 |
 |
 |
| |
Heightened Risk of Peripheral Arterial Disease With HIV in Veterans
|
| |
| |
9th IAS Conference on HIV Science (IAS 2017), July 23-26, 2017, Paris
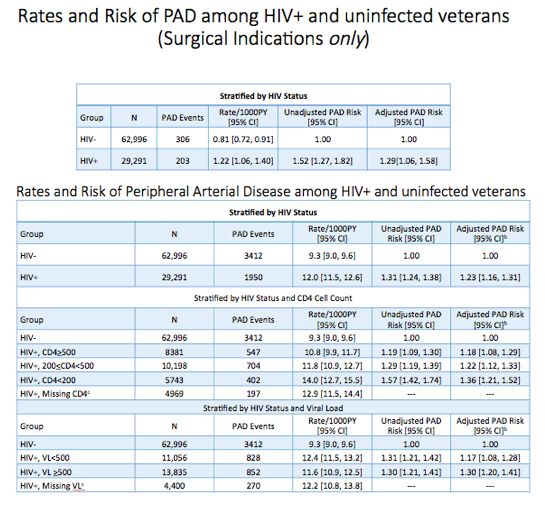
from Jules: this is an interesting and eye-raising study. HIV+ have a 50% higher PAD/Peripheral Artery Disease rate vs HIV-nagtives, due to HIV & inflammation plus having worse traditional risk factors, and not exercising or eating a good diet. Peripheral artery disease is associated with heart disease & stroke. Look at the table immediately below & you see the risk for peripheral artery disease in HIV+ vs HIV-negative vets who are themselves not the healthiest comparison group. And look at the affect of low CD4 and detectable viral load. Other associations with peripheral artery disease, which is second largest clinical manifestation of atherosclerosis; individuals with PAD have increased risk for MACE, major cardiovascular events - associations include: diabetes with or without insulin; hypertension controlled or not; elevated LDL; low HDL; triglycerides over 150; of course smoking with current smoking much worse bur former smoking has increased risk; HCV infection; low eGFR <30 (kidney disease); anemia: low hemoglobin; history of cocaine use; and COPD.
Mark Mascolini
A study of 92,000 US veterans linked HIV infection to a higher risk of peripheral arterial disease even after accounting for classic cardiovascular risk factors [1]. Veterans with higher HIV loads and lower CD4 counts ran the highest risk of peripheral arterial disease.
Peripheral arterial disease, the second most frequent manifestation of atherosclerosis, affects about 8 million people in the United States and 202 million worldwide. Prior research links HIV infection to a higher risk of acute myocardial infarction [2] and stroke [3]. To determine whether a similar association holds for peripheral arterial disease, Veterans Aging Cohort (VACS) investigators conducted this study.
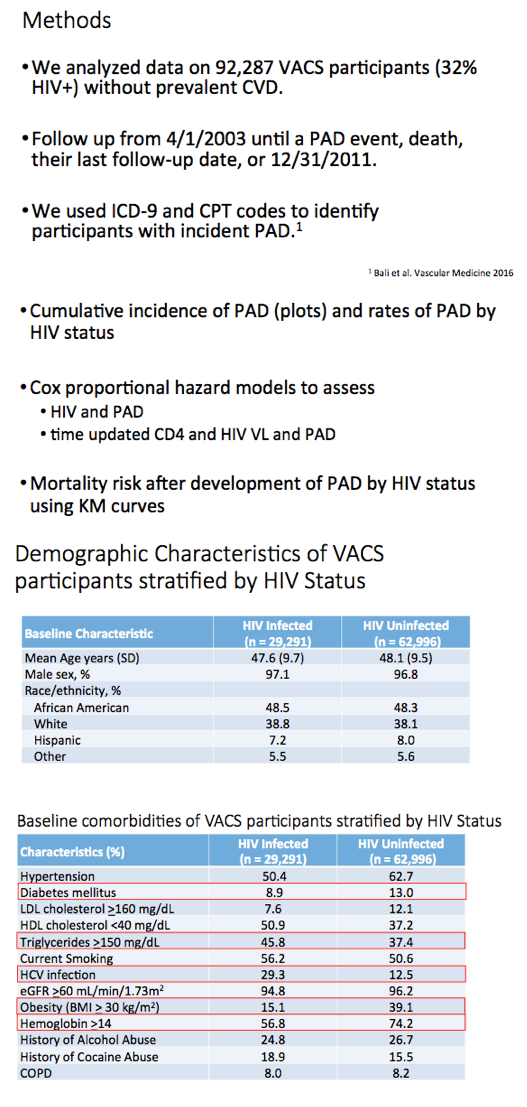
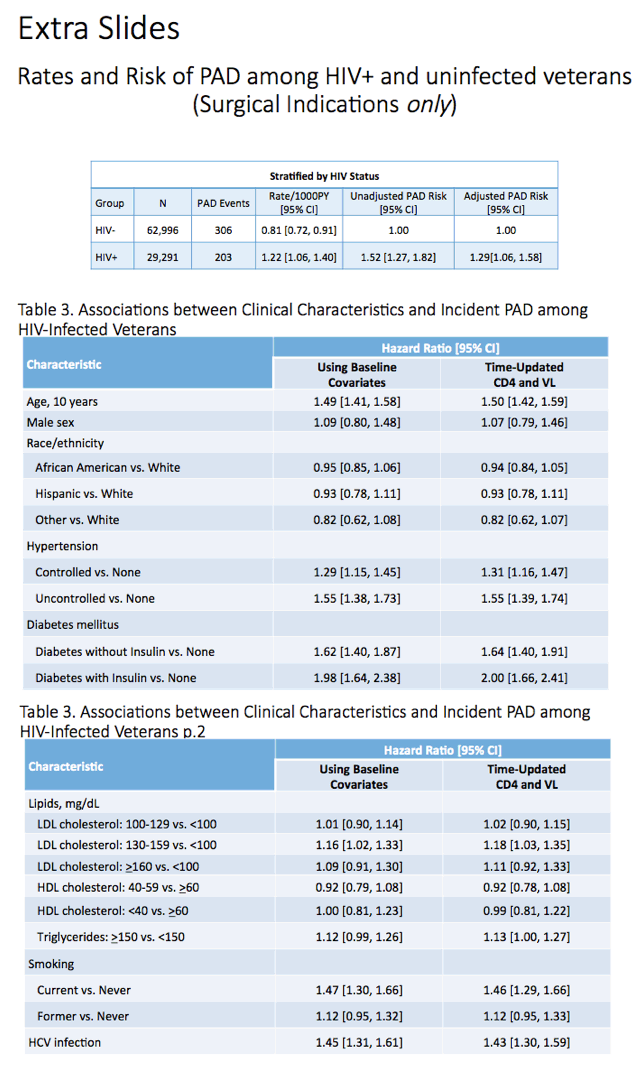
The analysis focused on 92,287 US veterans, 29,291 of them (32%) with HIV. Follow-up ran from April 2003 until peripheral arterial disease, death, last follow-up date, or December 2011. The investigators identified incident (newly diagnosed) peripheral arterial disease with ICD-9 and CPT codes. They used Cox proportional hazard models to assess potential associations between (1) HIV and peripheral arterial disease and (2) time-updated CD4 count and viral load and peripheral arterial disease. These analyses adjusted for age, sex, race/ethnicity, hypertension, diabetes, antiretroviral treatment status, and numerous other clinical variables. The researchers used Kaplan-Meier analysis to assess risk of death after peripheral arterial disease developed.
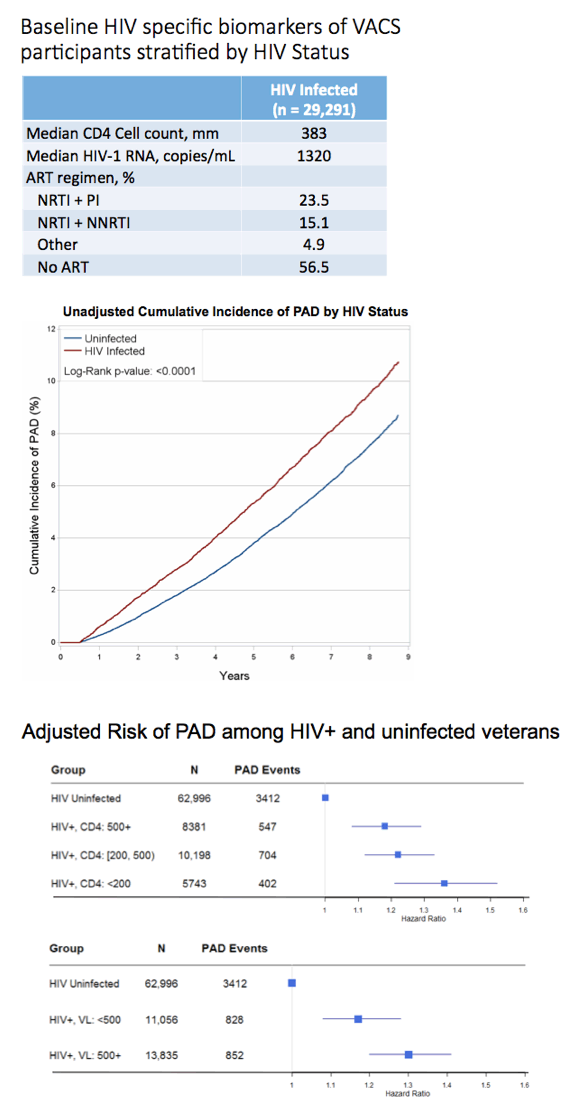
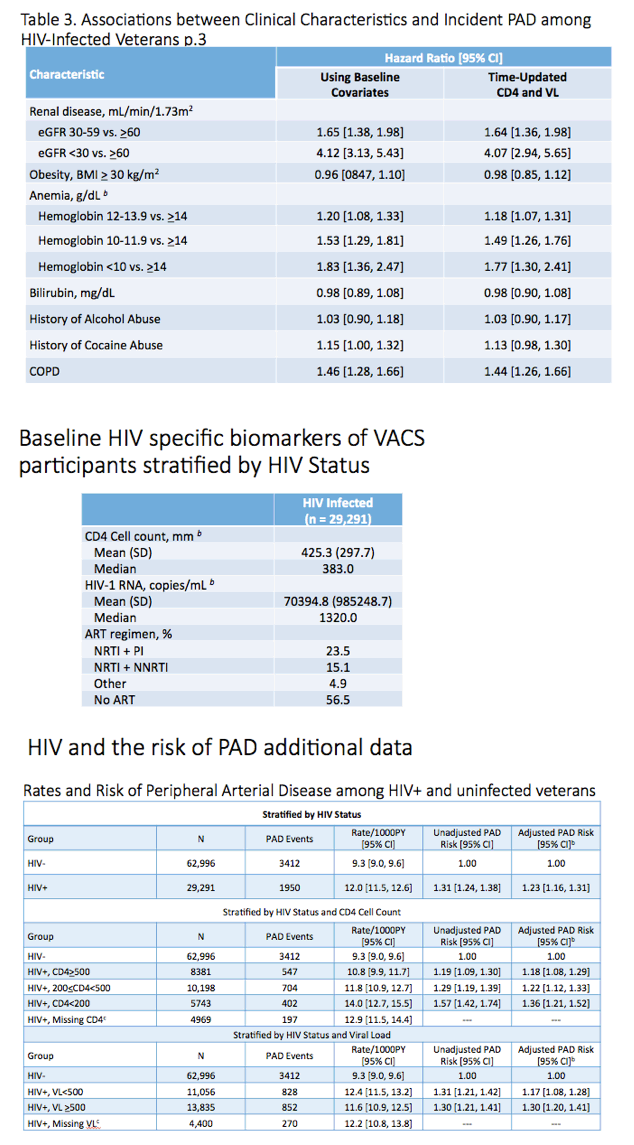
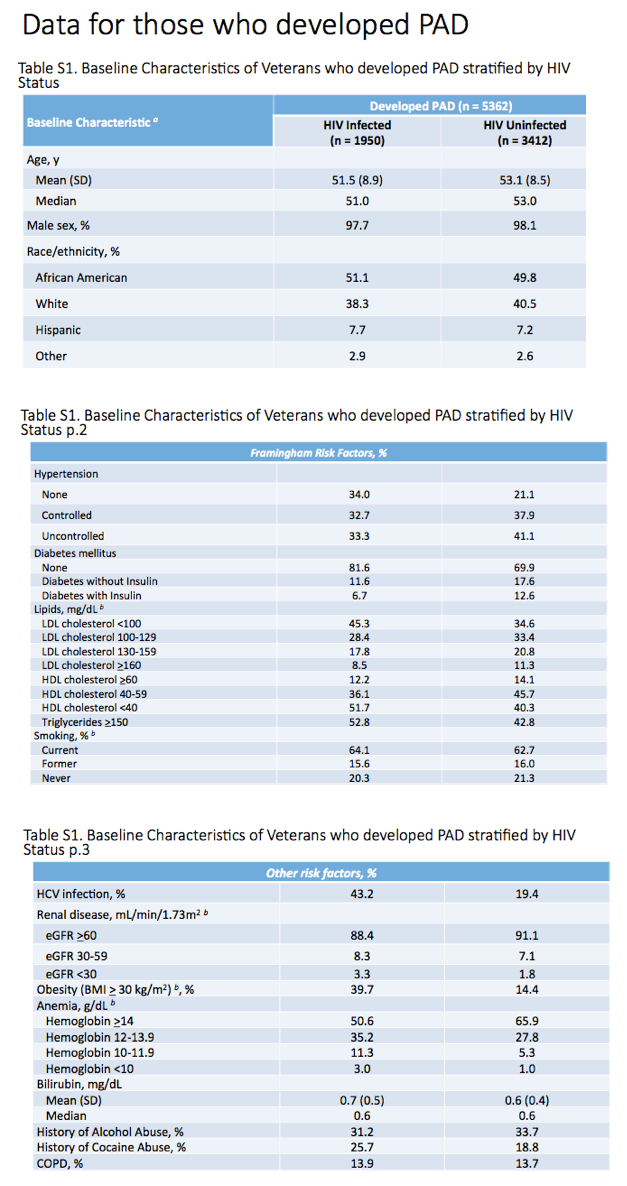
The HIV group was similar to the HIV-negative group in average age (47.6 and 48.1), proportion of men (97.1% and 96.8%), and proportions of blacks (48.5% and 48.3%), whites (38.8% and 38.1%), and Hispanics (7.2% and 8.0%). Lower proportions of HIV-positive veterans had hypertension (50.4% versus 62.7%) or diabetes (8.9% versus 13%), but a higher proportion had triglycerides at or above 150 mg/dL (45.8% versus 37.4%). Among veterans with HIV, median baseline CD4 count stood at 383 and median viral load at 1320 copies. At baseline 56.5% of veterans with HIV were not taking antiretroviral therapy.
In adjusted analysis HIV infection was independently associated with incident peripheral arterial disease regardless of CD4 bracket (hazard ratios [HR] ranging from about 1.2 to almost 1.4) or viral load (HR ranging from almost 1.2 to 1.3).
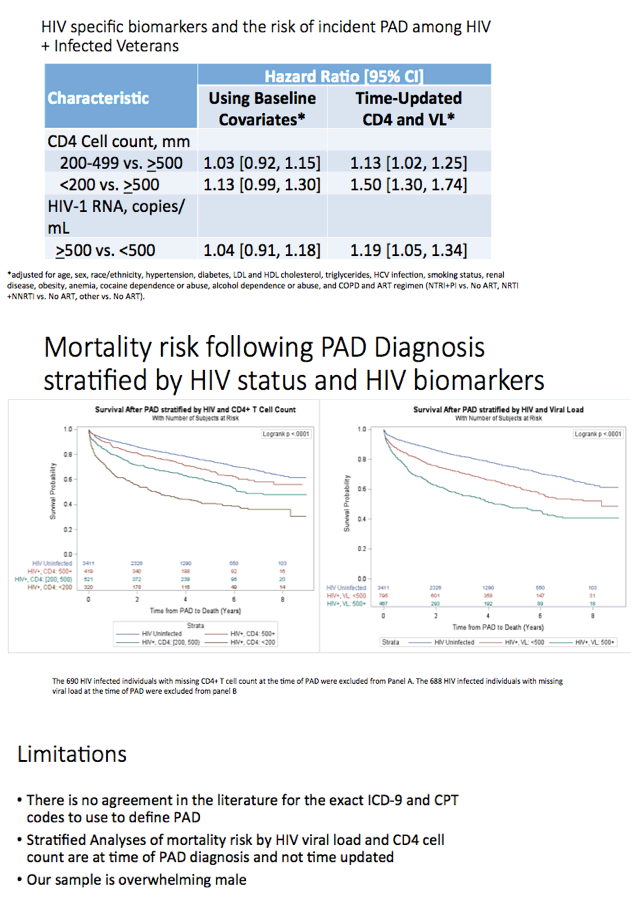
In the adjusted analysis with time-updated CD4 count, HIV-positive veterans with 200-499 CD4s versus 500 or more had a 13% higher risk of peripheral arterial disease (HR 1.13, 95% confidence interval [CI] 1.02 to 1.25) while veterans with fewer than 200 CD4s versus 500 had a 50% higher risk (HR 1.5, 95% CI 1.30 to 1.74). An adjusted analysis with time-updated viral load determined that veterans with a load of 500 copies or more versus a lower load had almost a 20% higher risk of peripheral arterial disease (HR 1.19, 95% CI 1.05 to 1.34).
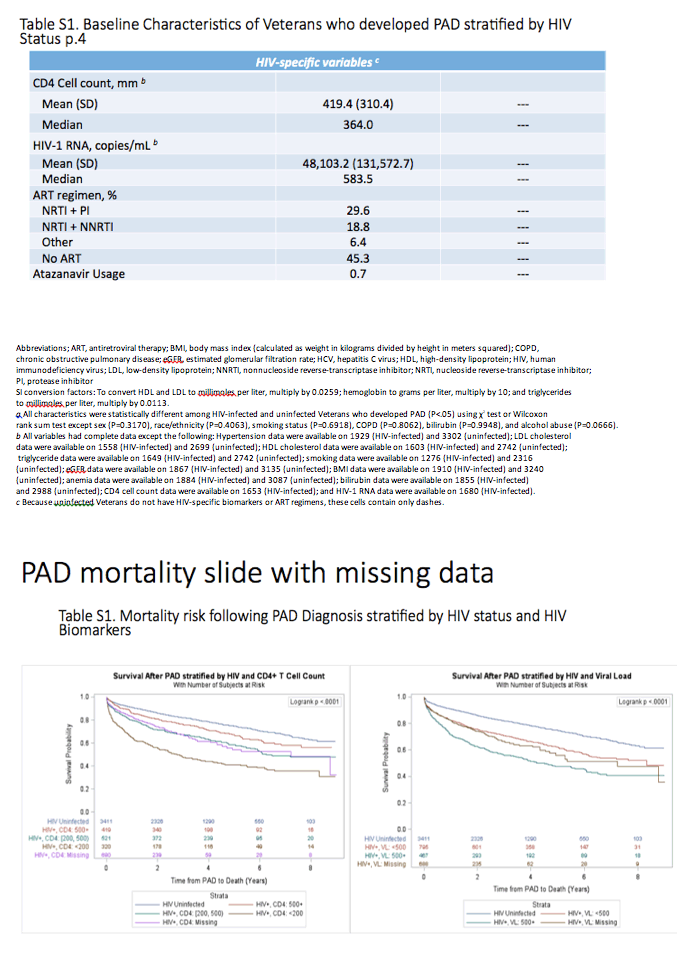
Analysis of survival through 8 years after peripheral arterial disease diagnosis excluded veterans with missing CD4 or viral load data. Compared with HIV-negative veterans, survival was shorter in veterans with more than 500 CD4 cells at diagnosis, shorter still in those with 200 to 500 CD4s, and shortest in those with fewer than 200 CD4s (P < 0.0001). Similarly, through 8 years of follow-up after diagnosis, survival was shorter with than without HIV in those with a viral load below 500 copies at diagnosis and shorter still in those with a higher viral load (P < 0.0001).
The VACS team concluded that, in veterans with HIV, "those with higher HIV viral loads and lower CD4 cell counts have the highest risk of peripheral arterial disease." And after diagnosis, mortality is greatest in HIV-positive veterans with immunodeficiency or a detectable viral load.
References
1. Freiberg M, Duncan M, Justice A, Beckman J, Veterans Aging Cohort Study. HIV infection and the risk of peripheral arterial disease. 9th IAS Conference on HIV Science (IAS 2017), July 23-26, 2017, Paris. Abstract WEAB0102.
2. Freiberg MS, Chang CC, Kuller LH, et al. HIV infection and the risk of acute myocardial infarction. JAMA Intern Med. 2013;173:614-622.
3. Chow FC, Regan S, Feske S, Meigs JB, Grinspoon SK, Triant VA. Comparison of ischemic stroke incidence in HIV-infected and non-HIV-infected patients in a US health care system. J Acquir Immune Defic Syndr. 2012;60:351-358.
a CI = confidence interval; HIV = human immunodeficiency virus; PAD = peripheral arterial disease; PY = person years
b adjusted for age, sex, race/ethnicity, hypertension, diabetes, LDL and HDL cholesterol, triglycerides, HCV infection, smoking status, renal disease, obesity, anemia, cocaine dependence or abuse, alcohol dependence or abuse, and COPD.
c missing category used only for calculation of incidence rates. For models, missing CD4 cell counts and viral load were imputed

Abbreviations; ART, antiretroviral therapy; BMI, body mass index (calculated as weight in kilograms divided by height in meters squared); COPD, chronic obstructive pulmonary disease; eGFR, estimated glomerular filtration rate; HCV, hepatitis C virus; HDL, high-density lipoprotein; HIV, human immunodeficiency virus; LDL, low-density lipoprotein; NNRTI, nonnucleoside reverse-transcriptase inhibitor; NRTI, nucleoside reverse-transcriptase inhibitor; PI, protease inhibitor
SI conversion factors: To convert HDL and LDL to millimoles per liter, multiply by 0.0259; hemoglobin to grams per liter, multiply by 10; and triglycerides to millimoles per liter, multiply by 0.0113.
a All characteristics were statistically different among HIV-infected and uninfected Veterans who developed PAD (P<.05) using χ2 test or Wilcoxon rank sum test except sex (P=0.3170), race/ethnicity (P=0.4063), smoking status (P=0.6918), COPD (P=0.8062), bilirubin (P=0.9948), and alcohol abuse (P=0.0666).
b All variables had complete data except the following: Hypertension data were available on 1929 (HIV-infected) and 3302 (uninfected); LDL cholesterol data were available on 1558 (HIV-infected) and 2699 (uninfected); HDL cholesterol data were available on 1603 (HIV-infected) and 2742 (uninfected); triglyceride data were available on 1649 (HIV-infected) and 2742 (uninfected); smoking data were available on 1276 (HIV-infected) and 2316 (uninfected); eGFR data were available on 1867 (HIV-infected) and 3135 (uninfected); BMI data were available on 1910 (HIV-infected) and 3240 (uninfected); anemia data were available on 1884 (HIV-infected) and 3087 (uninfected); bilirubin data were available on 1855 (HIV-infected) and 2988 (uninfected); CD4 cell count data were available on 1653 (HIV-infected); and HIV-1 RNA data were available on 1680 (HIV-infected).
c Because uninfected Veterans do not have HIV-specific biomarkers or ART regimens, these cells contain only dashes.

|
| |
|
 |
 |
|
|