 |
 |
 |
| |
Development of Hepatocellular Carcinoma in HCV Cirrhotic Patients Treated with Direct Acting Antivirals
|
| |
| |
Reported by Jules Levin
EASL 2016 April 14-17 Barcelona
Federica BUONFIGLIOLI1, Fabio CONTI1, Pietro ANDREONE1, Cristina CRESPI2, F. Giuseppe FOSCHI3, Marco LENZI1, Giuseppe MAZZELLA1, Gabriella V

Program abstract
DEVELOPMENT OF HEPATOCELLULAR CARCINOMA IN HCV CIRRHOTIC PATIENTS TREATED WITH DIRECT ACTING ANTIVIRALS
Federica Buonfiglioli* 1, Fabio Conti1, Pietro Andreone1, Cristina Crespi2, Francesco Giuseppe Foschi3, Marco Lenzi1, Giuseppe Mazzella1, Gabriella Verucchi1, Stefano Brillanti1
1DIMEC, University of Bologna, 2Medicina Interna, Policlinico S.Orsola-Malpighi, Bologna, 3Medicina Interna, Ospedale di Faenza, Faenza (RA), Italy
Introduction: Therapy of chronic hepatitis C with direct-acting antivirals (DAAs) is able to induce a sustained virological response (SVR) in over 85% of patients, even if liver cirrhosis is present. Eradication of HCV infection should prevent the development of major complications, including hepatocellular carcinoma (HCC). At our referral centre, we analysed the whole cohort of patients with liver cirrhosis treated with DAAs in order to evaluate whether HCV eradication affects the development of HCC.
Material and Methods: Between March and November 2015, 344 consecutive HIV negative patients with HCV-related Child-Pugh A/B cirrhosis, without active HCC, were treated with DAAs: Sofosbuvir+Simeprevir (34%), 3D combination (22%), SOF+Ribavirin (17%), SOF+Daclatasvir (16%), SOF+Ledipasvir (10%). Ribavirin (RBV) was added at the physician's discretion according to weight. Occurrence of HCC was assessed by contrast enhanced-ultrasonography and MR/CT-scan during the six-month post-treatment follow-up period.
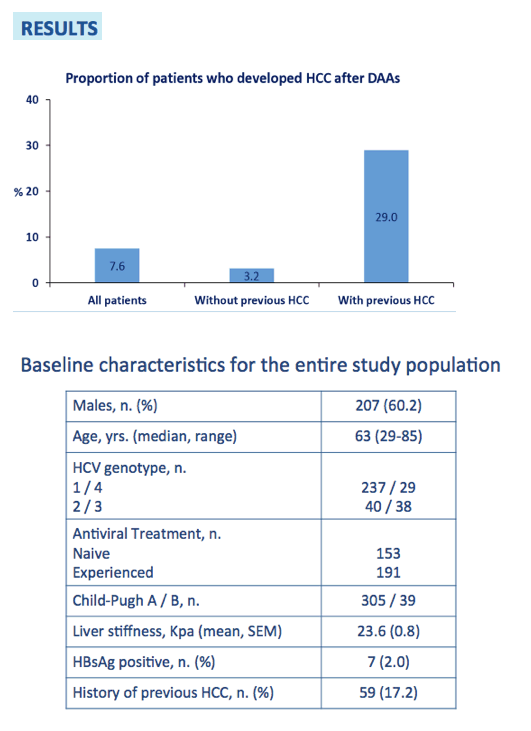
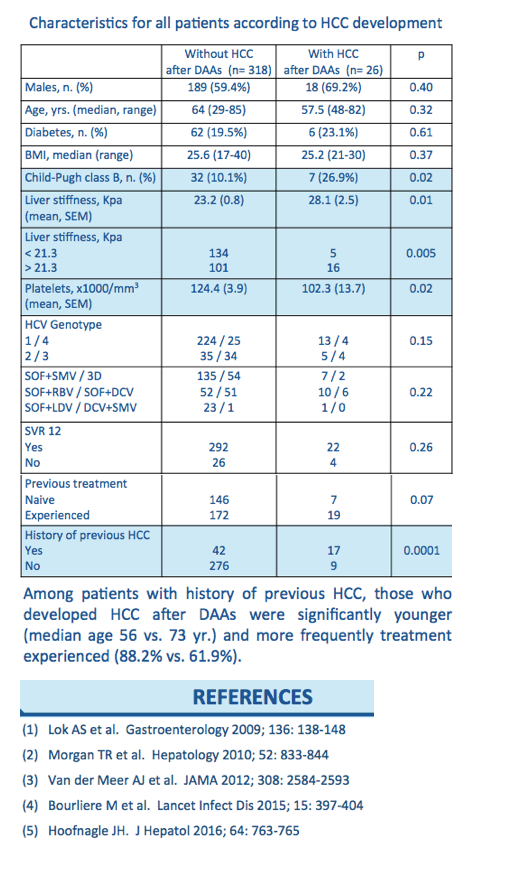
Results: Median age was 63 years (29-85) and 60% were males. The majority (69%) had genotype 1 infection; 55% had experienced previous treatment failure to PegIFN+RBV. History of previous HCC, treated with TACE and/or RFA, without evidence of active neoplastic lesion by MR and/or CT-scan, was present in 59 patients (17%). At 12-week follow-up, SVR was achieved in 89% of patients. Between treatment end and 24-week follow-up, active HCC was detected in 26 patients (7.6%): median age was 58 years (48-82), M/F ratio was 19/7 and Child-Pugh class was A in 19 (73%). A single nodule was detected in 21 (81%) and multiple nodules in 5 (19%). HCV genotype 1 infection was found in 13 patients (1a/1b: 6/7), genotype 2 in 5, genotype 3 in 4, and genotype 4 in 4. 22/26 (85%) had SVR. HCC developed in 17 (29%) of the 59 patients with a history of previous HCC. Among those without history of HCC, novel HCC was detected in 9 (3.2%). At the time of HCC detection, alphafetoprotein (AFP) was increased (>50 ng/mL) in only 2/26 (8%).
Conclusion: In this large retrospective cohort study on cirrhotic patients treated with DAAs, we observed a high rate of HCC recurrence and a standard rate of HCC occurrence in a relatively short follow-up observation. Development of HCC was rarely associated with increase in AFP levels. Cirrhotic patients should be closely monitored after treatment, and the biological significance of our findings deserve further investigations.

|
| |
|
 |
 |
|
|