| |
Safety and efficacy of ledipasvir/sofosbuvir for the treatment of
genotype 1 hepatitis C in subjects aged 65 years or older
|
| |
| |
Download the PDF here
Hepatology 2016 - Sammy Saab,1 Sarah H. Park,1 Masashi Mizokami,2 Masao Omata,3 Alessandra Mangia,4 Ed Eggleton,5 Yanni Zhu,5 Steven J. Knox,5 Phil Pang,5 Mani Subramanian,5 Kris Kowdley,6 and Nezam H. Afdhal7
Safety and Efficacy of Ledipasvir/Sofosbuvir for the Treatment of Genotype 1 Hepatitis C in Patients Aged 65 Years or Older: A Retrospective Analysis of International Phase 3 Studies - (05/28/15)
Abstract
Elderly subjects have been historically underrepresented in clinical trials involving antiviral hepatitis C therapies. The aim of this analysis was to retrospectively evaluate the safety and efficacy of ledipasvir/sofosbuvir (LDV/SOF) by age groups of <65 years versus ≥65 years among subjects enrolled in phase 3 trials. Four open-label phase 3 clinical trials evaluated the safety and efficacy of LDV/SOF with or without ribavirin (RBV) for the treatment of genotype 1 chronic hepatitis C virus. Sustained virological response at 12 weeks, treatment-emergent adverse events (AEs), and graded laboratory abnormalities were analyzed according to age group. Of the 2293 subjects enrolled in four phase 3 trials, 264 (12%) were ≥65 years of age, of whom 24 were aged ≥75 years. Sustained virological response at 12 weeks was achieved by 97% (1965/2029) of subjects aged <65 years and 98% (258/264) of subjects aged ≥65 years. The most common AEs in both LDV/SOF groups that occurred in ≥10% of subjects were headache and fatigue. The rate of study discontinuation due to AEs was similar in the two age cohorts. The use of RBV in 1042 (45%) subjects increased the number of AEs, treatment-related AEs, and AEs leading to study drug modification/interruption, particularly among elderly subjects. Conclusions: LDV/SOF with or without RBV was highly effective for treatment of genotype 1 chronic hepatitis C virusin subjects aged 65 and older. Addition of RBV did not increase sustained virological response at 12 weeks rates but led to higher rates of AEs, especially in elderly subjects.
Chronic hepatitis C viral (HCV) infection is an important cause of morbidity and mortality in infected individuals worldwide.[1] The World Health Organization estimates that the worldwide prevalence of HCV infection is 2.2%, representing 123 million people.[2] Globally, HCV accounts for 27% of liver cirrhosis and 25% of hepatocellular carcinoma cases.[3] Although the rate of HCV is decreasing overall due to attrition from mortality,[4, 5] the rate of HCV-related cirrhosis is anticipated to increase by nearly two-fold between 2000 and 2030, from 472,000 to more than 879,000 based on estimates from US population data.[6] At present, the estimated prevalence of HCV in the United States and Western Europe is 0.2%-0.5% and that in Japan is 1%-3%.[7, 8]
The elderly population is disproportionately affected by HCV. Approximately 70% of all patients with hepatitis C in the United States and western Europe were born between the years 1945 and 1965.[9] In the United States, it is estimated that between 20% and 25% of patients with HCV have cirrhosis. Patients with HCV-associated liver disease make up approximately 40% of liver transplantation candidates, with a median age of 51 years at the time of registration.[10, 11] In Europe and Japan, HCV is identified as one of the most common causes of chronic liver disease, and its prevalence in the population aged 61-70 years has been up to 12%.[12-15] Antiviral therapy with interferon-based therapy has been demonstrated to improve patient survival and reduce the likelihood of liver-related complications.[16-18] Historically, age has been a major limitation of antiviral treatment with interferon-based therapy because of its poor tolerability, adverse effects (AEs), and poorer response in older patients.[19-25] There is a lack of efficacy and safety information on HCV therapy in older patients, primarily due to underreporting and the exclusion of elderly subjects from clinical trials.[26, 27]
The combination of ledipasvir, an NS5A inhibitor, and sofosbuvir, a nucleotide polymerase inhibitor, has been approved by the US Food and Drug Administration, the European Medicines Agency, and in Japan as a fixed-dose combination tablet for the treatment of HCV genotype 1.[28] Ledipasvir/sofosbuvir (LDV/SOF) has been found to be effective against a variety of HCV clinical scenarios including special populations such as those with compensated and decompensated cirrhosis, HCV/human immunodeficiency virus coinfection, and immunosuppressed liver transplant recipients who historically have lower sustained virological response than the general population.[29-32]
Given the aging population of patients with HCV and the increased efficacy of LDV/SOF over prior antiviral therapeutic regimens, we compared the efficacy, safety, and tolerability of this combination between subjects below and above 65 years of age.
Discussion
The cohort of patients with HCV is aging globally, and the elderly tend to have more advanced liver disease. Historically, elderly patients have been excluded from clinical studies because of the toxicities associated with interferon-based therapies, and advanced age was a predictor of nonresponse for interferon-based therapy.[23] The treatment of elderly patients has thus represented a major unmet need in the management of liver disease.
LDV/SOF is an approved, interferon-free, single-tablet, once-daily regimen that has demonstrated high efficacy in genotype 1–infected subjects, with an improved safety profile and shorter treatment duration than interferon-based regimens. This retrospective analysis of pooled data from four phase 3 clinical studies (ION-1, ION-2, ION-3, and GS-US-337-0113)32-35 evaluating LDV/SOF with or without RBV for 8, 12, and 24 weeks helps to demonstrate the efficacy and safety of this regimen in elderly subjects. In all four phase 3 studies, no upper limit to age was applied, and as a result 264 subjects ≥65 years of age were enrolled and evaluated, with the oldest subject being 80 years of age.
There are several important findings in our study. First, the results of our analysis demonstrate that age is not a barrier to achieving SVR12. Overall, 97% and 98% of subjects <65 and ≥65 years of age, respectively, achieved SVR12. It was not possible to identify predictors of response due to the high SVR in both groups. Of the six elderly subjects there was no common factor associated with treatment failure. For instance, only three of the six subjects who did not have a durable response to therapy had baseline NS5A RAVs. Another important finding is that subjects ≥65 years of age were more likely to have cirrhosis. This is consistent with previous observations demonstrating greater severity of liver disease with advancing age.[27] Additional analysis stratified by the presence or absence of cirrhosis and treatment experience yielded similar findings; treatment with LDV/SOF was highly effective even in the setting of cirrhosis. In addition, subjects ≥65 years of age had lower mean eGFR, which may increase the risk of anemia with RBV. Indeed, RBV was associated with an increase in anemia in all subjects and an increase in study drug modification in the elderly cohort ≥65 years of age. This is consistent with previous findings in the elderly Japanese population who had higher rates of AEs (68% versus 76%).[35] Moreover, the risk of anemia appeared to be greater among elder subjects without cirrhosis compared to those with cirrhosis. The similar differences in anemia rates in patients with cirrhosis could be explained by greater likelihood of RBV modification in the elderly with cirrhosis.
Recently, the Food and Drug Administration approved a 12-week course of LDF/SOF and RBV in addition to 24 weeks of LDF/SOF as an option in patients who are treatment-experienced and have cirrhosis.[36] Given the possibility of anemia and RBV dose reduction in the elderly, consideration should be made for the 24-week treatment course in the elderly. Thus, RBV-free regimens should be considered for the treatment of elderly patients, and elderly patients treated with RBV should be closely monitored for the development of anemia, particularly when reduced renal function is present.
The results of recent studies highlight the benefits of treating HCV beyond achieving SVR. Subjects who achieve SVR demonstrate improved quality of life, patient-related outcomes, and work productivity with LDV/SOF,[37] irrespective of the severity of liver disease. Younossi et al. demonstrated that subjects over 65 years of age also realized a significant benefit in patient-related outcomes after achieving SVR.[38] However, there was a decrement during therapy if interferon and RBV were used. In addition to potential improvement in survival with SVR, elderly patients may achieve improved quality of life and patient-related outcomes.
There are several limitations to our exploratory analysis. First, the study was retrospective and not designed to assess the impact of LDV/SOF among the elderly.
Nevertheless, this evaluation represents the largest experience of antiviral therapy among the elderly. The results were consistent across the different analyses. Another limitation is that our definition of "elderly" is quite broad. Although we defined "elderly" at a threshold of 65 years of age, our results may not be completely generalizable to the very elderly. Nonetheless, the cohort of subjects over 75 years of age demonstrated that the safety and efficacy of LDV/SOF are not limited by advanced age. Another limitation is the differential distribution of genotypes 1a and 1b between non-Asian and Asian elderly subjects. Genotype 1b has been associated with greater likelihood of achieving SVR12 than genotype 1a, and a greater percentage of 1b patients and Asians was found in our elderly cohort. Nevertheless, the SVR12 was similar between non-Asian and Asian genotype 1b elderly subjects (97.6% [95% CI 95.1%-100%] versus 99.1% [95% CI 91.5%-99.7%]).
There are limited data on the association of the frequency of baseline RS5A RAVS as it pertains to patient age. One might anticipate that as patients age, the likelihood of harboring baseline RS5A RAVS would increase. However, we found that similar percentages of nonelderly and elderly subjects have baseline RS5A RAVS (17% versus 20%, respectively).
Whereas in the past age may have been a negative predictor of SVR and associated with increased AEs, the results of this study suggest that LDV/SOF is an effective, tolerable, and safe treatment option for elderly patients with chronic HCV. Elderly patients should not be denied therapy based on an expected lower SVR rate.
Patients and Methods
Patients
Efficacy and safety data were pooled from four randomized, open-label phase 3 clinical trials (ION-1, ION-2, ION-3, and GS-US-337-0113) evaluating LDV/SOF (90 mg/400 mg) in genotype 1 HCV-infected subjects in the United States, Europe, and Japan. Eligible subjects were at least 18 years old with chronic genotype 1 HCV infection and a baseline HCV RNA ≥104 IU/mL at screening. Both treatment-naive and treatment-experienced subjects with or without cirrhosis were enrolled and included in this pooled analysis. Details concerning the eligibility criteria for these studies are included in the supporting appendix of the respective studies. Subjects were classified as having cirrhosis if liver biopsy showed cirrhosis (METAVIR score 4 or Ishak score ≥5), if FibroScan indicated cirrhosis (value >12.5 kPa), or if laboratory biomarkers indicated cirrhosis (FibroTest score >0.75 and aspartate aminotransferase to platelet ratio index >2). Deep sequencing of the NS5A and NS5B regions was conducted at baseline and at the time of failure for all subjects who had virological failure.
The ION-1 study (United States and European Union) enrolled 865 treatment-naive subjects, and 16% of subjects had cirrhosis at the time of the study.[32] The ION-2 study (United States) enrolled 440 treatment-experienced subjects, 20% of whom had cirrhosis at the time of the study.[33] The ION-3 study (United States) enrolled 647 treatment-naive subjects without cirrhosis.[34]
Study GS-US-337-0113, conducted in Japan, enrolled 341 treatment-naive and treatment-experienced subjects, and 22% of them had cirrhosis.[35] All four studies administered LDV/SOF (90 mg/400 mg) fixed-dose combination tablet orally, once daily with or without weight-based ribavirin (RBV; two divided doses) for 8, 12, or 24 weeks.
Pooled data from each study were analyzed in subjects age ≥65 grouped as LDV/SOF with and without ribavirin, receiving 8, 12, or 24 weeks of treatment. A subgroup analysis was done for subjects aged ≥75 years old.
Statistical Analysis
The efficacy and safety analyses included all enrolled and treated subjects. In this combined efficacy analysis, pooled data were analyzed for the total subject population by age at baseline (<65 or ≥65 years). HCV RNA was analyzed by COBAS TaqMan HCV Test v2.0 HPS, with a lower limit of quantification of 25 IU/mL. The point estimate and the two-sided 95% exact confidence interval (CI) based on the Clopper-Pearson method were calculated for the sustained virological response 12 weeks after treatment completion (SVR12) rate for each age group. In the safety analysis, the number and the percent of subjects experiencing AEs or laboratory abnormalities were summarized descriptively. For each age group, the Mantel-Haenszel method was used to calculate the two-sided 95% CI of the overall risk difference of experiencing an AE between LDV/SOF+RBV and LDV/SOF adjusted for treatment duration (8, 12, and 24 weeks). All AEs were coded using the Medical Dictionary for Regulatory Activities, Version 17.0 ( http://www.meddra.org/how-to-use/support-documentation). A diagnosis of anemia was made if the hemoglobin was ≤10 g/dL.
Results
Baseline Characteristics
A total of 2293 subjects were enrolled across all four studies, of whom 2029 (88%) were <65 years old and 264 (12%) were ≥65 years old (Table 1). The cohort of subjects ≥65 years of age had a mean age of 68 years (range 65-80 years), and 24 subjects (1%) were aged 75 years or older, 49% (n = 130) of subjects were male, 11% (n = 30) were black, 45% (n = 119) were white, and 43% (n = 113) were Asian. In the <65-year-old cohort, the mean age was 52 (range 18-64 years), 59% (n = 1187) of the subjects were male, 14% (n = 278) were black, 73% (n = 1481) were white, and 12% (n = 250) were Asian.
In the 264 subjects with age ≥65, 194 (73%) had genotype 1b and a mean estimated glomerular filtration rate (eGFR) of 77 mL/min. Among the 2029 subjects with age <65, 633 (31%) had genotype 1b and the mean eGFR was 107 mL/min at baseline. The elderly also had a higher rate of compensated cirrhosis (20% versus 12%).
Efficacy
Overall Outcomes
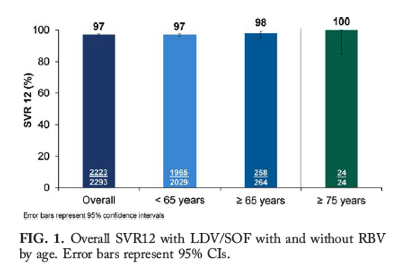
The overall SVR12 in subjects treated with LDV/SOF with or without RBV was 97% (95% CI 96%-98%) (Fig. 1). The SVR12 was 97% (95% CI 96%-98%) and 98% (95% CI 95%-99%) in subjects <65 years and ≥65 years, respectively. The 24 subjects who were aged ≥75 years had 100% SVR12 (95% CI 86%-100%). The SVR12 among non-Asian and Asian elderly subjects was 96.6% (96.6% CI 92.3%-98.9%) and 99.1% (95% CI 95.2%-100%), respectively. The SVR12 of the 111/112 Asian elderly subjects infected with genotype 1b was 99.1% (95% CI 95.1%-100%). The SVR12 in non-Asian genotype 1a and 1b subjects was 95.5% (95% CI 87.3%-99.1%) and 97.6% (95% CI 91.5%-99.7%), respectively.
Of the elderly subjects who experienced virological failure or had no confirmed virological outcome, three were genotype 1a and three were genotype 1b (Table 2). One of the subjects (genotype 1b) expired. Baseline NS5A resistance-associated variants (RAVs) were found in three subjects (Table 2). The percentages of nonelderly and elderly subjects having baseline RS5A RAVS were 17% and 20%, respectively.
Treatment-Naive Subjects
The SVR12 in treatment-naive subjects was 97% for those <65 years of age (1454/1506) and 97% (167/172) for those ≥65 years of age (see Supporting Fig. S1). Among treatment-naive subjects without cirrhosis and an HCV RNA <6 million IU/mL treated for 8 weeks with LDV/SOF, 96% (105/109) of those <65 years of age and 100% (14/14) of those ≥65 years of age achieved SVR12.
Treatment-Experienced Subjects
Treatment-experienced subjects <65 years old achieved an overall SVR12 of 98% (511/523), while the SVR in subjects ≥65 years old was 99% (91/92) (see Supporting Fig. S2). In treatment-experienced subjects ≥65 years old, SVR12 was achieved in 100% (45/45) of subjects who received LDV/SOF for 12 weeks, 97% (30/31) with LDV/SOF+RBV for 12 weeks, 100% (9/9) with LDV/SOF for 24 weeks, and 100% (7/7) with LDV/SOF+RBV for 24 weeks.
Impact of Cirrhosis
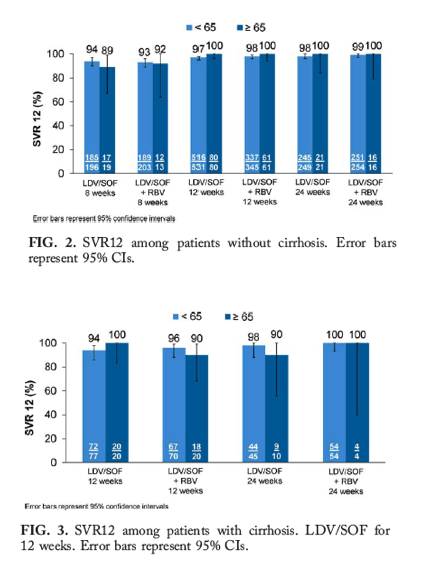
The SVR12 was 97% (1723/1778) in subjects <65 years of age without cirrhosis and 99% (207/210) in subjects ≥65 years of age (Fig. 2). Twelve weeks of LDV/SOF was an effective treatment regimen for subjects with cirrhosis. Overall, the SVR12 was 96% (237/246) in subjects with cirrhosis who were <65 years old and 94% (51/54) in subjects ≥65 years of age (Fig. 3).
Safety
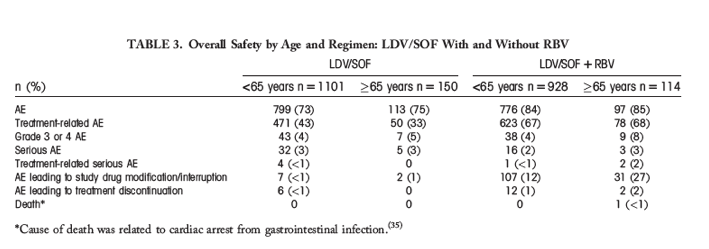
A total of 78% and 80% of subjects <65 years of age and ≥65 years of age, respectively, experienced at least one AE during the study (Table 3), with 54% of subjects <65 years of age and 48% of subjects ≥65 years of age experiencing a treatment-related AE. Serious AEs were reported in 2.4% of subjects <65 years and 3% of subjects ≥65 years of age.
The most common AEs were fatigue and headache in both age groups, with and without RBV (see Supporting Table S1). Of subjects ≥65 years of age being treated with LDV/SOF, AEs seen in ≥10% were fatigue (14%) and headache (10%). With the addition of RBV the rate of most AEs increased; 25% experienced fatigue, 13% pruritus, 11% headache, 11% nausea, 10% insomnia, and 11% rash.
The rate of study drug modification or interruption due to AEs was 6% for those <65 and 13% for those ≥65 years of age. The rate of drug discontinuation due to AE was 1% and 1% in subjects <65 years of age and ≥65 years of age, respectively (Table 3). There was one death from cardiac arrest in a subject ≥65 years old with a number of comorbidities that included pulmonary fibrosis, sarcoidosis, cirrhosis, diabetes mellitus, and splenectomy who was treated with LDV/SOF+RBV. The cause of death was related to cardiac arrest from gastrointestinal infection.[35]
RBV use increased the number of AEs reported, treatment-related AEs, and AEs leading to study drug modification/interruption for subjects ≥65 years of age (Table 3). The addition of RBV increased the number of elderly subjects who experienced at least one AE from 75% to 85%. In addition, the treatment-related AEs increased from 33% to 68%, AEs leading to study drug modification or interruptions increased from 1.3% to 27%, and drug discontinuation due to AE increased from 0% to 2%. The rate of serious AEs was the same with or without RBV at 3%. The treatment-related AE risk difference between regimens with and without RBV in the older group was 35% (95% CI 24%-47%), adjusted for treatment duration (8, 12, and 24 weeks). The corresponding risk difference in the younger group was 24% (95% CI 19%-28%).
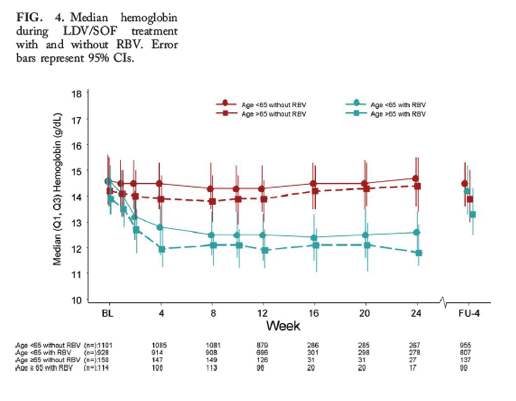
The addition of RBV increased hemoglobin abnormalities in subjects ≥65 years of age from 4.0% to 64.0%. The two-sided 95% CI was 51%-69%, which is based on the Mantel-Haenszel method adjusted for treatment duration (8, 12, and 24 weeks) (Fig. 4). Anemia rates were similar between elderly and nonelderly subjects with cirrhosis who received RBV (12.5% and 10.5%) but higher in elderly subjects without cirrhosis (15.6% and 4.8%).
|
|
| |
| |
|
|
|