 |
 |
 |
| |
DETERMINANTS OF HIV-1 RESERVOIR SIZE AND
LONG-TERM DYNAMICS UNDER SUPPRESSIVE ART
|
| |
| |
Initial HIV Load, Blips Are Strong Drivers of HIV DNA Reservoir Size
25th Conference on Retroviruses and Opportunistic Infections (CROI), March 4-7, 2018, Boston
Mark Mascolini
Starting antiretroviral therapy (ART) during acute HIV infection, shorter time to viral suppression, and other factors predicted initial size of the HIV DNA reservoir in a study of 1078 successfully treated people in Switzerland [1]. Viral blips strongly predicted both initial reservoir size and decay.
Impervious to ART that controls viral replication in plasma, HIV reservoirs pose a substantial challenge to any HIV cure strategy. Nadine Bachmann (University Hospital Zurich) and colleagues analyzed HIV DNA levels to isolate predictors of the initial size of that reservoir 1.5 years after treatment began and subsequent reservoir decay in the following 1.5 to 5.5 years.
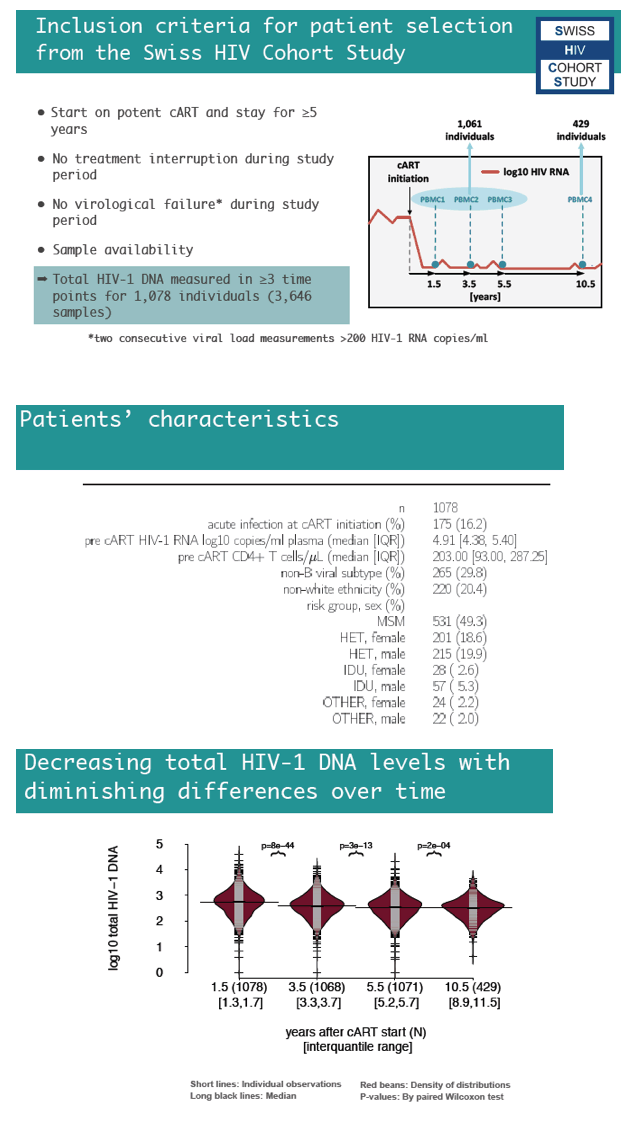
The Swiss team used total HIV DNA as a surrogate for the viral reservoir. They focused on members of the Swiss HIV Cohort Study (SHCS) who started a potent antiretroviral regimen and stayed on treatment for at least 5 years with no interruption. During that time, no one had virologic failure, defined as consecutive viral loads above 200 copies. The investigators measured total HIV DNA 3 or more times in 3646 samples from 1078 people.
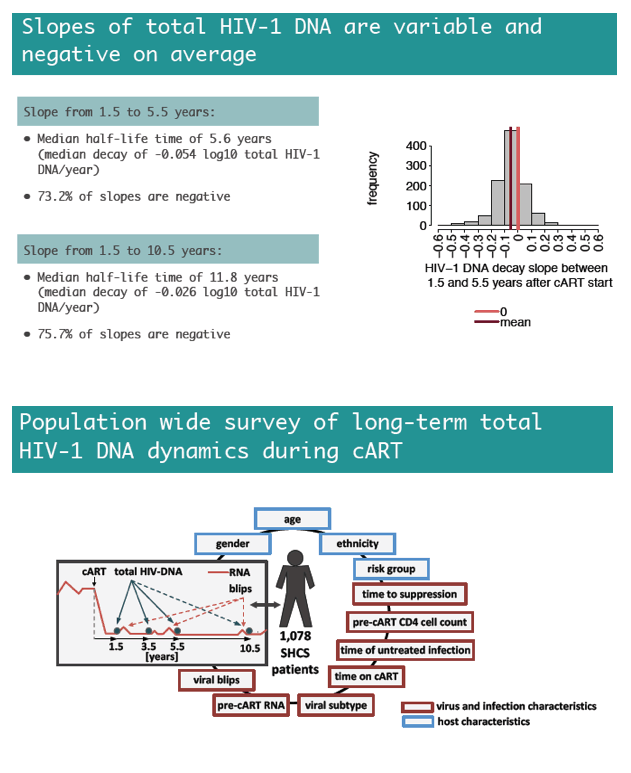
The study population included 175 people (16%) who started ART during acute infection. Median pretreatment viral load for the whole group stood at 4.91 log10 copies, or about 81,000 copies. Median pre-ART CD4 count measured 203. While 30% of participants had a non-B HIV-1 subtype, 20% were nonwhite. Average total HIV DNA levels fell significantly across the four intervals assessed--1.5, 3.5, 5.5, and 10.5 years after ART began. From 1.5 to 5.5 years after ART began, median HIV DNA decay measured -0.054 log10 copies per year, and 73.2% of participants had negative slopes. From 1.5 to 10.5 years, median decay slowed to -0.026 log10 copies per year, and 75.7% of participants had negative slopes.
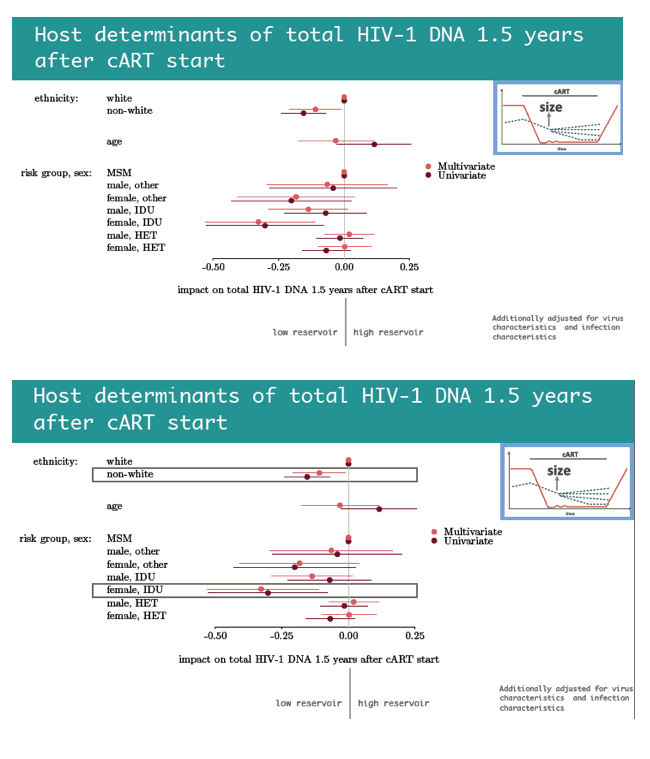
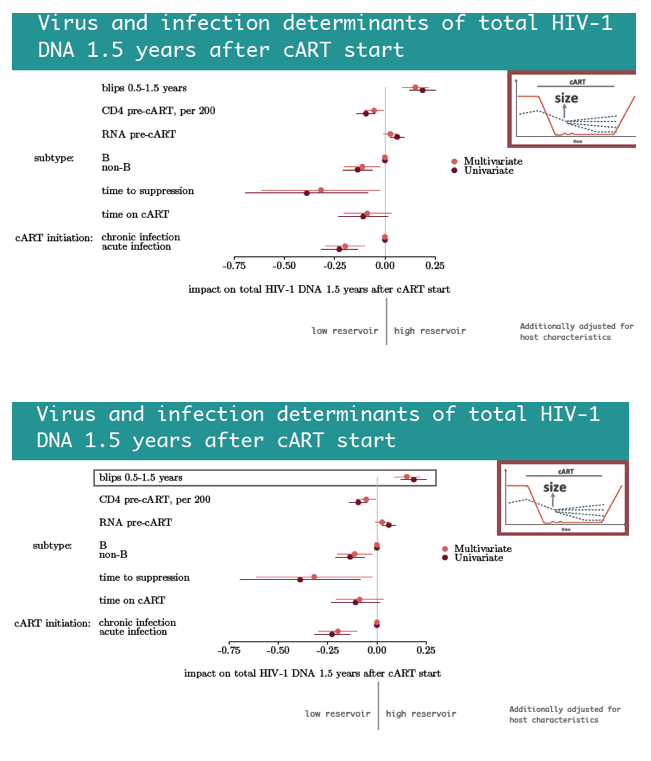
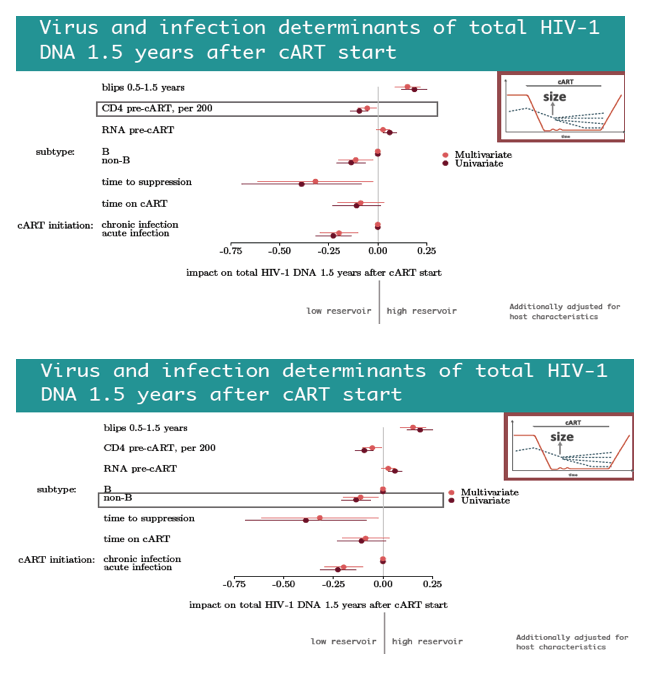
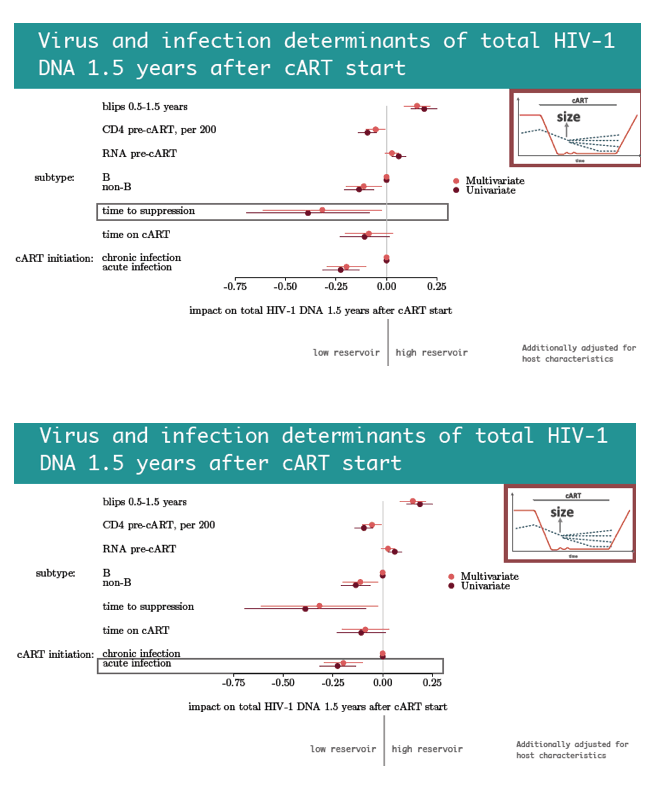
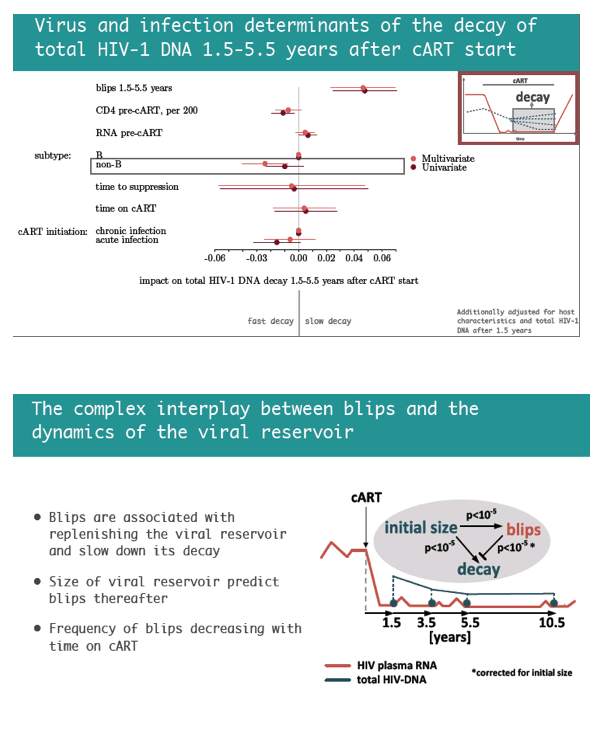
Two host variables independently predicted lower versus higher HIV DNA reservoirs 1.5 years after ART began: nonwhite ethnicity and being a woman who acquired HIV while injecting drugs. Four viral factors independently predicted a lower reservoir 1.5 years after ART began--every 200-cell higher pre-ART CD4 count, infection with a non-B HIV-1 subtype, shorter time to viral suppression in plasma, and starting ART during acute versus chronic infection. In contrast, viral blips in the first 0.5 to 1.5 years of ART predicted a bigger HIV DNA reservoir.
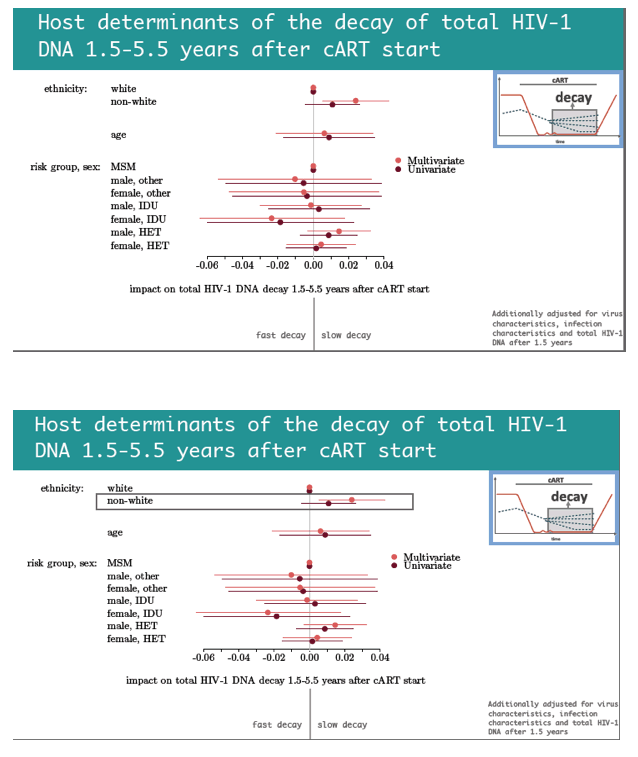
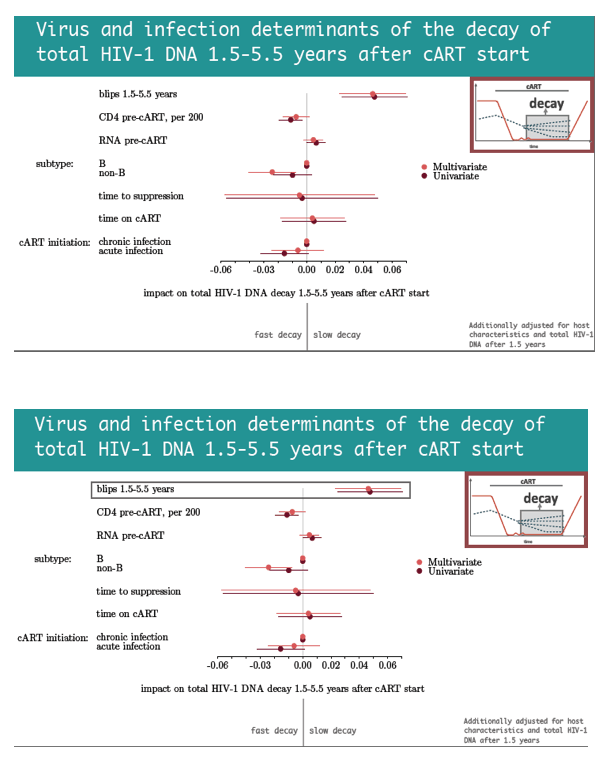
Next the researchers identified factors associated with fast versus slow HIV DNA decay in the 1.5 to 5.5 years after treatment began. Among host variables only nonwhite ethnicity independently predicted slow decay, while no factors predicted fast decay. Among viral factors, blips 1.5 to 5.5 years after ART began strongly predicted slow HIV DNA decay, whereas infection with non-B subtype HIV-1 independently predicted fast decay.
Bachmann and colleagues stressed that even in this efficiently treated population, one quarter of participants had a flat or positive HIV DNA decay slope. In other words, this viral reservoir did not diminish over time in some people--and sometimes grew larger--despite HIV suppression in plasma.
In the first 1.5 years after ART began, starting ART during acute infection, faster time to viral suppression in plasma, higher pre-ART CD4 count, a non-B subtype, nonwhite ethnicity, and being a woman who injected drugs were associated with low total HIV DNA levels. Viral blips predicted both high total HIV DNA levels 1.5 years after ART began and slower subsequent decay of the HIV DNA reservoir. The researchers believe these last findings add to evidence indicating the biological relevance of blips, which thus "may have implications for cure research."
In the question-and-answer session after the presentation, Daniel Kuritzkes (Harvard Medical School) and others questioned the validity of using total HIV DNA as a reservoir surrogate because total DNA contains defective virus. Bachmann answered that associations between HIV-related factors and reservoir size--all going in the expected direction--argue for the validity of using HIV DNA.
Reference
1. Bachmann N, von Siebenthal C, Vongrad V, et al. Determinants of HIV-1 reservoir size and long-term dynamics under suppressive art. 25th Conference on Retroviruses and Opportunistic Infections (CROI). March 4-7, 2018. Boston. Abstract 69LB.
WEBCAST: http://www.croiwebcasts.org/console/player/37084?mediaType=slideVideo&&crd_fl=1&ssmsrq=1521308193021&ctms=5000&csmsrq=813
CROI: No Evidence of Residual Virus Replication in a Randomised Controlled Trial of Dolutegravir Intensification - (03/07/18)


|
| |
|
 |
 |
|
|