 |
 |
 |
| |
Is on-demand PrEP with TDF/FTC effective
among MSM with infrequent sexual intercourse?
|
| |
| |
Reported by Jules Levin
9th IAS Conference on HIV Science (IAS 2017), July 23-26, 2017, Paris
A sub-study of the ANRS Ipergay trial
Guillemette Antoni 1, Cecile Tremblay2, Isabelle Charreau1, Eric Cua3, Daniela Rojas4, Nolwenn Hall5, Julie Chas6, Thomas Huleux7, Bruno Spire8,
Catherine Capitant1, Laurent Cotte9, Laurence Meyer1,10, Jean-Michel Molina11,12
1: INSERM SC10 2: Centre Hospitalier de l'Universite de Montreal 3: Hopital de l'Archet, Nice 4: Association AIDES 5: Hotel-Dieu, Nantes 6: Hopital Tenon, Paris 7: Hopital G. Dron, Centre Hospitalier Universitaire de Tourcoing 8: INSERM UMR 912 SESSTIM 9: Hopital de la Croix Rousse, Centre Hospitalier et Universitaire de Lyon 10: Universite Paris Sud 11: Hopital Saint-Louis, Assistance Publique Hopitaux de Paris 12: Universite de Paris Diderot Paris 7, Sorbonne

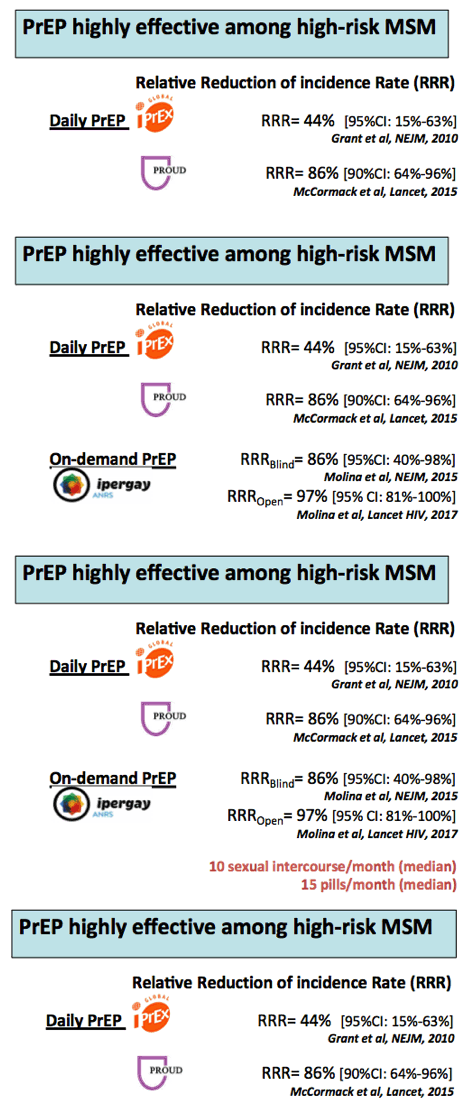
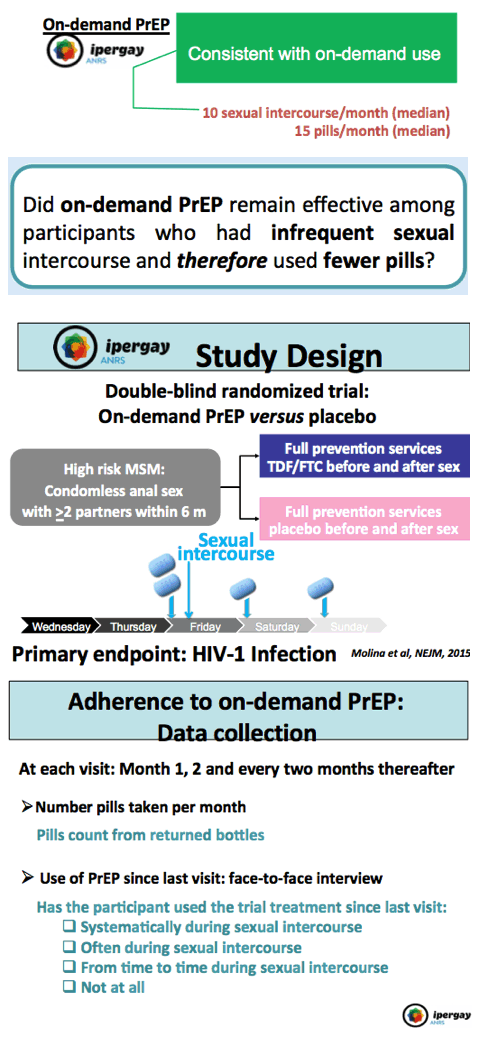
Background: The ANRS IPERGAY trial demonstrated among MSM a 86% relative reduction of HIV-1 incidence with on demand PrEP in the TDF/FTC arm (2 infections, 219 person-years (py) of follow-up (FU), incidence: 0.91/100 py) as compared to the placebo arm (14 infections, 212 py of FU, incidence: 6.60/100 py). Participants in this trial used a median of 15 pills /month and had a median of 10 sexual intercourse /month. We wished to investigate whether on demand PrEP remained effective among participants having less frequent sexual intercourse and using fewer pills.
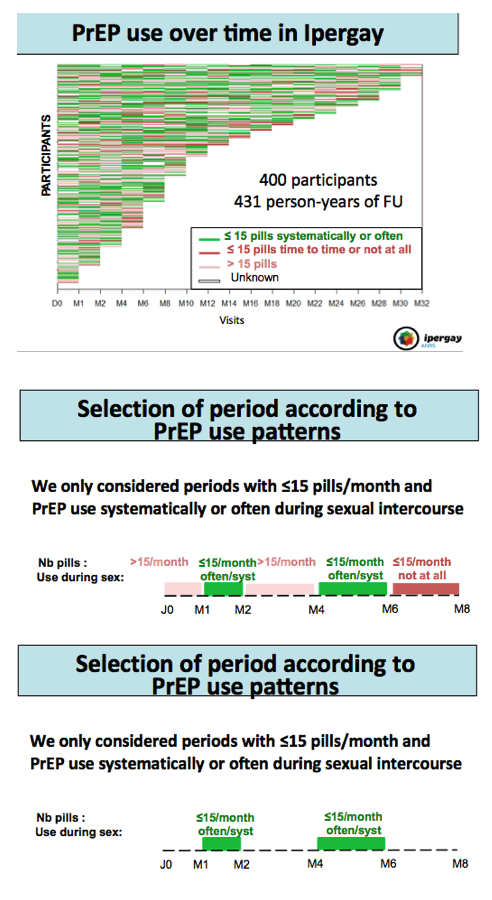
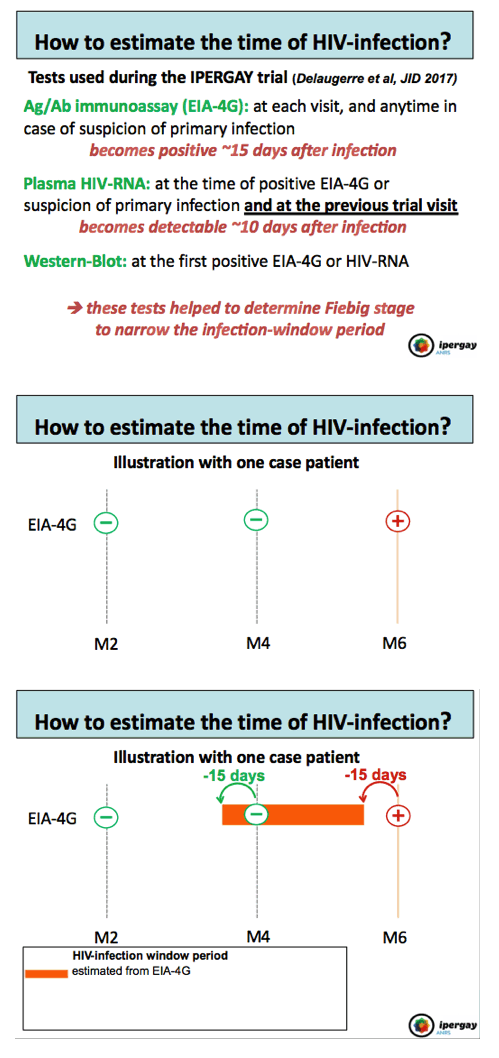
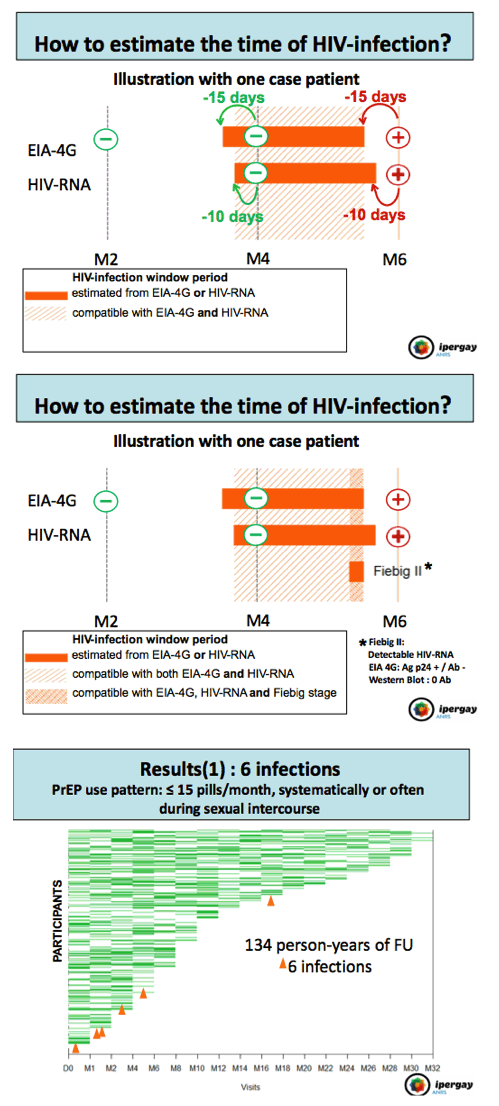
Methods: Assuming that participants with less frequent sexual intercourse would use fewer pills, and because individual patterns of pill use showed large intra-participant variability over time, we focused our analysis on person-time between 2 consecutive visits when participants used < 15 pills /month and PrEP was used "systematically or often" during sexual intercourse, and not "from time to time or never". We then cumulated in each arm FU time spent with this pattern of pill use. A 4th generation HIV-1/2 ELISA assay was performed at each visit allowing to date the time of HIV-infection. Incidence rates of HIV-infection/100 py in both arms were then compared using mid-p exact test.
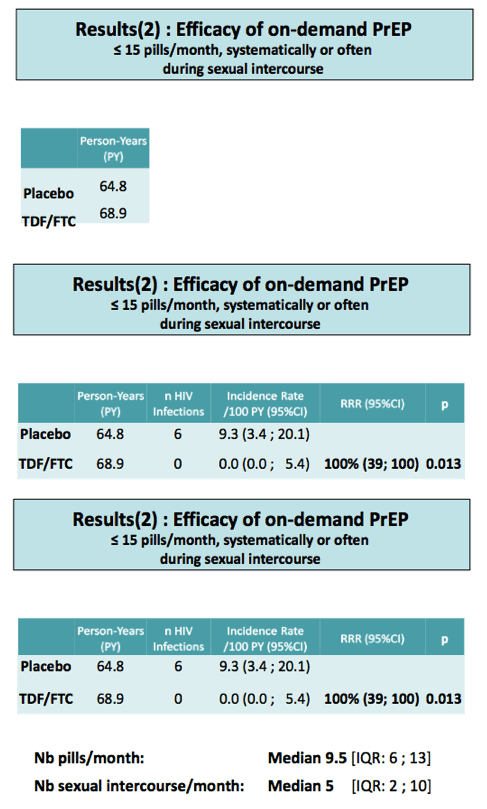
Results: Six HIV-1 infections occurred during FU among participants using < 15 pills/month taken "systematically or often" during sexual intercourse: 6 in the placebo arm (incidence: 9.3/100 py, total FU time: 64.8 py) and 0 in the TDF/FTC arm (incidence: 0/100 py, total FU time: 68.9 py, p=0.013). The relative reduction of HIV incidence was 100% (95% CI: 20-100). During these follow-up periods, a median of 5 (IQR: 2-10) sexual intercourse/month were reported and a median of 9.5 (IQR: 6-13) pills/month were used. Restricting the analysis to periods when participants reported at least one condomless sexual act yielded similar results with HIV incidence of 12.3/100 py in the placebo arm (6 infections, 48.8 py of FU) and 0/100 py in the TDF/FTC arm (0 infection, 54.3 py of FU, p=0.011).
Conclusions: On-demand PrEP with TDF/FTC remains highly effective in MSM having infrequent sexual intercourse.



|
| |
|
 |
 |
|
|