 |
 |
 |
| |
DAA-induced HCV clearance does not restore the altered cytokine
and chemokine milieu in patients with chronic hepatitis C.... from Jules: is HCC recurrence associated with lack of benefit associated with Interferon-based therapy? and cytokine response?
|
| |
| |
Reported by Jules Levin
EASL 2016 April 14-17 Barcelona
Julia Hengst* 1, Verena Schlaphoff1, Katja Deterding1, Christine S. Falk2, Michael P. Manns1, Markus Cornberg1, Heiner Wedemeyer1
1Gastroenterology, Hepatology and Endocrinology, 2Institute of Transplant Immunology, IFB-Tx, Medical School Hannover, Hannover, Germany
from Jules: I noted that IFN-2a was lower in SVR vs relapse, is this related to the suggestion in recent published report I distributed finding that HCC recurrence was 28% after SVR & the authors suggesting this might be related to IFN response, that preliminarily it appears recurrence was not seen in interferon-based therapies before DAAs and reference was made to HALT-C....
Unexpected early tumor recurrence in patients with hepatitis C virus -related hepatocellular carcinoma undergoing interferon-free therapy: a note of caution - (04/27/16)
"the use of IFN may have secured the immune cancer control benefits induced by IFN. As an example, interferons are known to exert an antiproliferative effect by prolongation of all phases of cell cycle, have extrinsic effects on tumors by regulation of angiogenesis and, moreover, can regulate the activity of almost all immune cell types (including macrophages, dendritic cells, B cells, T cells and innate lymphocytes), creating a well-orchestrated immune response against infectious and malignant diseases. Indeed, it seems that IFN therapy is more effective at targeting disseminated cancer cells and minimal residual disease (MRD) before they form large proliferative metastases, suggesting that promoting antitumor immunity, rather than an antiproliferative response, is the likely mechanism of action[29]......Meissner et al demonstrated that HCV clearance achieved during treatment with sofosbuvir and ribavirin is accompanied by hepatic downregulation of type II and III IFNs, their receptors, and interferon stimulated genes (ISGs)[31]. This might have a negative impact on immune cancer control. In the same study, the authors show that HCV patients able to reestablish IFN homeostasis by the end of treatment with SOF/RBV may be more likely to achieve a sustained virological response (SVR), whereas patients who fail to restore homeostasis may be more prone to viral relapse."
EASL: Development of Hepatocellular Carcinoma in HCV Cirrhotic Patients Treated with Direct Acting Antivirals - (04/25/16)

Program abstract
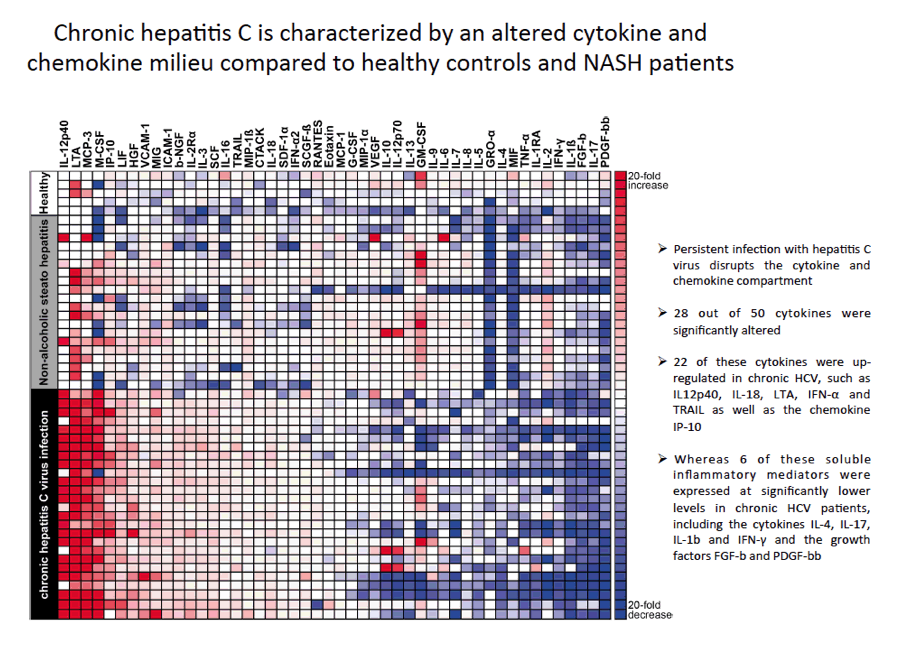
Background and Aims: Persistent infection with the hepatitis C virus (HCV) is accompanied by an inflammation of liver tissue and a profound alteration of the cytokine/chemokine milieu (CCM) in the peripheral blood. The natural course of chronic hepatitis C (cHC) shows a high inter-individual variability in progression to liver fibrosis and cirrhosis. Whether these progressions are influenced by an altered CCM is unclear. Moreover, it is unknown to what extent the CCM is restored by interferon-free antiviral therapy.
The aim of this study was to investigate to what extent the CCM is altered in cHCV infection, to identify potential cytokines/chemokines associated with viral infection vs. stage of liver disease and to analyze whether DAA-treatment restores this milieu.
Methods: We performed multianalyte profiling of 50 cytokines and chemokines in the plasma of patients with persistent HCV infection using the BioPlex bead array method. A total of 27 patients were recruited, who were treated for 24 weeks with sofosbuvir and ribavirin. Samples were collected longitudinally during therapy and after treatment cessation. All patients had advanced stages of liver fibrosis or cirrhosis, roughly 40% of the patients experienced a viral relapse after end of therapy. Principle component analysis was performed to identify networks of interactions and associations.
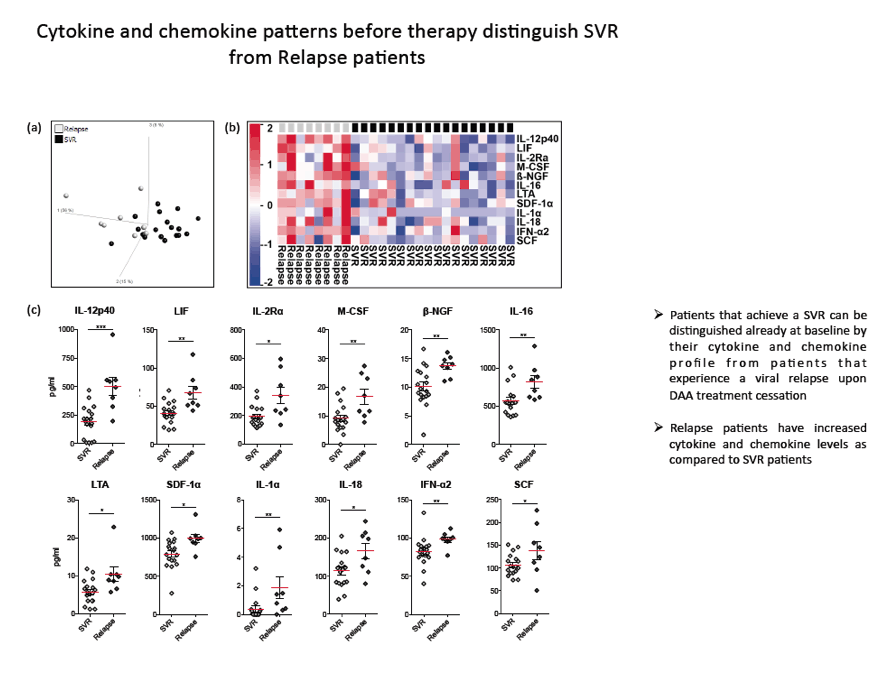
Results: We found that (I) the CCM was markedly altered in cHC patients compared to healthy controls and individuals with nonalcoholic steatohepatitis; (II) CCM patterns and distinct cytokines and chemokines were associated with the level of fibrosis (fibroscan values) (e.g. HGF, IL-18) while others were driven by inflammation or viral replication (HGF, IFNγ, VCAM-1, or GRO-α, IP-10, TNF-β); (III) SVR and relapse patients could be differentiated by several baseline cytokine and chemokine levels, i.e. IL-12p40, IL-16, IFN-α2 and TGF-β; (IV) significant changes of the CCM could be observed during therapy, however the CCM pattern was not normalized even in SVR patients for the majority of parameters.
Conclusions: In conclusion, our results show that cHCV infection appears to disrupt the cytokine/chemokine compartment and that these alterations persist even after viral clearance. Thus, HCV cure does not lead to immunological restitution. Further, CCM patterns may be used to individualize treatment duration with novel DAAs as some cytokines and chemokines were associated with treatment outcome.
|
| |
|
 |
 |
|
|