 |
 |
 |
| |
Tolerability of integrase inhibitors in a real-life setting - Barcelona
|
| |
| |
More Toxicity Stops With Elvitegravir Than Other Integrase Inhibitors
18th International Workshop on Comorbidities and Adverse Drug Reactions in HIV, September 12-13, 2016, New York
Mark Mascolini
HIV patients at a Barcelona university clinic quit taking elvitegravir less often than raltegravir or dolutegravir in the first year of therapy [1]. But discontinuations for toxicity proved most frequent in people starting elvitegravir in this 1091-patient analysis.
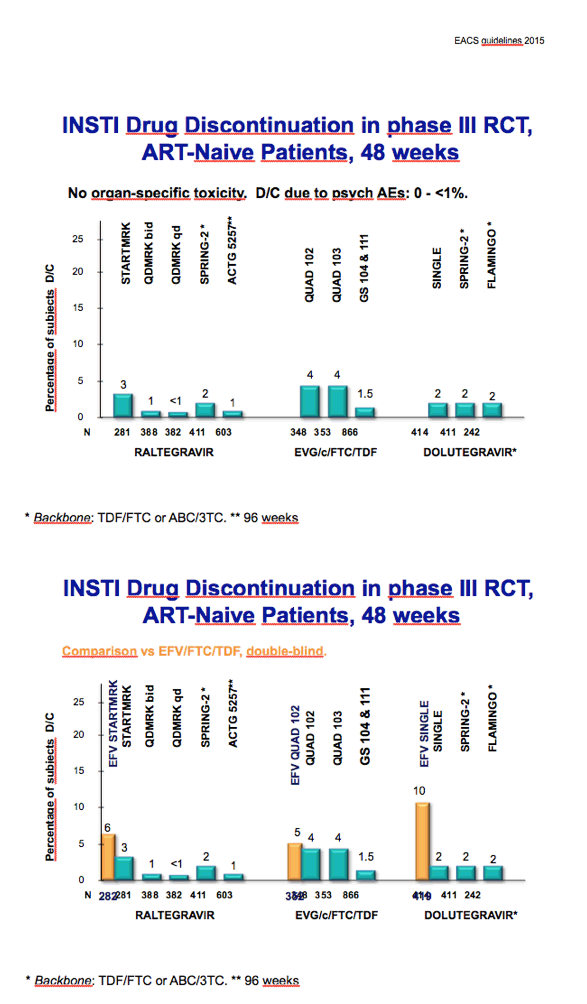
European and US health authorities both recommend each of the three licensed integrase inhibitors as part of first-line therapy. Esteban Martinez and University of Barcelona Hospital Clinic colleagues who conducted this analysis noted that 48-week discontinuation rates lay below 5% in phase 3 trials of antiretroviral-naive people starting any of the three integrase inhibitors. In studies comparing a first-line integrase inhibitor with the nonnucleoside efavirenz, higher proportions of participants always quit efavirenz.
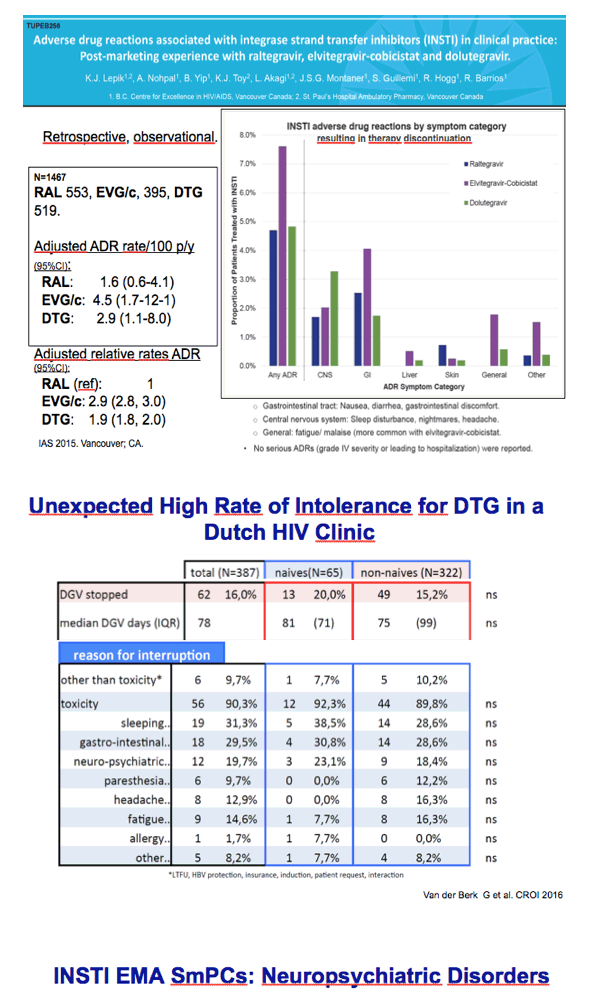
Martinez cited postmarketing data indicating adjusted adverse drug reaction rates of 1.6 per 100 person-years for raltegravir, 2.9 per 100 for dolutegravir, and 4.5 per 100 for elvitegravir/cobicistat. Compared with raltegravir, adverse drug reaction rates were twice higher with dolutegravir (adjusted relative rate 1.9, 95% confidence interval [CI] 1.8 to 2.0) and 3 times higher with elvitegravir (adjusted relative rate 2.9, 95% CI 2.8 to 3.0). An observational study in a Dutch HIV clinic found surprisingly high rates of stopping dolutegravir--20% in first-line regimens and 15.2% in later regimens [2].
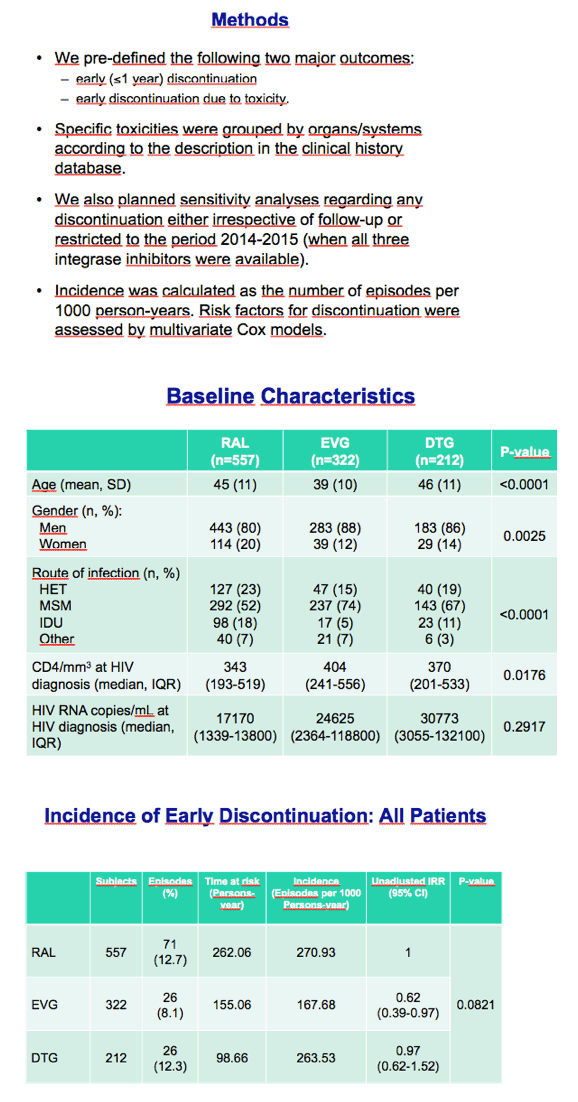
This retrospective analysis involved all antiretroviral-naive or experienced patients who started raltegravir, elvitegravir, or dolutegravir at the Barcelona clinic and who had at least 1 year of follow-up. Treatment-experienced patients had an undetectable viral load when switching to an integrase inhibitor. The investigators aimed to determine how many people stopped their integrase inhibitor during the first year of treatment and how many did so because of toxicity. They used multivariate Cox models to explore risk factors for discontinuation.
The study group included 557 people starting raltegravir, 322 starting elvitegravir, and 212 starting dolutegravir. The raltegravir group included a higher proportion of women (20% versus 12% on elvitegravir and 14% on dolutegravir, P = 0.0025) and had a lower median CD4 count at HIV diagnosis (343 versus 404 versus 370, P = 0.0176). The raltegravir group also included a significantly lower proportion of men who have sex with men and a higher proportion of injection drug users.
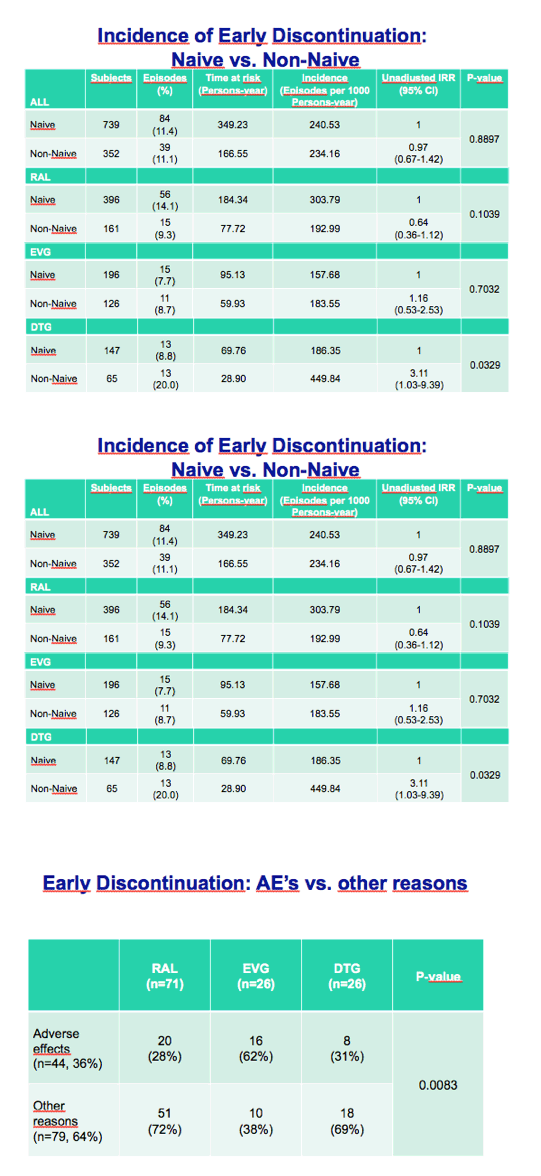
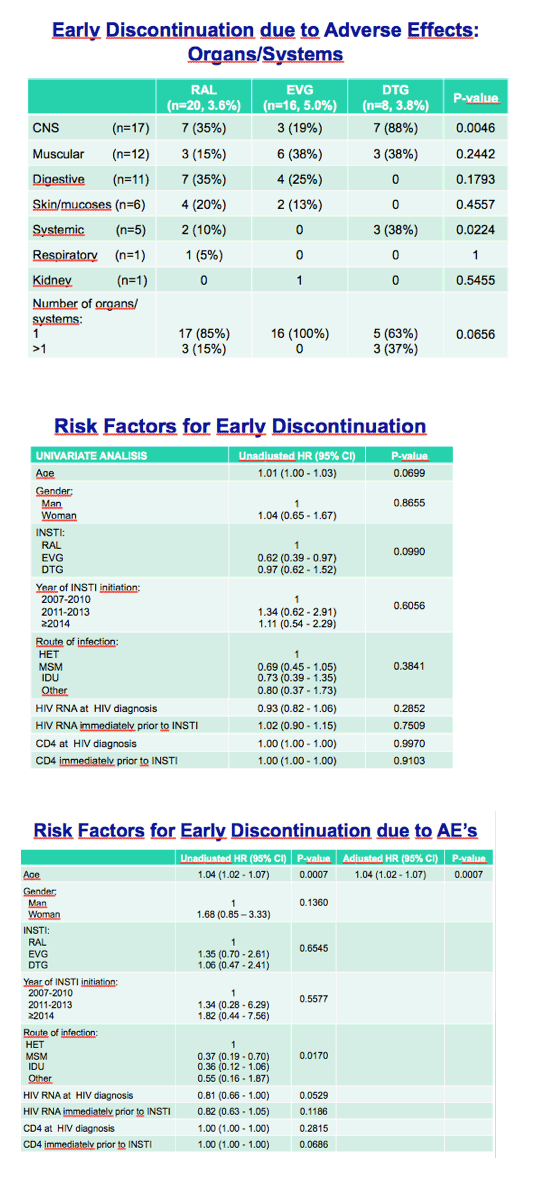
A higher proportion of people stopped raltegravir in the first year (270.9 per 1000 person-years) than stopped elvitegravir (167.7 per 1000) or dolutegravir (263.5 per 1000), a nonsignificant trend in this unadjusted analysis (P = 0.0821). A significantly lower proportion of people quit raltegravir because of adverse events (28%) than quit elvitegravir (62%) or dolutegravir (31%) (P = 0.0083). Central nervous system problems accounted for a significantly higher proportion of discontinuations with dolutegravir (88%) than with raltegravir (35%) or elvitegravir (19%) (P = 0.0046).
The Cox model adjusted for age, gender, integrase inhibitor, route of HIV infection, CD4 count and viral load at diagnosis, and other variables identified only one independent predictor of early discontinuation because of adverse events--older age (adjusted hazard ratio 1.04, 95% CI 1.02 to 1.07, P = 0.0007).
The Barcelona team concluded that a lower proportion of patients tended to quit elvitegravir in the first year than the other two integrase inhibitors. But among the three integrase inhibitors, people quit elvitegravir most frequently because of toxicity. Neuropsychiatric toxicity, however, was more frequent with dolutegravir than with raltegravir or elvitegravir.
References
1. Padilla M, Rojas J, Gonzalez-Cordon A, et al. Tolerability of integrase inhibitors in a real-life setting. 18th International Workshop on Comorbidities and Adverse Drug Reactions in HIV, September 12-13, 2016, New York.
2. van den Berk G, Oryszczyn J, Blok W, et al. Unexpectedly high rate of intolerance for dolutegravir in real-life setting. 2016 Conference on Retroviruses and Opportunistic Infections. February 22-25, 2016, Boston. Abstract 948. http://www.croiconference.org/sessions/unexpectedly-high-rate-intolerance-dolutegravir-real-life-setting


|
| |
|
 |
 |
|
|