 |
 |
 |
| |
The HIV Continuum of Care for Adolescents and Young Adults (12-24 years) Attending 13 Urban US Centers of the NICHD-ATN-CDC-HRSA SMILE Collaborative .........Only 7% of Youth in US Study Reach an Undetectable Viral Load After HIV Diagnosis
|
| |
| |
IAS 2015, July 19-22, 2015, Vancouver
Mark Mascolini
Faster referral to youth-friendly care after HIV diagnosis predicted virologic suppression in 1548 US youth from 12 to 24 years old [1]. But only 7% of the young people in this 2012-2014 study achieved viral suppression, compared with about 40% of adults in the Centers for Disease Control and Prevention (CDC) Medical Monitoring Project.
Researchers from the National Institute of Child Health and Human Development (NICHD), the CDC, and other institutions organized the Strategic Multisite Initiative for the Identification, Linkage and Engagement in Care of HIV-infected youth (SMILE) to connect newly infected young people with youth-friendly care across the country. The investigators noted that people 13 to 24 years old now account for one quarter of new HIV infections in the United States. But data on the continuum of care in this group are scant.
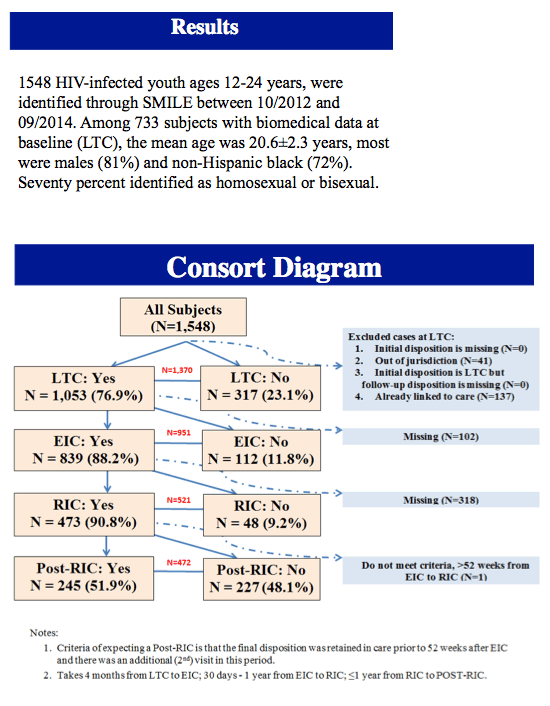
This analysis involved 12- to 24-year-olds in the Adolescent Medicine Trials Network for HIV/AIDS Interventions (ATN) diagnosed with HIV infection and identified through SMILE between October 2012 and September 2014. The investigators defined linkage to care as a record of care within 42 days of HIV referral; they defined engagement in care as 1 or more additional visits within 16 weeks of linkage; and they defined retention as 1 or more additional visits within 52 weeks of engagement. Viral suppression meant a plasma viral load below detection during the study period.
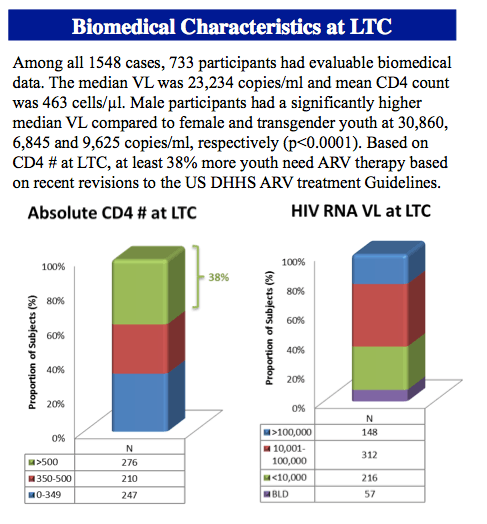
The investigators identified 1548 HIV-infected youth. Among 733 young people with baseline biomedical data, age averaged 20.6 years, 81% were male, 72% were non-Hispanic black, and 70% identified themselves as homosexual or bisexual. Baseline CD4 count averaged 463, and median baseline viral load stood at 23,234 copies/mL. Male participants had a significantly higher median baseline viral load (30,860) than females (6845) or transgender persons (9625) (P < 0.001).
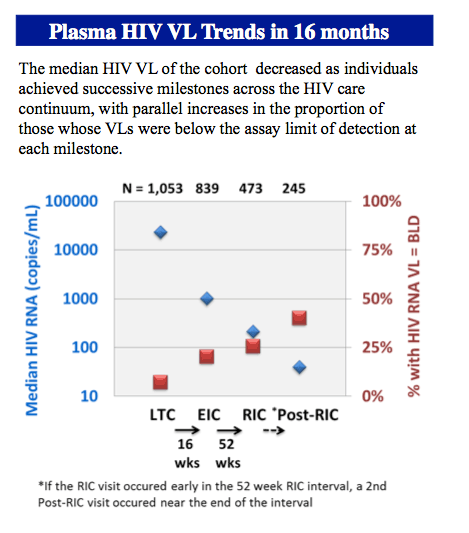
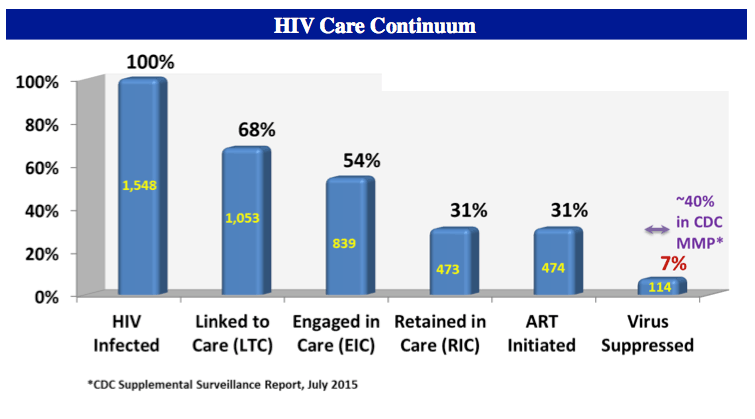
Among the 1548 young people initially identified, 1053 (68%) were linked to care, 839 (54%) were engaged in care, 473 (31%) were retrained in care, 474 (31%) started antiretroviral therapy, and 114 (7%) reached an undetectable viral load during the study period.
Outlining a similar continuum of care for US adults in the Medical Monitoring Project, the CDC reported in 2015 that about 40% of those diagnosed with HIV reached an undetectable viral load. In contrast, linkage rates were similar between youth in this analysis and adults in the Medical Monitoring Project.
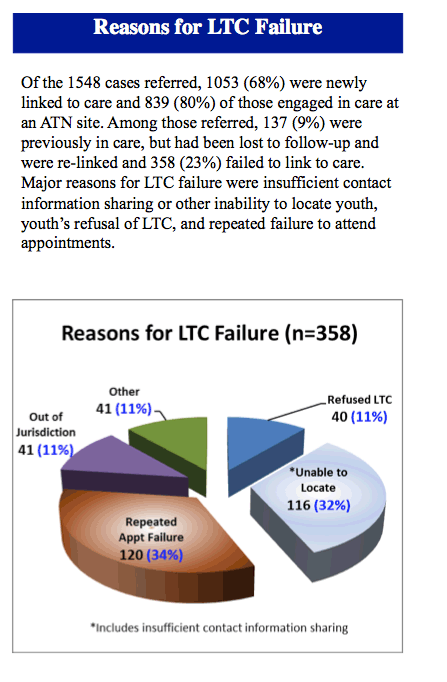
Major reasons for failure to engage young people in care were insufficient contact information sharing, inability to locate youth, refusal of linkage by youth, and repeated failure to keep appointments.
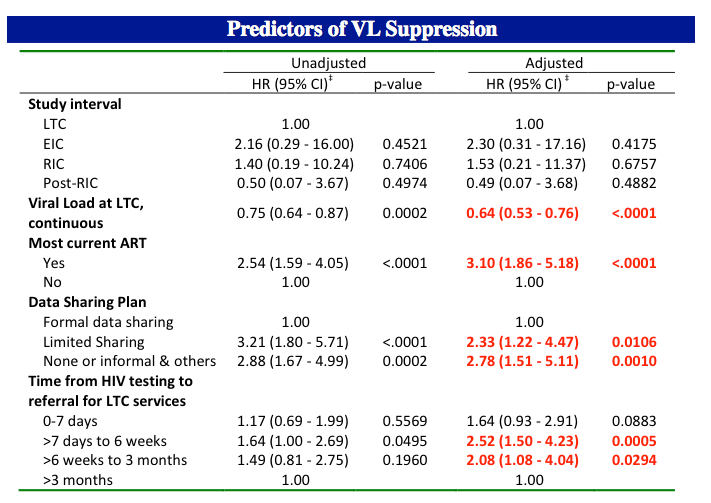
Cox proportional hazards models identified several independent predictors of viral suppression in these young people, including receiving antiretroviral therapy in the time interval before the most recent clinical visit (adjusted hazard ratio [aHR] 3.10, 95% confidence interval [CI] 1.86 to 5.18, P < 0.0001), starting off with a lower viral load at linkage to care (1.56-fold increased likelihood of viral suppression per 10-fold decrease in viral load, 95% CI 1.32 to 1.89, P < 0.0001), and shorter time from HIV testing to referral to care:
Compared with more than 3 months:
-- 0 to 7 days: aHR 1.64 (95% CI 0.93 to 2.91, P = 0.0883, not significant)
-- More than 7 days to 6 weeks: aHR 2.52 (95% CI 1.50 to 4.23, P = 0.0005)
-- More than 6 weeks to 3 months: aHR 2.08 (95% CI 1.08 to 4.04, P = 0.0294)
The NICHD team and collaborators stressed that the high viral loads and advanced HIV infection at baseline "have implications for disease progression and transmission potential." They see an urgent need for interventions "to improve knowledge of undiagnosed HIV infection, access to and retention in care, medication adherence and long-term viral load outcomes in youth."
Reference
1. Kapogiannis BG, Xu J, Mayer KH, et al. The HIV continuum of care for adolescents and young adults (12-24 years) attending 13 urban US centers of the NICHD-ATN-CDC-HRSA SMILE collaborative. IAS 2015. 8th Conference on HIV Pathogenesis, Treatment and Prevention. July 19-22, 2015. Vancouver. Abstract WELBPE16.
-----------------

The HIV Continuum of Care for Adolescents and Young Adults (12-24 years) Attending 13 Urban US Centers of the NICHD-ATN-CDC-HRSA SMILE Collaborative
Reported by Jules Levin
IAS 2015 Vancouver July 19-23
B. Kapogiannis1, J. Xu2, K.H. Mayer3, J. Loeb2, L. Greenberg2, D. Monte2, L.J. Koenig4, M. Banks-Shields5, D. Fortenberry6
and the Adolescent Medicine Trials Network for HIV/AIDS Interventions.
National Institute of Child Health and Human Development (NICHD) / National Institutes of Health (NIH)1, Bethesda, MD; Westat, Rockville, MD2; Fenway Health, Boston, MA3; Centers for Disease Control and Prevention (CDC), Atlanta, GA4; Health Resources and Services Administration (HRSA), Rockville, MD5; Indiana University-Purdue University Indianapolis, Indianapolis, IN6


|
| |
|
 |
 |
|
|