 |
 |
 |
| |
Under One Third of ID Fellows Think They Got Enough Training on ART or PrEP
|
| |
| |
IDWeek2017/IDSA, October 4-8, 2017, San Diego
Mark Mascolini
Fewer than one third of infectious diseases (ID) fellows attending a 2016 workshop reported believing they had adequate training in managing preexposure prophylaxis (PrEP) or guideline-directed antiretroviral therapy (ART) [1]. After the 8-hour workshop, 55% of the same fellows strongly agreed they felt comfortable in both areas.
Research indicates that internal medicine residents perceive they have inadequate HIV training, experience with HIV patients, and clinical HIV skills [2,3]. Because there are no comparable studies of ID fellows, researchers from the University of California, San Diego, and other centers surveyed ID fellows attending a workshop about their self-perceived adequacy in HIV-related experience and care.
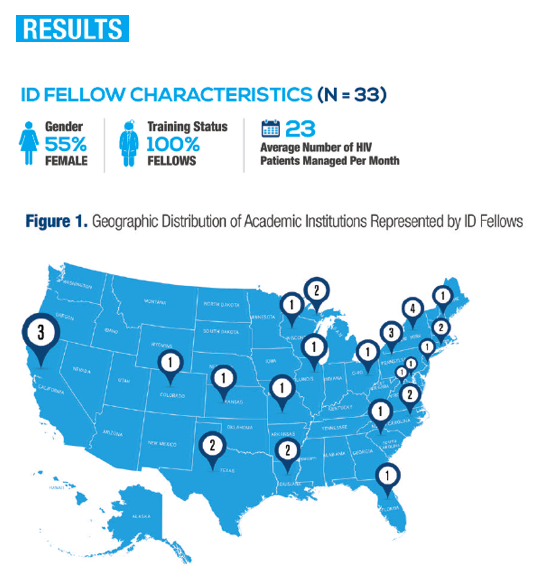
The analysis involved 33 ID fellows from across the country who were picked by their program directors to attend an 8-hour interactive workshop. Eighteen fellows (55%) were women, and the group averaged 23 HIV patients per month. Three HIV experts led the session, which involved case-based problem solving, interactive panel discussions, and question-and-answer sessions. Attending fellows completed surveys before and after the workshop.
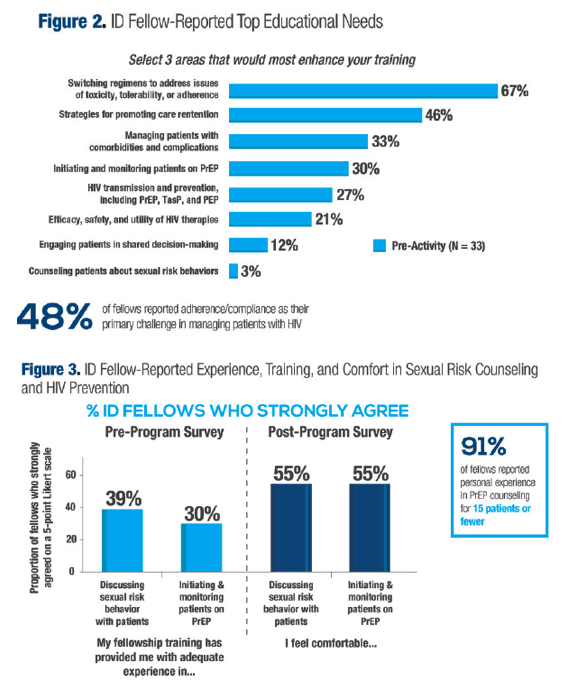
Before the workshop 67% of ID fellows reported their HIV training would be most improved by instruction in switching antiretroviral regimens to address toxicity, tolerability, or adherence, while 46% felt a need for more training in promoting retention in care. Almost half of the fellows, 48%, reported promoting antiretroviral adherence as their primary challenge in managing people with HIV. One third of fellows felt a need for more instruction on managing HIV-related comorbidities and complications, and 27% felt poorly prepared on HIV transmission and prevention, including PrEP, treatment as prevention, and postexposure prophylaxis.
In the survey before the workshop, 39% of ID fellows strongly agreed that their fellowship training provided inadequate experience in discussing sexual risk behavior with patients, while 30% felt inadequate training in starting and monitoring patients on PrEP. Thirty fellows (91%) noted they had experience in PrEP counseling with 15 or fewer patients. After the workshop, 55% of fellows felt comfortable discussing sexual risk and 55% felt prepared to prescribe and monitor PrEP.
Half of participants (51%) reported personal experience in starting and monitoring ART for 15 or fewer patients. Before the workshop only 22% of attendees strongly agreed that their fellowship training offered adequate experience in starting guideline-directed ART, 22% felt the same about experience in planning individualized ART, and 9% felt they had adequate training on drug-drug interactions. After the workshop, proportions who strongly agreed they felt comfortable in those three areas were 55%, 45%, and 21%.
The researchers concluded that ID fellows feel they lack experience in counseling patients about sexual health, starting and monitoring PrEP, and prescribing ART. But a 1-day intensive interactive workshop improved their comfort level in these aspects of HIV care.
References
1. Hicks C, MD1, Johnson SC, Daar E, Heggen-Peay C, Sapir T, Moreo K. HIV/AIDS training and skills of infectious disease fellows among 33 US academic institutions. IDWeek2017/IDSA. October 4-8, 2017. San Diego. Abstract 1444.
2. Phillips KA, Cofrancesco J Jr, Sisson S, Wu AW, Bass EB, Berkenblit G. A multicenter study of internal medicine residents' perceptions of training, competence, and performance in outpatient HIV care. AIDS Patient Care STDS. 2010;24:159-164.
3. Adams J, Chacko K, Guiton G, Aagaard E. Training internal medicine residents in outpatient HIV care: a survey of program directors. J Gen Intern Med. 2010;25:977-981.



|
| |
|
 |
 |
|
|