 |
 |
 |
| |
Favourable effects on vitamin D and bone of switching from Atripla to
Darunavir/Ritonavir monotherapy: a randomised controlled clinical trial
|
| |
| |
Reported by Jules Levin
IAS 2015 Vancouver July 19-23
Hamzah, L., Tiraboschi, J.M., Iveson, H., Toby, M, Mant, C. , Cason, J. , Burling, K., Wandolo, E., Jendrulek, I., Dew, T., Kulasegaram, R., Teague, A., Post, F.A., Fox, J.

---------------------------------
Program Abstract
Favourable effect on vitamin D and bone after switching from Atripla to darunavir/ritonavir: a randomised controlled clinical trial
Presented by Lisa Hamzah
L. Hamzah1, J.M. Tiraboschi2, M. Toby2, H. Iveson2, C. Mant1, C. John1, K. Burling3, R. Kulasegaram2, A. Teague2, F.A. Post4, J. Fox2, MIDAS Study Group
1King's College London, London, United Kingdom, 2Guys and St Thomas' NHS Foundation Trust, London, United Kingdom, 3Cambridge University NHS Foundation Trust, Cambridge, United Kingdom, 4King's College Hospital NHS Foundation Trust, London, United Kingdom
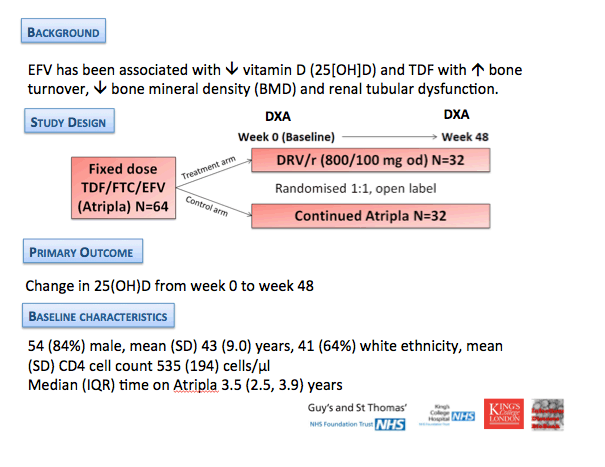
Background: Efavirenz has been associated with reductions in vitamin D (25[OH]D) and Tenofovir with increased bone turnover, reductions in bone mineral density (BMD), and renal tubular dysfunction (RTD). We hypothesized that switching from Atripla to Darunavir/Ritonavir monotherapy (DRV/r) might increase 25[OH]D, and improve BMD and RTD.
Methods: Patients with HIV RNA < 50 copies/mL on Atripla for ł 6 months were randomized 1:1 to receive ongoing Atripla or DRV/r (800/100 mg once daily) for 48 weeks. Primary endpoint was change from baseline in 25[OH]D at week 48. Secondary endpoints included changes in BMD, bone turnover markers and RTD. Linear regression estimated the mean difference in 25[OH]D in patients on Atripla vs. DRV/r. Secondary endpoints were expressed as the mean (95% CI) observed between-arm difference from baseline.
Results: 70 subjects (86% male, 66% white, mean (SD) CD4 cell count 537.3 (191.5) per mm3) were randomized, of whom 26 (DRV/r) and 31 (Atripla) completed the 48 week study on the allocated treatment. The mean (SD) difference between baseline and week 48 25[OH]D was 5.0 (5.9) ng/mmol for DRV/r and 1.2 (6.0) for Atripla. After adjustment for baseline 25[OH]D and demographics, at week 48 DRV/r monotherapy was associated with a +3.5 (95% CI 0.5, 6.4) ng/mmol increase in 25[OH]D compared to Atripla (p=0.02). Subjects in the DRV/r arm experienced increases in BMD (mean between-arm difference (0.02 [0.003, 0.04] g/cm2 at the lumbar spine, p=0.03, and 0.03 [0.006, 0.06] g/cm2 at the neck of femur, p=0.02), and reductions in parathyroid hormone (PTH) (-20.4 [-38.8, -2.0] ng/l, p=0.03), bone-specific alkaline phosphatase (-7.1 [-9.7, -4.5]) IU/L, p< 0.0001) and serum type 1 pro-collagen (-16.9 [-26.5, -7.4] ug/L, p=0.0008), as compared with subjects on Atripla. No significant difference in RTD (urine retinol-binding protein/creatinine ratio and phosphate reabsorption) was observed. Reasons for discontinuation in the DRV/r arm included side effects (n=4) and virus load rebound (n=2), all of which resolved with DRV/r discontinuation or regimen intensification.
Conclusions: A switch from Atripla to DRV/r resulted in significant improvements in 25[OH]D and PTH, and a 2-3% increase in BMD. DRV/r monotherapy provides a bone-friendly treatment option to patients with osteoporosis or increased fracture risk.
-----------------
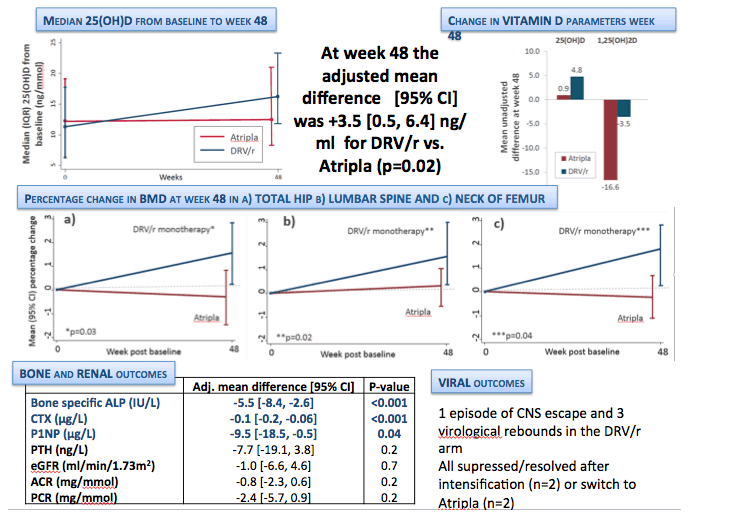
At week 48, 25[OH]D levels were higher in the DRV/r arm compared to the Atripla arm.
This graph demonstrates the median 25(OH)D levels at baseline and week 48, with DRV in the blue and Atripla in the red.
The mean adjusted difference was +3.5 ng/ml for DRV/r compared to Atripla arm and this result was statistically significant
1,25[OH]2D concentrations decreased in both arms, but significantly less in the DRV/r arm.
Subjects in the DRV/r arm also had significant improvements in BMD at all three sites measured; hip, lumbar spine and NOF. You can see in these figures the mean % change in BMD with the DRV arm in blue and the Atripla arm in red
Most bone biomarkers showed significant improvement in the DRV arm at week 48, including ALP, BAP, CTX (a marker of bone reabsortion) and P1NP (a marker of bone formation).
PTH concentrations also improved in the DRV arm, but this did not reach statistical significance in the adjusted analysis.
There were no differences in renal outcomes between arms including eGFR, ACR and PCR. Although the data are not shown here, there was no change in more specific markers of renal tubular function, such as tubular reabsorption of phosphate or urinary retinal binding protein
Overall, we had one case of HIV VL CNS escape presenting with headache and altered mood, and 3 virological rebounds, all these cases were in the DRV arm. All supressed and symptoms resolved after intensification with Truvada or switch to Atripla and there was no documented HIV resistance
In summary, while not always successful virologically, DRV monotherapy may be an attractive strategy for patients on a TDF and EFV containing regimen who have developed osteoporosis or fragility fractures or for those at high risk of developing these complications.
|
| |
|
 |
 |
|
|