 |
 |
 |
| |
2 ART Interruption Cure Studies at IAS 2017
|
| |
| |
1st study reports viral rebound in semen after interruption. 2nd study below: many participants in the placebo arm had detectable viremia at week 2 after ART was stopped. In the VRC01 arm, there appears to be a modest delay in the time to viral rebound…...Viral rebound was associated with a small but statistically significant increase in total HIV DNA in the placebo group but not the VRC01 group.
2nd study: "HIV-Specific Broadly-Neutralizing Monoclonal Antibody, VRC01, Minimally Impacts Time to Viral Rebound Following Treatment Interruption in Virologically-Suppressed, HIV-Infected Participants who Initiated Antiretroviral Therapy during Acute HIV Infection"
--------------------------------
ART Interruption Associated with HIV in the Brain: "Reseeding CNS during ART Interruption Leading to Intrathecal Immune Activation" - "HIV-1 Viral Escape in Cerebrospinal Fluid of Subjects on Suppressive Antiretroviral Treatment" - (09/18/17)
-------------------------------
Viral rebound in semen after treatment interruption in a HIV therapeutic vaccine double-blind trial (VRI02/ANRS149-LIGHT)
Reported by Jules Levin
Presented at IAS 2017 Paris
J. Ghosn1, R. Palich2, A. Chaillon3,4, V. Boilet5,6, M.-L. Nere2, P. Delobel7, F. Lutch8, O. Bouchaud9, J.-M. Molina10, M.-L. Chaix2,4, C. Delaugerre2,4, V. Rieux4,11, R.
Thiebaut5,6, Y. Levy4,12,13, J.-D. Lelièvre4,12,13

Institutions
1Hotel-Dieu university hospital center, university of Paris Descartes, Therapeutic, Immunology and Infectious Disease, Paris, France, 2Saint-Louis university hospital center, university of Paris Diderot, Virology, U941, Paris, France, 3University of California San Diego, Medicine, San Diego, United States, 4Vaccine Research Institute - VRI, Paris, France, 5INSERM U1219, ISPED, Bordeaux Population Health, Bordeaux, France, 6Vaccine Research Institute - VRI, CMG, Bordeaux, France, 7Toulouse-Purpan University Hospital Center, Infectious Diseases, Toulouse, France, 8Saint-Etienne University Hospital Center, Infectious Diseases, Saint-Etienne, France, 9Avicenne University Hospital Center, Infectious Diseases, Paris, France, 10Saint-Louis university hospital center, university of Paris Diderot, Infectious Diseases, U941, Paris, France, 11French National Agency for Research on AIDS and Viral Hepatitis (ANRS), Paris, France, 12INSERM U955, IMRB, Equipe 16, Creteil, France, 13Henri Mondor University Hospital Center, Creteil, France
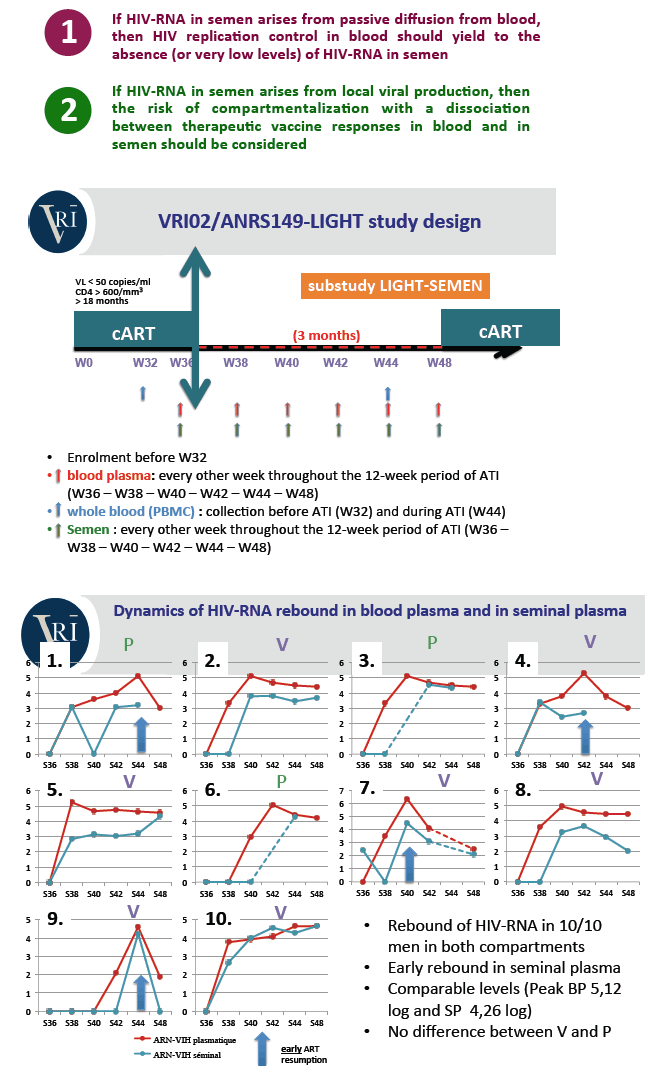
Background: Antiretroviral treatment interruption (ATI) leads to HIV replication rebound in both blood and semen, however dynamic of HIV-RNA rebound in semen is poorly known. We compared HIV-RNA timing of and level of rebound in blood and seminal plasmas (BP-SP) and characterized the HIV rebounding populations in both compartments after ATI in HIV-1 infected patients enrolled in the therapeutic vaccine trial VRI02/ANRS149-LIGHT.
Methods: Ten male from the VRI02/ANRS149-LIGHT trial with CD4 cells ≥600/mm3 and HIV-RNA < 50cp/ml under treatment for at least 18 months were studied. ATI occurred from week (W)36 to W48. Paired blood and semen samples were collected at W32 (before ATI), W36, W38, W40, W42, W44 and W48 following ATI, for HIV-RNA and DNA quantification. Ultradeep sequencing (UDS, 454/Roche) of partial env (C2/V3) HIV-DNA and -RNA was performed in 5 out of 10 participants in PBMC before ATI and in plasma/semen during ATI. Sequenced reads were quality filtered and assembled using an in-house data processing pipeline.
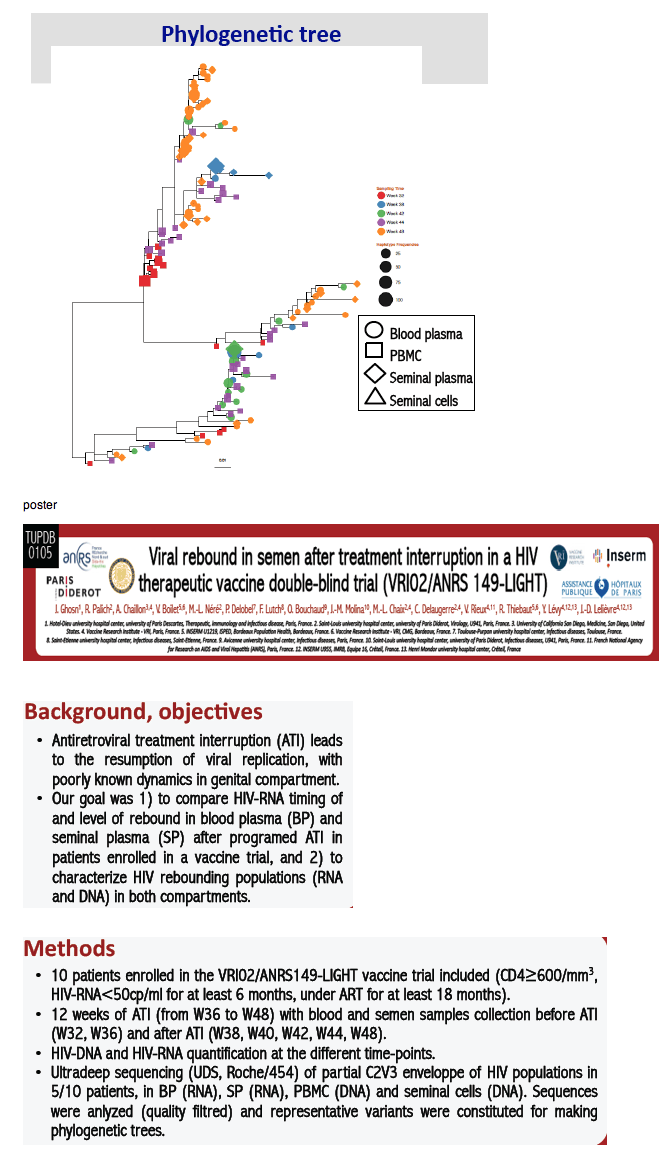
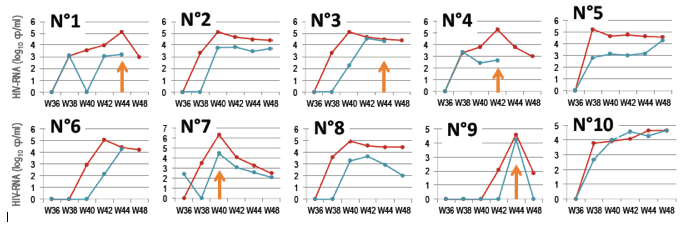
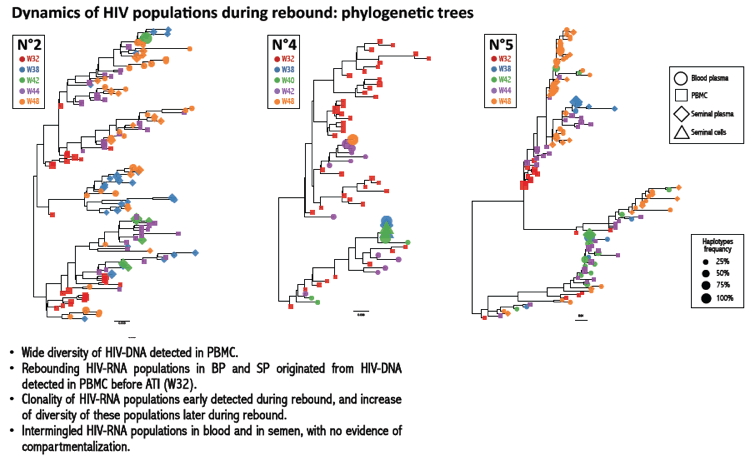
Results: Patients had sustained suppressed blood viral load for a median of 44 months (range: 28-152) before ATI. HIV-RNA rebounded in blood and semen in all patients after ATI (median 5.12 log10 cp/ml (range: 4.61-6.35) and 4.26 log10 cp/ml (range: 3.20-4.67), respectively). BP HIV-RNA rebounded as soon as W38 in 8/10 patients, and SP HIV-RNA between W38 and W40 in 8/10 patients. HIV-DNA median level was 2.97 log10 cp/106 PBMC (range: 1.61-3.26) at W32 and 3.30 log10 cp/106 PBMC (range: 2.50-3.67) at W44. Non-sperm cells HIV-DNA was detected in at least one sample in 6/10 patients. Phylogenetic analysis of UDS revealed that 1) rebounding HIV-RNA population in BP and in SP originated from PBMC HIV-DNA at the time of ATI and 2) intermingled HIV-RNA populations in BP and in SP with no evidence of compartmentalization.
Conclusions: The rapid and intense HIV RNA rebound observed very early both in blood and semen after ATI emphasizes the need for targeted prevention strategies to reduce the risk of sexual transmission during ATI. PBMC HIV-DNA is the major contributor for HIV-RNA rebound in both compartments, even after several years of sustained suppressed viral replication.


---------------------------------------------------
RV397 clinical trial of VRC01 administration to participants who initiated antiretroviral therapy during acute HIV infection.
HIV-Specific Broadly-Neutralizing Monoclonal Antibody, VRC01, Minimally Impacts Time to Viral Rebound Following Treatment Interruption in Virologically-Suppressed, HIV-Infected Participants who Initiated Antiretroviral Therapy during Acute HIV Infection
Trevor A. Crowell, Donn J. Colby, Suteeraporn Pinyakorn, Jintana Intasan, Khunthalee Benjapornpong, Kamonkan Tanjnareel, Nicolas Chomont, Lydie Trautmann, Sodsai Tovanabutra, Shelly Krebs, Diane Bolton, Adrian McDermott, Robert Bailer, Nicole Doria-Rose, Bijal Patel, Robert J. Gorelick, Brandie A. Fullmer,
Pornsuk Visudhiphan, Robert J. O'Connell, Randall Tressler, John Mascola, Nelson L. Michael, Merlin L. Robb,
Nittaya Phanuphak, and Jintanat Ananworanich
for the RV397 and RV254/SEARCH010 Study Groups.
In this small experience, VRC01 was generally well-tolerated when administered during intensely monitored interruption of antiretroviral therapy.
This randomized study demonstrated that VRC01 administration was associated with a trend toward delayed virologic rebound when given to participants who initiated ART during acute HIV infection.
However, VRC01 monotherapy was insufficient to maintain viral suppression, even in this carefully selected population. Mechanisms investigating breakthrough viremia require further investigation.
The efficacy signal observed in this study gives hopes that combination therapies, particularly ones with the next generation of more potent and long-lasting agents may be more efficacious.
Further research is needed to investigate mechanisms of virologic control and factors that impact time to viral rebound, particularly in the one person with sustained virologic control.
This study also adds to the body of evidence that treatment interruption studies can be safely conducted and future studies may also consider allowing for more prolonged periods of viremia prior to ART re-initiation in order to better observe the virologic effects of novel interventions.

For reasons that have been previously described, individuals who initiated ART during acute HIV infection are excellent candidates for the testing of novel therapies with the goal of achieving HIV remission.
VRC01 is such a therapy. It is a broadly-neutralizing HIV-specific monoclonal antibody that targets the CD4 binding site. It's antiviral activity has been well-established in pre-clinical and clinical trials. In participants with chronic, otherwise untreated HIV, VRC01 decreases plasma HIV RNA. In participants with chronic, treated HIV, VRC01 serial infusions delayed viral rebound after ART interruption as compared to historic controls.
⋅ Based on these prior findings, we undertook a randomized, placebo-controlled clinical trial of VRC01 administered to participants who initiated ART during acute HIV infection.

We hypothesized that participants receiving VRC01 would maintain a higher rate of viral suppression at 24 weeks following analytic treatment interruption as compared to participants receiving placebo.

Participants for this study were recruited from the RV254 cohort in Bangkok, Thailand. The study targeted enrollment of 24 adults who initiated suppressive ART during Fiebig stages I-III and whose HIV had been well-controlled for at least 2 years.
1) On the day of each participant's first study infusion, ART was discontinued. Participants were randomized in a 3:1 ratio, stratified by Fiebig stage, to receive either VRC01 or placebo every 3 weeks for up to 24 weeks.
2) At 24 weeks, participants received their final study infusion and the study's primary endpoint-virologic control with HIV RNA <50 copies/mL-was assessed.
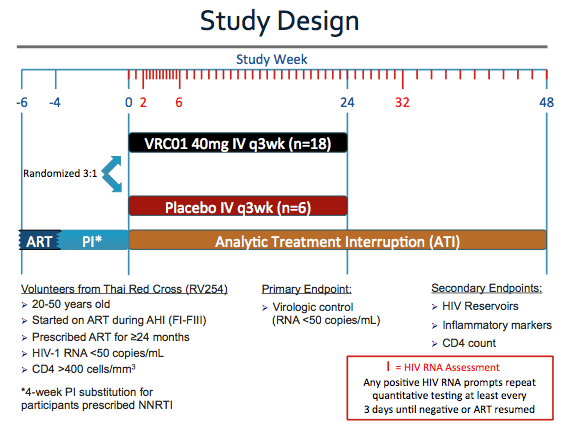
The protocol stated that ART would be resumed for any of the reasons listed here.
Ultimately, every participant who restarted ART did so because of this first criterion, plasma HIV RNA above 1,000 copies/mL on two separate measurements at least one day apart.

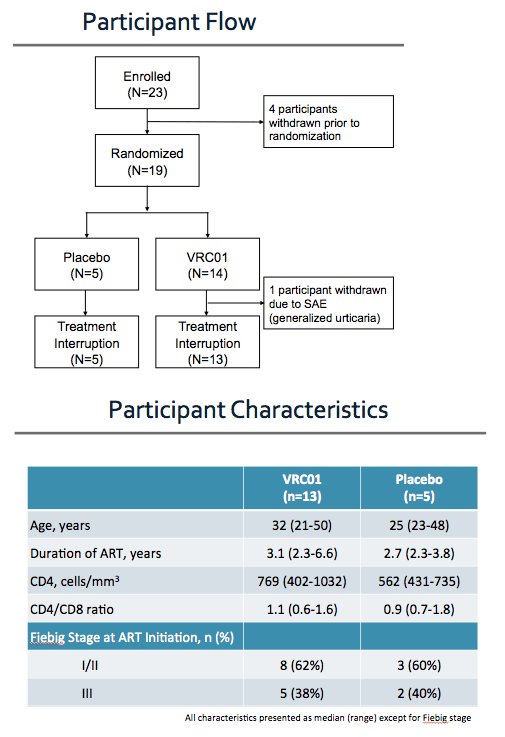
This study had a target enrollment of 24 participants. However, enrollment was halted early because of barriers to the importation of study product into Thailand that developed after the study had started.
Nineteen participants were randomized and one of these participants experienced severe generalized urticaria during the first study infusion. The study infusion was discontinued and this participant did not undergo treatment interruption.
http://emedicine.medscape.com/article/137362-overview
http://www.merckmanuals.com/professional/dermatologic-disorders/approach-to-the-dermatologic-patient/urticaria
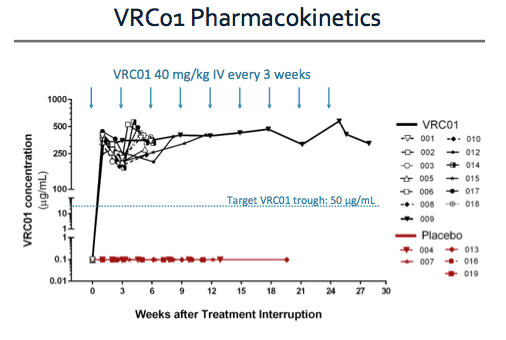
Serum VRC01 levels at various timepoints are shown here. For all participants randomized to the VRC01 arm of the study, serum VRC01 levels were consistently above the target trough level of 50 micrograms/mL.
Additionally, functional assays demonstrated expected neutralization activity against tier-1 and tier-2 viruses when mixed with participant serum throughout the dosing interval.
VRC01 levels were in the target range even at the time of viral rebound in participants who experienced viral rebound during the infusion phase of the study.
There was one serious adverse event in the study, which was the severe generalized urticaria that was previously mentioned. Most other adverse events were mild and rates were not substantially different between the VRC01 and placebo groups.
There were no hospitalizations, no cases of acute retroviral syndrome, and no participants with new drug resistance mutations at the time of viral rebound.
All participants were tested for anti-VRC01 antibodies at various timepoints, including at the time of ART resumption, and no anti-VRC01 antibodies were observed.
Once ART was reinitiated, all participants achieved virologic resuppression within about five weeks and many did so in considerably less time.

This figure shows viral load measurements for the 18 study participants who underwent treatment interruption. The black lines represent participants in the VRC01 arm and the red lines represent those in the placebo arm. You can see that many participants in the placebo arm had detectable viremia at week 2 after ART was stopped. In the VRC01 arm, there appears to be a modest delay in the time to viral rebound.
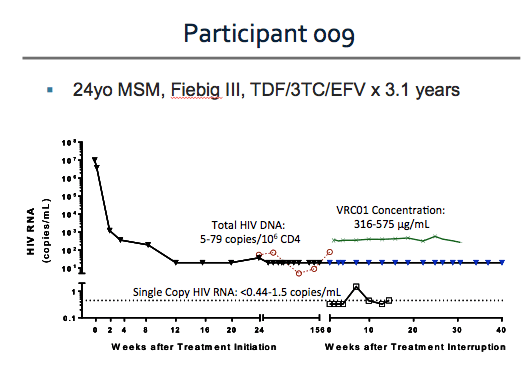
(1) There is one participant, Participant 009 in the VRC01 arm, who maintained an undetectable viral load through week 42. This participant just experienced a detectable qualitative HIV RNA on Thursday.
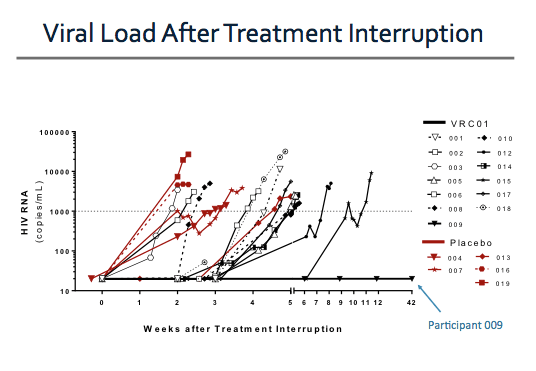
Participant 009 is a 24-year-old Thai man who has sex with men. He initiated ART during Fiebig stage III and had been virologically suppressed on tenofovir, lamivudine, and efavirenz for about 3 years at the time of entry into RV397. Serial viral load assessments for this participant were as shown.
⋅ (1)Additional assessments via the ultrasensitive single copy assay reveal low-level viremia up to 1.5 copies/mL during the study period without progression to detectable viremia on standard clinical assays.
⋅ (2)Total HIV DNA was measured in peripheral CD4 cells at multiple time points prior to treatment interruption and was in the range of 5-79 copies/106 cells.
⋅ (3)VRC01 concentrations were well above the target trough of 50 mcg/mL throughout this participant's dosing.
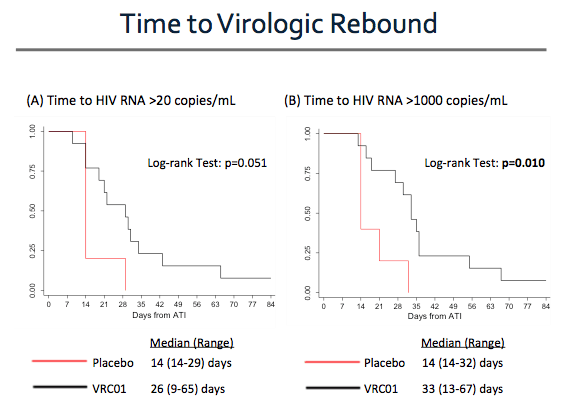
Overall, there is a trend toward delayed virologic rebound among participants receiving VRC01. This slide presents Kaplan-Meier curves evaluating time to rebound using two different threshold viral load levels.
On the left, 20 copies/mL is used, representing the lower limit of detection for the clinical HIV RNA assay used in this study. Participants in the placebo group experienced their first detectable viral load at a median of 14 days after treatment interruption, whereas participants in the VRC01 group experienced their first detectable viral load at a median of 26 days.
On the right side of the slide, the same analysis is presented using a higher threshold for viral rebound of 1000 copies/mL. Here we see a statistically significant delay in the time to viral rebound in the VRC01 group as compared to placebo.
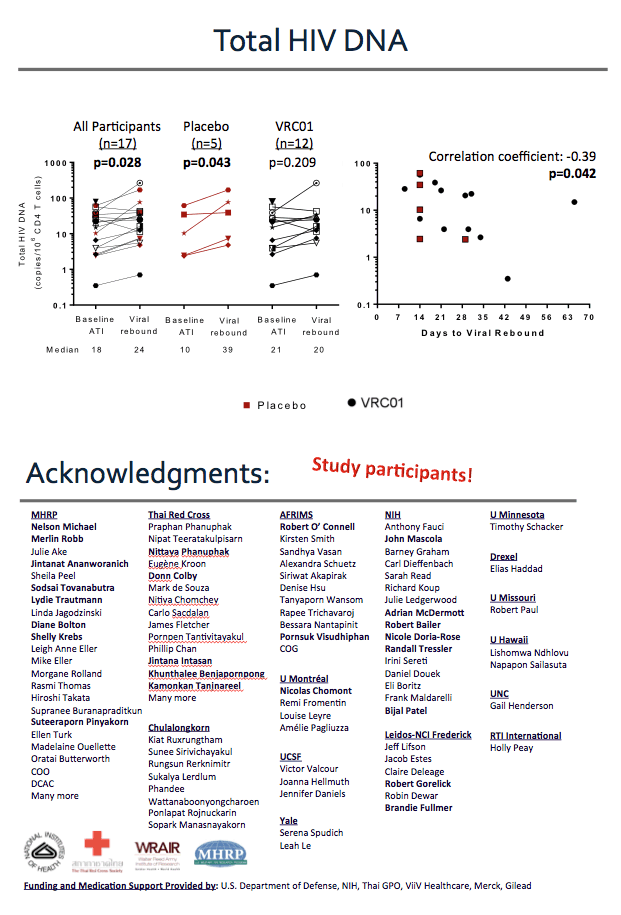
Viral rebound was associated with a small but statistically significant increase in total HIV DNA in the placebo group but not the VRC01 group.
In both groups, the overall frequency of infected cells remained low at all time points as compared to what is observed in individuals who initiated ART during the chronic phase of HIV infection.
Total HIV DNA at the time of treatment interruption was significantly, but not strongly, correlated with the time to rebound viremia.
|
| |
|
 |
 |
|
|