 |
 |
 |
| |
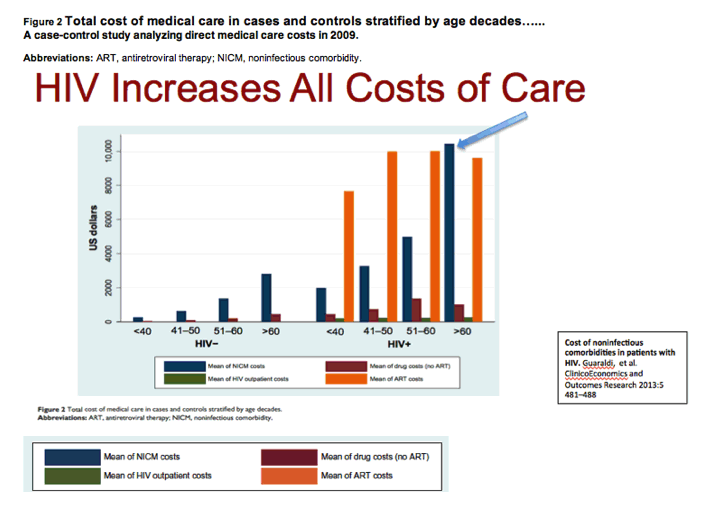
Cost of noninfectious comorbidities in patients with HIV
- Cost of HIV CARE Increases 5 fold Due to Cost for Comorbidities from <40 to >60
|
| |
| |
Download the PDF here
from Jules - see slide below on Comorbidities care Costs & ART costs: patient ages 40-60 the comorbidities care costs are about 20-35% of the ART costs - by the age of 60 these costs go up 5 fold they are $10,000 a year & greater than ART costs
75% Predicted will be frail in 14 years, 60% frail now among older aging HIV+ and predicted 40% will have to be confined to old age homes as they will be disabledIWCADRH: Future challenges for clinical care of an ageing population infected with HIV: a "geriatric-HIV" modelling study - [Healthcare Costs].... Very Sobering Analysis go Aging in HIV+....60% frail- (09/15/16)
"In 15 years time the HIV geriatric population [65-67 yo] will increase from 4% to 37%" http://www.natap.org/2016/AGE/AGE_18.htm
"In 15 years time the most frail HIV population will increase from 24% [now, 2016] to 48%"
"In 15 years time 34% of PLWH will be disabled" [burden of IADLs - independent activities of daily living]
HIV+ >65 on Medicare Have 2 Times More Comorbidities vs HIV-neg AND Blacks & Latinos Have 4-Fold Increased Risk for the 5 Comorbidities Examined vs Whites - CDC Report Chronic health conditions in medicare beneficiaries 65 years and older with HIV infection. - (10/08/16)
Older adults with HIV have higher burdens of cardiovascular, metabolic, pulmonary, renal, bone, and malignant diseases http://www.natap.org/2016/AGE/AGE_25.htm
"advance care planning is essential in older adults with HIV"
"With increasing disease burden, individuals with HIV with multimorbidity are also at risk of fragmentation of or contradictions in care plans because of involvement of multiple clinicians in multiple settings"
AGE: Non-HIV care provider....Aging, Worse Still to Come?....Aging Clinic at Weill-Cornell, NYC; aging $costs in HIV skyrocket -
--------------------------
Cost of noninfectious comorbidities in patients with HIV
Giovanni Guaraldi,Stefano Zona1,Marianna Menozzi1,Federica Carli1,Pietro Bagni1,Alessandra Berti2,Elisa Rossi2,Gabriella Orlando1,Giuliana Zoboli3,Frank Palella4
"With regards to estimates, we were able to demonstrate that the total direct cost increases two-fold moving from the <40 years age strata of HIV-infected patients (US$10,588.45) to those older than 60 years (US$21,280.72)."
The clinical picture of HIV disease has changed rapidly in the last 10 years. Noninfectious comorbidities (NICMs) including cardiovascular disease (CVD), hypertension (Htn), bone fractures, renal failure, and diabetes mellitus (DM), became the most frequently observed causes of morbidity and mortality in HIV-infected patients.11–17 NICMs aggregate to give rise to complex polypathology pictures that typically occur in advanced age and describe geriatric syndromes.18–20.21,22 It is necessary to update total cost of medical care in HIV in order to better predict resource and allocation needs for the care of people living with HIV (PLWHA).
Our objective was to provide estimates and determinants of direct cost of medical care for HIV-infected patients, including direct cost of NICMs.
Abstract
Objectives:
We hypothesized that the increased prevalence of noninfectious comorbidities (NICMs) observed among HIV-infected patients may result in increased direct costs of medical care compared to the general population. Our objective was to provide estimates of and describe factors contributing to direct costs for medical care among HIV-infected patients, focusing on NICM care expenditure.
Methods:A case-control study analyzing direct medical care costs in 2009.
Antiretroviral therapy (ART)-experienced HIV-infected patients (cases) were compared to age, sex, and race-matched adults from the general population, included in the CINECA ARNO database (controls). NICMs evaluated included cardiovascular disease, hypertension, diabetes mellitus, bone fractures, and renal failure. Medical care cost information evaluated included pharmacy, outpatient, and inpatient hospital expenditures. Linear regression models were constructed to evaluate predictors of total care cost for the controls and cases.
Results:There were 2854 cases and 8562 controls. Mean age was 46 years and 37% were women. We analyzed data from 29,275 drug prescription records. Positive predictors of health care cost in the overall population: HIV infection (β = 2878; confidence interval (CI) = 2001-3755); polypathology (β = 8911; CI = 8356-9466); age (β = 62; CI = 45-79); and ART exposure (β = 18,773; CI = 17,873-19,672). Predictors of health care cost among cases: Center for Disease Control group C (β = 1548; CI = 330-2766); polypathology (β = 11,081; CI = 9447-12,716); age < 50 years (β = 1903; CI = 542-3264); protease inhibitor exposure (per month of use; β = 69; CI = 53-85); CD4 count < 200 cells/mm3(β = 5438; CI = 3082-7795); and ART drug change (per change; β = 911; CI = 716-1106).
Conclusion:Total cost of medical care is higher in cases than controls. Lower medical costs associated with higher CD4 strata are offset by increases in the care costs needed for advancing age, particularly for NICMs.
Figure 1 Comparative risk of hypertension, diabetes, cardiovascular disease (CVD), fracture, and renal failure, by age strata, among cases and controls.
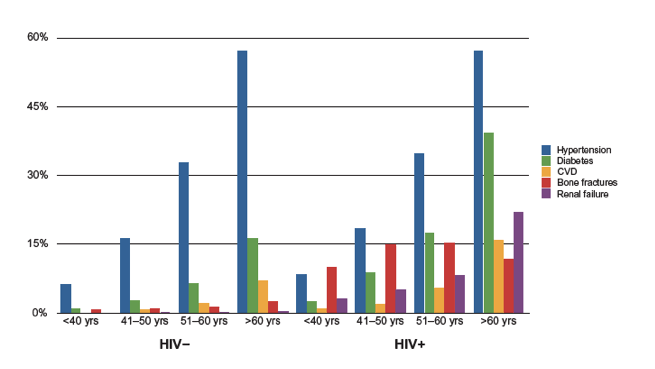
Figure 2 Total cost of medical care in cases and controls stratified by age decades.
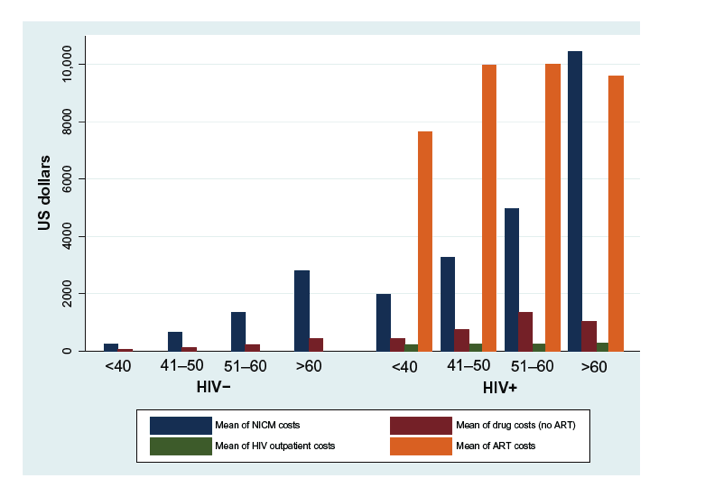
Methods
This is a case-control study analyzing all direct medical costs in the 2009 calendar year.
Cases were ART-experienced HIV-infected patients > 18 years of age who had access to the metabolic clinic of the University of Modena and Reggio Emilia, Modena, Italy.
This outpatient clinic is a multidisciplinary center for the management of NICMs in ART-experienced patients, as previously described.23 Patients attending this referral service are the patients attending the Modena HIV clinic as well as individuals referred from neighboring HIV centers.
Controls were matched according to age, sex, race, and geographical area and were selected from the CINECA ARNO observational database.24 The ARNO Observatory is an online, multicenter, observational database in which population-based data is collected and epidemiological methods are used to combine and aggregate huge volumes of health and health care-related data for each individual patient. These data include primary care provider-generated medication prescriptions, records from hospital admissions and discharges, diagnostic laboratory tests, and radiographic examinations. This information is linked to other sources of patient data (including vital statistics and patient demographics) in order to construct a tool that is used to provide comprehensive tracking of clinical diagnoses and health care use trends throughout Italy. The ARNO observatory has been active since 1986 and includes health care prescription data generated by 8300 general practitioners for a population of 11 million persons cared for at 32 health units in Italy. The database is updated monthly.
Direct health care cost analysis
Direct health care cost was retrospectively analyzed in the 2009 calendar year using the following indicators:
1. Hospitalization cost: calculated by collecting International Classification of Diseases (ICD)-9 codes in cases and controls. All hospitalization with a primary or secondary ICD-9 comorbidity diagnosis code, including CVD, Htn, DM, bone fractures, and renal failure diagnosis, were selected.25
2. Outpatient HIV medical care cost. With the movement of HIV care into the outpatient setting, it was no longer possible to evaluate the cost of medical care using ICD-9 codes, therefore we decided to attribute a mean patient care cost obtained by the most recent reference value able to better define HIV-related care cost in patients with ART. This estimate is adjusted for current CD4 count strata and in particular, it accounts for US$1,381/year for patients with CD4 < 75 cells/mm3, US$1,241/year for 76 < CD4 < 200 cells/mm3 and US$190/year for CD4 > 201 cells/mm3.26
3. NICM medication cost: calculated using pharmaceutical tracing by average wholesale prices obtained by the Agenzia Italiana del Farmaco (AIFA) national pharmaceutical handbook.27
4. ART medication cost: calculated using pharmaceutical tracing, by average hospital sale price.
Total cost is defined as the sum of mean of NICM costs plus mean of HIV hospitalization costs plus mean of drug costs.
For the purpose of this study, the following NICM conditions were eligible for the assessment of direct cost: CVD, Htn, DM, bone fractures, and renal failure. ICD-9 hospital codes and drug tracing criteria were used to identify NICM diagnoses and direct medical cost in the study population. Polypathology (Pp) was defined as the simultaneous presence of two or more NICMs.28
The category of CVD included the following diagnoses: myocardial infarction, coronary artery disease, peripheral vascular disease, stroke, angina pectoris, coronary artery bypass grafting, and angioplasty.
In cases, the following HIV-specific variables were collected from patient charts:
⋅Cumulative exposure to nonnucleoside reverse transcriptase inhibitors (NNRTIs), nucleoside RTIs (NRTIs), and protease inhibitors (PIs)
⋅Number of previous ART drug switch before the current regimen
⋅Current CD4 < 200/mm3
⋅Age categories "young" and "old," using 50 years as the cutoff age
⋅HIV viral load was categorized as undetectable if <40 copies/mL
⋅Previous AIDS diagnosis was defined according to the Centers for Disease Control and Prevention (CDC) group "C" category29
Statistical analysis
Comparisons of variables considered in our study performed between groups and among age strata, were analyzed using χ2-test for categorical variables and t-test or analysis of variance (ANOVA) for continuous variables. P-value < 0.05 was considered significant. Post hoc analyses were performed using Bonferroni's adjustment and significance level was considered for P < 0.008.
Considering the non-normal distribution of total costs, generalized linear models (GLMs) were constructed to evaluate independent factors associated with total cost in the whole population and in the subgroup of HIV-infected patients, using inverse Gaussian family distribution.
In the regression analysis in the HIV-positive cohort, age was stratified using the threshold of 50 years to evaluate the effect of aging on total cost.
The variables for regression analyses were chosen on the basis of their clinical relevance.
Statistical analyses were conducted using the Intercooled STATA software package, version 12.1 for Mac (StataCorp LP, College Station, TX, USA).
|
| |
|
 |
 |
|
|