 |
 |
 |
| |
Factors Impacting Appropriate HIV/STI Screening and PrEP Persistence in Primary Care in SF
|
| |
| |
Reported by Jules Levin
CROI 2018 March 4-7 Boston MA
Matthew A. Spinelli1; Hyman Scott1,2; Eric Vittinghoff1; Albert Y. Liu1,2; Alicia Morehead-Gee1; Rafael Gonzalez2; Monica Gandhi1; Susan P. Buchbinder1,2
1University of California, San Francisco; 2San Francisco Department of Public Health Funding: This project was supported by NIMH Grant # R01MH109320


Program Abstract:
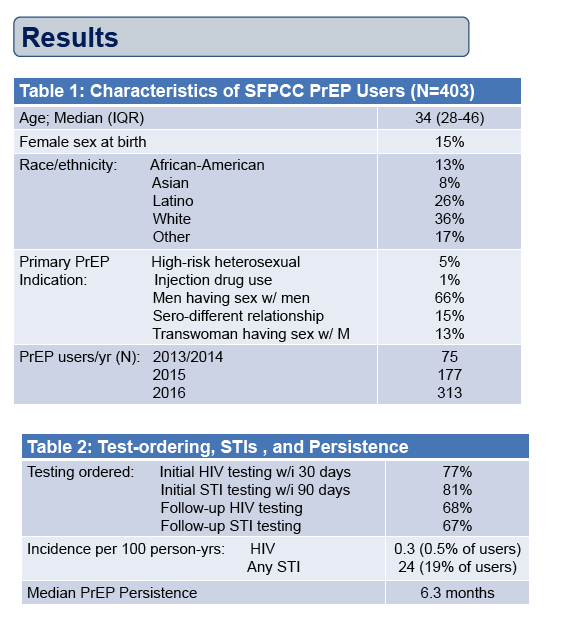
Given increasing PrEP uptake, to optimize PrEP safety and impact, persons at HIV-risk must have appropriate HIV/STI testing and persist on PrEP. We evaluated patient and provider characteristics associated with HIV/STI testing and PrEP persistence in the San Francisco Public Health Primary Care Clinics (SFPCC).
Demographic, lab, and prescription data were abstracted from charts of SFPCC PrEP users from 3/1/13-7/31/17. Multivariable logistic regression models assessed factors associated with lack of appropriate HIV/STI testing at PrEP initiation defined as HIV testing 30 days prior, and rectal, pharyngeal, urine, or vaginal gonococcus (GC) or C. trachomatis (CT) testing 90 days prior to or 7 days after initial prescription, respectively. We examined factors associated with PrEP persistence (number of days with an active prescription) using a Cox proportional-hazards model, defining discontinuation as 90 days without an active prescription.
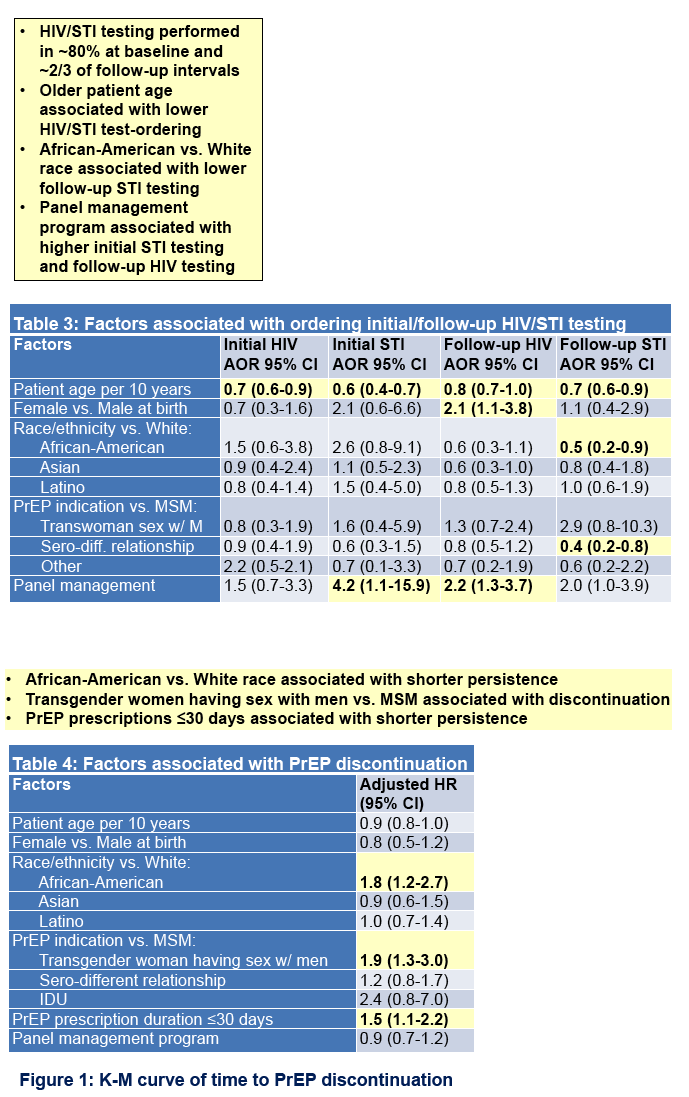
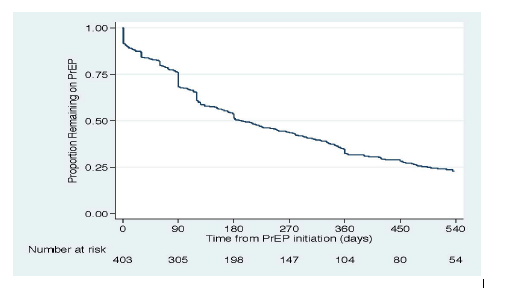
Overall, 401 PrEP patients had pharmacy and lab data available. Mean age was 37 years; 85% were male; 8% Asian, 13% Black, 26% Latino, and 36% White. PrEP prescriptions increased each year, from 108 patients in 2013/4 to 913 in 2016/7. PrEP panel size was 1, 2-5, or >5 for 19%, 32% and 49% of providers, respectively. Only 76% of patients received an HIV antibody test ≤30 days prior to PrEP initiation: 61% in 2013/14 and 83% in 2016/17. Lack of a baseline HIV test was associated with older age (p=0.01) and earlier prescription year (p=0.001 for trend). Among patients on PrEP for ≥6 months, 70% had follow-up HIV testing at least every 6 months. Only 71% received any baseline testing for GC or CT; lack of testing was also associated with older age (p<0.001) and earlier year (p<0.001 for trend). Median PrEP persistence was 11.3 months. In multivariable analysis, shorter persistence was associated with young age, Black race, earlier PrEP prescription index number, larger provider PrEP panel size, and current prescription of ≤30 pills (Table).
SFPCC PrEP users are a diverse and growing population cared for by both high and low volume providers. Short duration prescriptions were associated with worse persistence, and may be a barrier for PrEP users. Appropriate HIV/STI screening is suboptimal but improving with time, possibly related to SFPCC PrEP education initiatives. Strategies to address provider and patient barriers to appropriate HIV/STI screening and PrEP persistence are needed.

|
| |
|
 |
 |
|
|