| |
NYC HCV Plan
NYC DOH: HEPATITIS C in NEW YORK CITY
|
| |
| |
Download the PDF here -
State of the Epidemic
and Action Plan
2013 - goals: public-provider
awareness/screening/surveillance/linkage-to-care/engage NYS
Some of you know I designed the NYC "Check Hep C" project about 5 years ago, raised $2 million in funding and gave these to the NYC DOH to implement. Jules
As many as 3.5 million Americans and 146,500 New York City residents may have chronic
hepatitis C (HCV).
HCV is a leading cause of death for people with HIV.8 Nationwide, deaths from HCV-related
disease - hepatic and extrahepatic - now surpass those caused by HIV.9 In New York City,
the Health Department's Bureau of Vital Statistics has estimated that the age-adjusted rate
for HCV-related deaths per 100,000 population increased by approximately 46% from 1999
to 2011. During the same period, HIV-related deaths decreased by approximately 60%
(Figure 1). If current trends continue, HCV-related deaths in New York City also will surpass
those from HIV within the next couple of years.
From Jules: We now have after 20 years of research ad billions of dollars new HCV treatment regimens approved by the FDA in the last 2 years that can cure HCV in 90-100% of patients, with newer more effective pangenotypic regimens in development in large global phase 3 studies with higher cure rates.
Federal funding for public health surveillance of HCV infections and for prevention
activities, case management, and treatment has been extremely limited. Of the 2011 funds
allocated by the Centers for Disease Control and Prevention's (CDC) National Center for
HIV/AIDS, Viral Hepatitis, STD, and TB Prevention (NCHHSTP), only 2% were for viral
hepatitis.10 Moreover, Congress has never passed legislation that provided safety net access
to HCV care and treatment for persons without health insurance, as the Ryan White Care
Act did for persons living with HIV. In 2010 and 2011, respectively, the Institutes of Medicine
(IOM) and Department of Health and Human Services (DHHS) published comprehensive HCV
needs assessments and action plans, articulating detailed strategies for controlling the HCV
epidemic (Figure 2).11,12 Federal budgets, however, have not included the investments
needed to implement them.
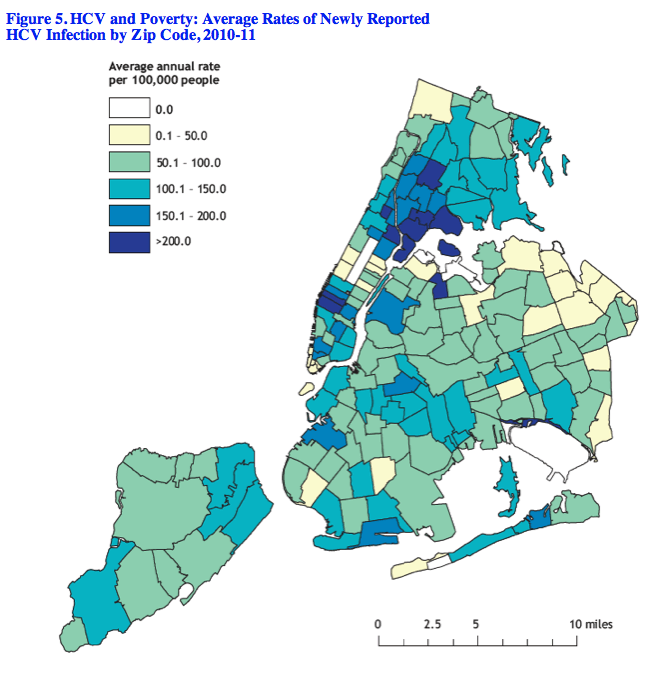
The disease is most prevalent in New York City neighborhoods with high
poverty.
The annual number of deaths
associated with HCV has been increasing yearly and, since 2007, has exceeded deaths
associated with HIV in the U.S.
It is estimated that approximately 50% of people living with HCV are unaware that they are
infected. Having ever injected drugs - even once in the remote past - is the most
frequently reported risk factor.
This action plan identifies 7 public health objectives to address the HCV epidemic in New
York City. Of them, the following 5 objectives are most critical for reducing illness and
death from HCV in New York City. They will be prioritized depending on available resources.

The New York City eligible metropolitan area received $121 million in Ryan White funding
from HRSA in FY 2011 to provide HIV-related programming.134 In view of the number of
people infected with HCV and the number of preventable deaths from HCV, federal funding
should similarly be provided to treat people with this infection.
More than 3 million New York City residents participate in
Medicaid.
Approximately 50%......are
unaware that they are infected with HCV.
PWID may be less likely to seek health care than other populations.
The New York State Department of Health began its support of New York City SEPs in 1992,
and funding has continued since then. Since 2003, the Injection Drug Users Health Alliance
(IDUHA), a coalition of community-based syringe access providing health services to
injection drug users in New York City, has successfully advocated for additional funding for
syringe exchange and other harm reduction/prevention services, including HCV screening,
HCV prevention education and referral for treatment, HAV and HBV vaccination, overdose
prevention, methadone and buprenorphine referral, and linkage/navigation to other clinical
care services.
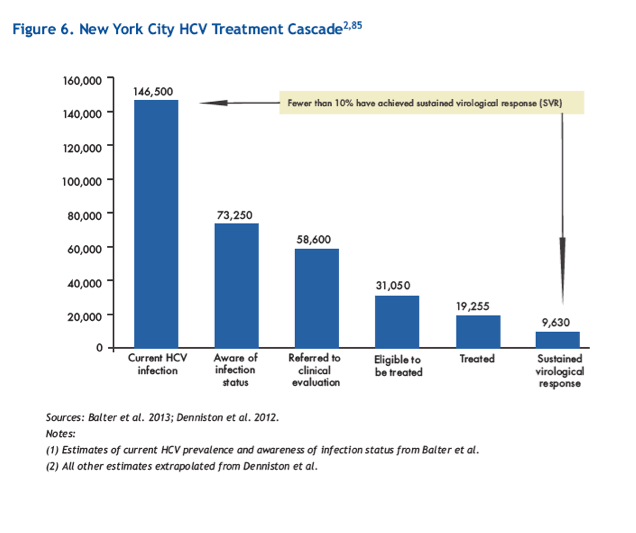
Figure 6 (page 33) illustrates that of the roughly 73,000 persons
in New York City living with HCV who are aware of their
infections, only a small proportion, approximately 13%, have
been cured. As elsewhere in the U.S., there are likely to be
structural, patient-, and provider-level barriers that interfere
with linking New Yorkers with current HCV infection to
appropriate care, including assessment for antiviral treatment.
The goal of the Check Hep C Program has been to demonstrate that persons living with HCV
in urban settings, many of whom are disproportionately poor, marginalized and lack
adequate access to medical resources, can be medically managed and treated effectively
and in a way that is both cost-containing and culturally competent. In its first year, the
program screened and tested 4,751 persons; 880 (18.5%) were seropositive for HCV
antibody. Of the 512 persons diagnosed with current HCV infection, 433 (84.5%) attended
their first appointment with an HCV provider. [I designed Check Hep C & raised $2 mill funding and gave the design & funding to NYC]
The Health Department
has not systematically assessed HCV incidence in two populations with emerging risk: MSM
who are HIV-infected and engage in unprotected, high-risk sexual activities23-25 and
adolescents and young adults who have started to inject drugs.
The Racial and Ethnic Approaches to Community Health
across the US Risk Factor Survey (REACH US RFS), a cross-sectional
study conducted 2009-2010........Approximately 70% of Hispanics and non-Hispanic blacks who reported injection drug use
were tested for HCV and roughly 80% reported HCV infection. However, of all persons who
reported risk factor, only 40% were tested for HCV and 65% of the Asians who reported
injection drug use were not tested for HCV. This suggests that a large number of racial and
ethnic minorities with HCV risk factors are not being tested and that the actual HCV
prevalence is likely to be higher than what has been reported
1. Enhance health provider awareness regarding screening, diagnosis, and
referral for HCV infection and clinical providers' capacity to manage and
treat HCV.


4. Enhance linkage to care of persons with current
HCV infection, identify and promote successful
models of care, and build clinical capacity to manage
and treat HCV.....
Many patients with HCV face social barriers, behavioral health issues or have co-occurring
medical conditions that make it challenging for them to initiate and remain in HCV-related
medical care. The Health Department proposes to work with health care facilities, care
management agencies, health homes and managed care in New York City to improve care
coordination. When persons living with HCV are released from custody, correctional
facilities will be encouraged and assisted to link them to health care providers in their
communities who can manage and treat HCV.
If tested, diagnosed and linked to appropriate care, the extent of liver damage could be
assessed and steps taken (e.g., HAV and HBV vaccination and liver health counseling)
to prevent additional hepatic damage.
It is likely that disparities in health care access limit the extent to which persons living with
HCV in New York City are linked to appropriate medical care. Most persons newly diagnosed
with current HCV infection live in neighborhoods with high levels of poverty and where
many residents lack health insurance and access to other resources
5. Engage and collaborate with the New York State Department of
Health and other state agencies and other relevant organizations
to develop, promote, and advance policies and regulations that
will support the goals of this strategy
This might include expanding the HCV-related services reimbursed by Medicaid (e.g., lab and other
diagnostic tests, patient navigation, drug treatment and antiviral medications), or changing lab test
reporting requirements for clinical laboratories and drug treatment programs.
The health
care sector also will be engaged to ensure the development and implementation of quality
control/assurance metrics related to HCV care and that network capacities are sufficient to
manage and treat HCV.
In 2010, 9,992 persons were newly reported with a positive HCV antibody or viral RNA test.
Of these, 65% were male, and 56% were 40 to 59 years of age. The greatest number of newly
reported HCV cases occurred in neighborhoods with high proportions of residents living in
poverty. Of all boroughs, the Bronx had the highest rate with 155 newly-reported HCV cases
per 100,000 persons. Among the 42 United Hospital Fund neighborhoods, those with the
highest rates included Hunts Point (227 per 100,000), Highbridge-Morrisania (205 per
100,000), East Harlem (318 per 100,000), and Central Harlem (221 per 100,000) (Figure 5).3
Among 165 persons newly reported and followed up by interviews from 2009 to 2011,
65% were black or Hispanic. Most (73%) were born in the US; the next most common
countries of birth were Haiti (4%), the Dominican Republic (4%), Russia (3%), and Pakistan (3%).
In NYC-HANES, non-Hispanic blacks were more than twice as likely to be seropositive for
HCV as non-Hispanic whites, Hispanics, or Asians (4.4%, 1.9%, 1.2%, and
1.8%, respectively). The socioeconomic factors significantly associated with HCV
seroprevalence were high school education or less, public assistance, and a history of ever
being incarcerated as an adult.61
Since most persons with chronic HCV were infected through
injection drug use, syringe exchange programs (SEPs) have
contributed greatly to a dramatic reduction in HIV transmission
among PWID.67-71 They are essential, but relying solely on this
harm reduction strategy is unlikely to have the equivalent impact
with HCV, which appears to have greater infectivity than other
bloodborne pathogens.
-----------------------------------
A PUBLIC HEALTH MODEL FOR REDUCING
ILLNESS AND DEATH FROM HCV INFECTION
IN NEW YORK CITY
Given that the current and anticipated disease burden from HCV infection in New York City
will soon rival that of HIV/AIDS, the Health Department has developed an action plan to
address this epidemic. Its primary goal is to reduce the morbidity and mortality from HCV
with the following measures:
1. Prevent HCV transmission and new infections;
2. Diagnose persons living with HCV, link them to appropriate care, and cure current HCV
infections with effective treatments;
3. Decrease complications and deaths from chronic HCV infections; and
4. Reduce disparities in prevalence and access to care and treatment among persons
infected with HCV.





|
|
| |
| |
|
|
|