| |
Eradication of HCV and non-liver-related non-AIDS-related events (CVD/diabetes/kidney/cancers) in HIV/HCV coinfection
|
| |
| |
Download the PDF here
from Jules: this study in HCV/HIV coinfected reports reduced diabetes from SVR and reduced renal disease that was not significant & they did nit find CVD reduced or cancers, but other studies in healthier patients have found that SVR can improve the risk for all these outcomes.......
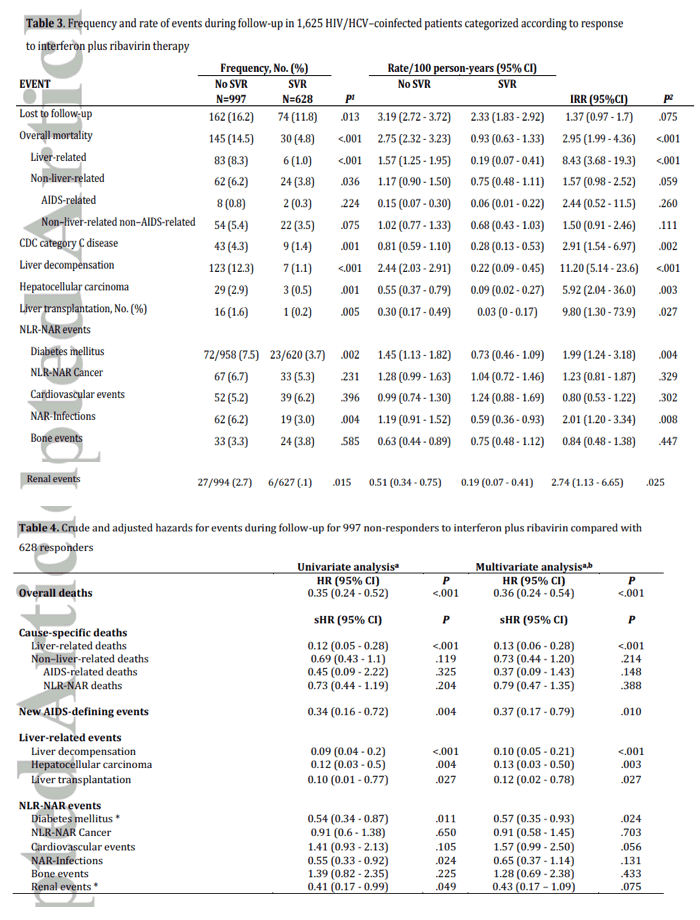
"Although the study design precludes determination of causality, our resultssuggest that eradication of HCV in coinfected patients is associated not only with a reduction in overall death, liver-related death [see table 3], new AIDS-related events, and alltypes of liver-related events, but also with a statistically significant reduced hazardof diabetes mellitus and a decline in the hazard of chronic renal failure very closeto the threshold of significance.These findings argue for the prescription of HCVtherapy regardless of liver fibrosis stage in coinfected patients."
from Jules: bear in mind that in this Spanish study 80% of patients had IDU history so this confounds benefits of SVR because IDU is associated with worse renal function & perhaps cancers & CVD. IDU is associated with increased immune activation which can lead to increased risk for comorbidities
CROI/2016: Understanding the Relative Contributions of IDU and HCV on Systemic Immune Activation HCV should be aggressively treated in current IDUs even more if HIV and/or HCV positive - (04/4/16)
Reported at AASLD was this study showing improved renal function with SVR-
AASLD: The Impact of Hepatitis C Viral Cure on Progression of Renal Disease - (11/14/16)
Extrahepatic Morbidity and Mortality of Chronic Hepatitis C Review - SVR Clears/Reduces Extrahepatic Manifestations.....http://www.natap.org/2015/HCV/110515_04.htm HCV-infected patients have increased rates of insulin resistance, diabetes, and atherosclerosis, which may lead to increased cardiovascular morbidity and mortality.....this review discusses the many extra hepatic manifestations of HCV including heart disease, NHL/cancer, neurologic & the brain, touches on kidney disease, mixed cryoglobulinemia (MC)....and describes how SVR reduces or clears these disease and improves overall survival....."In a long-term study of 530 patients with advanced fibrosis or cirrhosis, SVR was associated with significantly reduced all-cause mortality.9 Other studies have also shown the extrahepatic benefits of HCV eradication (Table 3); patients with SVR after peginterferon and ribavirin therapy have reduced steatosis, a lower incidence of malignant lymphoma,121 reduced risk of type 2 diabetes mellitus143 and insulin resistance,38, 39, 144, 145, 146 improved cognitive performance,105 reduction in fatigue,147, 148 improvement in myocardial perfusion defects,75 reduced incidence of stroke,76 reduced renal and cardiovascular outcomes in the presence of diabetes,51 complete resolution of MC-related complications,17, 117 and regression or complete remission of HCV-associated lymphoma.119 It is also clear that interferon and ribavirin-free treatment results in improved patient-reported outcomes in many patient groups after as early as 2 weeks of treatment. Clinically important gains in quality of life are associated with SVR.20, 21 Thus, multiple studies have shown that durable HCV eradication achieved with interferon-based therapies improves both liver-related and non-liver-related outcomes."
and this study finding HCV associated with increased risk for non-HCV associated cancers for which perhaps SVR can reduce risk.
AASLD: Chronic Hepatitis C Virus Infection and Cancer Risks: A Population-Based Cohort Study - (11/14/16)
DDW/2015: CANCER RATES IN PATIENTS WITH CHRONIC HEPATITIS C IN A LARGE U.S. HEALTH MAINTENANCE ORGANIZATION - (05/28/15)
Increased incidence of cancer and cancer-related mortality among persons with chronic hepatitis C infection, 2006-2010 - (09/18/15)

Eradication of HCV and non-liver-related non-AIDS-related events in HIV/HCV coinfection
Hepatology Jan 21 2017
Juan Berenguer1,2, Elena Rodriguez-Castellano3, Ana Carrero1,2, Miguel A VonWichmann4, Marta Montero5, Mar.a J Galindo6, Josep Mallolas7, Manuel Crespo8,Maria J Tillez9, Carmen Quereda10, Jos. Sanz11, Carlos Barros12, Cristina Tural13,Ignacio Santos14, Federico Pulido15, Josep M Guardiola16, Rafael Rubio15, Enrique
Ortega17, Mar.a L Montes3, Juan J Jusdado18, Gabriel Gaspar19, Herminia Esteban20,Jos. M Bell.n1,2, Juan Gonzalez-Garcia3, and the GESIDA HIV/HCV Cohort StudyGroup.
Abstract
We assessed non-liver-related non-AIDS-related (NLR-NAR) events and mortality in a cohort of HIV/HCV-coinfected patients treated with interferon and ribavirin between 2000 and 2008. The censoring date was May 31, 2014. Cox regression analysis was performed to assess the adjusted hazard rate (HR) of overall death in responders and non-responders. Fine and Gray regression analysis was conducted to determine the adjusted sub-hazard rate (sHR) of NLR deaths and NLR-NAR events considering death as the competing risk.
The NLR-NAR events analyzed included diabetes mellitus, chronic renal failure, cardiovascular events, NLR-NAR cancer, bone events, and non-AIDS-related infections. The variables for adjustment were age, sex, prior AIDS, HIV-transmission category, nadir CD4+ T-cell count, antiretroviral therapy, HIV-RNA, liver fibrosis, HCV genotype, and exposure to specific anti-HIV drugs. Of the 1,625 patients included, 592 (36%) had a sustained viral response (SVR).
After a median five-year follow-up, SVR was found to be associated with a significant decrease in the hazard of diabetes mellitus (sHR 0.57 [95% CI, 0.35 - 0.93] P= .024) and decline in the hazard of chronic renal failure close to the threshold of significance (sHR 0.43 [95% CI, 0.17 - 1.09], P=.075).
Conclusion: Our data suggest that eradication of HCV in coinfected patients is associated not only with a reduction in the frequency of death, HIV progression, and liver-related events, but also with a reduced hazard of diabetes mellitus and possibly of chronic renal failure. These findings argue for the prescription of HCV therapy in coinfected patients regardless of fibrosis stage.
The patients were selected from the cohort of the "Grupo de Estudio del SIDA"(AIDS Study Group, GESIDA) of the "Sociedad Espa.ola de Enfermedades
Infecciosas y Microbiolog.a Cl.nica" (Spanish Society of Infectious Diseases andClinical Microbiology, SEIMC). This cohort was composed of patients who werenaive to anti-HCV therapy and who were treated with interferon and ribavirin
Data from the 1,625 patients who started treatment between January 2000 andJanuary 2008 were included in the database
median baseline CD4cell count was 527 cells/mm3, 69.4% had an undetectable HIV viral load, 62.4%
were infected with genotypes 1 or 4, and 60.6% had an HCV RNA ≥500,000 IU/mL
Baseline liver biopsy was performed in 1154 patients, of whom 445 (38.6%) hadbridging fibrosis or cirrhosis. At baseline, 77 (4.7%) patients reported a highintake of alcohol, 47 (2.9%) had diabetes mellitus, and 4 (0.2%) had chronic renalfailure
Treatment Response
A total of 791 (48.7%) patients were treated with pegylated interferon α2a plusribavirin, 615 (37.8%) were treated with pegylated interferon α2b plus ribavirin,and 219 (13.5%) were treated with the standard interferon α plus ribavirinregimen (three times weekly). The initial treatment response was categorized assustained viral response in 592 (36%) patients and as no response in 1033 (64%)patients. During follow-up, six (1%) of 592 responders developed HCV reinfectiona median of 49 months after discontinuing anti-HCV therapy (minimum 22months, maximum 87 months). A total of 198 patients were retreated duringfollow-up: 192 patients whose first course of anti-HCV therapy failed, and the sixpatients who experienced reinfections. A total of 42 retreated patients achievedsustained viral response, including one of the six reinfected patients. For thepurpose of the primary analysis, there were 628 responders and 997non responders.
A detailed description of incident NLR-NAR events during follow-up is shown inTable 2. By order of frequency these were cancer (n=100 [6.2%]), diabetes
mellitus (n=95 [6.0%]), cardiovascular events (n=91 [5.6%]), non-AIDS-relatedinfections (n=81 [5.0%]), bone-related events (n=57 [3.5%]), and renal events(n=33 [2.0%]).
The results of the univariate and multivariate proportional hazards regressionanalyses of factors associated with clinical outcomes are shown in Table 4. Incomparison with no response, sustained viral response was associated with astatistically significant reduced adjusted hazard of overall death (hazard ratio [HR]and 95% CI, 0.36 [0.24 - 0.54]; P<.001), liver-related death (sub-hazard ratio[sHR]; 95% CI, 0.13 [0.06 - 0.28]; P<.001), new AIDS-defining events (sHR [95%CI],0.37 [0.17 - 0.79]; P=.010), liver decompensation (sHR [95%CI], 0.10 [0.05 - 0.21];P<.001), hepatocellular carcinoma (sHR [95%CI], 0.13 [0.03 - 0.50]; P=.003), andliver transplantation (sHR [95%CI], 0.12 [0.02 - 0.78]; P=.027). As for NLR-NARevents, sustained viral response was independently associated with a statisticallysignificant reduced hazard of diabetes mellitus (sHR [95%CI], 0.57 [0.35 - 0.93];P=.024), with a reduced hazard of renal events close to the threshold ofsignificance (sHR [95%CI], 0.42 [0.17 - 1.09], P=.074), and with a higher hazard ofcardiovascular events also close to the threshold of significance (sHR [95%CI], 1.57[0.99 - 2.50]; P=.056). The results of the primary analysis were confirmed in thesensitivity analyses based on the definitions of treatment response, although in thethird subanalysis, the reduced adjusted hazard of renal events followingeradication of HCV was statistically significant (Supplementary Material. Table 4).
Discussion
We evaluated the clinical course of 1,625 HIV/HCV-coinfected patients who werefollowed up for a median of five years after the end of treatment with interferonplus ribavirin, with the primary objective of evaluating the effect of treatmentresponse on incident NLR-NAR events. We found that during follow-up, theincidence rates of diabetes mellitus, renal events, and non-AIDS-related infectionswere significantly lower in responders than in non-responders. However, nosignificant differences were found between the groups in the rates of NLR-NARcancers, cardiovascular events, and bone events. When we carried out regressionanalysis after adjusting for clinically significant covariates and considering deathas a competitive risk, we found that sustained viral response was associated with asignificant decrease in the hazard of diabetes mellitus. However, the decrease inthe hazard of renal events almost reached statistical significance. In agreementwith previous reports from this cohort, we found that treatment response wasassociated with a decreased hazard of overall and liver-related death, all types ofliver-related events, and new AIDS-related conditions (7, 21).
Our finding that treatment response in HIV/HCV-coinfected patients wasassociated with a significant decrease in the hazard of diabetes mellitus lendsfurther support to the causative role of HCV infection in insulin resistance and type2 diabetes (22) and agrees with findings from previous studies in which sustainedviral response caused a reduction in the risk of type 2 diabetes in HCV-monoinfectedpatients (11). It is also worth mentioning that insulin resistance anddiabetes are associated with progression of liver disease, hepatic decompensation,and death in patients with chronic HCV (23-26) and with hepatocellular carcinomain patients with HCV-related cirrhosis with or without HIV infection (27, 28). Forthese reasons, patients with chronic hepatitis C and insulin resistance or type 2diabetes might benefit from antiviral therapy irrespective of their stage of fibrosis(29).
HCV infection has been associated with an increased risk of end-stage renaldisease in HCV-monoinfected individuals (30, 31) and HIV/HCV-coinfectedindividuals (32, 33). HCV infection has also been found to increase the mortality ofpatients with end-stage renal disease (34). In addition, antiviral treatment for HCVhas been associated with a lower risk of end-stage renal disease in largeprospective cohorts in HCV-monoinfected individuals (12, 13). We found asignificantly higher incidence of renal events in non-responders than inresponders. However, with the stricter multivariate competing risk regressionanalyses, the lower hazard of chronic renal failure in responders than in nonresponders
did not reach the conventional threshold for significance (P=0.075).The clinical and public health repercussions of this finding are relevant becausethe risk of death, cardiovascular events, and hospitalization increasesproportionally with reductions in estimated glomerular filtration rates below 60mL per minute per 1.73 m2 (35).
In our study, NLR-NAR cancer was the most common NLR-NAR event duringfollow-up; however, the hazard of this event was not found to be modified byeradication of HCV. Despite advances in HIV therapy, cancer rates are still higheramong HIV-infected individuals than among matched non-HIV-infected individuals(36), probably owing to the high prevalence of traditional cancer risk factors,coinfection with other oncogenic viruses, and associated immunodeficiency amongthe HIV-infected individuals (37). In addition, non-AIDS-related cancer is currentlythe leading non-AIDS cause of death among people with HIV in high-incomesettings (38). For all the above reasons, evidence-based cancer screening must beconsidered an essential component in the care of HIV-infected individuals.
Intriguingly, although the crude incidence of cardiovascular events was notsignificantly different between responders and non-responders, competing riskregression analysis showed the adjusted hazard of cardiovascular events to behigher in responders than in non-responders, although once again, on the verythreshold of statistical significance (P=0.056). This finding contrasts with thoseother studies in which HCV clearance following anti-HCV therapy has been foundto reduce the risk of stroke (39, 40). The association between HCV infection and
cardiovascular events is a contentious issue. Several observational studies havefound that in the general population, HCV is an independent factor associated withcoronary artery disease (41-45), stroke (39, 46, 47), and peripheral artery disease(48). HCV infection has also been found to increase the likelihood of cardiovasculardisease among HIV-infected individuals (49, 50). However, other authors have notfound an association between HCV infection and angiographic coronary arterydisease (51, 52) or myocardial infarction (53). Meta-analyses have demonstratedan increased risk of cardiovascular events associated with HCV infection in somepatients (54, 55), but not in others (56). It is important to note that HCV infectionhas opposing effects on the pathophysiology of atherosclerosis. On the one hand,HCV induces an alteration in markers of inflammation and endothelial dysfunctionthat could potentially stimulate atherogenesis (57-59). On the other hand, HCVinfection is associated with lower total cholesterol and LDL cholesterol levels (60,61), probably owing to increased deposition of lipids in hepatocytes, where thelipids are used to promote HCV replication and secretion of lipoviroparticles. Alsonoteworthy are the different effects of eradication of HCV on atherogenesis,namely, reversion of inflammation and endothelial dysfunction (62) and reboundof LDL and total cholesterol to levels associated with increased risk of coronarydisease (60, 63). The above findings indicate that further work is needed to assessthe effects of eradication of HCV on preclinical atherosclerosis and cardiovascularevents.
Both injection drug use and liver cirrhosis can contribute to bacterial infectionsamong HCV-infected individuals. As for liver cirrhosis, the only identified factor forbacterial infections is advanced liver disease (64). In the combinationantiretroviral therapy era, HCV infection has been shown to predispose to severebacterial infections associated with hospitalization or death in HIV-infectedindividuals (65). However, we did not find a significant association betweenresponse to anti-HCV treatment and the hazard of non-AIDS-related infections.
Chronic HCV infection is associated with low bone mineral density, even in theabsence of cirrhosis (66); in coinfected patients, both HIV infection and HCVinfection have been found to reduce bone mineral density through differentpathophysiologic mechanisms (67). Furthermore, HCV has been found to increasethe risk of osteoporotic fractures among HIV-infected patients, a risk that isexplained only in part by the severity of liver disease (68). We did not find anassociation between eradication of HCV and the hazard of bone fractures; however,it has yet to be determined whether successful treatment of HCV will significantlyimprove bone mineral density in HIV/HCV-coinfected patients.
The main limitation of our study is that its design was not entirely prospective.However, we believe that its characteristics make it unlikely that the results differconsiderably from those that would have been obtained in an entirely prospectivestudy: patients were followed by the same infectious diseases physicians in thesame reference hospitals throughout the course of the disease, with standardclinical and laboratory parameters assessed at least every 6 months. In addition,the frequency of loss to follow-up was higher among non-responders than amongresponders. However, we believe that the potential bias caused by this differencewould tend to minimize the frequency and rates of events among non-respondersrather than increase them. Our study is also limited by the lack of informationabout pneumococcal vaccination, smoking, alcohol and drug use during follow-up,and cardiovascular risk factors; therefore, we cannot rule out the possibility thatdifferences in these variables could have affected outcome. The strengths of ourstudy include the high number of patients included and the long follow-up period.
We also emphasize the use of multivariate Fine and Gray regression as analternative to Cox regression for survival data in the presence of competing risksand the performance of sensitivity analyses that confirmed the findings of theprimary analysis. Finally, in our study, all the information in the database wasmonitored to verify that it was consistent with the patient's medical records.
Although the study design precludes determination of causality, our resultssuggest that eradication of HCV in coinfected patients is associated not only with areduction in overall death, liver-related death, new AIDS-related events, and alltypes of liver-related events, but also with a statistically significant reduced hazardof diabetes mellitus and a decline in the hazard of chronic renal failure very closeto the threshold of significance. These findings argue for the prescription of HCVtherapy regardless of liver fibrosis stage in coinfected patients.
|
|
| |
| |
|
|
|