 |
 |
 |
| |
Summary from EASL 2017 for Hepatitis C - Global implementation of Hepatitis C (HCV) treatment: What are the successes, what are the remaining challenges?
|
| |
| |
Jurgen K. Rockstroh M.D., Professor of Medicine
University of Bonn, Germany
Correspondence:
Prof. Dr. J.K. Rockstroh
Department of Medicine I
University of Bonn
Sigmund-Freud-Str. 25
53105 Bonn
Germany
Introduction
The International Liver Congress™ (ILC) (the annual meeting of the European Association for the Study of the Liver (EASL)) was held in April from 19-23rd, 2017 in Amsterdam, Netherlands. Once again, issues around HCV screening, treatment and post HCV cure monitoring represented a main focus of the conference. However, in contrast to previous EASL conferences there was no longer a dominance of HCV phase II and II treatment trials in the late-breaker session but rather within the general program multiple reports back from real-life implementation of HCV all oral direct acting antiviral (DAA) therapy and first insights from national elimination programs. This coincided nicely with the release of the new WHO global hepatitis report from 2017 which included new numbers on incidence and prevalence of HCV infections worldwide and outlined the ambitious 2030 HCV global elimination strategy. Indeed, the number of HCV infections was reported considerably less than before with a prevalence of 71 Million worldwide (1). A breakdown of HCV prevalence by region from the WHO report is shown in figure 1. The incidence was estimated as 1.75 million new HCV infections per year (mostly due to unsafe health care and injection drug use).
Figure 1: Status of Hepatitis C by region: Results from the WHO report 2017
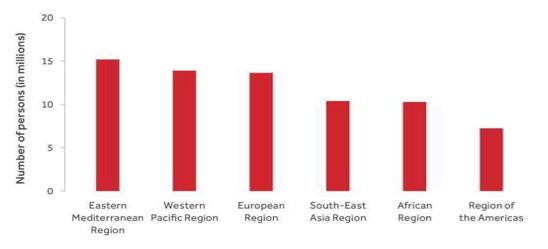
Of note 20% of all HCV infections globally are estimated to be diagnosed in 2017. Under consideration of the 2030 goal of 90% HCV infections diagnosed globally there still is a long way to go. Also HCV treatment coverage worldwide is still below 10% emphasizing the need of considerable HCV treatment scale-up to reach the WHO 80% HCV treatment target in 2030.
Reassuringly, the high success rates of all oral DAA therapy was further confirmed from a wealth of data particularly from somewhat more challenging patient populations including PWIDs, homeless, elderly patients >65years of age, and patients with unfavorable HCV disease characteristics including decompensated cirrhosis but also from the use of newer DAA combinations (2-8). Most importantly, for the first time larger data sets were presented for DAA therapy in children above the age of 6 finally making DAA therapy also possible in this so far understudied patient group (9,10). Previously, reported issues on HBV reactivation following sustained virological response (SVR) under DAA therapy as well as the question of increased hepatocellular carcinoma (HCC) incidence after DAA therapy were readdressed (11-15). Overall, HBV serology needs to be performed prior to commencing HCV therapy. Risk of reactivation remains very low and predominantly only concerns patients with chronic hepatitis B and persistent HBs-AG positivity (12). Prophylactic HBV active nucleos(t)ide therapy is one option; in any case increased monitoring for hepatic flares in HBs-Ag positive patients is recommended. HCC occurrence remains a risk in cirrhotic patients having been successfully treated with DAAs but reports on increased rates of HCC in DAA treated cirrhotic patients more likely just reflects a change in age and cirrhosis stages in HCV patients treated today (13-15). Obviously, increased age and inclusion of more liver disease advanced patients which were not treated previously increases overall likelihood of observing HCC development. Finally, new drugs, particularly a rich set of studies around the new Abbvie pangenotypic Glecaprevir (formerly ABT-493) NS3/4A protease inhibitor and Pibrentasvir (formerly ABT-530) NS5A inhibitor (G/P) fix-dose combination were presented (16-18) as well as data from upcoming triplet combinations including Gilead`s fix-dose combination Sofosbuvir (SOF)/Velpatasvir (VEL)/Voxilaprevir(VOX) (19) and Merck`s fix-dose Grazoprevir (GZR)/Ruzasvir (RZR)/Uprifosbuvir (UPR) (20) which are particularly interesting in the context of retreatment of prior DAA failures promising further additions to the HCV drug armentarium in 2017. The following EASL summary report tries to capture the major new findings and results presented around the topics raised above as well as to outline some of the status reports of the ongoing ambitious HCV elimination programs throughout the world.
Feedback from the real world
Among the many reports back from use of DAAs in real-world populations one particularly interesting one was on the first feedback from using the newly available Elbasvir/Grazoprevir (EBR/GZR) fix-dose combination in the U.S. Veterans Health Administration (7). All patients who initiated treatment from February 1, 2016 to August 1, 2016 with this DAA combination were included. Patients who were treated >17 weeks, or had RBV added >1 month after treatment initiation were excluded from the analysis. Overall, 2436 subjects were included into the evaluable population analysis (Evaluable population (EP) denominator - all patients with SVR outcomes available) and 2257 subjects into the per protocol analysis (Per Protocol (PP) denominator limited to patients who completed treatment course). The study population investigated is shown below in figure 2.
Figure 2: Study population
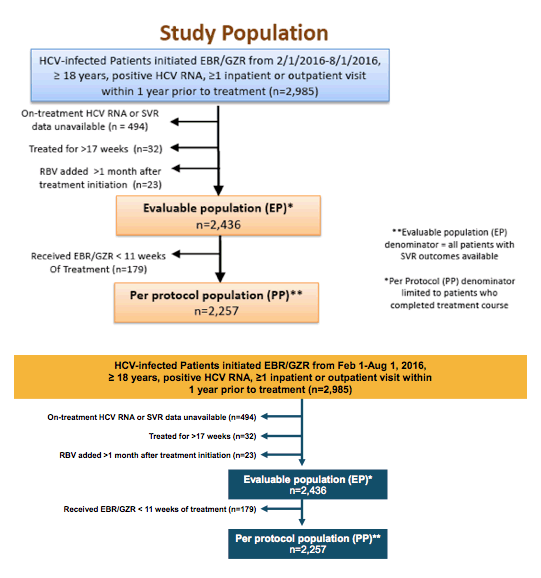
The HCV related patient characteristics are summarized in table 1 and highlight that the majority of treated patients had either GT1a or 1b and indeed a considerable number (33%) already had liver cirrhosis at baseline as well as a considerable amount of comorbidities representing a somewhat more challenging patient group to treat. Of note also more than 50% of study participants were African Americans.
Table 1: Patient characteristics at baseline
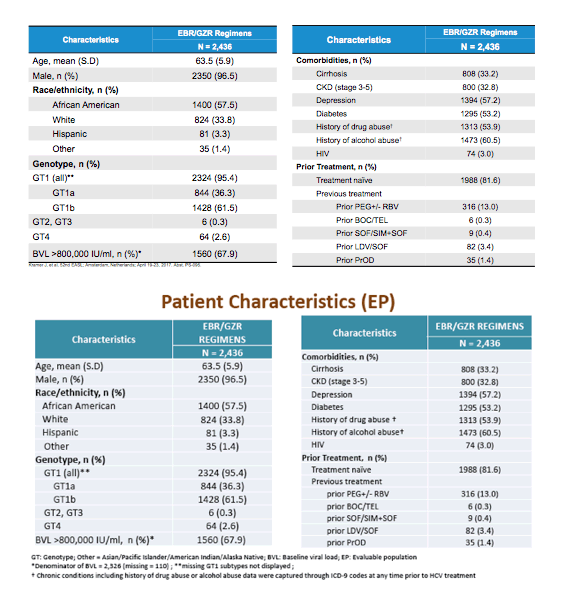
The SVR rates observed were overall excellent, with 2328/2436 (95,6%) patients achieving SVR in the EP population and 2190/2257 (97%) in the PP population. These HCV cure rates are clearly impressive and superimposable to what has been observed as outcome in clinical trials. What however, cannot be answered at this early analysis time point is which GT1a patients were selected. Did they receive genotypic resistance testing prior to EBR/GZR therapy? Was ribavirin added or did they have low viral loads and no cirrhosis? Indeed, resistance testing prior to the use of EBR/GZR is recommended by the label of this fix-dose combination and in the presence of NS5A mutations which may impact EBR susceptibility, extension of therapy to 16 weeks and addition of RBV is recommended. Of note much more GT1b patients were included which are on average easier to treat with this combination which may also present a selection bias in who was treated with this DAA combination. Figure 3a summarizes the SVR rates by genotype and figure 3b by cirrhosis status, presence of chronic kidney disease (CKD) and HIV-coinfection.
Figure 3a: SVR rate by baseline HCV genotype
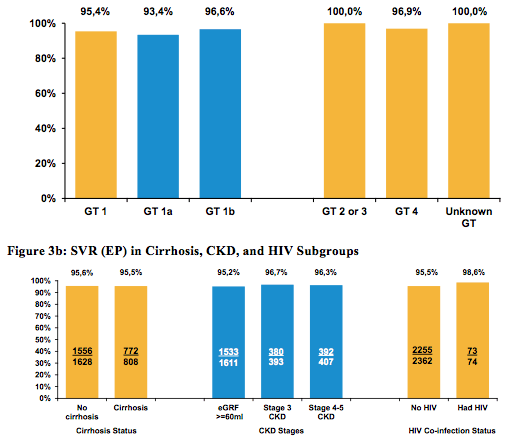
Similar high SVR rates were obtained with EBR/GZR in patients with history of alcohol abuse, patients with history of drug abuse, cirrhosis (n=808), CKD stage 4-5 (n=407), HIV infection (n=74), GT4 (n=64), African Americans (n=1400) and Hispanics (n=81). In conclusion, EBR/GZR was well tolerated and led to impressive SVR rates in this more tough to treat patient population. More data is however needed to understand how well the combination performed in the most challenging patient groups (especially in treatment naïve and experienced GT1a patients with cirrhosis).
Real-World Experience of Elbasvir/Grazoprevir in the Veterans Affairs Healthcare System at DDW 2017 - (05/15/17)
Further interesting data came from first real-world cohorts which received HCV treatment with the newly available Sofosbuvir/Velpatasvir fix-dose combination (8). Utilization of SOF/VEL in G2-6 HCV infected patients was reported from the TRIO Network and compared to the outcome of previously used DAAs for treatment of GT2 (SOF/VEL versus SOF + RBV) and GT3 (Daclatasvir + SOF ± RBV versus SOF/VEL ± RBV and 4-6 (Ledipasvir/SOF versus SOF/VEL). The study disposition for GT 2 and 3 patients for the various study groups studied are shown below in figure 4.
Figure 4a + b: Study disposition from the TRIO network
a) Genotype 2 b) Genotype 3
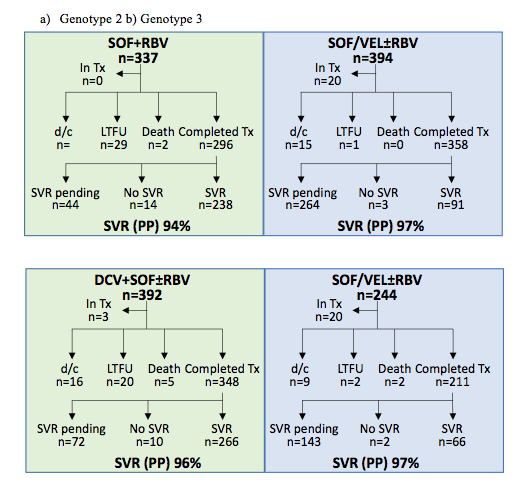
Of note, many study subjects have not yet finished their full 12 weeks of SOF/VEL treatment. Clearly, for GT 2 and 3 impressively high SVR rates have been obtained which are numerically even slightly higher than the comparator DAA treatments. A more detailed comparison for different patient groups including different fibrosis stages and treatment naïve versus treatment experienced patients for GT 2 and 3 respectively, is shown below in figure 5.
Figure 5: SVR rates by fibrosis stage and treatment history from the TRIO network
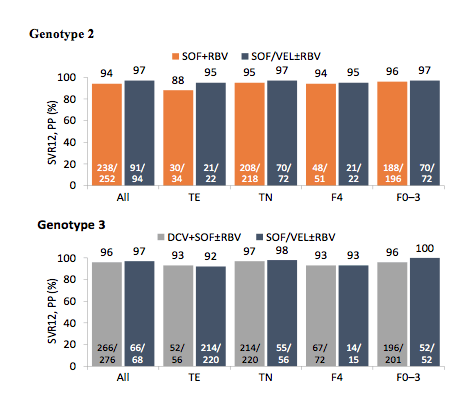
Of note, the biggest difference in SVR rates was observed in the treatment experienced GT 2 patients where 95% were cured with SOF/VEL ± RBV versus only 88% in the SOF + RBV group. For GT 3 overall for all subpopulation studied SVR rates were high and comparable between SOF/VEL ± RBV or DCV + SOF ± RBV. The study disposition for the HCV genotypes 4-6 is shown below in figure 6.
Figure 6: Study disposition TRIO network for HCV GT4-6
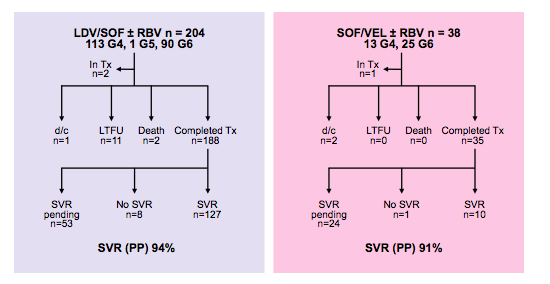
EASL: Sofosbuvir/velpatasvir compared to existing Standards of Care in GT2-6 HCV Real-world experience from the TRIO Network - (04/24/17)
Various studies reported back from DAA-based HCV treatment studies in patients with recent or ongoing active drug use or being on opioid agonist therapy (OAT) (2-4). The PREVAIL study was a randomized controlled clinical trial of HCV treatment for PWIDs with genotype 1 on OAT, including those actively using drugs (4). 158 Participants were randomized from October 2013 to May 2016 to one of three models of HCV care delivered on-site in an OAT program and 150 started DAAs. Directly observed treatment was given to 51 subjects, 48 received therapies during group medical visit and 51 received individual treatment as usual. All HCV regimens were administered as per AASLD/IDSA guidelines. The baseline characteristics for the three groups with different models of HCV care delivery are summarized in table 2.
Table 2: Baseline characteristics by HCV care delivery model
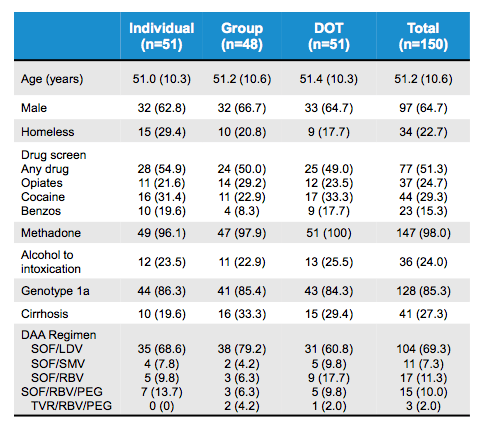
Overall, drug screen at baseline revealed a very high rate of ongoing active drug use despite almost all patients being on methadone substitution therapy. Increased alcohol intake was noted in almost a quarter of all patients. The results from all drug screens during the study is shown below in figure 7 which shows that drug use continued unchanged throughout the study clearly emphasizing the real-world character of this cohort. Most patients had GT1a infection and more than a quarter already had cirrhosis.
Figure 7: Urine drug screen findings during HCV treatment
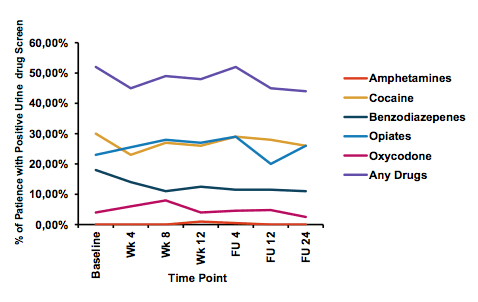
Overall, an impressive high SVR rate of 94.0% (141/150) was noted for the total study population, clearly underlining that high SVR rates can be achieved in persons receiving opiate agonist therapy including those actively using drugs. Directly observed and group therapy had higher rates of adherence compared to individual care and may encourage the use of these HCV care delivery models where possible in similar patient populations. Table 3 summarizes the corresponding SVR and adherence outcomes.
Table 3: SVR rates and adherence outcomes
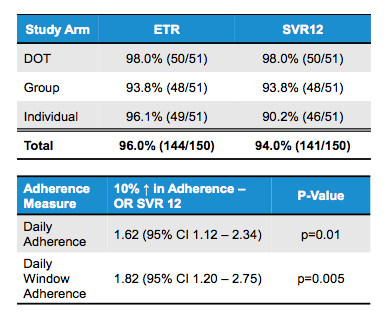
EASL: The PREVAIL Study: Intensive Models of HCV Care for People Who Inject Drugs - (04/26/17)
Similarly good SVR rates were reported back from an international study of SOF/VEL for 12 weeks in persons with recent IDU (< 6 months) from Australia/New Zealand, North America and Europe (2). Overall, 103 subjects were included of which 96% achieved an end-of-treatment response and 91% an SVR12. Modified ITT increased SVR rates to 94%. Therefore, people with HCV and recent or ongoing active drug use should also be considered as candidates for DAA combination therapy.
EASL: Efficacy and safety of sofosbuvir/velpatasvir in people with chronic hepatitis C virus infection and recent injecting drug use: The SIMPLIFY study - (04/24/17)
Another gap closed: finally more treatment data in HCV infected children
Another important patient population which so far has only limited data available is HCV infected children. At this year EASL for the first time larger data sets of HCV therapy in children between 6 and 12 years of age was presented (9). The estimated prevalence of HCV infection in children is up to 0.4% in Europe and USA, and up to 6% in resource-limited countries. Although, SOF and LDV/SOF have been recently approved for children ≥12 years of age or ≥35 kg, for other pediatric patients, the standard of care is still limited to pegylated interferon + ribavirin (RBV) treatment for 24-48 weeks. More recently, a "half strength" single tablet fixed dose combination has been developed for younger children. The study presented at EASL now had the primary objective to study safety and tolerability of the half strength LDV/SOF 45/200 mg tablet in children aged between 6 and 12 years. The study design is shown below in figure 8.
Figure 8: Study design
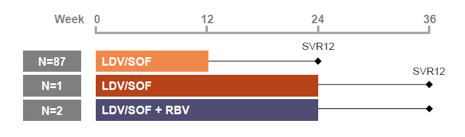
Of note in this open-label study in children aged 6-11 all patients received 12 weeks of LDV/SOF except GT1 treatment experienced cirrhotic patients (N=1) and GT3 patients (N=2). In the few subjects receiving RBV this was administered weight based. A PK lead-in substudy was performed in the first 12 patients to confirm dose. LDV/SOF 45/200 mg resulted in plasma concentration in children 6-11 years old generally within range of those observed in adults. The baseline characteristics of the entire study population are captured in table 4. Most children had acquired HCV infection vertically, mean age was 9.
Table 4: Baseline characteristics
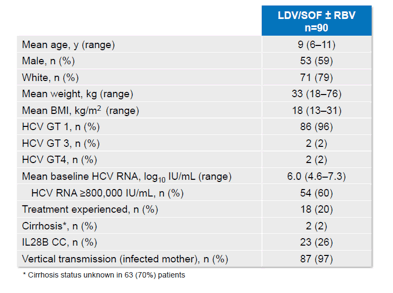
The overall SVR rates were excellent with only one GT1a child with cirrhosis developing relapse. The SVR12 rates fir the different study arms are shown in figure 9.
Figure 9: SVR12 results: LDV/SOF in Children 6 to 11 years
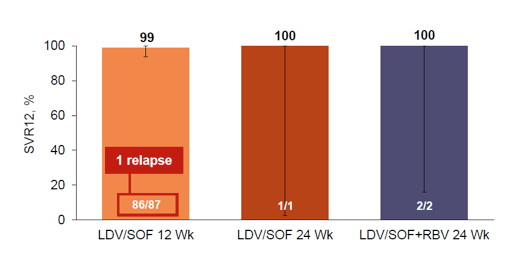
Baseline NS5A (15%) and NS5B (3%) NI RAVs (assessed by resistance testing using the 15% deep-sequencing cut-off) had no impact on SVR rates. LDV/SOF was very well tolerated; no child had to discontinue therapy due to any adverse event.
In summary, in GT1, 3, or 4 infected patients 6 to 11 years old, a single tablet regimen of LDV/SOF 45/200mg ± RBV for 12 or 24 weeks resulted in impressive high SVR12 rates ≥ 99%; within the study LDV/SOF 45/200 mg was very well tolerated.
Additional interesting data was presented from a smaller series of adolescents from Egypt which included 13 adolescents between 15 and 17 years (median: 16 years) with chronic HCV
infection (10). All subjects were negative for HBV, HIV and had no comorbidities; patients with cirrhosis beyond CHILD "A" score were excluded. The adolescents were classified according to the presence of cirrhosis (defined as ≥12.5 Kpa by fibroscan) into: Group (1): non-cirrhotics (n = 9) which then received sofosbuvir+daclatasvir for 12 weeks and Group (2): cirrhotics (n = 4): which received sofosbuvir + daclatasvir + ribavirin for 12 weeks. All patients in both treatment arms showed sustained viral response at 12 weeks post treatment (100%). Sofosbuvir and Dacalatasvir were safe and well tolerated. Indeed in this small number of patients ribavirin in cirrhotics did not increase the risk of adverse events. This pilot study prompts larger scale clinical trials in adolescents and children particularly in elimination models adopting treatment as prevention.
EASL: Ledipasvir/Sofosbuvir ± Ribavirin for 12 or 24 Weeks Is Safe and Effective in Children 6-11 years old with Chronic Hepatitis C Infection - (04/24/17)
What does the HCV treating physician need to watch out for under and after DAA based HCV therapy?
HBV reactivation under and after DAA therapy: what are the risks?
Previously, the FDA has issued a black-box warning on HBV reactivation in association with DAA-based HCV therapy following reports of HBV reactivation under DAA therapy with some severe clinical outcomes including liver failure and liver transplantation (11). The full overview of these findings have just been published in Annals of Internal Medicine (11). Overall, the FDA identified 29 unique reports of HBV-R in patients receiving DAAs from 22 November 2013 to 15 October 2016. Two cases resulted in death and 1 case in liver transplantation. Patients in whom HBV reactivation developed were heterogeneous regarding HCV genotype, DAAs received, and baseline HBV characteristics. At baseline, 9 patients had a detectable HBV viral load, 7 had positive results on hepatitis B surface antigen (HBsAg) testing and had an undetectable HBV viral load, and 3 had negative results on HBsAg testing and had an undetectable HBV viral load. For the remaining 10 patients, data points were not reported or the data were uninterpretable. Despite provider knowledge of baseline HBV, HBV reactivation diagnosis and treatment were delayed in 7 cases and possibly 7 others. Clearly, these reports have helped to alert clinicians for the possibility of HBV reactivation and emphasized the need for HBV screening prior to HCV therapy. As not all cases reported have full data available there are questions remaining in particular how frequent this really is and which patients may be at highest risk. At EASL results from a multicenter, open-label study at 14 sites in Taiwan was reported with administered HCV therapy to HBsAg positive patients only (12). Therefore, this is the first set of prospective data in a cohort of well-defined patients with chronic HBV/HCV coinfection. The study only included genotype (GT) 1 or 2 HCV-infected adults with HBV coinfection (HBsAg positive) who were currently not on HBV treatment (>6 months). The study design is shown below in figure 10.
Figure 8: Study design
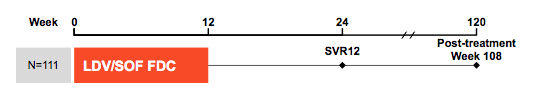
The baseline patient characteristics of the 111 subjects included into the trial are summarized below in table 4. Of note 16% had already compensated cirrhosis.
Table 4: Baseline characteristics

Of note on average HBV viral load was low but there were at least some patients with higher HBV-DNA levels up to 5.8 log10 IU/ml. HCV disease characteristics showed that only few patients were cirrhotic (16%) and one third was already HC treatment experienced. Overall response to 12 weeks of LDV/SOF was excellent with all patients achieving SVR12 (see figure 9).
Figure 9: SVR12 rates by genotype
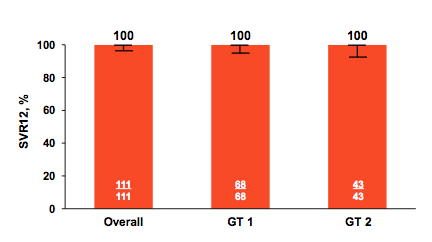
The main question of this trial however, was not overall SVR rate but really the risk for HBV reactivation or HBV associated hepatic flares. Long-term follow-up was performed through post-treatment Week 108 accordingly. Of note no patient had clinical adverse events recorded of jaundice, liver decompensation, liver failure or liver transplant. Increase in HBV viral load from undetectable at baseline to above lower limit of detection in combination with an increase in liver enzymes was not observed in a single patient. For the patients with detectable HBV-DNA at baseline 35% experienced a >1 - <2 log10 IU/mL increase in viral load, one patient in combination with significant ALT increase. 18% of HBV-DNA detectable patients had an even higher viral load increase of ≥2 log10 IU/mL at any visit; 4 subjects also developed an ALT >2x ULN increase. The HBV reactivation findings are summarized according to the reactivation criteria in table 5.
Table 5: Results: HBV reactivation
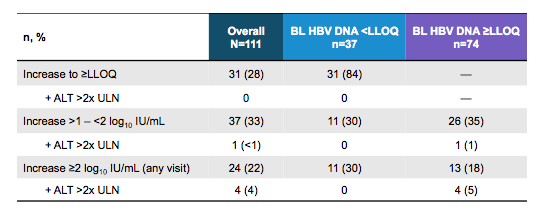
In summary, the risk of clinically relevant reactivation with significant liver enzyme increases was only noted in few patients with detectable HBV-DNA at baseline but not in one single case of a patient with undetectable HBV-DNA at baseline. Overall, only two patients started HBV therapy throughout the trial. One was a 60-year-old female with HCV GT 1b infection who was HBeAg negative and had cirrhosis at baseline. HBV DNA increased from 1.54log10 IU/mL(BL) to 3.8log10 IU/mL at Day 57 (Week 8) which was associated with an ALT increase from a nadir value of 41 to 71 IU/mL. The patient started HBV treatment on study Day 71 which normalized ALT and led HBV-DNA drop to below LLOQ. The second patient was a 61-year-old male with HCV GT 2 infection who was HBeAg negative without cirrhosis. HBV DNA increased from 2.28log10 IU/mL (BL) to 5.95log10 IU/mL 30 days post last dose (post-treatment Week 4) and was associated with ALT increase from a nadir value of
47 to 115 IU/mL. The patient started HBV treatment during post-treatment follow-up Week 5 and also reached ALT normalization and a decline in HBV-DNA levels.
In conclusion, LDV/SOF for 12 weeks achieved 100% SVR12 rate in patients with HBV and HCV GT 1 or 2 infections. Silent HBV viral reactivation was observed in 63% of patients (70/111) with however, no patient experienced clinical signs or symptoms of HBV reactivation. 5 (5%) patients had concomitant increase in ALT; 2 (2%) patients were started on HBV therapy. The updated EASL guidelines provide guidance on how to manage HCV therapy in HBV coinfected individuals: Patients commencing DAA-based treatment for hepatitis C should be tested for HBs antigen, anti-HBc antibodies and anti-HBs antibodies (21). If HBs antigen is present or if HBV DNA is detectable in HBs antigen-negative, anti-HBc antibody-positive patients (''occult" hepatitis B), concurrent HBV nucleoside/nucleotide analogue therapy is indicated (see recommendation box below). Assiduous monitoring of serum aminotransferase levels is indicated in anti-HBs and anti-HBc antibody-positive patients. Increased monitoring but not necessarily HBV antiviral therapy is recommended by other international guidelines.

EASL: Ledipasvir/Sofosbuvir for 12 Weeks Is Safe and Effective in Patients with Chronic Hepatitis C and Hepatitis B Coinfection: A Phase 3 Study in Taiwan - (04/24/17)
Hepatitis B Virus Reactivation Associated With Direct-Acting Antiviral Therapy for Chronic Hepatitis C Virus: A Review of Cases Reported to the U.S. Food and Drug Administration Adverse Event Reporting System - (05/30/17)
Is the risk for HCC occurrence or recurrence altered after DAA therapy?
At this year a whole set of studies was presented which dealt with the question whether the risk for HCC occurrence is impacted by DAA therapy (13-15). One paper which was presented during EASL was a systematic review and meta-analysis of more than 40 studies of initial or recurring HCC following DAA treatment (15). Out of more than 4000 potential studies, the researchers discarded those with incomplete data about the endpoints of interest, ending up with 26 relevant studies of HCC occurrence and 15 studies of HCC recurrence. Together these studies included a total of 13,875 participants. In an unadjusted analysis, the rate of initial HCC occurrence was 3.09 per 100 person-years (PY) for DAA-treated patients compared to 1.14 per 100 PY for those treated with interferon. For HCC recurrence, the rates were 12.14 vs 9.21 per 100 PY, respectively. Importantly, people treated with DAAs differed in some important ways from those treated during the interferon era. DAA-treated patients who initially developed liver cancer were older, on average, than those treated with interferon (60 vs 52 years). The age difference was less pronounced for people with recurrent HCC treated (64 vs 66 years, respectively). People treated with DAAs also had more advanced liver disease. All patients in the initial HCC occurrence studies who were treated with interferon had milder Child-Pugh Class A compensated cirrhosis, but about 30% of those treated with DAAs had more severe Class B or Class C decompensated disease. These were clearly patients who would not have been able to be treated with interferon based regimens in the past. Also it needs to be addressed that in these advanced patients with highest HCC risk some may already have had small tumors upon starting DAA therapy. Finally, follow-up time was much shorter for the DAA treated patients which may also impact the HCC rate in unadjusted analysis. After accounting for all factors mentioned, in a meta-regression analysis, the adjusted relative risk of DAA versus interferon treatment was 0.75 for initial HCC occurrence and 0.62 for HCC recurrence. Therefore the authors concluded, that there was no increased risk for HCC occurrence with DAAs, and in fact there was even a non-significant trend toward reduced risk.
Another large data set was presented from the Scottish HCV Clinical Database. HCC-naive individuals diagnosed with liver cirrhosis who received a course of antiviral therapy in Scotland from 1996-2016 resulting in a SVR were identified and followed from their treatment start date to the earliest of: date of death, date of HCC occurrence, or July 2016 (13). Poisson regression was then used to compare the risk of HCC occurrence according to treatment regimen (IFN-containing versus IFN-free) after adjusting for relevant co-factors (including: socio-demographic factors; baseline liver disease stage; comorbidities/health behaviours, virology, and previous treatment experience). Outcome data on HCC occurrence was ascertained directly from the HCV clinical database and validated against the Scottish Cancer registry. Treatment regimen was categorized as IFN-free versus IFN-containing, and alternatively (as, for instance, 26% of this cohort were treated with IFN in combination with sofosbuvir) as direct-acting-antiviral (DAA)-containing versus DAA-free. The marked differences in the patient population studied for the different HCV treatment regimens are captured in table 6.
Table 6: De-Novo HCC Risk Post-SVR Study: IFN-Containing Patients vs. IFN-free Patients: Baseline characteristics
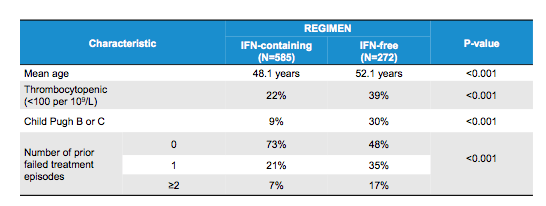
The results of the univariate and multivariate analysis evaluating the risk for de novo HCC occurrence following DAA therapy are shown below in figure 10.
Figure 10: Association Between IFN-Free versus IFN-containing Therapy and HCC Occurrence, in Univariate and Multivariate Analysis
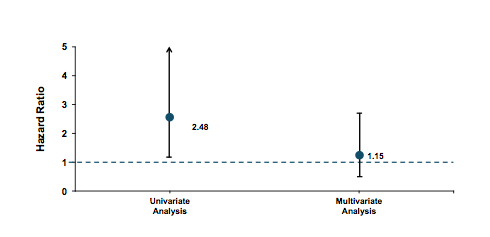
This study shows that there is no evidence that IFN-free therapy increases the risk of HCC occurrence in patients achieving an SVR. Baseline characteristics of patients treated with IFN-free regimens however differed significantly from those treated with IFN-containing regimens. Multivariate analysis demonstrated that the risk of HCC occurrence was equivalent between these two groups of patients.
At EASL also data from a prospective study was presented which evaluated the HCC occurrence in Chinese patients who achieved SVR after pegylated interferon-α plus ribavirin (PR) or direct-acting antivirals (DAAs) treatment in a real-life setting (14). Again compared to IFN, DAAs were not a risk factor for HCC (AHR 1.5 (95%CI 0.4-5.6), p= 0.50 in the cohort (n=721) with adjustment of age, sex, liver stiffness, diabetes mellitus, ALT and APRI score. Indeed, higher liver stiffness in combination with comorbid DM and increased age in Chines patients with HCV GT1b infection achieving SVR under DAA therapy.
EASL: Among Cirrhotic Patients with a Hepatitis C Sustained Viral Response, the Risk of De-novo Hepatocellular Carcinoma Relates to Baseline Factors and Not the Use of Direct Acting Antivirals: Results from a Nationwide Cohort - (04/21/17)
EASL: No evidence for higher risk of hepatocellular carcinoma occurrence or recurrence following direct-acting antiviral HCV therapy: A systematic review, meta-analyses, and meta-regression - (04/21/17)
EASL: No increase in the occurrence rate of HCC in Chinese treated by DAAs compared to PR after eradication of HCV: a long-term follow-up - (04/28/17)
New HCV drugs and combinations
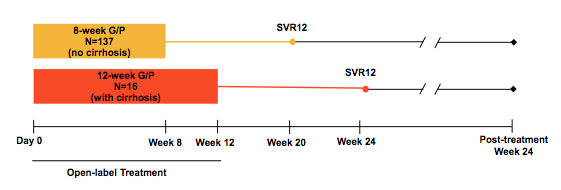
At this year EASL clearly the most new DAA data was presented for the new AbbVie combination with Glecaprevir (formerly ABT-493) a pangenotypic NS3/4A protease inhibitor coformulated with Pibrentasvir (formerly ABT-530) a pangenotypic NS5A inhibitor which are more commonly referred to as G/P (16-18). This was of particular interest as the new G/P combination is expected to receive FDA approval shortly and become commercially available this summer. In vitro data has shown a high barrier to resistance for this combination with potency against common NS3 polymorphisms (e.g., positions 80, 155, and 168) and NS5A polymorphisms (e.g., positions 28, 30, 31 and 93). Both drugs exert synergistic antiviral activity. G/P is coformulated and dosed once daily as three 100 mg/40 mg pills for a total dose of 300 mg/120 mg with food. Clinical PK characteristics are minimal metabolism and primary biliary excretion with negligible renal excretion (<1%). The first study to report back on was the EXPEDITION-1 study which had the objective to evaluate the efficacy and safety of G/P for 12 weeks in patients with HCV GT1, 2, 4, 5 or 6 infection and compensated cirrhosis (16) (GT3 patients with compensated cirrhosis had been previously enrolled in a separate study (22). The study design is shown below in figure 11.
Figure 11: Study design of the EXPEDITION-1 study
Patients were enrolled at 40 study sites in Belgium, Canada, Germany, South Africa, Spain, and the United States. Key inclusion criteria were: Chronic HCV GT1, 2, 4-6 infection (HCV RNA ≥1000 IU/mL) with compensated cirrhosis. Patients were either treatment-naïve or treatment-experienced with IFN, pegIFN ± RBV, or sofosbuvir (SOF) + RBV ± pegIFN. The baseline characteristics are shown below in table 7a and b.
Table 7a: Baseline characteristic of the EXPEDITION-1 study
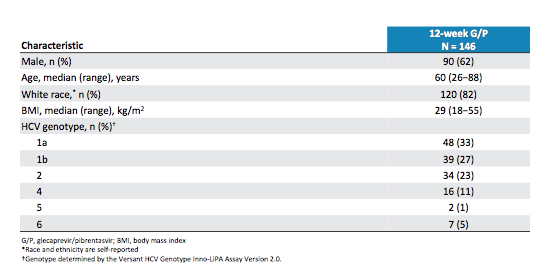
Of note most patients included had a genotype 1 infection so numbers for some of the other genotypes become too small to allow relevant conclusions.
Table 7b: Baseline characteristic of the EXPEDITION-1 study
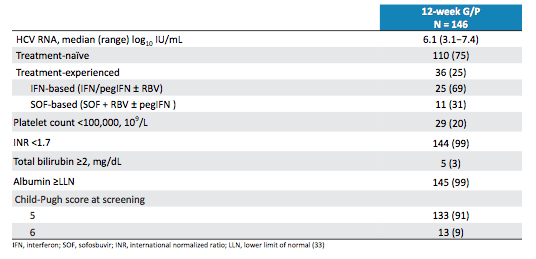
25% of the patients had already failed a prior HCV treatment. At baseline only 2% of patients had NS3 key baseline polymorphisms upon resistance testing, whereas 40% had only NS5A key polymorphisms. The overall SVR rates are shown below in figure 12.
Figure 12: SVR12 by Intent-to-Treat (ITT) Analysis
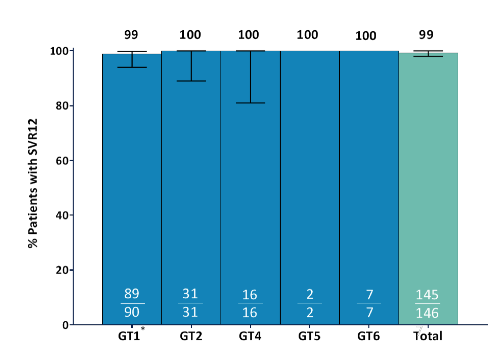
*One patient with HCV GT1a infection relapsed at PTW8 with no treatment-emergent substitutions present in NS3. In NS5A, Y93N was present at baseline; Y93N, Q30R and H58D were present at the time of failure. All other patients responded underlining the great potency of this regimen in early cirrhotics. Tolerability and safety were also excellent with no adverse events leading to study discontinuation. Table 8 summarizes the adverse events documented throughout the trial. There were no Grade 2 or higher ALT elevations in the trial, Grade 3 lab abnormalities were rare.
Table 8: Adverse events in EXPEDITION-1
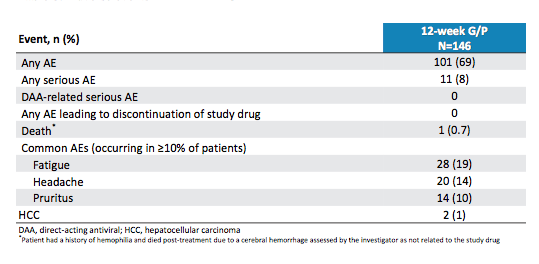
In summary, Glecaprevir/pibrentasvir for 12 weeks achieved a 99% SVR12 rate in the ITT population in patients with HCV GT1, 2, 4, 5 or 6 infection (but note very few GT 5 and 6 patients) and compensated cirrhosis. G/P was well-tolerated with a favorable safety profile with no DAA-related serious AEs or drug discontinuations.
EASL: EXPEDITION-I: Efficacy and Safety of Glecaprevir/Pibrentasvir for Treatment of Chronic Hepatitis C Virus Genotype 1, 2, 4, 5 or 6 Infection in Adults with Compensated Cirrhosis - (04/21/17)
AASLD: SURVEYOR-II, PART 3: EFFICACY AND SAFETY OF GLECAPREVIR/PIBRENTASVIR (ABT-493/ABT-530) IN PATIENTS WITH HEPATITIS C VIRUS GENOTYPE 3 INFECTION WITH PRIOR TREATMENT EXPERIENCE AND/OR CIRRHOSIS - (11/14/16)
The next G/P study to report back on was the first study with this DAA combination in HCV patients with HIV coinfection (17). The EXPEDITION-2 study was a phase 3, multi-center global study evaluating 8- or 12-week treatment with G/P in HCV/HIV-1 co-infected adults without or with compensated cirrhosis, respectively. The study design is shown below in figure 13.
Figure 13: Study design of the EXPEDITION-2 study.
With regard to baseline antiretroviral therapy (ART) patients either had to be (ART) naïve with CD4+ count ≥500 cells/mm3 or ≥29% or on a stable ART regimen for at least 8 weeks prior to screening, with CD4+ count ≥200 cells/mm3 or ≥14% and plasma HIV-1 RNA < LLOQ. Patients were mostly on an unboosted integrase inhibitor regime or Rilpivirin (see table 9). Boosted PIs were allowed after amendment II but since this was already late in the trial and most patients had been randomized no patient with boosted PI at baseline was included. Table 9a and b summarizes the main HIV and HCV disease characteristics at baseline.
Table 9a: Baseline characteristics from the EXPEDITION-2 study
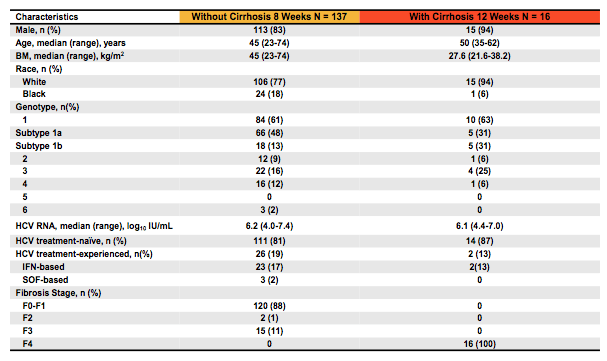
Table 9b: Baseline characteristics from the EXPEDITION-2 study
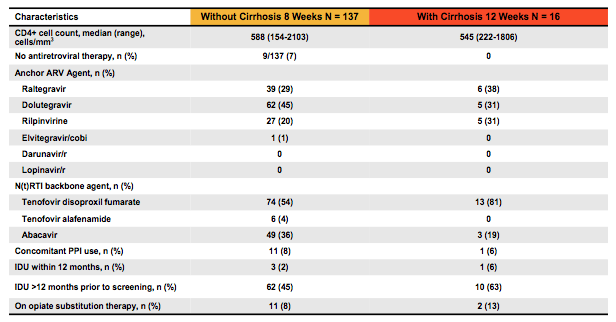
Overall, only 16 cirrhotics were included. Few patients were treatment experienced, mostly with IFN based therapy. A substantial proportion of patients included reported IDU >12 months prior to study inclusion. Quite impressively, all but one cirrhotic GT 3 patient who developed on-treatment virological failure at treatment week 8 achieved HCV cure. Genotypic evaluation of the failing patient revealed no NS3 polymorphisms at baseline; there was however an Y56H mutation at failure. In the NS5A region an A30V was found at baseline; S24F & M28K were determined at failure; (A30V not detected). The SVR12 results are summarized in figure 14.
Figure 14: EXPEDITION-2 Study: efficacy results
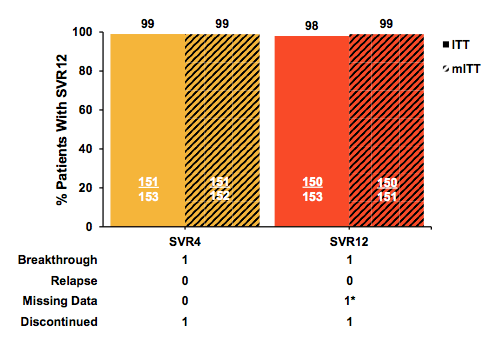
In conclusion, an overall SVR12 rate of 98% with no relapses was achieved in HCV/HIV-1 co-infected patients without or with cirrhosis following 8 or 12 weeks of G/P, respectively. Achievement of SVR12 was not impacted by high baseline viral load, cirrhosis status, or any other baseline factor. All patients maintained HIV-1 RNA suppression while on treatment. G/P was well tolerated and exhibited a similar safety profile in HCV/HIV-1 co-infected patients with or without cirrhosis; serious adverse events, clinically significant laboratory abnormalities, and treatment discontinuations were rare. In HCV/HIV-1 co-infected patients without cirrhosis, 8-week G/P yielded a 99.3% SVR12 rate, with no virological failures. These results suggest that the G/P regimen could be the first 8-week pangenotypic treatment option for HCV/HIV-1 co-infected patients without cirrhosis.
EASL: Efficacy and Safety of Glecaprevir/Pibrentasvir in Patients Co-infected With Hepatitis C Virus and Human Immunodeficiency Virus-1: The EXPEDITION-2 Study - (04/20/17)
The largest and probably most important G/P study presented was the ENDURANCE-3 trial (18). The ENDURANCE-3 trial compared the safety and efficacy of coformulated glecaprevir and pibrentasvir with SOF + DCV in GT3-infected patients without cirrhosis. Hepatitis C virus (HCV) genotype 3 (GT3) is the second most prevalent globally (30%) and is now increasingly recognized as the most difficult-to-cure HCV genotype. In GT3-infected patients without cirrhosis, a recommended treatment option is sofosbuvir (SOF) plus daclatasvir (DCV) for 12 weeks. Therefore, this study is one of the few HCV DAA trials with a comparator arm. The corresponding study design is depicted below in figure 15. Of note per discussion with regulatory authorities after phase 2 treatment data became available suggesting that shorter treatment durations may be feasible with this regimen, an 8 week treatment Arm of G/P was added to the study design allowing also to study shorter treatment duration for GT3 patients for whom so far did not exist. Note that only patients with chronic HCV GT3 infection (HCV RNA ≥1000 IU/mL), absence of cirrhosis (METAVIR score ≤3, or equivalent) and who were treatment-naïve were included, so clearly this was a somewhat more easy GT3 patient population to treat.
Figure 15: Study design of the ENDURANCE-3 trial.
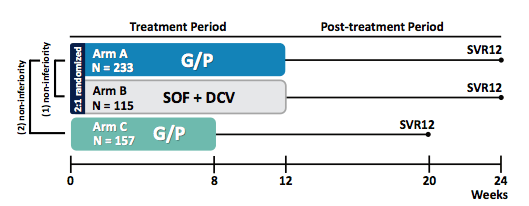
Patients were randomized 2:1 to the G/P and SOF + DCV arm, respectively. The main baseline characteristics are summarized below in table 10.
Table 10: Baseline characteristics of the ENDURANCE-3 study
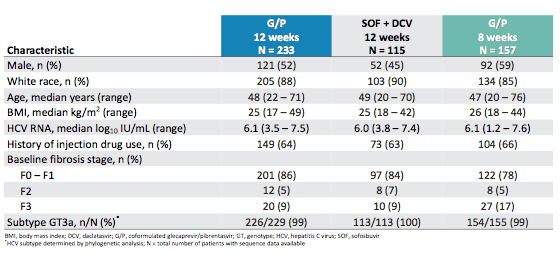
The majority of patients had a history of intravenous drug use (between 63 and 66%) and only few patients already had F3 fibrosis (between 9-17% for the 3 arms respectively). The main study results are shown below in figure 16.
Figure 16: SVR12 by Intent-to-Treat (ITT) Analysis: Results from the ENDURANCE trial.
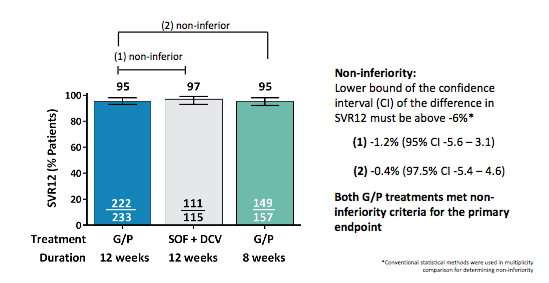
Most impressively, G/P achieved high efficacy in non-cirrhotic, treatment-naïve patients with chronic HCV GT3 infection with 12 weeks of G/P beings non-inferior to 12 weeks of SOF + DCV as well as 8 weeks of G/P being non-inferior to 12 weeks of G/P. These results suggest that indeed a shorter treatment duration of 8 weeks in easier to treat non-cirrhotic, treatment-naïve GT3 subjects may become available shortly. The treatment outcomes are depicted in table 11.
Table 11: Overall treatment outcomes
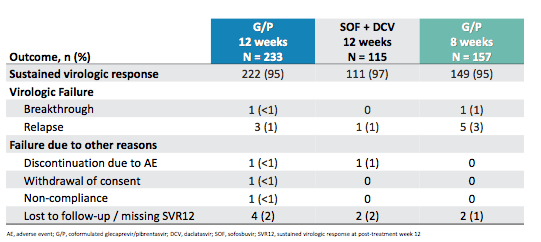
Overall, very few relapses occurred in three arms but numerically they were slightly higher in the 8 week arm. The therapy was well tolerated in all study arms and discontinuations because of adverse events were very rare. The SVR12 results in relation to the baseline resistance analysis are shown below in table 12.
Table 12: Resistance analysis from the ENDURANCE-3 study.
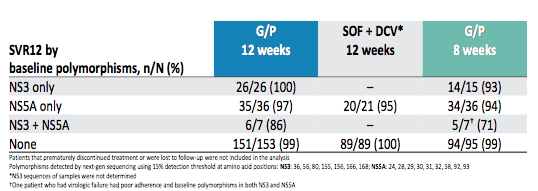
One patient who had virologic failure had poor adherence and baseline polymorphisms in both NS3 and NS5A
Overall, 97% (mITT analysis; 371/381) of GT3 infected patients receiving G/P achieved SVR12. 3% of patients (n = 10) had virologic failure. Common baseline polymorphisms in the NS3 region were A166S (n = 3) and in the NS5A region A30K (n=5). Common substitutions at failure were A30K+Y93H (n = 5) which confers a 69-fold resistance to PIB. Of note in the G/P for 8 weeks arm 5/5 (100%) patients with Y93H at baseline achieved SVR12.
Overall, G/P appears to show good GT3 activity and offers the option of 8 weeks treatment duration in easier to treat GT3 patients.
EASL: ENDURANCE-3: SAFETY AND EFFICACY OF GLECAPREVIR/PIBRENTASVIR COMPARED TO SOFOSBUVIR PLUS DACLATASVIR IN TREATMENT-NAïVE HCV GENOTYPE 3-INFECTED PATIENTS WITHOUT CIRRHOSIS - (04/21/17)
New HCV drugs and their role in retreatment of prior DAA failures.
Although, HCV cure rates under modern all oral DAA combination therapy are high, still a small percentage of up to 5% of patients exists which fail DAA combination therapy and where development of resistance may also impact subsequent salvage therapies. Therefore, a lot of interest has been generated for so called triplet regimens which include HCV drugs from three different drug classes and thereby may offer rescue options even for those patients who have developed prior drug resistance after failing on a HCV DAA combination therapy.
At previous conferences data on the new pangenotypic combination of Sofosbuvir/Velpatasvir/ Voxilaprevir (SOF/VEL/VOX) has been presented. SOF/VEL/VOX administered for 12 weeks demonstrated 96% sustained virologic response rate 12 weeks after treatment end (SVR12) in NS5A inhibitor-experienced patients and 98% SVR12 in direct-acting antiviral (DAA)-experienced patients who had not previously received an NS5A inhibitor in the POLARIS-1 and -4 Phase 3 studies, respectively (23,24). At EASL an integrated resistance analysis was presented from the POLARIS 1 and 4 study (23a). The objective of the study was to evaluate the effect of baseline resistance-associated substitutions (RASs) on treatment outcome and to determine the emergence of RASs in patients who experienced virologic failure in DAA-experienced patients treated with SOF/VEL/VOX for 12 weeks in POLARIS-1 and -4, respectively. The prevalence and impact on treatment outcome of NS3 and NS5A class RASs at baseline in DAA-Experienced Patients from the POLARIS 1 and 4 study are shown in figure 17.
Figure 17: Prevalence and Impact on Treatment Outcome of NS3 and NS5A Class RASs at Baseline in DAA-Experienced Patients
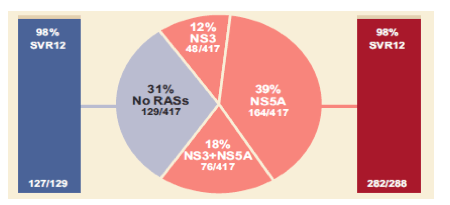
In DAA-experienced patients, overall or by study, baseline RASs did not impact SVR12 rate. The impact of RASs at baseline is further investigated by genotype in figure 18. In POLARIS-1 and -4, 93% (41/44) and 100% (9/9) of patients, respectively, with HCV GT 3 and NS5A RASs achieved SVR12 Indeed, numerically the lowest SVR12 rates were seen in GT3 patients with NS5A RASs at baseline, suggesting that despite very encouraging overall response rates there still will remain few patients who even under triplet retreatment will experience virological failure.
Figure 18: SVR12 in DAA-Experienced Patients With and Without Class RASs By HCV GT
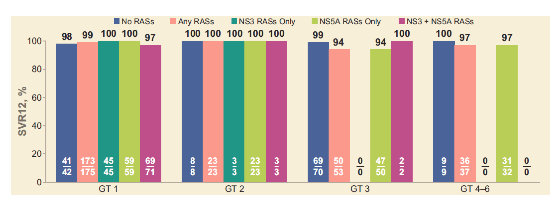
Overall, high SVR12 rates were observed in DAA-experienced patients treated with SOF/VEL/VOX for 12 weeks, and the presence of NS3, NS5A, and NS5B NI RASs did not impact treatment outcome significantly.
EASL: No Impact of RASs on the High Efficacy of SOF/VEL/VOX for 12 Weeks in DAA-Experienced Patients: an Integrated Resistance Analysis of the POLARIS-1 and POLARIS-4 Studies - (04/26/17)
AASLD: A Randomized, Controlled, Phase 3 Trial of Sofosbuvir/Velpatasvir/Voxilaprevir or Sofosbuvir/Velpatasvir for 12 Weeks in Direct-Acting Antiviral-Experienced Patients With Genotype 1-6 HCV Infection: The POLARIS-4 Study - (11/14/16)
AASLD: Sofosbuvir/Velpatasvir/Voxilaprevir for 12 Weeks as a Salvage Regimen in NS5A Inhibitor-Experienced Patients With Genotype 1-6 Infection: The Phase 3 POLARIS-1 Study - (11/15/16)
EASL2017: No Impact of RASs on the High Efficacy of SOF/VEL/VOX for 8 Weeks in DAA-Naïve Patients: an Integrated Resistance Analysis of the POLARIS-2 and POLARIS-3 Studies - (04/20/17)
AASLD: Integrated Analysis of Sofosbuvir +Ribavirin, Ledipasvir/Sofosbuvir or Sofosbuvir/Velpatasvir for the Treatment of Genotype 4 Chronic HCV Infection - (11/15/16)
The next interesting three drug class DAA combination therapy in previous DAA failures which was presented at EASL was the fixed-dose combination of grazoprevir (GZR), ruzasvir (RZR), and uprifosbuvir (20). These three drugs are co-formulated as a fixed-dose combination tablet; administered as 2 tablets once-daily for a total daily dose of 100 mg grazoprevir (GZR), 60 mg ruzasvir (RZR), and 450 mg of uprifosbuvir. The C-SURGE study was a multicenter, open-label trial which randomized 94 HCV GT1-infected participants who relapsed after a regimen of LDV/SOF or EBR/GZR were randomized 1:1 (stratified by GT1a/1b and cirrhosis) to either 16 weeks of GZR + RZR + UPR + RBV or 24 weeks of GZR + RZR + UPR without RBV. The study design is shown below in figure 19.
Figure 19: Study design of the C-SURGE study
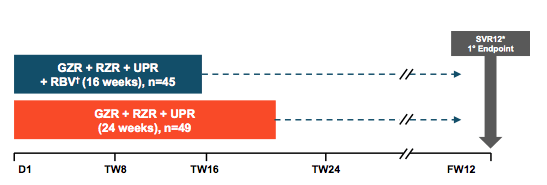
Overall, 94 subjects were enrolled into this study. The majority had failed prior 8-12 weeks of LDV/SOF and the rest (24%) EBR/GZR. Almost all patients had baseline NS5A RASs so clearly a difficult to treat patient group. Table 13 summarizes the main baseline characteristics of the patients for the two study arms.
Table 13: Baseline characteristics in the C-SURGE study
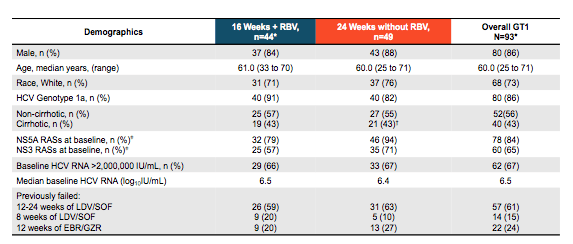
The overall response rates were very impressive with all patients responding in the modified data analysis (see figure 21) despite the extensive resistance conferring mutations at baseline (see figure 20).
Figure 20: C-SURGE Study: Baseline NS5A or NS3 RASs
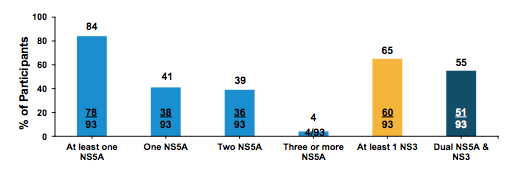
Figure 21: C-SURGE Study: Efficacy Results
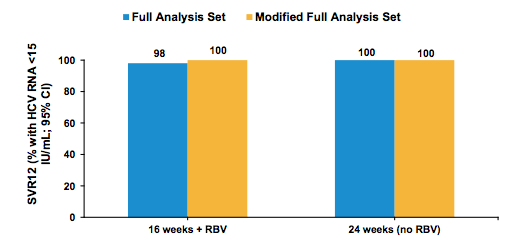
The full analysis set included all patients who received at least one dose of study medication;
The modified full analysis excluded one participant from the 16-week + RBV arm who withdrew from the study after taking only 3 doses of study medication. No difference in response was seen between the two arms thereby offering also a ribavirin free retreatment option with 24 weeks with superimposable SVR12 rate. The impact of the baseline RASs on SVR12 rates is shown in more detail in figure 22.
Figure 22: C-SURGE Study: Baseline NS5A or NS3 RASs on SVR12
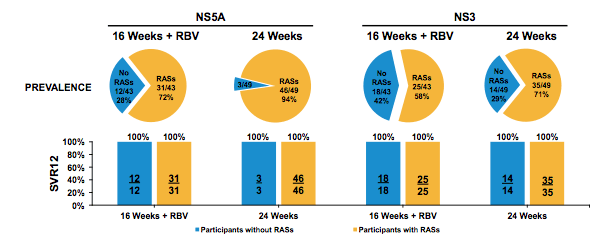
Additional analysis looking at the impact of baseline Y93 RASs in NS5a on SVR12 rate revealed that all patients were cured irrespective of the presence of this baseline RAS which is known to impact some of the other commercially available dual DAA combinations.
The results of the safety and tolerability investigations are summarized below in table 14.
Table 14: C-SURGE Study: Adverse Events
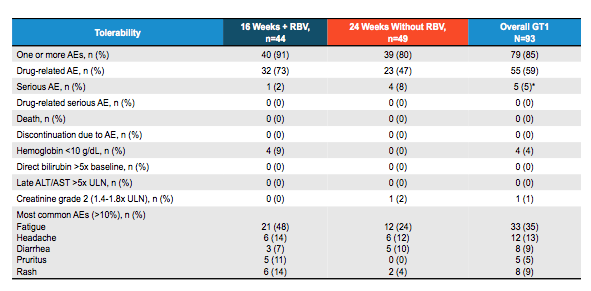
Of note, no patient discontinued therapy because of adverse events.
In conclusion, high efficacy was observed with grazoprevir(GZR)/ruzasvir (RZR)/uprifosbuvir (UPR) ± ribavirin (RBV) for treatment of GT1 prior DAA failures despite a high prevalence of baseline NS3 and NS5A RASs in this population. Treatment was generally safe and well tolerated. Considering the excellent outcome of this trial the question arises whether there is also potential for investigating the dual combination of RZR/UPR further. HCV PIs always have limitations as they cannot be used in very advanced liver cirrhosis stages.
EASL: Safety and Efficacy of the Fixed-dose Combination Regimen of Uprifosbuvir (MK-3682) / Grazoprevir / Ruzasvir in Cirrhotic or Non-cirrhotic Patients with Chronic HCV GT1 Infection Who Previously Failed a Direct-acting Antiviral Regimen (C-SURGE) - (04/24/17)
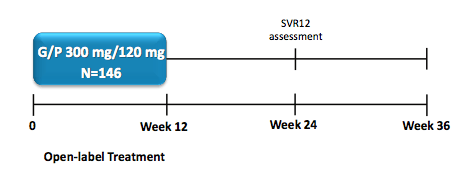
Finally, also interesting data was presented on G/P in the context of its use in prior DAA failures. In the MEGALLAN-1 study part 2 the objective was to determine the efficacy and safety of G/P for 12 or 16 weeks in patients with chronic HCV GT1, 4, 5 or 6 infection and prior DAA failure, including those with compensated cirrhosis. The study design is shown below in figure 23.
Figure 23: Study design MEGALLAN-1 part 2
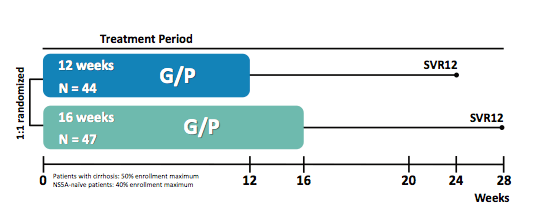
Patients were randomized 1:1, stratified by HCV GT and prior DAA experience, to receive 12 or 16 weeks of coformulated GLE/PIB (G/P; 300/120 mg). The primary endpoints were safety (including all patients receiving ≥1 dose of study drug) and the percentage of patients achieving sustained virologic response (HCV RNA <15 IU/mL) at post-treatment week 12 (SVR12). The baseline characteristics are summarized in table 15 a + b.
Table 15 a: Baseline characteristics of the MEGALLAN-1 part 2
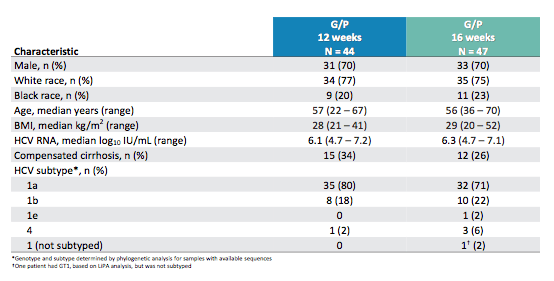
Of note, the majority of patients had GT1a HCV infections. 22-34% of patients already were classified as being cirrhotic at baseline thereby ensuring that there was a substantial proportion of very hard to treat patients included into this study.
Table 15 b: Baseline characteristics of the MEGALLAN-1 part 2 (continued)
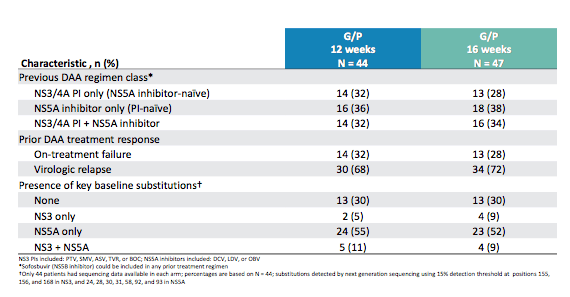
The majority of the prior DAA failures harbored NS5A baseline substitutions. Between 9-11% of patients had dual class resistance detectable upon resistance testing. Figure 24 a and b show SVR rates by DAA class in prior therapy and by key baseline substitutions from resistance testing.
Figure 24a: SVR12 by DAA Class in Prior Therapy
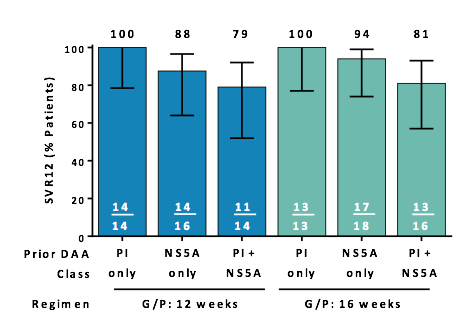
Figure 24b: SVR12 by Key NS3 and NS5A Baseline Substitutions
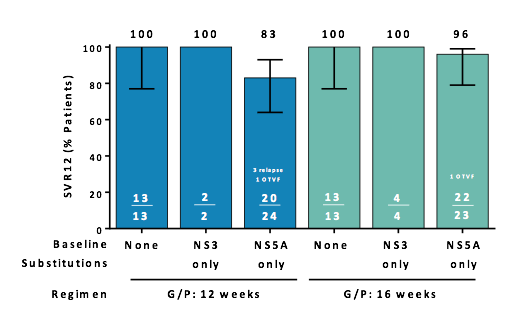
These results are very interesting as they do provide a strong basis for resistance testing after DAA failure in case G/P is considered as retreatment option. Patients with prior failure to PI containing regimens (NS5A inhibitor-naïve) achieved a 100% SVR12 with 12 or 16 weeks of G/P treatment whereas patients with prior failure to both PI- and NS5A inhibitor-containing regimens had significantly lower SVR12 rates. Patients with prior failure to NS5A inhibitors (i.e., LDV or DCV); NS3/4A PI-naïve achieved a 94% SVR12 rate with 16 weeks of G/P treatment with no relapse suggesting that duration extension may be helpful in this particular patient group. Whereas there was no impact of baseline NS5A substitutions on SVR12 rates, SVR12 rates were strongly impacted in the presence of both baseline NS3 and NS5A substitutions, respectively. Indeed only 5/9 patients with double class resistance achieved SVR12. G/P for 12 or 16 weeks was well tolerated; Grade 3 lab abnormalities were rare, with no discontinuations due to AEs, and no DAA-related serious AEs.
EASL: MAGELLAN-1, PART 2: GLECAPREVIR/PIBRENTASVIR FOR 12 OR 16 WEEKS IN PATIENTS WITH CHRONIC HCV GENOTYPE 1 OR 4 AND PRIOR DIRECT-ACTING ANTIVIRAL TREATMENT FAILURE - (04/24/17)
EASL: New HCV Drugs at EASL 2017 - (05/09/17)
HCV elimination programs: what is working, where are the gaps?
Georgia is a country in the Caucasus with an estimated population of ~3.7 million. A very high hepatitis C prevalence can be found in Georgia which is estimated to be about 7.7% antibody (exposed) and 5.4% PCR+ (150,300 chronic infections). Back in 2015 an HCV elimination plan was launched which became possible because of a very tight cooperation between all stakeholders in the HCV arena as well as considerable governmental good will and the donation of HCV DAAs for free from Gilead. Besides increased roll-out of HCV DAA therapy the national program also incorporated efforts to increase screening for HCV and introduce increased harm reduction measures. Thereby, Georgia is one of the first countries which can potentially reach the new WHO elimination targets for HCV. At EASL work was presented which projected the impact of the program in terms of infections and HCV-related deaths averted and also assessed the feasibility of achieving the elimination goal (26). The authors developed a model of HCV transmission incorporating changing demographics of people who inject drugs (PWID) and the general population in Georgia. The model was calibrated to HCV prevalence by age, gender and PWID status with data from a 2015 national serosurvey and PWID surveys from 1997 to 2015. Then infections and deaths averted by 2030 were estimated due to the 19,338 initiated treatments (98% of the first ∼9000 treatments were to patients with METAVIR scores of F3-F4). The authors projected whether the elimination goal will be reached if treatment continues at the current rate of 2100/month or 80% of prevalent infections annually when prevalence is low, including scenarios combining treatment with increased coverage of harm-reduction measures for PWID (opiate
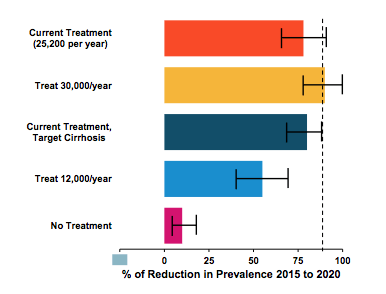
substitution therapy (OST) and needle and syringe programs (NSP)) or prioritizing treatments for PWID. Of note HCV prevalence is already declining slightly in Georgia without intervention. According to their calculations the current treatment rate (25,200 per year) will lead to 87.1% (73.4 - 93%) reduction in prevalence by the end of 2020. However, if treatment numbers decline target will not be reached. The findings of this analysis are captured in figure 25.
Figure 25: HCV Elimination in Georgia Study: Impact on Prevalence
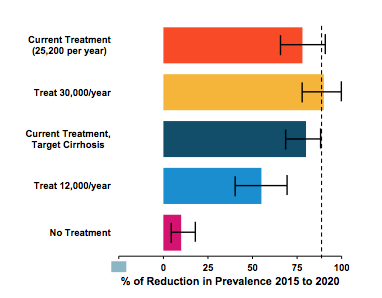
The HCV incidence in Georgia is already declining due to harm reduction. As with prevalence, the targeted approach is a 90% reduction by 2020. If PWID are not treated, there will be a reduced impact on incidence. It is estimated that 11,000 (4,800-24,000) new infections have been averted by 2030 due to treatments given so far. The impact of the elimination program is demonstrated in figure 26.
Figure 26: HCV Elimination in Georgia Study: Impact on Incidence
Liver disease associated mortality however, is still increasing due to the aging of the infected population and due to the fact that most infections were acquired back in the 1990s. The authors calculated that it would be unlikely to reach the WHO target by
2020 (65% reduction in mortality). A 35% (18-48%) decrease in mortality was estimated if one would not target cirrhosis and a 45% (31-54%) decrease was estimated if cirrhosis was targeted. Clearly, targeting patients with cirrhosis increases the impact on mortality. Overall, 2200 (136-3,269) HCV-related deaths are estimated to be averted by 2030 due to HCV treatments in Georgia so far. The impact on mortality through the Georgian elimination program is summarized in figure 27.
Finally,
Figure 27: HCV Elimination in Georgia Study: Impact on Mortality
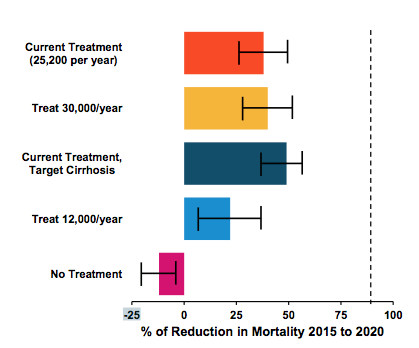
In conclusion, Georgia is on the path to achieving the HCV elimination target by 2020 if current rates of HCV treatment continue, especially if treatments for PWID and harm-reduction measures are prioritized. However, to maintain the necessary treatment rate, current rates of case-finding need to be scaled up. So far only 20% of all people living with HCV in Georgia are believed to be having been already diagnosed successfully making increased screening and identification of further HCV cases crucial for meeting WHO targets.
EASL: Projected impact and pathways to success of the hepatitis C virus elimination program in Georgia, 2015-2020 - (05/30/17)
One other often discussed patient population with potential for HCV elimination efforts are prison inmates. Obviously, the prison setting provides a unique opportunity to engage and treat high risk individuals with the goal of reducing HCV prevalence and preventing transmission. However, to date there have been few data to support the efficacy of prison-based treatment programs using IFN-free DAA therapy. A nurse-led state-wide hepatitis program has been developed and implemented in 14 prisons in Victoria, Australia to assess and treat prisoners living with chronic viral hepatitis. At EASL data was presented from a study which evaluated the efficacy of antiviral therapy delivered in the prison system using this model (27). All prisoners were offered screening for viral hepatitis on prison entry and when moving between prison sites. Seropositive prisoners were referred for protocol-driven face-to-face (F2F) assessment by a Clinical Nurse Consultant (CNC) who visited their local prison. CNCs conducted interviews, clinical assessments, liver stiffness measurement using transient elastography, and organized blood tests with participants in their local prisons. Patients were triaged for consultation by supervising hepatologists via telemedicine or F2F at a central prison. The study reported on > 6,000 prisoners in Victoria with an estimated HCV seroprevalence of >30%. Clinical assessments started in October 2015, the DAA treatment program started in March 2016 with initially 6 treatments per week Mar - June and eventually 16 treatments per week from July 2016 onwards. Overall, 1180 prisoners have been assessed in the program so far with 718 prisoners being eligible for therapy and 633 having started DAA therapy. 244 prisoners have already achieved SVR12 rates which were presented at this first analysis at EASL. 87% (n = 212) were male, genotype 3 HCV = 46%, Genotype 1a HCV = 46%. 37% of subjects had a liver stiffness measurement > 9.5%. 92% reported a history of injecting drug use. Only 8% were HCV treatment experienced, with the majority (78%) never have being engaged in HCV care before. This already underlines how through this program patient groups are brought into HCV management and health care which previously mostly have not been reached at all. The prisoners were commenced on a whole variety of DAA combination therapies including Sofosbuvir + Ledipasvir for 8 (32%) and 12 (17%) weeks, respectively, Sofosbuvir + Daclatasvir 12 weeks (34% or 24 weeks (9%) and to a smaller extent other regimens including the Abbvie 3D regimen. The treatment outcome for the first patients which had SVR12 data available is shown in figure 28.
Figure 28: Outcome of antiviral HCV therapy in the prison setting
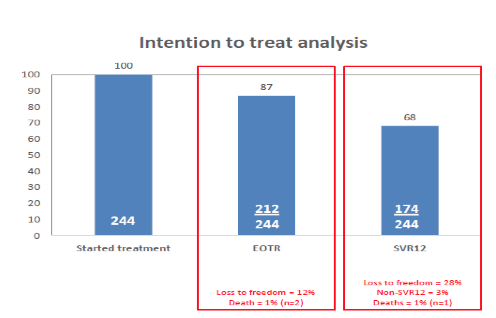
Overall, efficacy looks very good but patients are increasingly lost to follow-up as they are being released into freedom during follow-up. In the per protocol analysis 95% achieved SVR12, 4 patients had documented relapse, 2 died and 2 were reinfected.
Clearly the first results of this ongoing effort suggest that treatment for HCV can be delivered safely, effectively and in high numbers in the prison setting using an innovative nurse led model of care. Prisoner uptake and treatment response rates have been excellent. The prison setting provides an excellent opportunity to engage and treat high risk individuals, and should be part of public health platforms that support the elimination of HCV.
EASL: Outcomes of Treatment for Hepatitis C Virus Infection in the Prison Setting - (05/30/17)
Clearly, cost of DAA based therapy is most often referred to as the main barrier to access of modern all oral HCV therapy. Successful examples of HCV treatment roll-out often in combination with increased screening HCV efforts and broader introduction of harm reduction programs however, underline that if all stakeholders in the HCV space get together and can spark governmental support large numbers of patients can be successfully treated. In particular models of reimbursement which tie the price of HCV DAAs to the volume of prescribed antivirals have allowed substantial cost reductions and allowed to treat significantly more patients. First effects on prevalence, incidence and liver disease associated mortality already can already been seen which should serve as a visionary hope that HCV elimination despite all barriers is moving ahead. Most importantly, the increased availability of generics has helped to further increase access to DAA based therapy. At this year EASL there was an update on the efficacy of generics for treatment of HCV in various regions of the world (28). This year analysis assessed the efficacy of generic imported DAAs in four treatment programs. Generic versions of Sofosbuvir (SOF), Ledipasvir (LDV), Daclatasvir (DCV) and Velpatasvir were sourced from generic suppliers in India, Bangladesh, Egypt and China. Four treatment access programs in Russia, South East Asia and Australia were included in the analysis. The choice of DAAs and treatment length were determined from baseline HCV Genotype and stage of fibrosis. Patients were evaluated pre-treatment, at week 4 (RVR), at the end of treatment (EOT) and then for SVR 4 and 12. The main end-of-treatment and SVR4 results for the different generic combinations used are shown in figure 29.
Figure 29: Generic DAA treatment: HCV RNA < LLOQ in EOT and SVR4
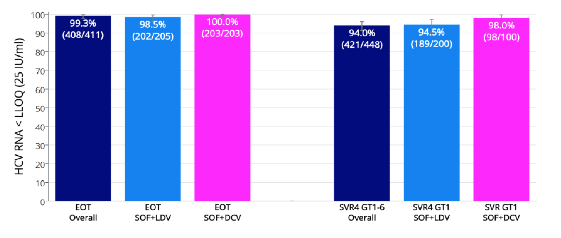
These SVR results underline once more that DAA based HCV therapy also as generics works very well and has great potential to contribute in achieving the WHO HCV elimination targets.
Summary
⋅The new estimated number of HCV infections globally was reported at EASL to be considerably less than before with a prevalence of 71 Million worldwide. The incidence was estimated as 1.75 million new HCV infections per year (mostly due to unsafe health care and injection drug use).
⋅Of note 20% of all HCV infections globally are estimated to be diagnosed in 2017. Also HCV treatment coverage worldwide is still below 10% emphasizing the need of considerable HCV treatment scale-up to reach the WHO 80% HCV treatment target in 2030.
⋅High SVR rates can be achieved in persons receiving opiate agonist therapy including those actively using drugs. In PWIDs directly observed and group therapy had higher rates of adherence compared to individual care.
⋅Real world effectiveness of EBR/GZR in the VA population is comparable to efficacy rates reported in clinical trials. SVR rates were high across patient subgroups regardless of gender, race/ethnicity, presence of cirrhosis, renal impairment or HIV co-infection.
⋅In GT1, 3, or 4 infected patients 6 to 11 years old, a single tablet regimen of LDV/SOF 45/200mg ± RBV for 12 or 24 weeks resulted in impressive high SVR12 rates ≥ 99%; within the study LDV/SOF 45/200 mg was very well tolerated.
⋅Sofosbuvir plus Daclatasvir is a safe, highly efficacious pangenotypic regimen in adolescents with chronic HCV and added ribavirin in cirrhotics (CHILD A) did not increase the risk of adverse events.
⋅LDV/SOF for 12 weeks achieved 100% SVR12 rate in patients with
HBV and HCV GT 1 or 2 infections. Silent HBV viral reactivation was observed in 63% of patients (70/111) with however, no patient experienced clinical signs or symptoms of HBV reactivation. 5 (5%) patients had concomitant increase in ALT; 2 (2%) patients were started on HBV therapy.
⋅No evidence for differential HCC occurrence or recurrence risk following SVR from DAA and IFN-based regimens was found in a meta-analysis on HCC risk after DAA therapy. The higher incidence following DAA therapy can be explained by shorter duration follow-up (cohort effect), and older age (higher baseline risk).
⋅Data from the Scottish HCV Clinical Database as well from Hong Kong and China suggest that the risk of HCC following SVR relates to baseline risk factors and not the use of DAAs.
⋅Glecaprevir/pibrentasvir for 12 weeks achieved a 99% SVR12 rate in the ITT population in patients with HCV GT1, 2, 4, 5 or 6 infection (but note very few GT 5 and 6 patients) and compensated cirrhosis. G/P was well-tolerated with a favorable safety profile with no DAA-related serious AEs or drug discontinuations.
⋅An overall SVR12 rate of 98% with no relapses was achieved in HCV/HIV-1 co-infected patients without or with cirrhosis following 8 or 12 weeks of G/P, respectively. G/P was well tolerated; serious adverse events, clinically significant laboratory abnormalities, and treatment discontinuations were rare. In HCV/HIV-1 co-infected patients without cirrhosis, 8-week G/P yielded a 99.3% SVR12 rate, with no virological failures. These results suggest that the G/P regimen could be the first 8-week pangenotypic treatment option for HCV/HIV-1 co-infected patients without cirrhosis.
⋅Overall, G/P appears to show good GT3 activity and offers the option of 8 weeks treatment duration in easier to treat GT3 patients.
⋅High SVR12 rates were observed in DAA-experienced patients treated with SOF/VEL/VOX for 12 weeks, and the presence of NS3, NS5A, and NS5B NI RASs did not impact treatment outcome.
⋅Grazoprevir (GZR)/ruzasvir (RZR)/uprifosbuvir (UPR) ± ribavirin (RBV) was highly effective in GT1 participants who previously failed an NS5A inhibitor-containing direct-acting antiviral regimen.
⋅Patients with prior failure to PI containing regimens (NS5A inhibitor-naïve) achieved a 100% SVR12 with 12 or 16 weeks of G/P treatment whereas patients with prior failure to both PI- and NS5A inhibitor-containing regimens had significantly lower SVR12 rates. Patients with prior failure to NS5A inhibitors (i.e., LDV or DCV); NS3/4A PI-naïve achieved a 94% SVR12 rate with 16 weeks of G/P treatment with no relapse suggesting that duration extension may be helpful in this particular patient group. For dual class resistant patients efficacy appears to be less so addition of RBV or longer durations would need to be studied.
⋅Georgia is on the path to achieving the HCV elimination target by 2020 if current rates of HCV treatment continue, especially if treatments for PWID and harm-reduction measures are prioritized. However, to maintain the necessary treatment rate, current rates of case-finding need to be scaled up. So far only 20% of all people living with HCV in Georgia are believed to be having been already diagnosed successfully making increased screening and identification of further HCV cases crucial for meeting WHO targets.
⋅Treatment for HCV can be delivered safely, effectively and in high numbers in the prison setting using an innovative nurse based model of care. Prisoner uptake and treatment response rates have been excellent. The prison setting provides an excellent opportunity to engage and treat high risk individuals, and should be part of public health platforms that support the elimination of HCV.
References
1. WHO Global Hepatitis Report.
www.who.int/hepatitis/publications/global-hepatitis-report2017
2. Grebly J, et al. SIMPLIFY Study: Efficacy and Safety of SOF/VEL in People with Chronic HCV Infection and Recent Injecting Drug Use. 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract FRI-234
3. Grebly J, et al: Safety and Efficacy of Ombitasvir, Paritaprevir/Ritonavir and Dasabuvir With or Without Ribavirin in Chronic Hepatitis C Patients Receiving Opioid Substitution Therapy: A Pooled Analysis Across 12 Clinical Trials. 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract FRI-236
4. Litwin AH, et al. The PREVAIL Study: Intensive Models of HCV Care for People who Inject Drugs. 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract PS-130
5. Flisiak R, et al. Patients Above 65 Years of Age Achieved the Same SVR12 as Younger Pati ents Despite Increased Comorbidities: Findings From a Large Real-World, Multi -Country, Observational Cohort of 12-Week Ombitasvir/Paritaprevir/Ritonavir ± Dasabuvir ± Ribavirin. 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract SAT-193
6. Ippolito AM, et al. HCV clearance after direct-acting antivirals in cirrhotic patients by stages of liver impairment: the ITAL-C network study. 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract THU-227
7. Kramer J, et al. Real World Experience with Elbasvir/Grazoprevir in the Veterans
Affairs Healthcare System. 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract PS-095.
8. Curry M, et al. Utilization of sofosbuvir/velpatasvir in genotype 2-6 HCV: real-world experience from the TRIO network. 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract PS-102
9. Murray KF, et al. Ledipasvir/Sofosbuvir ± Ribavirin for 12 or 24 Weeks Is Safe and Effective in Children 6-11 years old with Chronic Hepatitis C Infection. 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract PS-101
10. El-Sayed M, et al. A pilot study for safety and efficacy of 12 weeks sofosbuvir plus daclatasvir with or without ribavirin in Egyptian adolescents with chronic hepatitis C virus Infection. 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract THU-412
11. Bersoff-Matcha SJ, et al. Hepatitis B Virus Reactivation Associated With Direct-Acting Antiviral Therapy for Chronic Hepatitis C Virus: A Review of Cases Reported to the U.S. Food and Drug Administration Adverse Event Reporting System. Ann Intern Med. 2017 Apr 25. doi: 10.7326/M17-0377. [Epub ahead of print]
12. Liu CJ, et al. Ledipasvir/Sofosbuvir for 12 Weeks Is Safe and Effective in Patients with Chronic Hepatitis C and Hepatitis B Coinfection: A Phase 3 Study in Taiwan. 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract PS-098
13. Innes H, et al. Among Cirrhotic Patients with a Hepatitis C Sustained Viral Response, the Risk of De-Novo Hepatocellular Carcinoma Relates to Baseline Factors and Not the Use of Direct Acting Antivirals: Results from a Nationwide Cohort. 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract PS-035
14. Ji D, et al. No increase in the occurrence rate of hepatocellular carcinoma in Chinese treated by direct-acting antivirals compared to Interferon after eradication of hepatitis c virus: a long-term follow-up. 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract PS-037
15. Waziry R, et al. No evidence for higher risk of hepatocellular carcinoma occurrence or recurrence following direct-acting antiviral HCV therapy: A systematic review, meta-analyses, and meta-regression. 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract PS-160
16. Forns X, et al. EXPEDITION-I: Efficacy and Safety of Glecaprevir/Pibrentasvir in
Adults with Chronic Hepatitis C Virus Genotype 1, 2, 4, 5 or 6 Infection and Compensated Cirrhosis. 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract GS-006
17. Rockstroh J, et al. Efficacy and Safety of Glecaprevir/Pibrentasvirin Patients Coinfected with Hepatitis C Virus and Human Immunodeficiency Virus-1: the EXPEDITION-2 Study. 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract LBP-522
18. Foster GR, et al. ENDURANCE-3: Safety and efficacy of glecaprevir/pibrentasvir
compared to sofosbuvir plus daclatasvir in treatment-naïve HCV genotype 3-infected patients without cirrhosis. 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract GS-007
19. Sarrazin C, et al. No Impact of RASs on the High Efficacy of SOF/VEL/VOX for 12 Weeks in DAA-Experienced Patients: an Integrated Resistance Analysis of the POLARIS-1 and POLARIS-4 Studies. 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract THU-248.
20. Wedemeyer H, et al. Safety and Efficacy of the Fixed-Dose Combination Regimen of MK-3682/Grazoprevir/Ruzasvir in Cirrhotic or Non-Cirrhotic Patients with Chronic HCV GT1 Infection who Previously Failed a Direct Acting Antiviral Regimen (C-SURGE). 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract PS-159
21. EASL Recommendations on Treatment of Hepatitis C 2016, J Hepatol in press
22. Gane E, et al. High Efficacy of ABT-493 and ABT-530 Treatment in Patients With HCV Genotype 1 or 3 Infection and Compensated Cirrhosis. Gastroenterology. 2016 Oct;151(4):651-659.
23. Bourliere M et al.: Sofosbuvir/Velpatasvir/Voxilaprevir for 12 Weeks as a Salvage Regimen in NS5A Inhibitor-Experienced Patients with Genotype 1-6 Infection: The Phase 3 POLARIS-1 Study. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 194
23a. No impact of RASs on the high efficacy of SOF/VEL/VOX for 12 weeks in DAA- experienced patients: an integrated resistance analysis of the POLARIS-1 and POLARIS-4 studies. 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract THU-248
24. Zeuzem S et al.: A Randomized, Controlled, Phase 3 Trial of Sofosbuvir/Velpatasvir/Voxilaprevir or Sofosbuvir/Velpatasvir for 12 Weeks in Direct Acting Antiviral-Experienced Patients with Genotype 1-6 HCV Infection: The POLARIS-4 Study. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 109
25. Poordad F, et al. MAGELLAN-1, Part 2: Glecaprevir/Pibrentasvir for 12 or 16 Weeks in Patients with
Chronic HCV Genotype 1 or 4 and Prior Direct-Acting Antiviral Treatment Failure. 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract PS-156
26. Walker JG, et al. Projected impact and pathways to success of the hepatitis C virus elimination program in Georgia, 2015-2020. 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract PS-125
27. McDonald L, et al. Outcomes of treatment for hepatitis C virus infection in the prison setting. 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract PS-126
28. Freeman J, et al. Sustained virological response for 94% of people treated with low cost, legally imported generic direct acting antivirals for hepatitis C: analysis of 1087 patients in 4 treatment programmes. . 52nd EASL; Amsterdam, Netherlands; April 19-23, 2017. Abstract PS-097
|
| |
|
 |
 |
|
|