| |
Treat HCV Early - Increased mortality among persons with chronic hepatitis C with moderate or severe liver disease: a cohort study
|
| |
| |
Download the PDF here
This is new published study - reported in full below following this section just below.
"Delaying treatment for anyone chronically infected with HCV regardless of fibrosis stage may be detrimental given the increased risk of mortality even for those with moderate disease and the inability to predict the transition from mild to moderate disease." - new study below following these links to previous studies with similar findings,
---------------------
from Jules: this is the latest in a series of studies over the past several years since the advent of the new DAA interferon free HCV treatments to find delaying therapy increases risk for advanced liver disease, reduced efficacy of the treatment & increased risk for HCC, liver transplant & death. Of note as I said delaying therapy also reduces the SVR rate as even treating at F0-1 increases SVR rates compared to F2. If HCV treatment is delayed that reduces chance to reverse fibrosis, HCV disease, and that IS the ultimate goal of therapy, to prevent disease progression & to reverse disease progression, and fibrosis regression cuts death risk by 64%, see link below to study. Even back in the earlier days when Peginterferon+Rbv was the only treatment, in 2001 up until Telaprevir & boceprevir the first HCV protease inhibitors became available - we knew that treating early was the best way to achieve the highest SVR rates & to prevent disease progression. Because insurers & Medicaids with federal complicity imposed harsh restrictions preventing unfettered access so anyone could be treated this forced researchers to do these types of studies to prove that early treatment is better, it is not the best way to use money & funding, it would have been better used to screen & treat patients. Another important point in treating early is the recent developments that HCV rates of new infections among young women of child-bearing age increased quite a lot, >200% in Kentucky & HCV vertical transmission increased 68% nationally - http://natap.org/2016/HCV/072616_02.htm - emphasizing the importance to screen & treat this group, for which there is very little if any funding support. And as well, there is no screening of at-risk newborns.
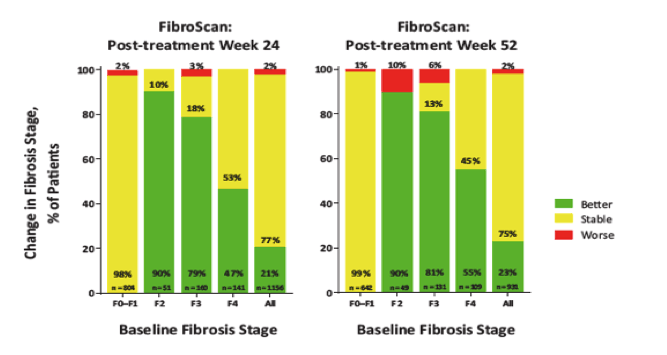
the best chance of improving fibrosis is to treat at F1 where 99% remain stable at week 52 when checked by Firbroscan, IF you wait until F2 90% improve, if you wait until F3 81% improve, if you wait until F4 55% improve. This table shows IF treated at F0-F1 99% achieve fibrosis stability BUT if you wait until F2 10% can worsen & 90% improve. Long-Term Evaluation of Liver Stiffness and Blood Markers in Hepatiti s C Virus Genotype 1-Infected Patients Receiving Ombitasvir/Paritaprevir/Ritonavir + Dasabuvir ± Ribavirin: Interim Results from TOPAZ-I and TOPAZ-II - from Jules: TREAT EARLY - (03/13/17)
Cost-effectiveness of Early Treatment of Hepatitis C Virus Genotype 1 by Stage of Liver Fibrosis in a US Treatment-Naive Population.....By treating all stages of fibrosis vs waiting to treat at stages F3 and F4, the percentage of averted cases of liver transplant, decompensated cirrhosis, hepatocellular carcinoma, and liver death are 26%, 17%, 27%, and 25%, respectively........cost of treating 50% of patients with HCV genotype 1 during the next 5 years could be as high as $29 billion, partly offset by $3 billion in savings in the management of chronic HCV and advanced liver disease......and treating earlier was more cost-effective
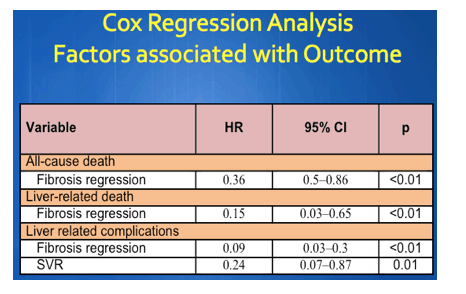
Frequent Fibrosis Regression With SVR in HCV/HIV+, Cutting Death Risk - http://www.natap.org/2015/IAS/IAS_55.htm - Patients with less advanced HCV disease were more likely to achieve SVR & of course patients with an SVR were more likely to achieve fibrosis regression: 55% of patients with SVR achieved fibrosis regression while only 15% without SVR achieved fibrosis regression, but of note 45% of patients with an SVR did not achieve fibrosis regression; delaying HCV therapy decreases chance for fibrosis regression & early HCV treatment increases chance for regression. Noteworthy study outcomes: Treat HCV EARLY, once a patient has advanced liver disease they face increased risk for disease & death because they were less likely to achieve fibrosis regression. Even patients who achieve fibrosis regression risk liver disease but in this study those rates were low but a few patients who achieved SVR & FR still died or had liver complications. The current restrictions by medicaids are supported by the federal govt because the federal govt is not doing anything to prevent the states from imposing these restrictions, so the federal govt is imposing increased death risk to patients. Of note ALL patients with cirrhosis even if they achieve SVR must have continuous followup with their doctors to look for HCC, liver cancer, even with an SVR there remains a risk for HCC forever, followup with MRI every 6 months forever is required & recommended, is the Standard of Care.
---------------------
Increased mortality among persons with chronic hepatitis C with moderate or severe liver disease: a cohort study
"Delaying treatment for anyone chronically infected with HCV regardless of fibrosis stage may be detrimental given the increased risk of mortality even for those with moderate disease and the inability to predict the transition from mild to moderate disease."
Clinical Infectious Diseases March 10 2017 - Javier A. Cepeda1 PhD, MPH; David L. Thomas2 MD, MPH; Jacquie Astemborski3, MS; Mark S. Sulkowski2, MD; Gregory D. Kirk2,3 MD, PhD; Shruti H. Mehta3 PhD, MPH
1. Division of Global Public Health, Department of Medicine, University of California, San Diego, La Jolla CA, USA
2. Division of Infectious Diseases, Johns Hopkins School of Medicine, Baltimore, MD, USA
3. Department of Epidemiology, Johns Hopkins Bloomberg School of Public Health, Baltimore, MD, USA
Summary: Individuals with mild/moderate liver disease due to chronic hepatitis C virus are often denied curative treatment. However, our data did not support that practice since, in those with mild/moderate disease, we found increased mortality and an inability to predict disease progression with sufficiently high diagnostic accuracy....."In summary, we observed increased mortality among persons with severe and moderate fibrosis and transitions to moderate fibrosis could not be predicted with high accuracy. These data support the AASLD/IDSA guidelines for treatment of all persons with chronic HCV infection and do not support withholding treatment from those with mild disease.".... "Successful treatment of HCV is associated with 80% reduction in mortality, as well as reduced incidences of liver failure and hepatocellular carcinoma [25]. This association has been demonstrated in several settings, including among individuals with moderate liver disease [26, 27] . While we were not able to evaluate the impact of SVR in our population, our data in combination with these other findings support the recommendation of the AASLD/IDSA to treat nearly all HCV infected persons immediately, a strategy also found to be cost-effective [28]......more than 80% of HCV infections in the US are due to illicit drug use and an estimated 75-80% were born between 1945-1965 "
ABSTRACT
Background:
Despite the availability of curative treatment for hepatitis C virus (HCV) infection, because of cost, treatment is often denied until liver fibrosis has progressed to at least moderate fibrosis and in some cases cirrhosis. That practice is justified on assumptions that there are no medical consequences to having moderate disease and that disease stage transitions can be anticipated.
Methods:
We performed transient elastography on 964 people chronically infected with HCV with a history of injection drug use living in Baltimore, Maryland. Liver stiffness was evaluated semiannually from 2006 to 2014 using validated cutoffs for moderate fibrosis (8.0 - 12.3 kPa) and severe fibrosis/cirrhosis (>12.3 kPa).
Results:
Among 964 persons, 62%, 23% and 15% had baseline measurements suggestive of no/mild fibrosis, moderate fibrosis and severe fibrosis/cirrhosis, respectively. All-cause and non-accidental mortality were elevated in persons with moderate fibrosis (adjusted hazard ratio [aHR]: 1.42, 95% CI: 0.96 - 2.11; aHR: 1.66, 95%CI: 1.06 - 2.59, respectively) after adjustment for sociodemographics, substance use, and HIV status. Despite the increased risk of mortality among those with moderate fibrosis, no combination of demographic, behavioral, clinical factors, nor changes in stiffness measurements themselves could predict the transition from mild to moderate fibrosis with sufficiently high diagnostic accuracy (C-statistic =0.72 for best performing model).
Conclusions:
Delaying treatment for anyone chronically infected with HCV regardless of fibrosis stage may be detrimental given the increased risk of mortality even for those with moderate disease and the inability to predict the transition from mild to moderate disease.
INTRODUCTION
Approximately 3 million people are chronically infected with hepatitis C virus (HCV) in the US [1]; however, the true burden may be underestimated by at least several hundred thousand [2]. Chronic HCV infection is a major risk factor for liver cirrhosis, liver failure, and hepatocellular carcinoma [3]. Treatment with highly efficacious, oral direct-acting antivirals (DAAs) is curative [4], however barriers to access exist. As of December 2014, out of 42 states that specified reimbursement procedures for DAAs, 31 restricted DAAs to patients with advanced fibrosis (METAVIR F3) or cirrhosis (METAVIR F4) [5], despite recommendations from the American Association for the Study of Liver Disease (AASLD) and the Infectious Diseases Society of America (IDSA) to treat nearly everyone chronically infected [6]. Treatment denials are justified by the assumption of no medical consequence to low stage HCV infection and that liver fibrosis progression can be safely monitored until advanced fibrosis/cirrhosis is detected.
Because guidelines recommend treatment for all, randomized trials to test the safety of treatment deferral for persons without advanced fibrosis/cirrhosis would be unethical. Thus, we characterize mortality rates by liver disease severity before widespread availability of DAAs in a community-based cohort of former/current people who inject drugs (PWID) in whom fibrosis was uniformly monitored with semiannual visits using transient elastography. We further examined whether liver disease progression from no/mild to moderate fibrosis could be predicted with high diagnostic accuracy. This is an aging cohort whose experience might be relevant to a large subgroup of persons in the US who acquired HCV from drug use and were born between 1945 and 1965[7, 8].
DISCUSSION
In this large sample of PWID with chronic HCV infection, we observed substantial mortality. Although increased mortality was evident among individuals with severe fibrosis/cirrhosis, we observed some increased risk of mortality even among those with moderate fibrosis. These findings, and our inability to identify with sufficiently high prognostic accuracy individuals who would transition from a lower mortality risk state (minimal liver disease) to a higher mortality risk state (moderate or severe liver disease), may not support withholding HCV treatment until that transition occurs.
Prior studies have demonstrated an association between severe fibrosis/cirrhosis and mortality [17, 18]. Indeed, surveillance data released by the CDC indicate that in 2014, HCV infection killed an estimated 20,000 persons in the US [19]. Much of the mortality is due to liver failure and hepatocellular carcinoma. But, as we observed, persons with HCV infection also have increased mortality that may be unrelated to HCV-induced liver disease and may be the result of a negative effect of HCV on other organ systems. Indeed, excess mortality due to circulatory and renal diseases was reported in a cohort of people chronically infected with HCV [20]. Here we report a higher rate of mortality in persons with moderate liver disease, compared to no/mild fibrosis which may be attributed to chronic inflammation resulting from chronic HCV infection and comorbidities [7]. Further, the increased mortality among those with moderate fibrosis at baseline may in part be due to progression to cirrhosis in this group. Although there were too few deaths to evaluate this hypothesis, higher mortality was observed for those who progressed from no/mild fibrosis to moderate fibrosis (8% of whom then progressed to cirrhosis) versus those who remained in the no/mild fibrosis state during the follow-up period (1.33 deaths per 100 PY vs. 1.06 deaths per 100 PY).
While the overall association between baseline moderate fibrosis and mortality attenuated slightly after including BMI, diabetes and hypertension in the model for non-accidental deaths, it is possible that these comorbidities, particularly diabetes are causally associated with fibrosis and mortality [21]. Much of the mortality observed was not liver-related which reflects both the nature of the population (all had a history of drug use) and the challenges in ascertaining cause of death from death certificates.
Consistent with previous studies, we found that high HIV RNA level was associated with an increased risk of progression from no/low to moderate fibrosis [8, 22, 23]. High HIV RNA level is a surrogate for untreated HIV infection, and use of antiretroviral therapy has been associated with attenuated liver fibrosis progression in HIV infected persons [8, 24]. However, while this association was statistically significant, high HIV RNA level did not discriminate among persons who did and did not progress with sufficiently high accuracy. Moreover, no other demographic, behavioral or clinical factor, nor changes in LSM themselves had high predictive accuracy for fibrosis progression.
Successful treatment of HCV is associated with 80% reduction in mortality, as well as reduced incidences of liver failure and hepatocellular carcinoma [25]. This association has been demonstrated in several settings, including among individuals with moderate liver disease [26, 27] . While we were not able to evaluate the impact of SVR in our population, our data in combination with these other findings support the recommendation of the AASLD/IDSA to treat nearly all HCV infected persons immediately, a strategy also found to be cost-effective [28].
Withholding medical treatment based on disease stage implies that there is a 'safe' disease stage. Additionally, it is assumed that the 'safe' stage and transitions out of that stage can be accurately detected. Whether detected by liver biopsy, LSM, or blood markers, liver fibrosis estimates cannot differentiate mild from moderate fibrosis with sensitivity >80% [29, 30]. Likewise, progression of liver fibrosis was not predicted with sufficiently high diagnostic accuracy in most other studies [22, 31]. These scientific and clinical realities should be carefully considered when formulating evidence-based approaches to delivering HCV treatment.
Limitations
The experience of the ALIVE cohort may differ from persons with chronic HCV in other settings, including those outside of the U.S. For example, this cohort had a higher prevalence of HIV and HCV than national CDC estimates [32] and findings from the National Health and Nutrition Examination Survey [2]. Additionally, more persons in this setting continued to use illicit drugs than in many primary care or specialty clinical practices. Nonetheless, more than 80% of HCV infections in the US are due to illicit drug use and an estimated 75-80% were born between 1945-1965, similar to ALIVE cohort members. Moreover, while there was high competing mortality, other unrelated causes of death should reduce our ability to detect an association based on liver disease stage rather than create a false finding. Indeed, elimination of accidental deaths strengthened the estimated mortality association. While we used death certificate data to determine cause of death, these data are often not comprehensive. For example, we considered deaths due to "chronic drug use" to be accidental because physicians may have ascribed this cause of death when they could not determine a precise natural cause of death. However it is possible that deaths due to chronic drug use may have been due to underlying liver disease, which has been shown to be underestimated in death certificates [33]. Some members of the ALIVE cohort have received successful HCV treatment and would have been excluded by having undetectable HCV RNA. However, the course of person-time evaluated was prior to the availability of all-oral medications in 2015. During that interval, fewer than 5% were cured by treatment [34]. This analysis was based chiefly on elastography. However, we observed high concordance between our LSM values and blood tests like FIB-4. Since these tests are often used in clinical practice, these data would still be germane to the subset of Medicaid supported patients currently denied HCV treatment in many states that require a minimum stage of F3 or F4 to obtain approval for treatment [5].
In summary, we observed increased mortality among persons with severe and moderate fibrosis and transitions to moderate fibrosis could not be predicted with high accuracy. These data support the AASLD/IDSA guidelines for treatment of all persons with chronic HCV infection and do not support withholding treatment from those with mild disease.
METHODS
Study population
Data came from participants enrolled in the ALIVE (AIDS Linked to the IntraVenous Experience) study, a prospective community-recruited cohort of former and current PWID residing in Baltimore, Maryland [9]. Enrollment began in 1988, with additional recruitment from 1994 - 1995, 1998, 2000, and 2005 - 2008. Participants visited the clinic biannually, were interviewed, and provided biospecimens. All participants were >18 years old and had a history of injecting drugs. We limited this analysis to those with detectable HCV RNA who had at least one liver stiffness measurement (LSM). During the time period of the mortality analysis (until 2012) , a negligible proportion of the cohort (<5%) reported receiving curative HCV treatment. The Johns Hopkins University IRB approved the study and all participants provided informed written consent.
Measurements
Liver stiffness measurements
Determination of liver fibrosis and cirrhosis was based on semiannual LSM by transient elastography using a FibroScan machine (Echosens, Paris, France), from 2006 until 2014. Briefly, a transducer on the end of an ultrasound probe emits a shear wave and instantaneously records its velocity in kiloPascals (kPa) as it passes through the liver. Trained personnel operated the machine in a research clinic. Valid examinations consisted of ≥8 valid measurements with a success rate of ≥60% (number of valid divided by total measurements) and limited variability (IQR divided by the median <0.30)[8, 10]. We used the median from each valid examination. No/mild fibrosis, moderate fibrosis, and severe fibrosis/cirrhosis were defined by an LSM of <8.0 (METAVIR F0-F1), 8.0-12.3 (METAVIR F2-F3), >12.3 kPa (METAVIR F4), respectively, according to validated cutoffs[10, 11].
Risk behaviors and serological testing
Data on risk behaviors were collected at baseline and at 6-month follow-up visits. Comorbidities were assessed by either self-report of physician diagnosis or evidence of hypertension defined by a systolic blood pressure >150 mmHg and diastolic blood pressure>90 mmHg; or diabetes if hemoglobin A1C level >6.5% [12]. The Alcohol Use Disorder Identification Test (AUDIT) was used to assess hazardous drinking/dependence [13].
Routine HIV serologic testing was conducted for participants not known to have HIV. Antibodies to HCV and hepatitis B virus surface antigen (HBsAg) were obtained at the first available visit. The Abbott RealTime HCV assay (Abbott Molecular, Des Plaines, Illinois) assessed HCV RNA level at the visit approximately when the first LSM was performed. Platelet count, alanine aminotransferase, and aspartate aminotransferase were collected and used to calculate FIB-4 [14] within one year of the baseline LSM.
Statistical analyses
Mortality
All anti-HCV positive persons with detectable HCV RNA and at least one LSM were included (n=964). Baseline for this analysis was the date of the first valid LSM. Mortality data, including data on cause, were obtained from the National Death Index (NDI) with confirmation from death certificates. Kaplan-Meier curves and Cox proportional hazards regression were used to compare mortality by baseline LSM. Persons were censored at their date of death or December 2012 (through which NDI data were complete). Selection of potential confounding variables included in multivariable regression models was based on previous mortality analyses in this cohort [12]. Two outcomes were considered: 1) all-cause mortality 2) non-accidental mortality where deaths due to trauma, chronic drug and alcohol use were censored as non-events. For both outcomes, we created four models. Model 1: sociodemographics; Model 2: sociodemographics and substance use; Model 3: sociodemographics, substance use, and HIV infection; Model 4: sociodemographics, substance use, HIV infection, and comorbidities (diabetes, hypertension). We assessed for violation of the proportional hazards assumption by examining interactions between covariates and time (none detected).
Predictors of disease progression
To characterize liver disease progression and identify whether disease progression could be predicted by risk factors or visit-to-visit changes in LSM, we restricted analyses to those with no/mild fibrosis, (e.g., LSM <8.0 kPa at first two visits [n=331]), and thus not eligible for treatment in most settings. We used Cox regression to characterize associations between previously defined risk factors for progression [8]. An event was defined as > two LSM consistent with moderate fibrosis (≥8.0 kPa) [10]. Individuals who never had two LSM ≥8.0 kPa during follow-up were censored. Model building was conducted using the same framework as the mortality analysis, however behavioral factors and BMI were included as time-varying. We included visit-to-visit rates of change in LSM (Δ) using three designations to represent typical times between clinical evaluations: T0: first LSM ≥ 8.0 kPa (event); T-1 : one visit (approximately 6 months) prior to first LSM ≥8.0, T-2: two visits (approximately 12 months) prior to first LSM ≥8.0, T-3: three visits (approximately 18 months) prior to first LSM ≥8.0 (Figure 1) and all combinations in changes between visits (ΔT-1, T-2; ΔT-2, T-3; ΔT-1, T-3). Change was calculated as the difference in the two LSM divided by the time between measurements. Thus, the analysis of visit-to-visit changes, was limited to individuals with at least four LSM (N=331, 2,719 LSM). Three separate models were run for each distinct visit-to-visit change to assess whether an individual visit pair was associated with future fibrosis progression. All models were adjusted for the LSM value T-3 (starting value). Most visits were between 6 - 12 months apart (median: 6.2, IQR: 6.0 - 11.9 months) and the median change in LSM between visits was 0 kPa (IQR: -1.0 - 1.0 kPa). No significant difference in visit-to-visit LSM change was detected between visits that occurred every 6-12 months and visits that occurred more than 12 months apart (p=0.41). Given potential differences on fibrosis progression due to HIV infection, we conducted sensitivity analyses stratifying by HIV status (supplementary material).
Harrell's C statistic was calculated to assess the models' ability to discriminate between those with and without evidence of disease progression, while allowing for inclusion of time-varying covariates and censored data [15, 16]. Methods described by Chambless et al. were used to calculate sensitivity and specificity of predicting progression to moderate fibrosis for the predictive risk scores at 5 years including a bootstrap to calculate confidence intervals. All statistical analyses were conducted using SAS v.9.4 (SAS Institute, Cary, North Carolina).
RESULTS
At baseline the median age was 49 years (IQR:44 - 53), 72% were male, and 87% African American (Table 1). Half (52%) were actively injecting and 14% had an AUDIT score indicating alcohol dependence. The median duration of drug injection was 27.5 years (IQR:20 - 35). Thirty-five percent were HIV co-infected, 52% of whom were not on antiretroviral therapy. Nearly two-thirds (n=604, 63%) had no or mild/fibrosis, 218 (23%) had moderate fibrosis, and 142 (15%) had severe fibrosis/cirrhosis and 4, 14, and 21% of those no/mild, moderate, and severe fibrosis had diabetes, respectively.
Mortality
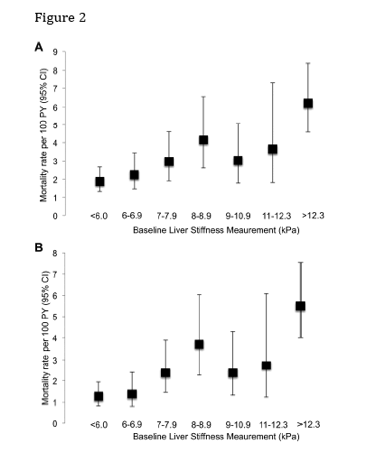
Over a median 5.9 years (IQR: 4.3-6.5) after the first LSM, 155 deaths were observed (mortality rate: 3.06 deaths per 100PY). All-cause mortality was highest among participants whose first LSM was consistent with severe fibrosis/cirrhosis (6.21 deaths/100PY). Mortality was also significantly elevated among participants whose first LSM was consistent with moderate fibrosis (3.59 deaths/100PY) compared to those whose first LSM was <8.0 kPa (2.21 deaths/100PY, p =0.014). When LSM were grouped into smaller intervals, similar trends in increasing mortality risk were observed (p-value for trend: <0.001) (Figure 2).
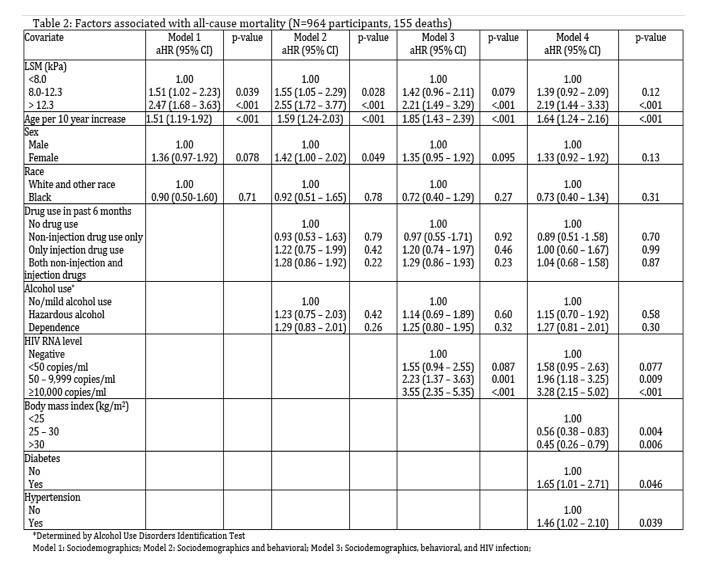
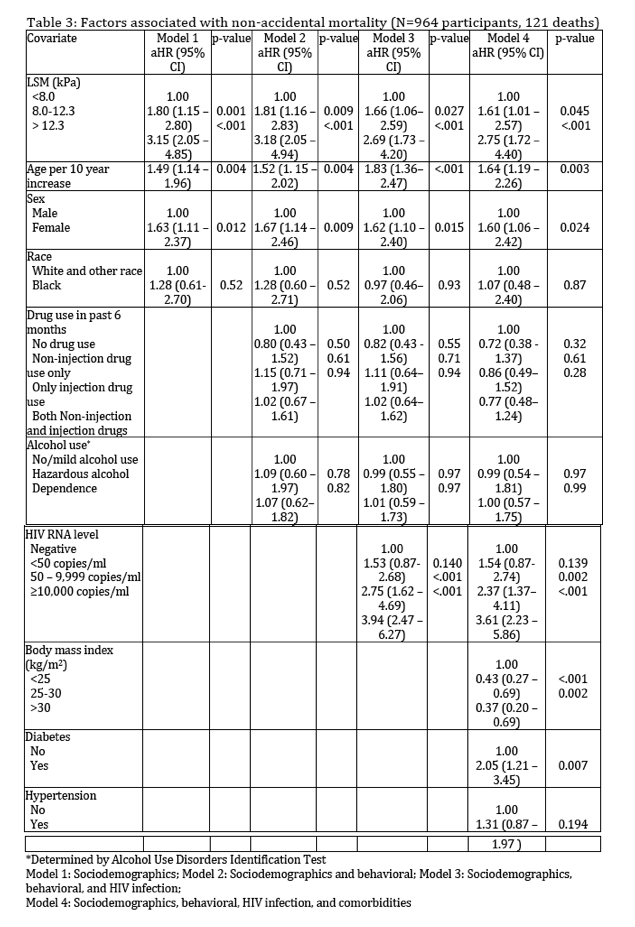
In multivariable models adjusting for only sociodemographics (Model 1) and substance use, (Model 2) mortality risk remained significantly elevated among individuals with moderate fibrosis and severe fibrosis/cirrhosis. After adjusting for HIV viral load, BMI, diabetes, and hypertension comorbidities, mortality risk remained significantly elevated among those with severe fibrosis/cirrhosis (aHR: 2.19, 95% CI: 1.44 - 3.33), however the association with moderate fibrosis was attenuated and did not retain statistical significance (Model 4), (aHR: 1.39, 95% CI: 0.92 - 2.09). Compared to all-cause mortality, the adjusted measure of association between fibrosis/cirrhosis and non-accidental mortality was stronger among those with severe fibrosis/cirrhosis (aHR: 2.75, 95% CI: 1.72 - 4.40) and moderate fibrosis (aHR: 1.61, 95% CI: 1.01- 2.57) after adjusting for sociodemographic, behavioral, and comorbid factors (Model 4). Similar trends were observed when using an alternative, validated method to ascertain liver fibrosis severity.
Compared to individuals with FIB-4 <1.45, those with FIB-4 >3.25 and between 1.45 and 3.25 had a 4.44 fold (95% CI: 2.52-7.82, p<0.0001) and 1.51 fold increased risk of mortality (95% CI: 0.89-2.56, p=0.124), respectively in an unadjusted model.
Progression to moderate fibrosis
Since mortality was elevated even in persons with moderate fibrosis, we evaluated whether this transition could be predicted with sufficiently high diagnostic accuracy to justify the practice of some insurers who deny treatment to this group. We studied 2,719 LSM over a median 5.7 years (IQR:3-7) per person. Of 331 individuals with no/mild fibrosis at baseline, 63 (19%) had evidence of significant progression measured by > two subsequent LSM ≥8.0 kPa (incidence rate: 3.55 per 100 PY). In univariable analysis, high HIV RNA (≥10,000 copies/ml), and higher initial LSM at T-3 were associated with an increased risk of progressing to ≥8.0 kPa (HR: 2.31 (95% CI: 1.32- 4.05) and HR: 1.30 per kPA (95% CI: 1.10-1.55), respectively). In multivariable analysis (Table 4) which did not include the visit-to-visit changes (Model 1), high HIV RNA level (≥10,000 copies/ml) (aHR: 2.75, 95% CI: 1.28-5.92, p=0.001), and being overweight (aHR vs. normal BMI: 1.88, 95% CI: 1.09 - 3.26) were significantly associated with an increased risk of progression, but had low predictive accuracy (C statistic=0.66 [95% CI: 0.60 - 0.73]). The sensitivity for predicting transition from no/mild to moderate fibrosis at 5 years among those whose risk score was in the top quintile was 32% and the specificity was 83%.
In models that included combinations of LSM visit-to-visit changes, only a one-year change in LSM was significantly associated with progression. For every one kPa increase in the one-year change in LSM, the risk of progressing to moderate fibrosis increased over 40-fold (aHR: 41.3; 95%CI: 3.15-542.3), after adjusting for sociodemographics, substance use behaviors, BMI, and LSM at T-3. However, this change had only fair predictive accuracy (C-statistic: 0.72 (95%CI: 0.66-0.78)). Associations with six-month changes were not significantly associated with progression regardless of whether the six-month change occurred one visit (ΔT-1, T-2: aHR: 1.32 [95% CI: 0.42 - 4.12]) or two visits (ΔT-2, T-3: aHR: 2.87 [95% CI: 0.84-9.75)) prior to the progression event. The C-statistics for the six-month changes were similarly in the fair prognostic accuracy range (ΔT-1, T-2 C-statistic: 0.70, 95% CI: 0.64-0.76, ΔT-2, T-3 C-statistic: 0.71, 95% CI: 0.65-0.76).
|
|
| |
| |
|
|
|