 |
 |
 |
| |
Direct Antiviral Agents after Successfully Treated Early Hepatocellular Carcinoma Improve Survival in Cirrhotic Patients with Chronic Hepatitis C
|
| |
| |
Reported by Jules Levin
AASLD 2018 Nov 9-13 SF

program abstract
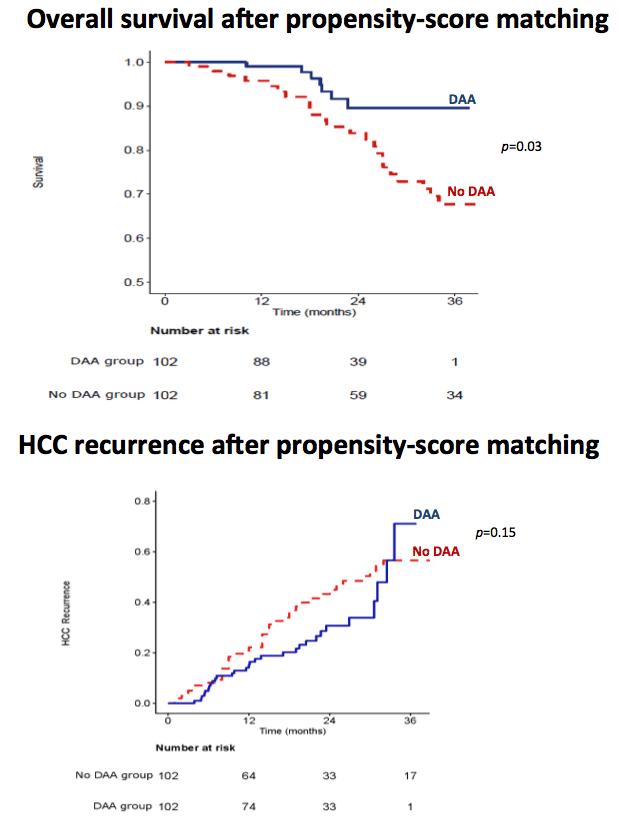
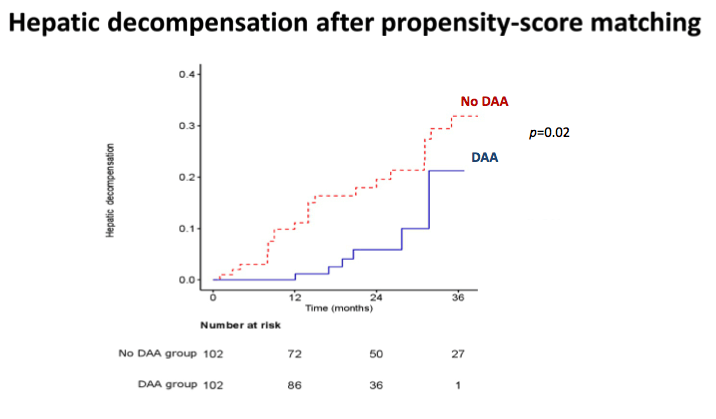
Background: The benefit of direct-acting antiviral agents (DAAs) against hepatitis C virus (HCV) after successfully treated early hepatocellular carcinoma (HCC) has been extensively studied, but impact on overall survival (OS) is unknown despite a reduction in the rate of HCC recurrence. Our aim was to assess if sustained virological response (SVR) by DAAs is effective in the reduction of overall mortality and in the prevention of HCC recurrence in patients with HCV cirrhosis and previously treated HCC.
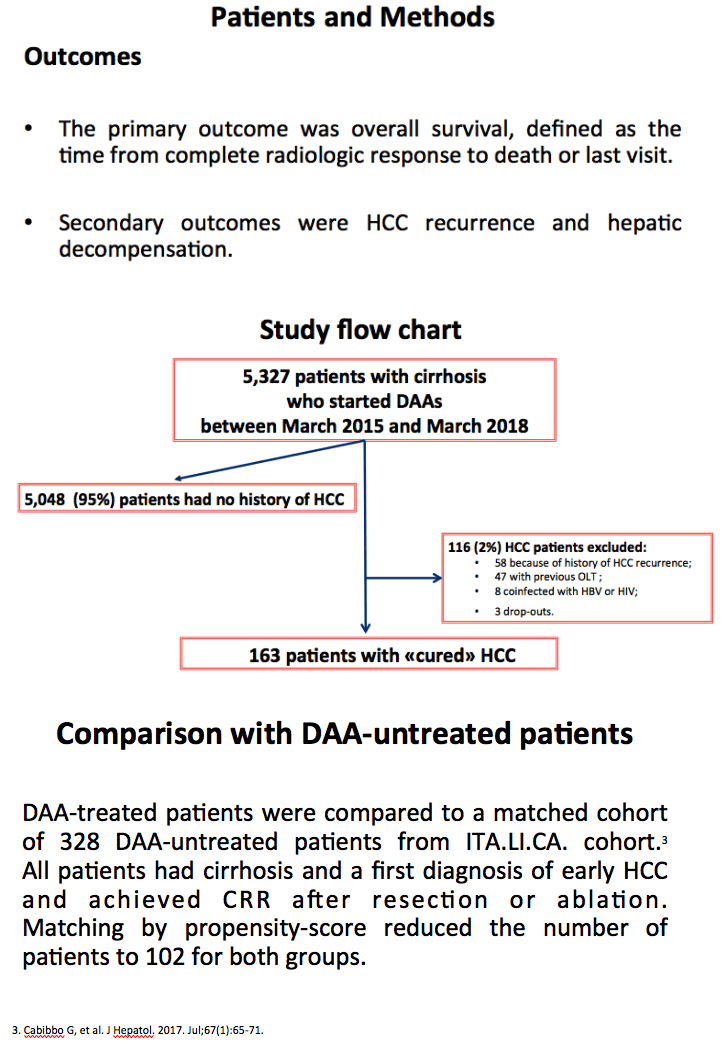
Methods: We prospectively enrolled 221 consecutive HCV patients with a first diagnosis of early (Barcelona Clinic Liver Cancer 0/A) HCC achieving complete radiological response after curative resection or ablation and subsequently treated with DAAs. All patients were monitored by web based RESIST-HCV network. Clinical, virological and radiological data were collected before DAAs start and during follow-up. Kaplan-Meier method was performed to assess the primary endpoint: probability of OS from DAAs starting and the secondary end point: time to HCC recurrence (TTR). Predictors of OS were established by Cox regression multivariate analysis.
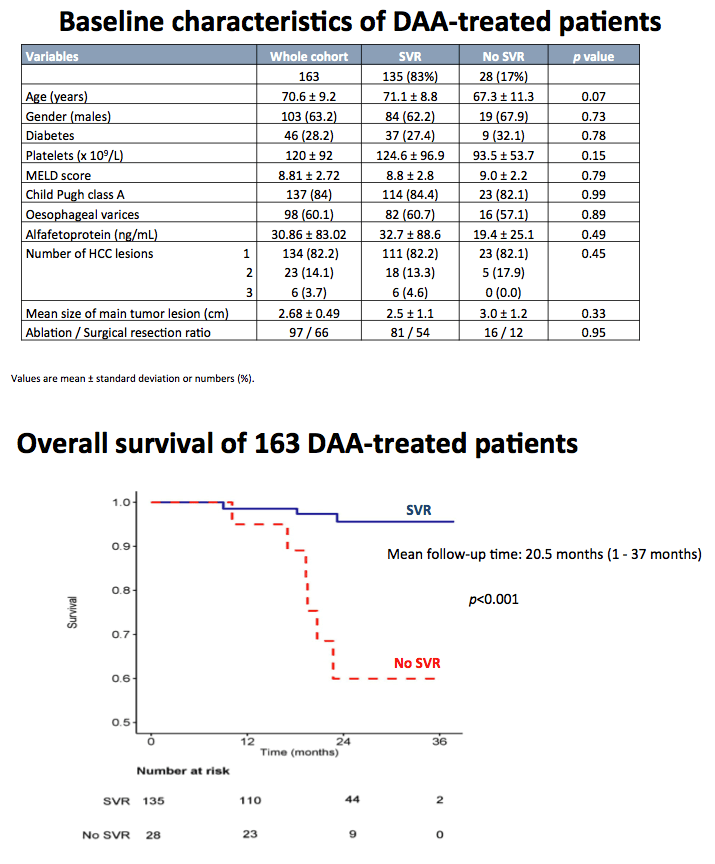
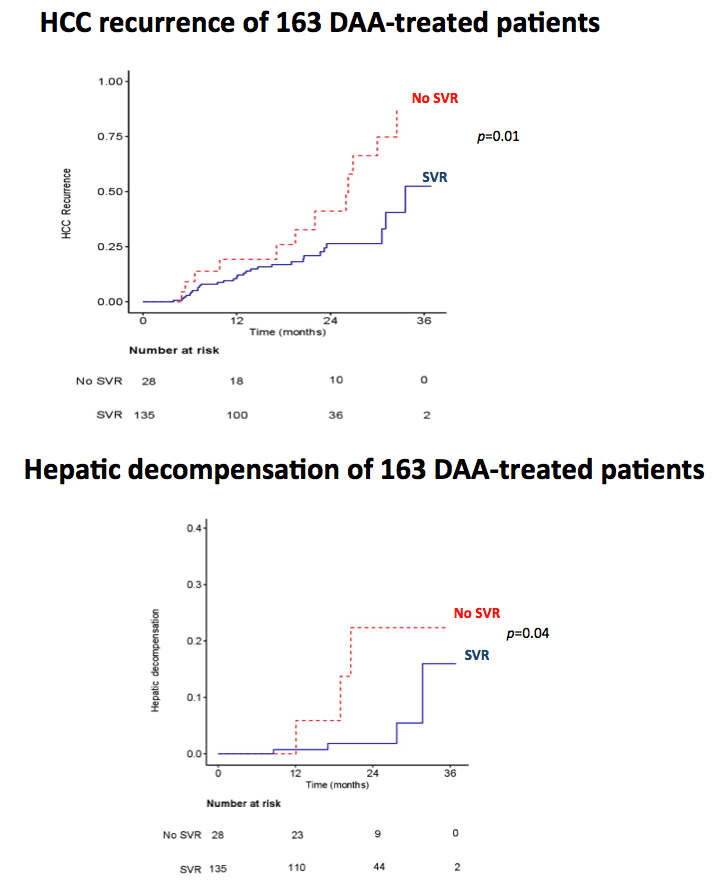
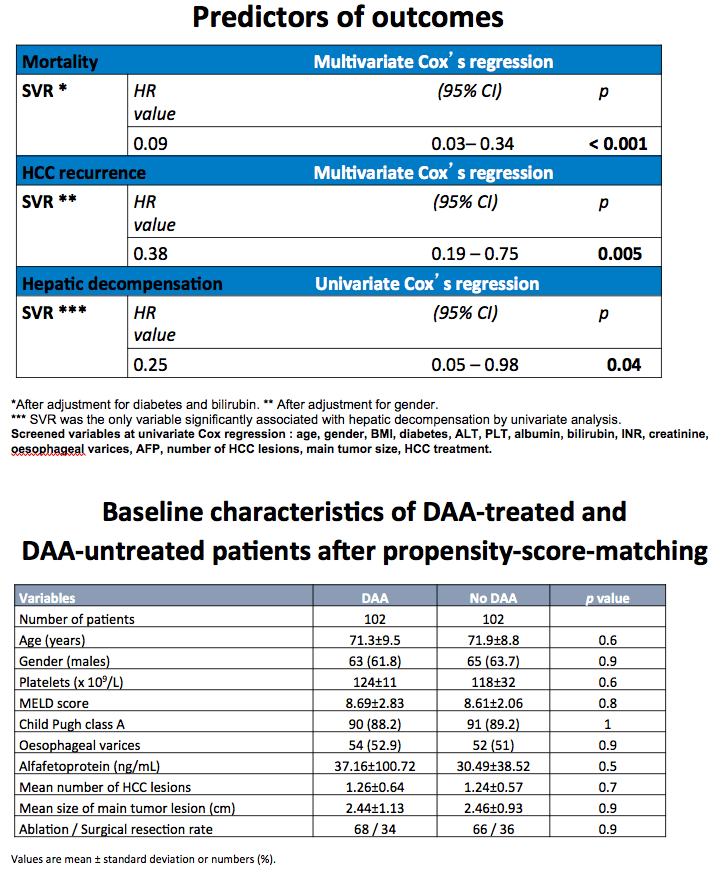
Results: Eighty-six per cent of patients were in Child-Pugh class A and 76% of patients were BCLC A. The median time-lag between HCC complete radiological response and DAAs starting was 1.7 months (range: 0.5-5.5) and the median length of follow-up after DAAs starting was 17 months (range 1-34) for the entire group. SVR was achieved in 188 patients (85%) by intention-to-treat analyses. Fifty-two HCC recurrences were observed, with nodular or infiltrative pattern in 83% and 17% of patients, respectively. Eleven patients (5%) died. Actuarial OS rates were 97.6% at 1 years and 92.9% at 2 years. Actuarial HCC recurrence rates were 7.6% at 6 months, 18% at 1 year, 34.5% at 2 years. The SVR group had significantly longer OS (p<0.0001) and TTR (p=0.008) than the no-SVR group by Kaplan-Meier analyses. SVR (hazard ratio [HR]=0.17; 95% Confidence Interval [CI]=0.05-0.58) and albumin level (HR=0.30; 95% CI=0.10-0.92) were independent predictors of OS. SVR (HR=0.48; 95% CI=0.25-0.91) was the only variable independently associated with TTR.
Conclusion: Our analysis demonstrated for the first time by multivariate analysis that in patients with HCV cirrhosis and successfully treated early HCC, SVR achieved by DAAs improves OS and reduces the risk of HCC recurrence.


|
| |
|
 |
 |
|
|