 |
 |
 |
| |
Summary from CROI 2017 for Viral Hepatitis
- HCV elimination on its way: dream or emerging reality?
|
| |
| |
Jurgen K. Rockstroh M.D., Professor of Medicine
University of Bonn, Germany
Correspondence:
Prof. Dr. J.K. Rockstroh
Department of Medicine I
University of Bonn
Sigmund-Freud-Str. 25
53105 Bonn
Germany
Introduction
At this year CROI in Seattle hardly any new results from new direct acting antivirals (DAA) in phase-3 clinical studies in hepatitis C mono- or coinfected patients were reported. Clearly, with the multiple DAA combinations currently available, allowing treatment for all HCV genotypes, the urge for developing further new agents has become less pressing. With HCV cure rates above 95% for almost all patient populations the bigger question becomes whether increased uptake and roll-out of DAA therapy can actually change HCV epidemiology and curve the epidemic. Targeting HIV-coinfected MSM appears a promising strategy towards HCV elimination as patients are well characterized and regularly seen for CD4-count and viral load checks allowing early HCV diagnosis. Indeed data was presented from the Netherlands suggesting that with broadening of inclusion criteria for DAA therapy for all HIV/HCV-coinfected patients independent of fibrosis stage, an almost 50% decline in new cases of acute HCV in the MSM population has been observed (1,2). The recently reported alarming finding of an HCV reinfection rate of almost 25% among HIV-seropositive European MSM clearly underlines that the current outbreak of acute HCV among HIV-infected MSM is still not under control in most countries and raises the question whether indeed increased roll-out of HCV therapy may change this (3). Other important feedback at CROI was around real-life efficacy and safety data in all kind of different patient populations as well as new insights into the risk of developing hepatocellular cancer (HCC) after achieving cure of HCV (sustained virological response 12 weeks after stopping HCV therapy; SVR12)(4-9). Also new data was presented on long-term treatment of hepatitis B with tenofovir containing regimens showing surprisingly high HBs-Ag clearance rates of above 15% in HIV/HBV coinfected patients (10). Moreover, interesting trial data was shown which demonstrated a protective effect of tenofovir as pre-exposure prophylaxis for preventing HCV vertical transmission in high risk HBV infected mothers with high HBV viral load (11). In summary, this year CROI was much less about new drugs but really more around current HCV management issues in the modern DAA era, barriers in receiving DAA therapy and eventually the impact of highly successful DAA therapy on HCV elimination.
Does increased roll-out of DAA therapy lead to a decline in new acute HCV infections among HIV+MSM?
Very interesting data was presented from the Netherlands from the ATHENA cohort which captures 98% of all Dutch HIV-patients (1). Overall, 22,042 HIV-positive patients were screened at least once for HCV with 2422 HCV-RNA positive subjects. Hereof 407 showed spontaneous clearance, 306 died, 60 moved abroad, 118 were lost to follow-up and 111 had their positive HCV RNA test never confirmed. Therefore, 1420 HCV/HIV+ patients
who were in care and alive in May 2016 represented the entire study population (1). Of note DAA therapy became available in the Netherlands in 2014 as telaprevir or boceprevir based HCV therapy but still in combination with PEG-IFN +/- ribavirin. Later in 2015 all oral DAA combination therapy was introduced. Of note initially DAA based HCV was only accessible in F3/F4 fibrosis stages. From November 2015 onwards all HCV patients could receive DAA therapy and there were no longer fibrosis stage restrictions. Overall, 1171 patients had HCV therapy initiated, 1127 completed HCV therapy and 939 achieved an SVR. The HCV treatment cascade is depicted in figure 1.
Figure 1: HCV treatment cascade
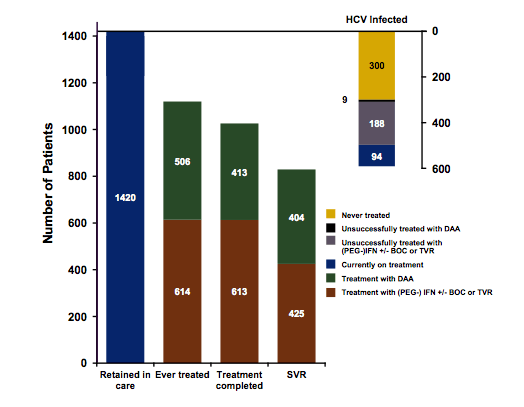
Of note, in January 2017, 70% of all HIV/HCV coinfected patients had either achieved SVR12 or were currently still on DAA therapy. Within the MSM HIV/HCV coinfection group even 76% had achieved SVR or were on current DAA therapy. Lower cure rates and therefore in remaining need of HCV therapy were in particularly females, ex-IVDU and patients with uncontrolled HIV-infection. Clearly, well described patient populations with limited numbers are ideal for studying HCV elimination strategies. Therefore, in their second oral presentation the Dutch colleagues examined the change in incidence of acute HCV among HIV-coinfected MSM (2). The analysis was performed via the Dutch Acute HCV in HIV Study group (DAHHS) which studies new therapies for acute HCV in a network of 8 HIV centers. Including referral of patients with acute HCV from other HIV centers ± 50% (2014) and 65% (2016) of patients with acute HCV in the Netherlands were included into these studies. The DAHHS study 1 was conducted in 2014 in acute HCV genotype 1 patients only which received 12 weeks of peginterferon + RBV + boceprevir. Overall, 86% of patients achieved SVR under this combination (49/57) (12). The DAHHS study 2 started in 2016 and is still ongoing. Patients with acute HCV infection, either with genotype 1 or 4 infection, receive grazoprevir + elbasvir for 8 weeks. So far 58 patients have been enrolled. Most interestingly, the incidence of acute HCV dropped from 11.2/1000 PYFU (95% CI 9-14) in 2014 to 5.5/1000 PYFU (95% CI 4-7) in 2016 (see figure 2).
Figure 2: Results: Change in acute HCV incidence between 2014 and 2016

These results are very encouraging and suggest that indeed with high HCV treatment coverage for chronic but also acute HCV infection a change in number of reinfections can be expected. Of note a look at other STDs in the same observation period showed that 629 syphilis cases were recorded in the first 6 months of 2016 which represents a 41% increase over the previous year underlining that the observed decline in acute HCV infections was not following a general trend of less STDs all together. German data from the GECCO cohort which also looked at reinfection rates in their large mixed HCV mono- and HIV/HCV coinfected cohort (n=1483) showed a reinfection rate of 11% in HIV positive MSM (19/166) after a median follow-up of 45 weeks versus only 1% in IVDU (5/454) after a median follow-up of 40 weeks (13). These results potentially also suggest a current decline in new acute HCV cases at least in comparison to the 25% reinfection rate from the European cohort (3). The very low reinfection rate in IVDU emphasizes that with corresponding harm reduction measures namely opioid substitution therapy as well as clean needle and syringe distribution programs reinfections can be successfully prevented.
CROI: Unrestricted Dutch Athena Cohort (HIV+/MSM/IDU) DAA Access Leads to Speedy Uptake, High Cure Rates ....'51% decrease in acute HCV, increased STD rates/syphillis'
CROI: HCV REINFECTION AFTER SUCCESFUL DAA TREATMENT -A GECCO ANALYSIS - 11% HIV+ MSM
What else is new around acute HCV in HIV-positives?
A further study on acute HCV cases was presented from the Swiss Cohort. Within their HCV elimination study (Swiss HCV free trial) 87% of all MSM participating in the Swiss Cohort study were screened for HCV with PCR. Most interestingly, increased screening efforts led to the identification of 31 incident cases (14). Of note, of these new cases 21% had a negative HCV antibody test but positive HCV-PCR underlining that in case of suspected acute HCV infection performance of an antibody test alone will miss some newly infected patients. Clearly HCV-RNA determination will be useful in this setting. Also two patients were identified with acute HCV and normal liver transaminases indicating that even in patients with normal liver enzymes a newly acquired HCV infection can be present. This is important, as most screening recommendations are based on elevated liver transaminases. Considering the overall high risk of acute HCV infection in HIV-positive MSM annual or even biannual HCV screening clearly is recommended. Figure 3 summarizes the corresponding findings of the Swiss cohort study.
Figure 3: Swiss Cohort: Routine PCR-based HCV Screening
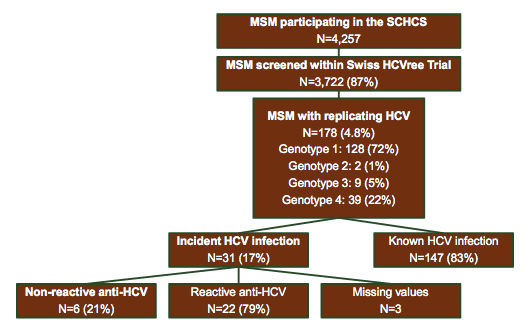
CROI: A Systematic HCV-RNA Screening in HIV+ MSM Reveals a High Number of Potential Transmitters: 5% HCV Prevalence, 17% acute HCV incidence, higher rates of condomless sex, IDU, syphillis
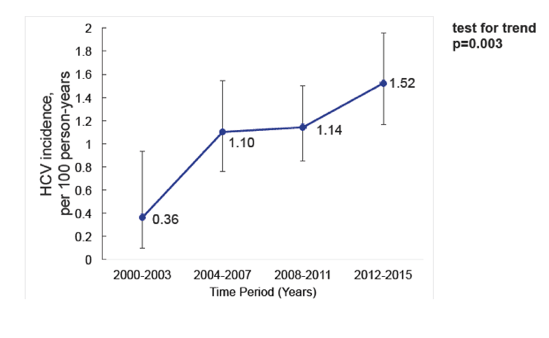
Further studies on the incidence of acute HCV among HIV-positive MSM was presented for San Diego. The study population consisted of HIV-positive MSM who attend the largest HIV clinic in San Diego, had a negative anti-HCV test sometime from 2000 through 2015, and had at least one more anti-HCV or HCR RNA test during follow-up through 2015. The researchers defined incident HCV as any positive anti-HCV or HCV RNA result after a negative anti-HCV test. Overall, 2395 MSM with a median age of 38 were included; two thirds were white, 10% black, and 26% Hispanic. While 42% of men reported methamphetamine use, another 5% both used meth and injected drugs. Figure 4 shows the increase in acute HCV incidence among HIV+ MSM in San Diego. Compared with men who never used meth or injected drugs, meth-only users had a tripled risk of HCV acquisition (incidence rate ratio [IRR] 3.024, 95% confidence interval [CI] 1.860 to 5.132, P < 0.001), men who only injected drugs had a 13-fold higher risk (IRR 13.167, 95% CI 1.497 to 53.965, P < 0.001), and drug injectors who also used meth had almost a 5-fold higher risk (IRR 4.896, 95% CI 2.401 to 9.644, P < 0.001). HCV acquisition risk did not differ significantly by age, race, or Hispanic ethnicity. The researchers also noted that almost 3 of every 100 men who attained SVR became reinfected every year. Again these data underline the urgent need for prevention measures in this particular patient group. The rise of meth use in these patients calls for the implementation of new drug use services which are able to tackle the complex issues coming along with amphetamine abuse. The hope remains, that in analogy to the Dutch data reinfection rate may drop significantly once DAA based treatment for acute hepatitis C becomes available.
CROI: High and Rising HCV Incidence in San Diego Study of 2395 MSM With HIV
Figure 4: Increasing HCV primary incidence among HIV+ MSM in San Diego
Feedback from real-life cohorts
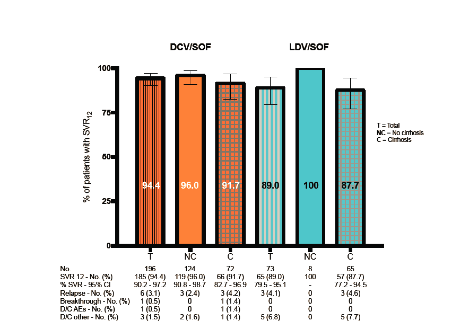
A huge amount of studies looked at efficacy and safety of all oral DAA combinations in various subgroups of coinfected patients including patients with the more difficult-to-treat genotype 3 or patients on opiate substitution therapy or marginally housing (4-7). Spanish real-life cohort data demonstrated that daclatasvir/sofosbuvir +/- ribavirin was highly effective in HIV/HCV-coinfected patients with GT3 with or without cirrhosis, thus confirming the results of clinical trials (4). The main findings from the ITT analysis are summarized in figure 5. Overall, 273 coinfected individuals met the inclusion criteria. The following regimens were analyzed: Daclatasvir + Sofosbuvir (DCV/SOF) 196 patients, 106 without RBV [8 wk, 1; 12 wk, 84; 16 wk, 2; 24 wk, 19] and 90 patients with RBV [12 wk, 43; 16 wk, 1; 24 wk, 46]. The combination of Ledipasvir/Sofosbuvir (LDV/SOF) was given to 73 patients; 62 with RBV [12 wk, 5; 24 wk, 57] and 11 without RBV for 24 wk.
Reassuringly, the real-life cohort from Madrid shows comparatively high HCV cure rates as in clinical trials underlining that already with daclatasvir + sofosbuvir a potent combination exists for GT3 treatment. With more pan-genotypic regimens recently licensed as well as on their way, future treatment options for GT3 are likely to increase and further improve shortly.
CROI: Effectiveness of All-Oral DAAs for HCV Genotype 3 In HIV/HCV-Coinfected Patients
Figure 5: DCV/SOF and LDV/SOF for GT3 - SVR12 by ITT analysis
Feedback at CROI from HCV treatment experience in PWIDS receiving opiate agonist therapy as well as in marginally housing patient groups underline that there are really no reasons to leave these patients behind as overall cure rates are very comparable to other less challenging to treat patient groups (5,7).
CROI: Real-world outcomes of HCV treatment in homeless and marginally housed adults
CROI: High Efficacy of IFN-free Anti-HCV Regimens for Individuals on Opiate Agonist Therapy
Another interesting study comes from the GECCO cohort in Germany (6). The GECCO cohort is a multicenter cohort from 9 sites in Germany. All HCV/HIV coinfected patients (349/1505) with complete follow-up having received one of the following DAA regimen were analysed: Pegylated interferon plus ribavirin (RBV) + sofosbuvir (SOF); SOF + RBV; SOF + simeprevir; SOF + daclatasvir +/- RBV; SOF + ledipasvir; paritaprevir/ritonavir, ombitasvir +/- RBV and +/- dasabuvir. Treatment outcome was measured as sustained virologic response 12 weeks after end of therapy (SVR12). Fisher's exact, chi-square and Mann-Whitney U test were used for statistical analysis. Liver cirrhosis was assessed mainly by transient elastography (FibroScan®) or APRI score. Overall SVR rate was 95% (1425/1505), 95% (1096/1156) in HCV mono- and 94% (329/349) in HCV/HIV coinfected (p=0.684). 10 patients stopped treatment (1 non-response, 2 viral breakthroughs, 7 toxicities). 3 reinfections
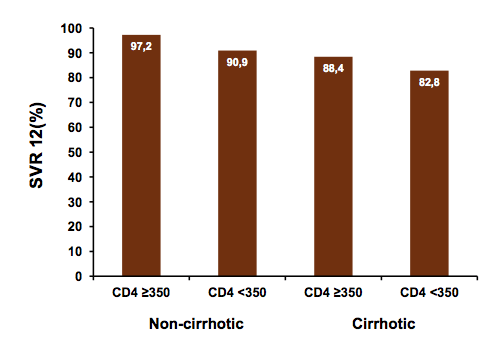
and 67 relapsers were noted. Among the 349 coinfected patients, neither sex (p=0.708), age (p=0.876), GT (p=0.594), high HCV RNA (p=0.873), ALT (p=0.262), TE (p=0.360), CD4 nadir (p=0.473) or OST (p=0.391) were statistically significantly associated with SVR in univariate analysis. However, patients with CD4 <350/ul (p=0.012), CD4 <20% (p=0.005) and liver cirrhosis (p=0.003) were less likely to achieve SVR (see figure 6). In multivariate analysis only liver cirrhosis (p=0.02, OR 3.5 (95%CI 1.2-9.9)) remained statistically significantly associated with Non-SVR. Despite considerably improved safety and efficacy of treatment of chronic hepatitis C with DAA in HCV/HIV-coinfection liver cirrhosis remains as a risk factor for DAA treatment failure in patients with additional impaired immune function. Low CD4 cells were highly correlated with liver cirrhosis probably due to splenomegaly causing lymphopenia but also because advanced immunodeficiency leads to progressive fibrosis formation in HIV/HCV coinfected individuals.
These findings further highlight the need for early initiation of DAA therapy in HCV/HIV coinfected patients before the onset of higher liver fibrosis/cirrhosis to allow for optimal rates of viral eradication and to substantially reduce morbidity and mortality in this patient population.
CROI: Same same but different? Risk of DAA therapy failure in real-life HCV/HIV coinfection: The GECCO Cohort
Figure 6: SVR12 according to CD4 count and cirrhosis status
What to look out for under and after achieving SVR with all oral DAA therapy.
At the last EASL and AASLD conference reports of HBV reactivation after cure of HCV as well as potentially increased rate of HCCs after SVR have been discussed (16, 17). At this year CROI for the first time an analysis was presented which evaluated the risk for HCC (depending on HCV therapy received) in a cohort of HIV/HCV coinfected individuals. The authors determined the proportion of HCC cases in cirrhotic patients after SVR and the evolution of the proportion over time. Overall, 319 HCV/HIV patients with HCC in 32 Spanish centers from 1996-2016 were included. 45% of the patients were pretreated and 295 cases of HCC occurred after a median of 16-24 months after SVR. Four study periods depending on available HCV therapy were defined: Period 1(≤2001): non-pegylated IFN, period 2 (2002-2001): pegylated IFN plus ribavirin, period 3 (2012-October 2014): DAA in combination with pegylated IFN and period 4 (October 2014-2016): DAA IFN-free regimens. The proportion of HCC cases in patients with previous SVR was 16.7% (1 out of 6), 9.9% (16 out of 161) and 9.0% (10 out of 111) in period 1, 2 and 3, respectively (Figure 7). By contrast, this proportion increased to 31.7% (13 out of 41) in the DAA IFN-free period (p<0.01 for the comparison between period 1-3 vs 4) (Figure 7).
Figure 7: Number of HCC after SVR/Total number of HCC cases
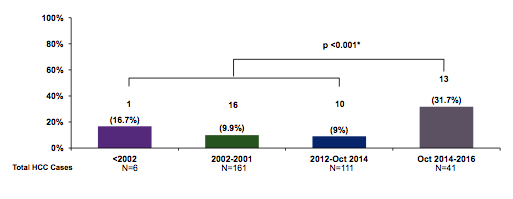
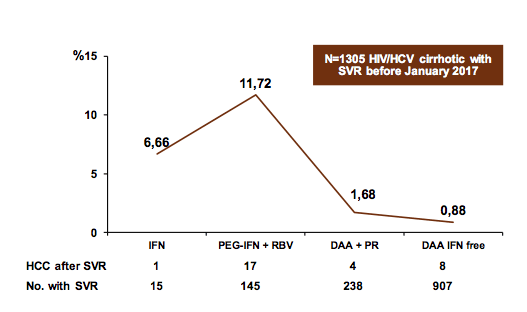
19 centers from the GEHEP-002 cohort reported data of the number of
HIV/HCV-coinfected patients with cirrhosis who achieved SVR in each period. Overall, 1305 HIV/HCV coinfected cirrhotics were included. Of note, the frequency of HCC diagnosis seems to not have increased in the more recent all oral DAA combination treatment era (see figure 8).
Figure 8: Frequency of HCC Diagnosis After SVR in HIV/HCV Coinfected Patients with Cirrhosis
In conclusion, the proportion of HCC cases diagnosed in HIV/HCV-coinfected patients with previous SVR has significantly increased parallel to the arrival of DAA IFN-free strategies. This finding may be, at least partially, explained by the fact that DAA have allowed treating patients at advanced stages of liver disease in which the protective effect of SVR on the risk of HCC could be less marked. This study has not found evidence for an increased incidence of HCC with DAA use so far.
In a further analysis the authors looked at the outcome of HCC patients who were treated for HCV after HCC diagnosis. Overall, 39 patients with HCC had received therapy against HCV after HCC diagnosis. 8 patients had received IFN-based therapy after HCC curative therapy. 31 were treated with IFN-free DAA combination therapy. 19 patients had been treated with previous curative therapies against HCC and ultrasound showed evidence of lack of nodules prior to HCV therapy. Interestingly, HCC recurrence rates after potentially curative treatments among those undergoing HCV therapy were comparable between IFN-based and IFN-free DAA treated patients.
In a smaller second study 1,154 Italian HCV patients, including 34% with HIV/HCV coinfection, were followed-up for an average of 16.7 months in the DAA era. Overall, 27 HCCs were observed, 21 were a first HCC event, 6 were a recurrence. The incidence of new HCC was 1.44/100 patient-years and comparable to a historical control rate of 1-3/100 patient-years. Therefore, this is a second study which also does not seem to suggest an increased HCC prevalence after achieving SVR under DAA therapy.
CROI: Liver Cancer Cases Rise After SVR With All-DAA Therapy in Spanish HCV/HIV Cohort...... "our study has not found evidence for an increased HCC incidence with DAA use"
CROI: HCC DEVELOPMENT IN HCV PATIENTS AFTER DAA: THE EXPERIENCE OF THE SCOLTA PROJECT
CROI: GLECAPREVIR AND PIBRENTASVIR INTERACTIONS WITH COMBINATION ANTIRETROVIRAL REGIMENS - (02/20/17)
Anything new on DAAs in development?
The only study on investigational DAAs was a PK interaction poster on the new Abbvie fix dose combination of glecaprevir (GLE) and pibrentasvir (PIB) together with combination antiretroviral regimens (19). As this new pan-genotypic fix-dose HCV combination contains a HCV protease inhibitor the question in particular is how it may interact with boosted HIV drugs. This study was therefore designed to evaluate the pharmacokinetics, tolerability, and safety of the combination of GLE and PIB co-administered with EVG/COBI/FTC/TAF or ABC/DTG/3TC. Adult male and female subjects in general good health (healthy volunteers) were selected to participate in the DDI study. GLE + PIB increased elvitegravir and cobicistat Cmax by 29-36%, AUC24 by 42-47%, and C24 by 71-72%. Emtricitabine and tenofovir exposures were not affected by GLE + PIB (≤ 25% change). When coadministered with ELV/COBI/FTC/TAF, GLE C max, AUC, and C24 were 2.5-, 3.1- and 4.6-fold, respectively, of GLE + PIB alone; PIB AUC24 and C24 were 57% and 89% higher.
Higher exposures of GLE and PIB are likely due to inhibition of P-gp, BCRP, and/or OATP transporters by elvitegravir and cobicistat. Based on label recommendations for interactions with other drugs, changes in exposures of elvitegravir, cobicistat, emtricitabine, and tenofovir
were not considered clinically significant. Exposure-safety analysis of Phase 3 data indicated that higher glecaprevir exposures when dosed with ELV/COBI/FTC/TAF are not expected to have a clinically significant effect on the safety profile of the GLE/PIB combination.
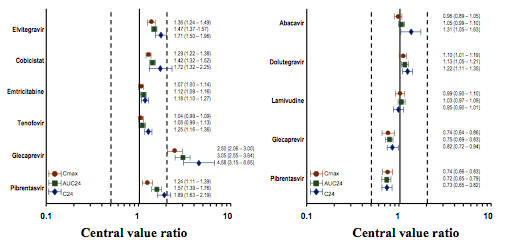
In the ABC/DTG/3TC DDI Sub-Study except for a 31% higher abacavir C24, exposures of abacavir, dolutegravir, and lamivudine were similar with or without GLE + PIB (≤ 22% difference). GLE and PIB Cmax and AUC were slightly lower (25% to 28%) when coadministered with ABC/DTG/3TC. Again, based on exposure-efficacy analysis of Phase 3 data, lower exposure of GLE and PIB are not expected to have a clinically significant effect on the efficacy of the regime. The corresponding findings are shown below in figure 9.
Figure 9a and b: a) Interactions of EVG/COBI/ELV/TAF and GLE + PIB (Central Value Ratios and 90% CIs) and b) Interactions of ABC/DTG/3TC and GLE + PIB (Central Value Ratios and 90% CIs)
CROI: GLECAPREVIR AND PIBRENTASVIR INTERACTIONS WITH COMBINATION ANTIRETROVIRAL REGIMENS - (02/20/17)
Anything else?
As already seen in previous liver meetings a new analysis was presented looking at the efficacy and safety of generics in the treatment of HCV (8). Clearly, high prices for HCV DAAs present a barrier to treatment access. High-income countries such as Russia, China, Southeast Asia and Eastern Europe are not included in voluntary license agreements, and prices of DAAs in these countries remain very high. In most of these countries, individual citizens can legally import non-registered medicines for their personal use. An increasing number of individuals are treating their Hepatitis C infection with generic drugs produced in India, China or Egypt. This analysis assessed the effectiveness of generic DAAs imported into 40 countries. Overall, 1150 patients sourced generic versions of sofosbuvir (SOF), ledipasvir (LDV) and daclatasvir (DCV) from suppliers in India, Bangladesh, China and Egypt via established Buyers Clubs and personal connections. The choice of DAAs and the length of treatment were determined based on baseline RNA levels, HCV Genotype and stage of fibrosis. Figure 12 summarizes the SVR12 findings for the various genotypes.
Figure 12: SVR12 rates
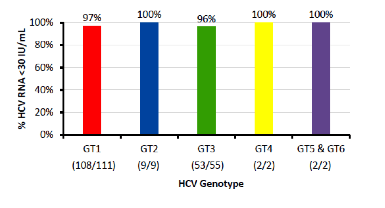
Reassuringly, treatment with legally imported generic DAAs achieved high rates of HCV RNA undetectability at the end of treatment and SVR in the majority of patients. The efficacy observed was similar to Phase 3 trials of the branded medicines. This is very important as it suggests that it is currently safe and efficacious to use generics for HCV therapy although the fear for introduction of fake drugs persists.
New findings in hepatitis B
Patients with HIV have a six times higher rate of developing chronic hepatitis B following acute HBV infection. Immune reconstitution under successful ART however, may increase the likelihood of clearing HBV infection successfully after prolonged dual HIV/HBV active nucleoside therapy. Data on rates of HBsAg loss over time under HBV nucleos(t)ide therapy are sparse. Therefore this German study evaluated the rates of HBV seroconversion under HBV active ART with a median follow-up of at least 8 years (10). Overall, 95 subjects were identified with chronic HBV and included into this observational cohort. The baseline demographics of the cohort are depicted below in Table 1. Of note all patients were eventually receiving a tenofovir containing ART, which is reassuring as a quality control as this is recommended by guidelines accordingly for treatment of chronic HBV infection in HIV coinfection. 84% received TDF, 16% TDF and 3TC. 55% received a boosted protease inhibitor, 40% NNRTI and 5% an integrase inhibitor.
Table 1: Baseline patient characteristics of the chronic hepatitis B cohort
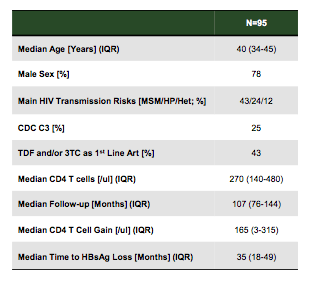
Most interestingly, HBV seroconversion (HBsAg loss) occurred in 16% (15/95) of patients which is much higher than what has been reported from long-term follow up of patients receiving tenofovir from the original registrational phase III trials in HBV monoinfected subjects. Figure 10 shows the loss in HBs-Ag over time.
Figure 10: HBs-AG loss over time
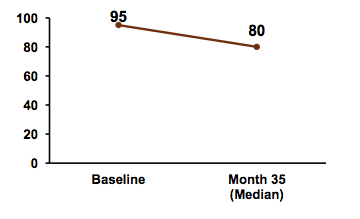
There was no significant correlation between HBsAg loss and gender (p=0.562), age (p=0.677), country of origin (p=0.274), CDC stage (p=0.585), CD4 cell count (p=0.249), CD4 gain (p=0.7), HBeAg (p=0.712), receiving TDF or TDF/3TC (p=0.576) or ART class (p=0.582). In summary, HBV seroconversion defined as HBsAg loss is occurring at a much higher rate in HBV HIV coinfected patients even after years on HBV active ART when compared to published seroconversion rates of 4.5% over 96 weeks from the extension phase III tenofovir trials in HBV monoinfected subjects. Positive predictors remain unclear to date but immune reconstitution under ART appears to allow better control of HBV infection. As a consequence, regular controls of HBV serology to document HBV seroconversion are required in HIV/HBV coinfected patients on long-term HBV active HIV therapy with tenofovir.
Another interesting HBV trial presented at CROI evaluated how to best prevent perinatal HCV transmission (11). Of note, pregnant women with high hepatitis B virus (HBV) DNA load still transmit to their infants despite infant HB immunoglobulin (HBIg) and HB vaccine.
This phase III, double-blind, clinical trial randomized pregnant women with HBV infection (HBsAg and HBeAg positive) to tenofovir DF (TDF) 300 mg once daily or matching placebo (1:1) from 28 weeks gestation through 2 months postpartum in 17 sites in Thailand. The study design is depicted below in figure 11. All infants received HBIg at birth, and vaccine at birth, 1, 2, 4 and 6 months of age. Main inclusion criteria were: age ≥18 years, confirmed ALT ≤60 IU/L, negative HIV and hepatitis C serology, creatinine clearance >50 mL/min, and no history of TDF treatment. Mothers and infants were followed until 12 months postpartum. The primary efficacy endpoint was detection of HBsAg confirmed by HBV DNA at 6 months of age. The target sample size was 156 evaluable mother/infant pairs per arm to detect a difference in HBV infected infants of 3% (TDF) vs. 12% (placebo) with 90% power accounting for one interim efficacy analysis, using a one-sided Fisher's exact test. Analyses are based on data through 6 months postpartum.
Figure 11: Study design
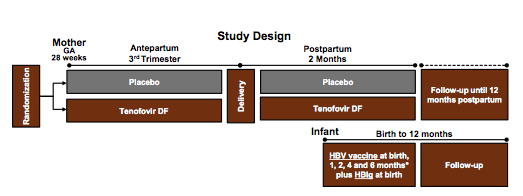
Overall, 331 women (168 TDF, 163 placebo) were enrolled into the trial from January 2013 to August 2015. The median age was 26.1 years (22.9, 30.0), the gestational age at baseline was 28.3 weeks (range: 26.6 to 29.6) and the median weight at entry was 61.2 kg (55.5, 69.7). HBV DNA viral load at enrollment was 8.0 log10IU/mL (7.1, 8.5). HBV DNA load at delivery declined significantly in the TDF group and was on median 3.9 log10 IU/mL (3.0, 4.8) on TDF, versus 7.8 log10 IU/mL (6.8, 8.5) on placebo. Within the trial 322 (97%) on-study deliveries were documented (85 Cesarean, 26%). 323 were live births (including 2 twin pairs) and 1 stillbirth (TDF arm). The gestational age at delivery was 38.9 weeks (38.1, 39.9). Overall, 21 (7%) (8 TDF, 13 placebo) preterm newborns were documented. Median birth weight was 3050 g (2796, 3352): 3028 g (TDF) and 3061 g (placebo). 320 (99%) infants received HBIg a median of 1.3 hours after birth and 322 (>99%) received HB vaccine a median of 1.2 hours after birth. In the primary complete case analysis at 6 months, 0/147 infants had HBV infection in the TDF arm versus 3/147 (2.0%) in the placebo arm (p=0.12). All 3 infected infants' mothers had HBV DNA >7.8 log10 IU/mL at delivery. The efficacy endpoints of the trial are summarized in Table 2 below.
Table 2: Efficacy endpoints at 6 months
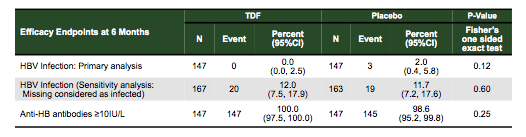
With regard to safety endpoints following study treatment discontinuation, 9 (6%) women experienced an ALT >300 IU/mL in the TDF arm vs. 5 (3%) in the placebo arm (two-sided p=0.29). Nine women ever had ALT >300 IU/mL during the trial in the TDF arm, and 8 in the placebo arm. The proportions of maternal and infant adverse events, and infant growth were similar between arms.
In summary, this trial shows that in mothers who were HBsAg and HBeAg positive, HBV mother-to-child transmission was only 2% in infants who received HBIg and HBV vaccine. TDF resulted in a small non-significant reduction in perinatal HBV transmission beyond the low risk achieved with HBIg and HBV vaccine. Of note, to date, no study has reported a transmission rate as low as 2% among untreated women with HBeAg whose infants received only hepatitis B vaccine and HBIg. The early timing of these interventions as well as the five vaccine applications may have had an impact here. Overall, TDF appeared safe for pregnant women and infants and there was no evidence of impaired infant growth. The additional administration of TDF in chronic HBV infected pregnant women with high viral load therefore appears advisable and is currently recommended by international guidelines.
CROI: TDF TO PREVENT PERINATAL HEPATITIS B VIRUS TRANSMISSION: A RANDOMIZED TRIAL (ITAP)
CROI: INCREASED RATES OF HBV SEROCONVERSION UNDER LONG-TERM HBV ACTIVE THERAPY IN HBV/HIV - [16%]
Summary
⋅For the first time in >10 years the incidence of acute HCV in HIV+MSM in the Netherlands dropped substantially. Unrestricted access and use of DAA for the treatment of chronic and acute HCV is the most likely explanation.
⋅Consider HCV-PCR for acute HCV diagnosis as HCV-Ab may still be negative. An intensified HCV-RNA based screening strategy among sexually active HIV-coinfected MSM is worth to detect potentially transmitters, and to offer universal treatment with DAAs in order to end the epidemic and to achieve a reduction of disease burden on a population level.
⋅HCV-infected PWID on opiate agonist therapy (OAT) achieve high SVR4 rates with IFN-free DAA. Because of this real life efficacy, HCV infection treatment should not be deferred among PWID due to ongoing OAT.
⋅Real-life cohorts demonstrated that daclatasvir/sofosbuvir was highly effective in HIV/HCV-coinfected patients with GT3 with or without cirrhosis, thus confirming the results of clinical trials.
⋅Patients with HIV/HCV coinfection and lower CD4-counts and cirrhosis show overall less favorable SVR rates.
⋅The proportion of HCC cases diagnosed in HIV/HCV-coinfected patients with previous SVR has significantly increased parallel to the arrival of DAA IFN-free strategies. This finding may be, at least partially, explained by the fact that DAA have allowed treating patients at advanced stages of liver disease in which the protective effect of SVR on the risk of HCC could be less marked.
⋅No dose-adjustment is required when GLE/PIB is co-administered with ELV, FTC, TAF, ABC, DTG, or 3TC.
⋅HBV seroconversion defined as HBsAg loss is occurring at a much higher rate (16%) in HBV HIV coinfected patients even after years on HBV active ART when compared to published seroconversion rates of 4.5% over 96 weeks from the extension phase III tenofovir trials in HBV monoinfected subjects. Positive predictors remain unclear to date but immune reconstitution under ART appears to allow better control of HBV infection.
⋅In mothers who are HBsAg and HBeAg positive, HBV mother-to-child transmission can be reduced to 2% in infants by administring HBIg and HBV vaccine. Additional TDF therapy results in a small non-significant reduction in perinatal HBV transmission beyond the low risk achieved with HBIg and HBV vaccine.
References
1. Boerekamp A et al. Unrestricted DAA access in the Netherlands: Rapid therapy uptake in HIV+HCV+ patients. 24th Conference on Retroviruses and Opportunistic Infections, February 13-16, 2017, Seattle; abstract 136
2. Boerekamp A et al.: Substantial decline in acute HCV infections among Dutch HIV+MSM after DAA roll out. 24th Conference on Retroviruses and Opportunistic Infections, February 13-16, 2017, Seattle; abstract 137LB
3. Ingiliz P, et al. NEAT study group. HCV reinfection incidence and spontaneous clearance rates in HIV-positive men who have sex with men in Western Europe. J Hepatol. 2017 Feb;66(2):282-287.
4. Gonzalez-Garcia J et al. Effectiveness of all-oral DAAs for HCV genotype 3 in HIV/HCV-coinfected patients. 24th Conference on Retroviruses and Opportunistic Infections, February 13-16, 2017, Seattle; abstract 572
5. Macias J et al. High efficacy of IFN-freee anti-HCV regimens for individuals on opiate agonist therapy. 24th Conference on Retroviruses and Opportunistic Infections, February 13-16, 2017, Seattle; abstract 555
6. Boesecke C et al. Same same but differenet? Risk of DAA therapy failure in real-life HCV/HIV coinfection. 24th Conference on Retroviruses and Opportunistic Infections, February 13-16, 2017, Seattle; abstract 551
7. Barocas JA et al. Real-world outcomes of HCV treatment in homeless and marginally housed adults. 24th Conference on Retroviruses and Opportunistic Infections, February 13-16, 2017, Seattle; abstract 557
8. Hill A et al. Ninety-six % SVR rates using imported generic DAAs for patients with hepatitis C. 24th Conference on Retroviruses and Opportunistic Infections, February 13-16, 2017, Seattle; abstract 569
9. Merchante N et al. Hepatocellular carcinoma after SVR with IFN-free regimens in HIV/HCV Coinfection. 24th Conference on Retroviruses and Opportunistic Infections, February 13-16, 2017, Seattle; abstract 139
10. Boesecke C et al. Increased rates of HBV seroconversion under long-term HBV active therapy in HBV/HIV. 24th Conference on Retroviruses and Opportunistic Infections, February 13-16, 2017, Seattle; abstract 580
11. Jourdain G et al. TDF to prevent perinatal hepatitis B virus transmission: A randomized trial (ITAP). 24th Conference on Retroviruses and Opportunistic Infections, February 13-16, 2017, Seattle; abstract 584LB
12. Hullegie SJ et al. Boceprevir, peginterferon and ribavirin for acute hepatitis C in HIV infected patients. J Hepatol. 2016 Apr;64(4):807-12. J Hepatology 2016
13. Ingiliz P et al. HCV reinfection after successful DAA treatment: A GECCO analysis. 24th Conference on Retroviruses and Opportunistic Infections, February 13-16, 2017, Seattle; abstract 567
14. Braun DL et al.: Systematic HCV-RNA screen in HIV+ MSM reveals high numbers of potential transmitters. 24th Conference on Retroviruses and Opportunistic Infections, February 13-16, 2017, Seattle; abstract 521
15. Chaillon A, et al. Incidence of hepatitis C among HIV-infected men who have sex with men, 2000-2015. 24th Conference on Retroviruses and Opportunistic Infections, February 13-16, 2017, Seattle; abstract 134
16. Bersoff-Matcha S, et al.: Hepatitis B Reactivation Associated with Direct Acting Antiviral Therapy for Hepatitis C: A Review of Spontaneous Post-Marketing Cases. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract LB-17
17. Romano A et al.: Incidence and pattern of "de novo" hepatocellular carcinoma in HCV patients treated with oral DAAs. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 19
18. Menzaghi B et al.: HCC development in HCV patients after DAA: The experience of the SCOLTA project. 24th Conference on Retroviruses and Opportunistic Infections, February 13-16, 2017, Seattle; abstract 542LB
19. Kosloski MP et al.: Glecaprevir and pibrentasvir interactions with combination antiretroviral regimens. 24th Conference on Retroviruses and Opportunistic Infections, February 13-16, 2017, Seattle; abstract 413
|
| |
|
 |
 |
|
|