 |
 |
 |
| |
Should Anal Cancer Screening Get More Aggressive for Some MSM With HIV?
- HPV-related disease in HIV-infected MSM with and without recent HCV
|
| |
| |
97% with HCV had High Risk HPV....nonsignificantly higher proportion of men with than without HCV had HSIL (43.9% versus 34.7%, P = 0.20)
IDWeek 2016, October 26-30, 2016, New Orleans
Mark Mascolini
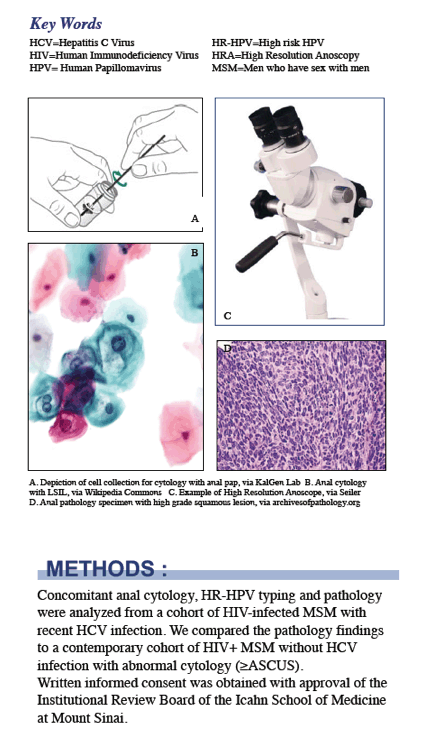
High-grade squamous intraepithelial lesions (HSIL) proved frequent in HIV-positive men with recent HCV infection, even in some with normal anal cytology (cells tested by anal pap) [1]. Researchers from New York City's Icahn School of Medicine at Mount Sinai, who conducted this large comparative analysis, suggested that initial screening with high-resolution anoscopy rather than cytology may be appropriate for high-risk HIV-positive MSM.
HIV-positive MSM run an increased risk of anorectal infection with high-risk human papillomavirus (HR-HPV), which can lead to HSIL and then, in some cases, to anal cancer. The United States has no anal cancer screening guidelines because research has yet to yield evidence that detecting and treating precancerous lesions prevents anal cancer. Epidemics of sexually transmitted HCV infection have struck MSM in the United States, Europe, and other places. Because HCV and HPV share an anal transmission route, the Mount Sinai team conducted this study to analyze the impact of recent HCV infection on rates of HPV-related anal abnormalities in MSM with HIV.
The researchers compared anal cytology (pap test) and pathology findings in two groups of MSM screened at the same institution during the same period: (1) HIV-positive MSM who have condom-free anal sex and recently acquired HCV infection, and (2) HIV-positive MSM without HCV infection. The 60 HCV-positive men were referred to Mount Sinai between January 2010 and September 2014 and had picked up HCV within the past year, probably through anal sex rather than sharing injecting equipment. All these men had anal pap testing for cytology and high-risk anoscopy with biopsy for pathology, regardless of cytology findings. The 1710 HIV-positive but HCV-negative comparison group had anal pap testing between April 2009 and September 2014 as part of a separate study. If anal cytology was normal, they underwent continued cytology at regular intervals. They underwent high-resolution anoscopy if the cytology indicated ASCUS, ASC-H, LSIL, or HSIL.*
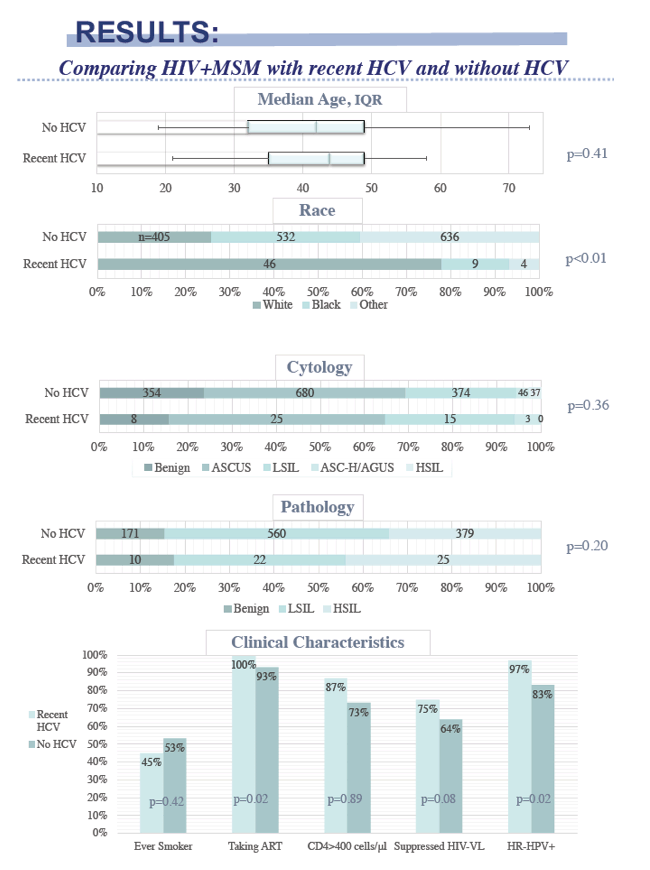
The HCV-positive and negative groups did not differ substantially in age (medians in the low 40s) or proportion of smokers (45% and 53%, P = 0.42). Men with HCV were more likely to be white (78% versus 26%, P < 0.01). Antiretroviral use was high in both groups but significantly higher in the men with HCV (100% versus 93%, P = 0.02); the same was true for CD4 count (656 versus 599, P = 0.02) and proportions with an undetectable viral load (75% versus 64%, P = 0.08).
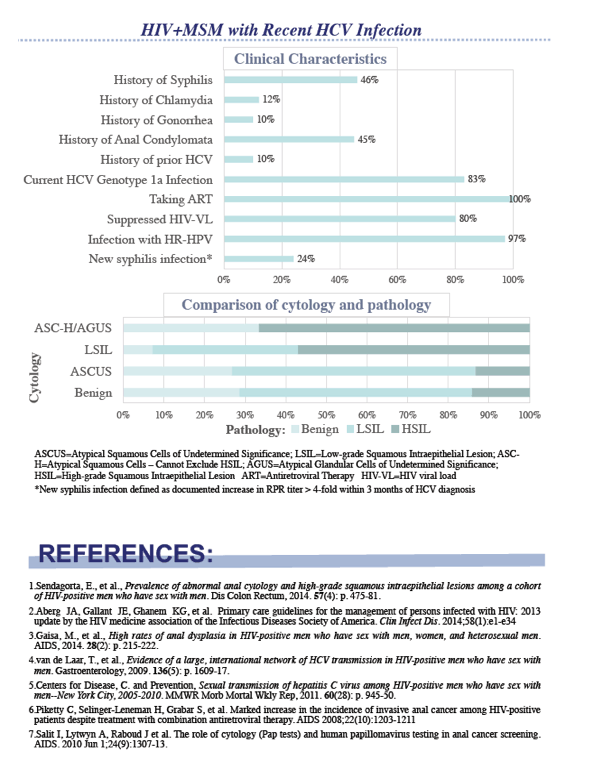
High proportions of both groups of MSM had at least one detectable HR-HPV type, though prevalence was nearly universal in the HCV group but not in the non-HCV group (97% versus 83% of specimens tested, P = 0.02). Although MSM with HCV had higher CD4 counts than men without HCV and had anoscopy regardless of pap cytology results, a nonsignificantly higher proportion of men with than without HCV had HSIL (43.9% versus 34.7%, P = 0.20). In the HCV group, 14% with benign anal cytology and 48% with ASCUS had HSIL detected by anal biopsy.
The researchers suggested that more sex or more high-risk sex in men with recent HCV than in those without HCV could account for their infection with two sexually transmitted viruses (HCV and HPV) instead of only HPV and could have increased their risk of infection with more HR-HPV types that might lead to HSIL. Alternatively, they could have had HPV-related rectal lesions that boosted their risk of HCV infection.
The Mount Sinai team stressed that "an alarmingly high proportion of participants with benign or ASCUS cytology had HSIL pathology," a finding suggesting the current screening practice-- annual anal cytology screening followed by high-resolution anoscopy if abnormal--"may be inadequate" for MSM with HIV. They suggested that HIV-positive men with recent sexually transmitted infections, including HCV, might be offered high-resolution anoscopy for initial screening--both because of their high rates of HSIL and because of the low sensitivity of anal cytology to detect HSIL.
Reference
1. Jacobson K, Michael Gaisa M, Sigel K, Foster A, Fierer D. HPV-related disease in HIV-infected men who have sex with men with recent hepatitis C virus infection. IDWeek 2016, October 26-30, 2016, New Orleans. Abstract 2135.
*ASCUS, atypical cells of undetermined significance; ASC-H, atypical squamous cells, cannot rule out HSIL; LSIL, low-grade squamous intraepithelial neoplasia; HSIL, high-grade squamous intraepithelial neoplasia.
-----------------
HPV-related disease in HIV-infected MSM with and without recent HCV




|
| |
|
 |
 |
|
|