| |
Survival of patients with HCV cirrhosis and sustained virologic response is similar to the general population.... Treated hepatitis C virus (HCV) cirrhotic patients can have normal life expectancy
|
| |
| |
Download the PDF here
"In conclusion, eradicative treatment of patients with compensated HCV cirrhosis is strongly justified since the achievement of SVR originates a major survival benefit, with a life expectancy similar to the general population. In patients with compensated HCV cirrhosis, treatment should be administered as early as possible in order to achieve the highest benefit."
Treated hepatitis C virus (HCV) cirrhotic patients can have normal life expectancy
The fact that a sustained virologic response (SVR) is associated with an improved outcome of chronic HCV infection, has been demonstrated in several studies by comparing patients with and without SVR. The study by Bruno et al., however, is the first to demonstrate that patients with compensated cirrhosis who achieve SVR will have a life expectancy similar to that of the sex- and age-matched general population. Patients were enrolled in historical prospective cohort studies from tertiary referral centers from Northern and Southern Italy. They were representative of the Italian general population, allowing for adequate comparison of patients long-term 10- and 20-year survival with national data. Intriguing observations of a trend to worse survival was observed in patients with compensated cirrhosis Child-Pugh class A6 as compared to A5. The incidence of hepatocellular carcinoma (HCC) during follow-up after SVR was also not negligible, underscoring the need for early treatment initiation, hereby preventing cirrhosis development as the main HCC determinant
----------------------------
Survival of patients with HCV cirrhosis and sustained virologic response is similar to the general population
Jnl of Hepatology June 2016
Savino Bruno1,⇑, Vito Di Marco2, Massimo Iavarone3, Luigi Roffi4, Andrea Crosignani5, Vincenza Calvaruso2, Alessio Aghemo3, Giuseppe Cabibbo2, Mauro Viganò3, Vincenzo Boccaccio1, Antonio Craxí2, Massimo Colombo3, Patrick Maisonneuve6
1Humanitas University and IRCCS Istituto Clinico Humanitas, Rozzano, Italy; 2Sezione di Gastroenterologia e Epatologia, DIBIMIS, Università degli Studi di Palermo, Palermo, Italy; 3UO Gastroenterologia ed Epatologia, Fondazione IRCCS Ca’ Granda Ospedale Maggiore Policlinico di Milano, Università degli Studi di Milano, Milan, Italy; 4Dipartimento di Medicina, A.O. Istituti Clinici di Perfezionamento, Milan, Italy; 5Dipartimento di Medicina Interna, A.O. San Paolo, Milan, Italy; 6Division of Epidemiology and Biostatistics, European Institute of Oncology, Milan, Italy
Background & Aims
Life expectancy of patients with compensated hepatitis C virus (HCV) cirrhosis achieving sustained virologic response (SVR) is limited by liver events as compared to the general population. Thus, survival benefit of SVR remains to be measured.
Methods
The study includes prospective surveillance data from three cohorts of Italian patients with compensated HCV cirrhosis who achieved SVR on an interferon-based (IFN) regimen, compared to simultaneously observed non-SVR, untreated and decompensated patients. Overall survival was calculated from the date of start of IFN to death. The number of deaths expected during the at-risk period was determined by applying age- and sex-specific mortality rates recorded in Italy for person-years adequate for the enrolment period. The standardized mortality ratio (SMR) determined the relative risk of death over that of the age and sex matched general population.
Results
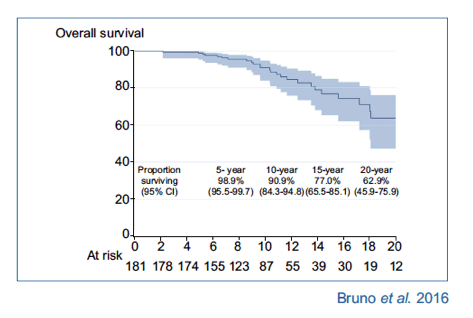
Overall, 28/181 patients followed-up for a median period of 9.6 years (range 1-25 years) died. The 10 and 20-year overall survival rates for the whole series were 90.9% (95% CI, 84.3-94.8) and 62.9% (95% CI, 45.9-75.9), respectively. The number of expected deaths in the corresponding age and sex matched general population was 28.1, corresponding to a SMR = 1.00 (95% CI, 0.72-1.35), with an SMR for non-SVR patients of 3.85 (95% CI, 3.43-4.30), for untreated of 3.01 (95% CI, 2.64-3.42) and for decompensated of 6.70 (95% CI, 5.39-8.22).
Conclusions
Patients with compensated HCV cirrhosis achieving SVR by IFN obtain a main benefit levelling their survival curve to that of the general population. Wider applicability of IFN-free regimens will possibly make this achievement more generalizable.
Introduction
Cirrhosis and liver events such as decompensation or hepatocellular carcinoma (HCC) developing in the long-term after infection with hepatitis C virus (HCV) still represent the main cause of death and liver transplantation in Western countries [1]. The current international guidelines give the highest priority for treatment with new direct antiviral agents (DAA) to HCV-infected individuals who have already reached the stage of cirrhosis [[2], [3]]. This choice is based on the favourable outcome of cirrhotic patients who obtained sustained virologic response (SVR) after interferon-based therapies (IFN) [[3], [4], [5]]. However, the improved prognosis associated to virologic response [[4], [5], [6]] was documented exclusively by comparing SVR patients with cirrhosis to similar patients unsuccessfully treated by IFN. As a result, several concerns have been raised about the real value of SVR, as a reliable marker of disease outcome, because selection biases and other hidden confounders may have limited the consistency of the reported results. Hence the actual survival benefit of obtaining SVR is yet at least partly unexplored, due to the lack of pairing of patients with compensated HCV cirrhosis to their appropriate comparators (treated patients without SVR, untreated patients and patients with decompensated disease) and of a comparison to an age and sex matched general population. Since treatment of cirrhosis with DAA has now become the absolute standard of care, such information can assist in justifying priority in the vast allocation of financial and healthcare resources devoted to these patients [7].
Patients and methods
Patients
The study includes prospective surveillance data from three independent cohorts of Italian patients with compensated HCV-related cirrhosis who underwent an IFN-based therapy in tertiary liver centres and achieved SVR.
The first cohort (Milan-1) included all patients with either compensated (Child-Pugh class A5 to A6) or decompensated (Child-Pugh B7 to B9) HCV cirrhosis who consecutively attended three liver centres in the Milan area between January 1989 and December 1992, as previously reported [[8], [9]]. The second cohort (Milan-2) included compensated cirrhosis patients (Child-Pugh class A5 to A6) consecutively seen at the Liver Unit Fondazione IRCCS Ca' Granda, Ospedale Maggiore in Milan from January 1997 to December 1997 [10]. Patients with decompensated cirrhosis were recorded, as well, but their follow-up observation was not planned in this study. Both Milan cohorts included treated and untreated patients because of co-morbidities, ineligibility to IFN-based therapy or refusal. The third cohort (Palermo) included all cirrhotic HCV patients (Child-Pugh class A5 to A6) enrolled at the Liver Unit (Dipartimento Biomedico di Medicina Interna e Specialistica of the University of Palermo) who started IFN-based antiviral therapy from January 2002 to December 2009 [11]. Patients excluded or ineligible to treatment and those with decompensated cirrhosis or previous decompensation were recorded but their follow-up observation was not planned in this study (Fig. 1).
Briefly, before starting IFN, the diagnosis of cirrhosis (F4 METAVIR, F5-6 Ishak) was either made by a liver biopsy or on clinical criteria. Notably, no patients with non-cirrhotic advanced fibrosis (F3 METAVIR, F3-4 Ishak) were included in any cohort. Anti-HCV, HCV RNA, including genotype, liver function tests were assessed by commercially-available standard methods in all cases. Co-morbidities including diabetes and history of alcohol intake (confirmed by relatives) were also recorded in dedicated datasets. All patients had Child-Pugh score determined according to established criteria [12]. Concurrent HCC was assessed by fine needle liver biopsy or by imaging, following clinical guidelines [[13], [14]]. Patients with any other than HCV cause of liver disease, were excluded. All enrolment criteria should have been carefully satisfied in the three cohorts.
Surveillance, treatment and outcome
IFN mono-therapy or IFN (pegylated or not) in combination with ribavirin were administered according to the standardized criteria that were current at the time of evaluation [15]. SVR was defined as undetectable serum HCV RNA by PCR at week 24 after the treatment cessation. SVR patients followed a surveillance protocol based on clinical, laboratory and abdominal ultrasound every 6 months. Esophago-gastro-duodenoscopy examination was planned at an annual interval for patients with varices and every three years or when clinically required for those free of varices at study entry. Until 2001, patients with a newly detected liver focal lesion underwent computed-tomography (CT) and ultrasound-guided fine needle biopsy, and after 2001 the diagnosis of HCC was made according to the Barcelona Conference and AASLD criteria [[13], [14]]. Portal hypertension complications, such as ascites, gastrointestinal bleedings and hepatic encephalopathy were treated following international guidelines.
Patients’ vital status and cause of death were recorded during patients’ surveillance. For patients lost to follow-up, vital status was updated in 2015 by phone call or in case of non-response by contacting their electronic residential town hall registry offices.
Data collection and analysis was already approved by the local Institutional Review Committees at the time of enrolment for the above mentioned purposes.
Statistical analysis
The main study outcome was overall survival (OS). OS was calculated from the date of enrolment (untreated patients) or from the date of initiation of antiviral therapy (treated patients) to the date of last follow-up or death. OS curves were plotted using the Kaplan-Meier method and survival between groups was compared with the Log-rank test. The number of deaths expected during the at-risk period was determined by applying age- (within 5-year groups) and sex-specific mortality rates recorded in Italy for the general population [16] in 2000 for person-years accumulated before 2005 and rates recorded in 2009 for person-years accumulated from 2005 onward. We used the standardized mortality ratio (SMR), defined as the ratio of the number of deaths observed to the number of deaths expected, to estimate the relative risk of death. We calculated 95% confidence intervals (CIs) for the SMR assuming that the observed deaths followed a Poisson distribution. All analyses were performed with the SAS software (version 9.2, Cary, NC). All analyses were two-tailed and p values <0.05 were considered statistically significant.
Results
The flow chart of the study, according to the Strobe recommendations for observational studies, is presented in Fig. 1.
In detail, Milan-1 cohort included 465 patients with both compensated (198 treated and 154 untreated) and 113 with decompensated disease. Milan-2 cohort included 306 compensated patients (153 treated and 153 untreated). 101 patients with decompensated disease were recorded but not followed-up. Palermo cohort included 444 treated compensated patients. 265 patients excluded from treatment and 220 with decompensated disease were recorded but not followed-up (Fig. 1).
Overall, 795 (44.1%) of 1802 patients with HCV-related cirrhosis in the three cohorts received IFN-based antiviral therapy. 434 patients (24.1%) were not treated because of decompensated disease and 572 (31.7%) compensated patients for comorbidity, ineligibility or refusal.
A total of 181 patients (40 in Milan-1, 33 in Milan-2 and 108 in Palermo) achieved SVR (10.0% overall or 22.8% among treated patients). Their characteristics are presented in Table 1. In 144 (79.6%) patients the diagnosis of cirrhosis was histologically proven.
Patients received antiviral treatment at a median age of 59 years (range 30 to 74 years) and 119 (65.7%) were men. 154 patients (85.0%) had Child-Pugh class A5 disease.
Forty-eight patients (22.7% in Child-Pugh A5 and 48.1% in Child-Pugh A6) had oesophageal varices at baseline, and 88 (48.6%) where infected with HCV genotype 1. We observed no differences in age, sex or Child-Pugh score, while the HCV genotype 1 prevalence varied (37.1%, 24.2% and 62.0%, respectively) among cohorts. Vital status was available for 176 (97.3%) of the patients in June 2015. For the five patients lost at follow-up, who moved to other residential area, follow-up was censored at their last visit. During a median follow-up of 9.6 years (16.3 years for Milan-1, 12.9 years for Milan-2, and 8.1 years for Palermo cohort) 28 patients died with no difference across cohorts (with respectively 15 deaths during 636 person-years of observation in the first cohort, four deaths during 427 person-years of observation in the second cohort, and 9 deaths during 863 person-years of observation in the third cohort (Log-rank p = 0.32) (data not shown)). The 10- and 20-year OS were 90.9% (95% CI, 84.3-94.8) and 62.9% (95% CI, 45.9-75.9) respectively (Fig. 2A), with no difference between sexes (Log-rank p = 0.12), Child-Pugh classes (Log-rank p = 0.12) or genotypes (Log-rank p = 0.69) (data not shown).
During follow-up, 11 patients developed decompensation (two after HCC) (Fig. 2C) and 18 liver related deaths (including four orthotopic liver transplantations) occurred (Fig. 2B). The 10- and 20-year cumulative incidence of decompensation and liver related death were respectively 5.2% (2.6-10.2) and 13.6% (6.3-28.2), 7.1% (4.0-12.7) and 23.3% (12.6-40.8).
Twenty patients developed HCC (16 in Child-Pugh A5 and 4 in Child-Pugh A6). The 10- and 20-year cumulative incidence of HCC was 10.3% (6.1-17.0) and 23.7% (14.4-37.6) respectively (Fig. 2D). During follow-up, 8 of the patients with HCC died, three (15%) underwent liver transplant. Of interest, all patients with HCC who received liver transplant are still alive after respectively 9, 10 and 13 years.
Table 2 shows the predictors of outcome (OS, liver related deaths, decompensation and HCC) in patients with SVR at univariate analysis. At multivariate analysis, only advanced age and low-platelets count were associated with OS; male gender, low albumin and low platelets count were associated with liver related deaths; low albumin and low platelets count were associated with decompensation; while alpha-fetoprotein level was the single predictor of HCC (Table 3).
Corresponding curves of observed vs. expected mortality in matched general population for treated patients without SVR, (SMR = 3.85 (95% CI, 3.43-4.30)), untreated patients (SMR = 3.01 (95% CI, 2.64-3.42)) and decompensated patients (SMR = 6.70 (95% CI, 5.39-8.22)), respectively are presented in Fig. 3B-D.
Discussion
We report herein that survival of patients with HCV compensated cirrhosis who achieve SVR is similar to that of the sex and age matched general population, hence achieving the maximal survival benefit and an optimal allocation of resources.
A few unique points of our study should be stressed. First, we included only patients with definite diagnosis of cirrhosis while those with advanced fibrosis were excluded. Inclusion of F3 patients, as in the retrospective study by van der Meer et al. [7], would conceivably reduce the number of disease events and enhance confounding factors. Moreover, we included patients enrolled in historical prospective cohort studies from tertiary referral centres from Northern and Southern Italy [[8], [9], [10], [11]], representative of the Italian general population. This allowed us to perform an adequate comparison of SVR patients’ survival with national data, thus avoiding the main limitation of the previous study [7]. Lastly and most relevant, the long duration of follow-up allows to report long-term (10- and 20-year) survival rates in cirrhotic patients achieving SVR, similar to those of non-cirrhotic patients previously reported with a shorter observation period [7]. Of note, antiviral therapy was generally offered to middle-aged patients (50 to 60 years), in an age fascia where life expectancy exceeded 20 years, thus making our surveillance period adequate for event recording.
A major issue is the fact that the eligibility criteria to receive IFN may originate from an under-representation of co-morbidities otherwise prevalent in the age matched general population. Moreover, the majority of patients enrolled in our study with previous alcohol intake stopped drinking at the time of starting treatment. These concerns may be at least in part balanced by the notion that HCV eradication is associated with numerous extrahepatic benefits which might have, indeed, led to a reduced overall mortality [17]. Furthermore, some patients developed decompensated cirrhosis or HCC after SVR and a few of them died of liver related disease, which represents a rare cause of death in the general population. Accordingly, in our opinion, the small excess of liver related deaths is likely offset by the small deficit of deaths due to incidental co-morbidities, observed during the initial follow-up period.
Another crucial result provided by this study is that the incidence of HCC during the follow-up of SVR patients was not negligible, thus confirming previous reports with smaller sample size or shorter follow-up time [[4], [5], [6]]. However, no patient with HCC who received orthotopic liver transplantation died, mainly due to the lack of graft re-infection which limited the progression of fibrosis over time. This observation confirms that antiviral treatment should be administered as early as possible thus avoiding the occurrence of cirrhosis, which is the main determinant of HCC development. Of interest, we also documented that alpha-fetoprotein values remain the most powerful predictor of tumour development. This would suggest that patients with borderline alpha-fetoprotein elevation are those most at need of immediate treatment with IFN-free regimens.
As expected, we observed a worse survival trend in compensated patients who had lower functional scores (Child-Pugh Class A6) at study entry. This outcome, not statistically significant due to the low likelihood of a Child-Pugh 6 in patients to be offered an IFN-based regimen, is attributable to the residual mortality observed in this sicker population in whom, irrespective to SVR, portal hypertension may still progress leading to end-stage liver disease.
Albeit the OS of SVR patients with compensated cirrhosis matches that of the general population, due to the low rate of viral clearance by IFN regimens and to the residual liver events, this result is obtained at a major cost for the healthcare system. The societal burden would be needlessly severe if costly resources such as IFN-free DAA combinations are used in unselected patients with competing causes of death. According to our data, untreated and non-SVR patients with compensated HCV cirrhosis are 3- to 4-fold more likely to die than comparable persons from the general population. Hence we may speculate that this population is highly likely to benefit from DAAs. Whether this phenomenon will be the case also for decompensated patients in whom the point of no return of the disease might have been already reached remains to be established.
Some limitations of our study are typical from multicenter historical cohort studies. The present analysis was not planned at the time the cohort was established. As a result, only Milan-1 assessed the outcome of decompensated patients, and Palermo followed only treated compensated patients. Second, in patients with compensated cirrhosis, baseline characteristics slightly differ between centres (see Table 1). Patients were enrolled in different regions in Italy and at different time periods, distinguished by different treatment protocols or patients management guidelines. Nevertheless, we did not observe any statistically significant differences in outcome across centres at multivariate analysis.
In conclusion, eradicative treatment of patients with compensated HCV cirrhosis is strongly justified since the achievement of SVR originates a major survival benefit, with a life expectancy similar to the general population. In patients with compensated HCV cirrhosis, treatment should be administered as early as possible in order to achieve the highest benefit. Availability of IFN-free DAA regimens will allow for an SVR to be achieved even in sicker patients and in those ineligible for IFN or previously excluded for co-morbidities, a major advance given that the mortality rate of these patients is extremely high in comparison to the general population. Since a failure in modifying the disease course in decompensated cirrhosis irrespective to viral eradication was recently reported in almost half of all treated subjects [18], with some patients seemingly beyond a point of no return even after viral eradication, the overall impact of SVR remains to be assessed in further dedicated studies.
|
|
| |
| |
|
|
|