 |
 |
 |
| |
QUANTIFICATION OF REPLICATION COMPETENT LATENT HIV-1 IN GALT AND SEMEN
|
| |
| |
New Assay Sometimes Sees More Latent HIV in Rectal Tissue and Semen Than in Blood
25th Conference on Retroviruses and Opportunistic Infections (CROI), March 4-7, 2018, Boston
Mark Mascolini
Using a new assay to measure replication-competent latent HIV, University of Pittsburgh researchers found higher levels in rectal tissue and semen than in blood in some people [1]. In other people, levels of latent HIV were lower in rectal tissue than in blood but still detectable. The findings add to evidence that potentially active HIV hides throughout tissues and body fluids.
Much research has explored the latent replication-competent HIV reservoir--an imposing obstacle to HIV cure--in resting CD4 cells. But few studies have tried to size up this reservoir in tissues for two reasons: (1) current assays have limited sensitivity in detecting latent HIV in tissue, and (2) gathering enough viable mononuclear cells has proved difficult.
The University of Pittsburgh team has crafted a reporter cell-based assay that measures inducible, replication-competent latent HIV-1 in blood [2]. This assay, dubbed TZA, has proved sensitive and rapid in quantifying latent HIV-1 in only a small volume of blood. The work presented at CROI detailed this groups' effort to adapt TZA to measuring replication-competent HIV in gut-associated lymphoid tissue (GALT) and semen of people with antiretroviral-induced viral suppression in plasma.
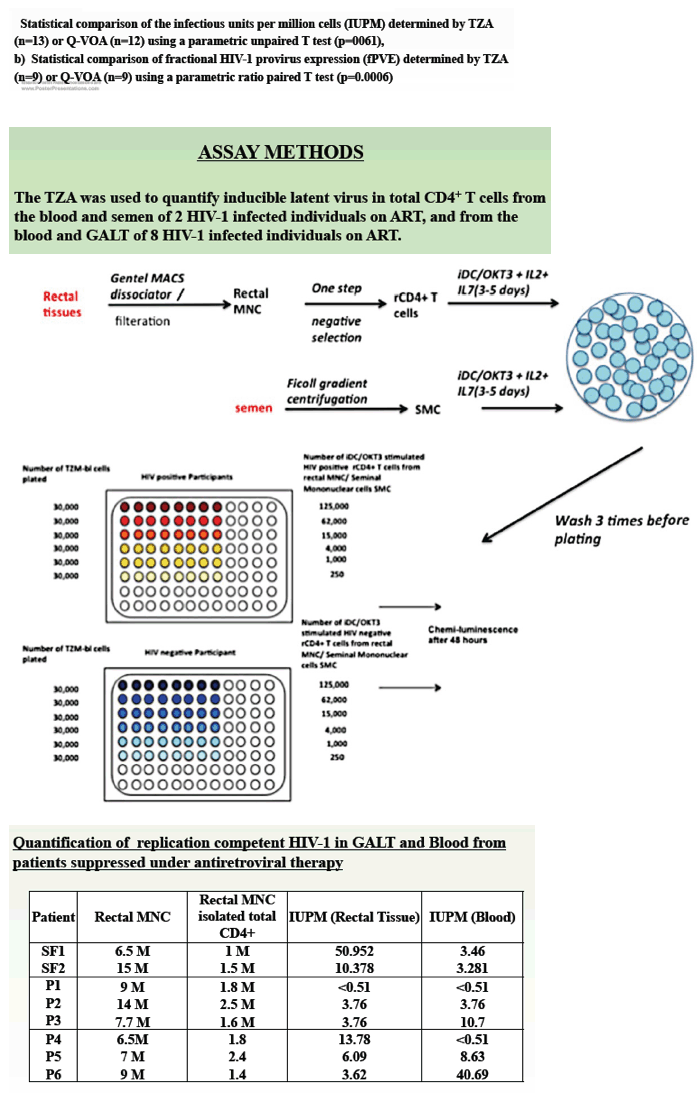
The Pittsburgh investigators used the MACS Octo Dissociator to isolate mononuclear cells from GALT. Their GALT analysis focused on rectal tissue from 8 people on suppressive antiretroviral therapy whose rectal mononuclear cell samples ranged from 1 million to 2.5 million CD4 cells. One of the 8 participants had HIV levels, measured as infectious units per million cells (IUPM), below 0.51 in both rectal tissue and blood, while another had the same level in tissue and blood (3.76 IUPM). Three people had lower HIV IUPM in rectal tissue than in blood (3.76 versus 10.7 IUPM, 6.09 versus 8.63 IUPM, and 3.62 versus 40.69 IUPM). The remaining 3 people had substantially higher levels of replication-competent HIV in rectal tissue than in blood (13.78 versus <0.51 IUPM, 10.378 versus 3.281 IUPM, and 50.952 versus 3.46 IUPM).
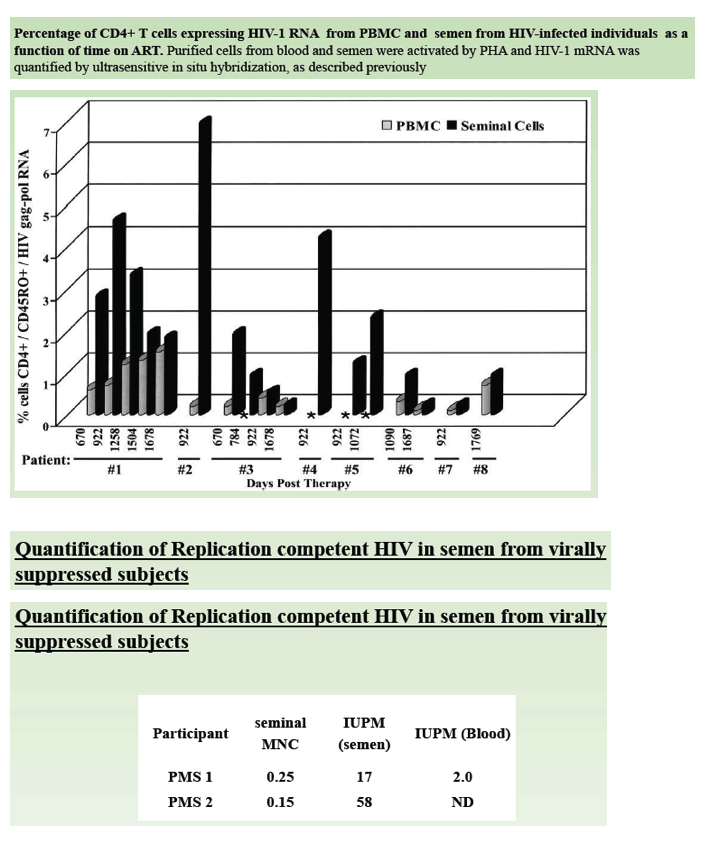
Two virally suppressed men gave semen samples to measure replication-competent HIV. One man had undetectable levels in blood and 58 IUPM in semen. The other had 2 IUPM in blood and 17 IUPM in semen.
These early results suggest a sometimes higher frequency of latent HIV in rectal tissue and semen than in blood of antiretroviral-treated people with an undetectable viral load in plasma. All told, latent HIV could be measured in 9 of 10 rectal tissue or semen samples. The researchers believe they successfully adapted the TZA assay to measure inducible replication-competent HIV in rectal tissue and semen.
References
1. Sanyal A, McGowan I, Somsouk M, Rinaldo C, Sluis-Cremer N, Gupta P. Quantification of replication competent latent HIV-1 in GALT and semen. 25th Conference on Retroviruses and Opportunistic Infections (CROI). March 4-7, 2018. Boston. Abstract 399.
2. Sanyal A, Mailliard RB, Rinaldo CR, et al. Novel assay reveals a large, inducible, replication-competent HIV-1 reservoir in resting CD4+ T cells. Nat Med. 2017;23:885-889. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5505781/

1Department of Infectious Diseases and Microbiology, Graduate School of Public Health and School of Medicine, University of Pittsburgh; 2Division of Gastroenterology, Hepatology, and Nutrition, Department of Medicine, University of Pittsburgh School of Medicine; 3Department of Medicine, University of California at San Francisco; 4Division of Infectious Diseases, Department of Medicine, University of Pittsburgh School of Medicine

Program Abstract:
The latent replication-competent HIV-1 reservoir represents a major obstacle to a cure. This reservoir has been well-characterized in resting CD4+ (rCD4+) T cells in blood. However, few studies have quantified the frequency of replication-competent latent HIV-1 in tissue, primarily due to the limitation of the sensitivity of current assays. We recently developed a reporter cell-based assay to quantify inducible, replication-competent latent HIV-1 in the blood (Sanyal et al., Nat. Med. 2017. 23:885) which is sensitive, requires only a small blood volume, and is less labor intensive than other available technologies. The goal of this study was to adapt this assay (termed TZA) to quantify replication competent HIV-1 in GALT and semen from virally suppressed individuals.
The TZA was adapted to quantify inducible replication-competent HIV-1 in tissue samples. Using this assay, we quantified inducible latent virus in total CD4+ T cells from the blood and semen of 2 infected individuals on ART, and from the blood and GALT of 6 infected individuals on ART.
We routinely isolated 2-3×106 CD4+ T cells of high purity from rectal tissue using the gentleMACSTM Octo Dissociator (Miltenyi). We found in 6 patients that there was more replication competent HIV-1 in the GALT than in the blood. The mean IUPM value for blood was determined to be 3.5 (range: 0.5 -3.76); whereas the mean IUPM value for tissue was 16.2 (range 0.5-51). Interestingly, we also observed more replication competent HIV-1 in the semen compared to blood. In one subject tested, the IUPM value was calculated to be 2.0 and 17.0 in the blood and semen, respectively. In the second subject, infectious virus could not be recovered from the blood, but an IUPM of 58.0 was determined in the semen.
We have adapted the TZA to quantify inducible replication-competent HIV-1 in the GALT and semen of HIV-1 infected subjects on ART. Preliminary studies suggest a higher frequency of HIV in both GALT and semen compared to blood.
|
| |
|
 |
 |
|
|