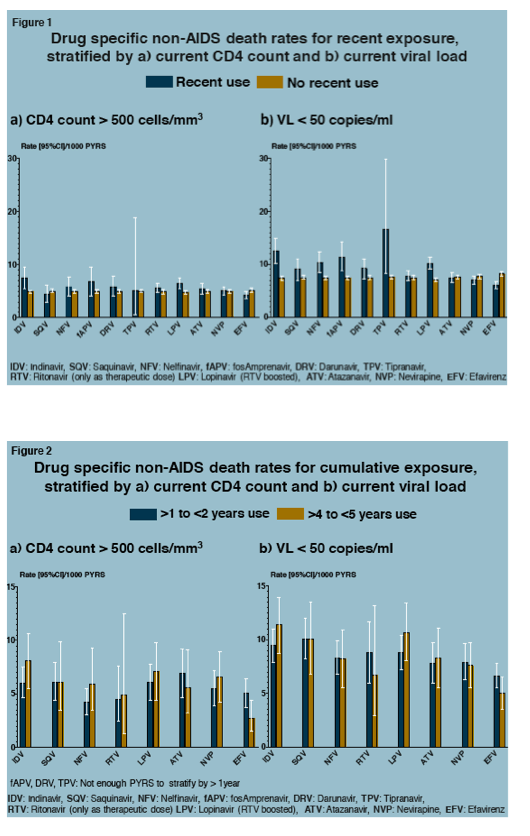
This analysis explored exposure to specific PIs and nonnucleosides in cohort members from when they entered D:A:D to death, January 2013, or 6 months after their last visit, whichever came earliest. The researchers classified antiretroviral exposure as recent (current use or use in the last 6 months) or cumulative (per year of exposure or per 5 years of exposure). They calculated total- and drug-specific non-AIDS mortality within different CD4 count and viral load strata for both recent and cumulative exposure.
Models comparing non-AIDS mortality for recent and cumulative use of specific antiretrovirals adjusted for baseline factors (gender, HIV acquisition mode, and ethnicity) and time-updated factors (age, CD4 count, viral load, HBV/HCV status, smoking, hypertension, diabetes, and calendar year). The researchers assessed the potential impact of nevirapine, efavirenz, and every PI licensed from saquinavir through darunavir. The analysis did not include integrase inhibitors or entry inhibitors.
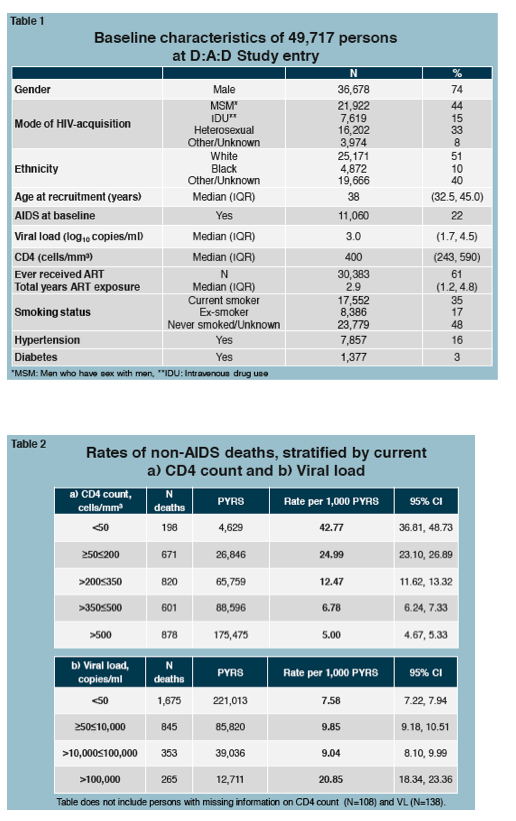
D:A:D investigators checked records of 49,717 cohort member, 74% of them men, 44% gay/bisexual men, 33% heterosexual, and 15% injection drug users. At cohort entry, 61% had already started antiretroviral therapy, median viral load measured 1000 copies, and median CD4 count stood at 400.
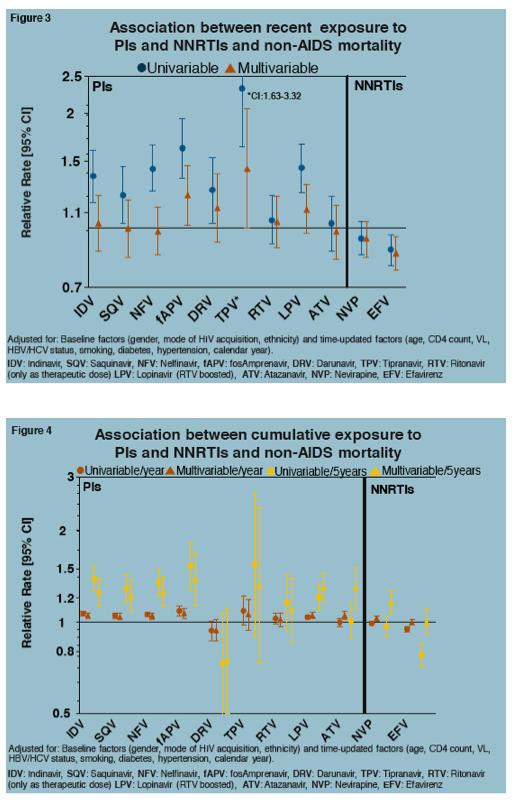
Through more than 370,000 person-years of follow-up, 3276 people died of non-AIDS causes to yield a death rate of 8.8 per 1000 person-year, meaning about 9 of every 1000 people died every year from a non-AIDS disease. After statistical adjustment for baseline risk factors and time-updated risk factors, recent use of fosamprenavir or tipranavir was independently associated with a higher non-AIDS death rate. But this analysis found no associations between commonly used current antiretrovirals and an increased non-AIDS death rate. The analysis tied recent efavirenz use to almost a 15% lower non-AIDS death rate (adjusted relative rate 0.86).
Among commonly used antiretrovirals, multivariable analysis determined that cumulative use of lopinavir, atazanavir, and nevirapine was associated with small but independent increases in non-AIDS mortality. These associations held true for both the 1-year cumulative analysis and the 5-year cumulative analysis. There was a trend toward a lower death rate with darunavir in the 1-year analysis and the 5-year analysis. Cumulative efavirenz use did not affect the non-AIDS death rate one way or the other. These results remained consistent across time-updated CD4 and viral load strata, when analyses were restricted to people currently on antiretroviral therapy, and when analyses excluded unknown causes of death or excluded injection drug users.
The D:A:D team believes their findings "suggest that cumulative exposure to some PI/NNRTIs is associated with a small but increased risk of non-AIDS mortality." The effects were consistent from one PI to the next and comparable to earlier D:A:D findings on non-AIDS events. "Although potential confounding [in such analyses] cannot be ruled out," they concluded, "our results argue for continued pharmacovigilance."
Reference
1. Hatleberg CI, Ryom L, Phillips AN, et al. Impact of specific antiretroviral drugs on non-AIDS mortality; the D:A:D study. CROI 2015. February 23-26, 2015. Seattle, Washington. Abstract 582.
----------------
Reported by Jules Levin
Impact of Specific Antiretroviral Drugs on Non-AIDS Mortality; the D:A:D Study
CI Hatleberg1, L Ryom1, A Phillips2, A Mocroft2, P Reiss3, M Law4, R Weber5, F Dabis6, C Pradier7, S de Wit8 , A d'Arminio Monforte9 , JD Lundgren1, C Smith2
On behalf of the D:A:D Study Group

1CHIP, Department of Infectious Diseases and Rheumatology, Section 2100, Rigshospitalet - University of Copenhagen, Denmark, 2Research Department of Infection and Population Health, UCL, London, UK, 3Div. of Infectious Diseases and Dept. of Global Health,
Academic Medical Center, University of Amsterdam, Amsterdam, Netherlands, 4The Kirby Institute for Infection and Immunity in Society, University of New South Wales, Sydney, Australia, 5Division of Infectious Diseases and Hospital Epidemiology,
University Hospital Zurich, Zurich, Switzerland, 6Univ.of Bordeaux, ISPED, Centre Inserm U0897-Epidemiologie-Biostatistique, Bordeaux, France, 7Department of Public Health, Nice University Hospital, Nice, France,
8Department of Infectious Diseases, CHU St. Pierre Hospital, Brussels, Belgium, 9Department of Health Sciences, San Paolo University Hospital, Milan, Italy



|
| |
|
 |
 |
|
|