 |
 |
 |
| |
More and earlier cardiovascular events (CVE) and shorter overall survival (OS) in HIV-positive patients (HIV+) compared to the general population differ by sex
|
| |
| |
"HIV+ males had the highest mortality rate and a higher risk to die or to get CVE at younger age than the general population."
Reported by Jules Levin
9th IAS Science 2017 July 23-26 Paris, France
Stefan Esser1, Marina Arendt2, Christina Schulze1, Volker Holzendorf3, Norbert H. Brockmeyer4, Robert Jablonka, Karl-Heinz Jockel2, Raimund Erbel2, Nico Reinsch5,6 on behalf of HIV HEART Study Group and Heinz Nixdorf Recall Investigative Group
1 Clinic of Dermatology, Department of Venereology, University Hospital Essen, Essen, Germany 2 Institute for Medical Informatics, Biometry and Epidemiology (IMIBE), University Hospital Essen, Essen, Germany
3 Clinical Trial Centre Leipzig - Coordination Centre for Clinical Trials (ZKS Leipzig - KKS), University Leipzig, Germany 4 Germany Clinic of Dermatology, Venerology and Allergology, Center for Sexuell Health and Medizin Ruhruniversity Bochum, Bochum, Germany
5 Department of Internal Medicine I and Cardiology, Devision of Electrophysiology, Alfried Krupp Hospital, Essen, Germany
6 University Witten/ Herdecke, Witten, Germany

abstract
Background: The OS of HIV+ should be adapted to the general population by antiretroviral treatment. But in the aging HIV+ CVE and strokes became more frequent.
Methods: We compare CVE, stroke and OS of HIV+ outpatients of the HIV HEART study (HIVH) and of HIV-negative controls of the population-based Heinz Nixdorf Recall study (HNR), both recruited from the German Ruhr area. HIVH cases with HNR controls are matched in a 1:2 ratio by sex and age. CVE are defined by myocardial infarction and sudden cardiac death. Cox proportional hazard models are used to investigate the impact of study affiliation on OS, CVE and stroke with time from study start to event or last contact. We adjust for age, active smoking and for men additionally for diabetes.
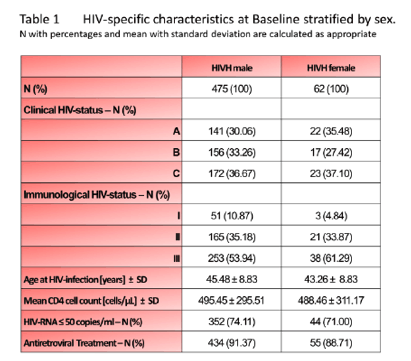
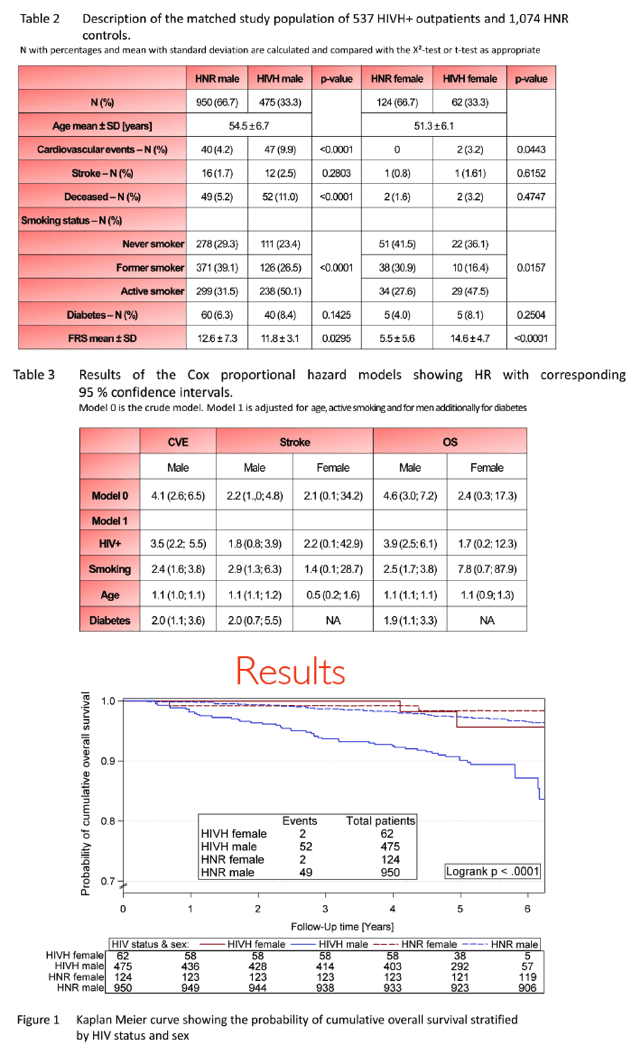
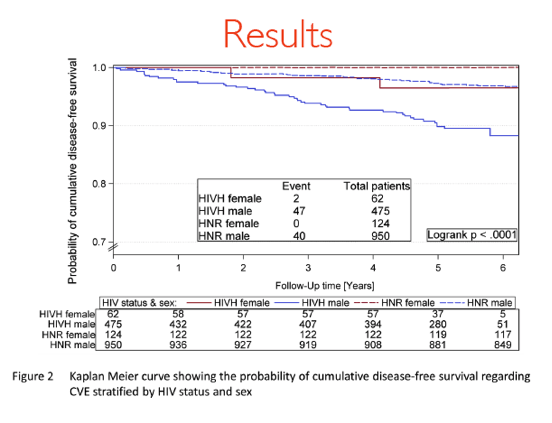
Results: Descriptions are shown in table 1. We observe adjusted Hazard ratios (HR) of 3.5 (95%-CI: 2.2; 5.5) for CVE for male HIVH vs. HNR and for stroke of 1.8 (0.8; 3.9) for male and 2.2 (0.1; 42.9) for female HIVH vs. HNR. The OS in male and female HIVH vs. HNR has an HR of 3.9 (2.5; 6.1) and 1.7 (0.2; 12.3), respectively. The smoking status is different in male subjects (p< 0.0001) and the Framingham Risk score (FRS) is different in female subjects (p< 0.0001). Men differ highly in variables related to blood fats and BMI, women differ in terms of blood pressure and heartrate which is also displayed in the highly different FRS.
Conclusions: HIV+ males had an increased incidence of CVE compared with HIV-negative controls in spite of similar FRS at baseline in contrast to HIV+ females with higher FRS than controls but comparable rates of CVE. HIV+ males had the highest mortality rate and a higher risk to die or to get CVE at younger age than the general population.

|
| |
|
 |
 |
|
|