 |
 |
 |
| |
HIV Linked to Higher Risk of Coronary Plaque Progression in MACS Men: "HIV Infection is Associated with Progression of Coronary Plaque: The MACS Longitudinal Coronary CT Angiography Study"
|
| |
| |
25th Conference on Retroviruses and Opportunistic Infections (CROI), March 4-7, 2018, Boston
Mark Mascolini
WEBCAST: http://www.croiwebcasts.org/console/player/37176?mediaType=slideVideo&&crd_fl=1&ssmsrq=1520618936707&ctms=5000&csmsrq=963
HIV-positive men in the Multicenter AIDS Cohort Study (MACS) ran a higher risk of coronary artery plaque progression than their HIV-negative MACS counterparts in a 555-man analysis [1]. Heightened progression risk with HIV held true for both calcified plaque and the more dangerous noncalcified plaque.
Wendy Post (Johns Hopkins University) and MACS collaborators at other centers previously reported that MACS men with HIV had a greater prevalence and extent of coronary atherosclerotic plaque than HIV-negative MACS men, demonstrated by coronary CT angiography [2]. But research had not explored potential associations between HIV and coronary plaque progression.
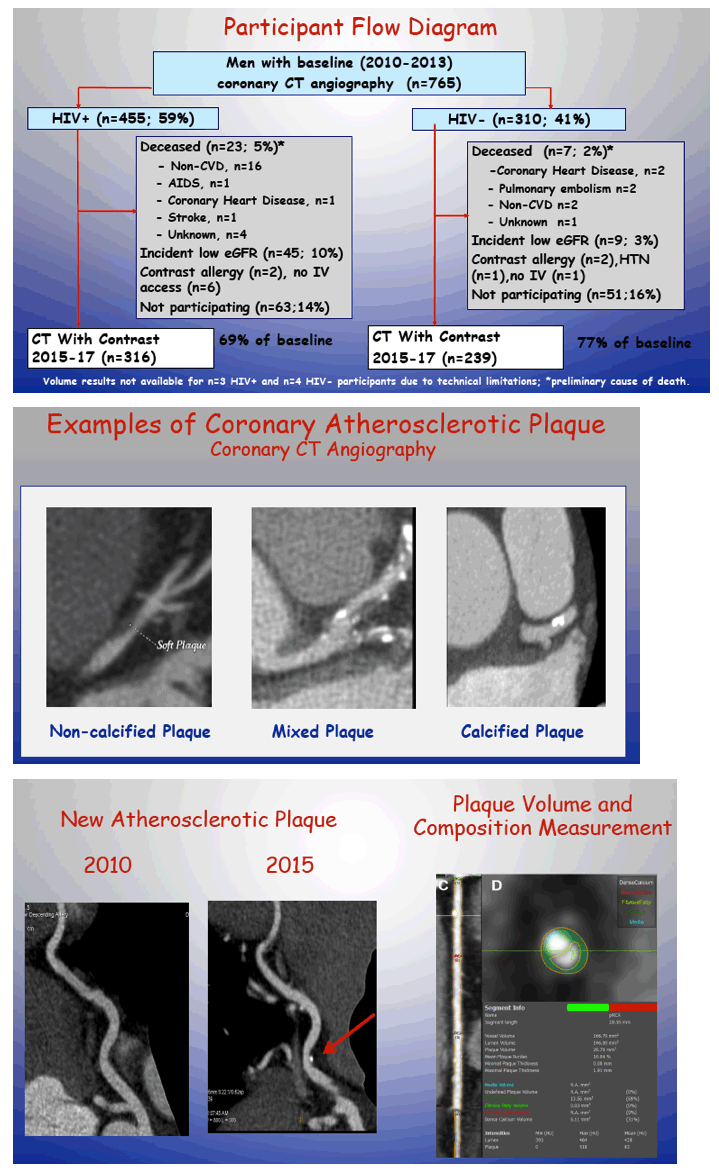
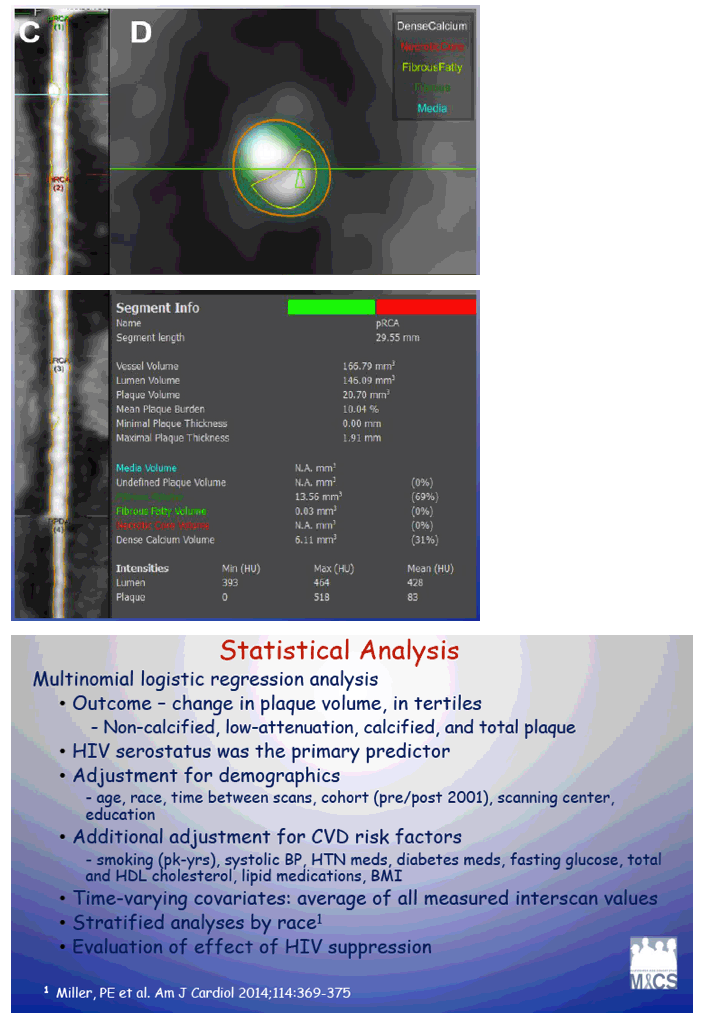
In 1984 MACS began enrolling HIV-positive gay or bisexual men and HIV-negative men at risk for HIV infection. The MACS Cardiovascular Study considered 40- to 70-year-old men with no previous cardiac surgery or coronary artery angioplasty or stent. The analysis involved 316 men with HIV and 239 without HIV who had coronary artery CT with contrast. The MACS investigators used multinomial logistic regression to explore the impact of HIV status on change in plaque volume over time after statistical adjustment for demographics and cardiovascular risk factors.
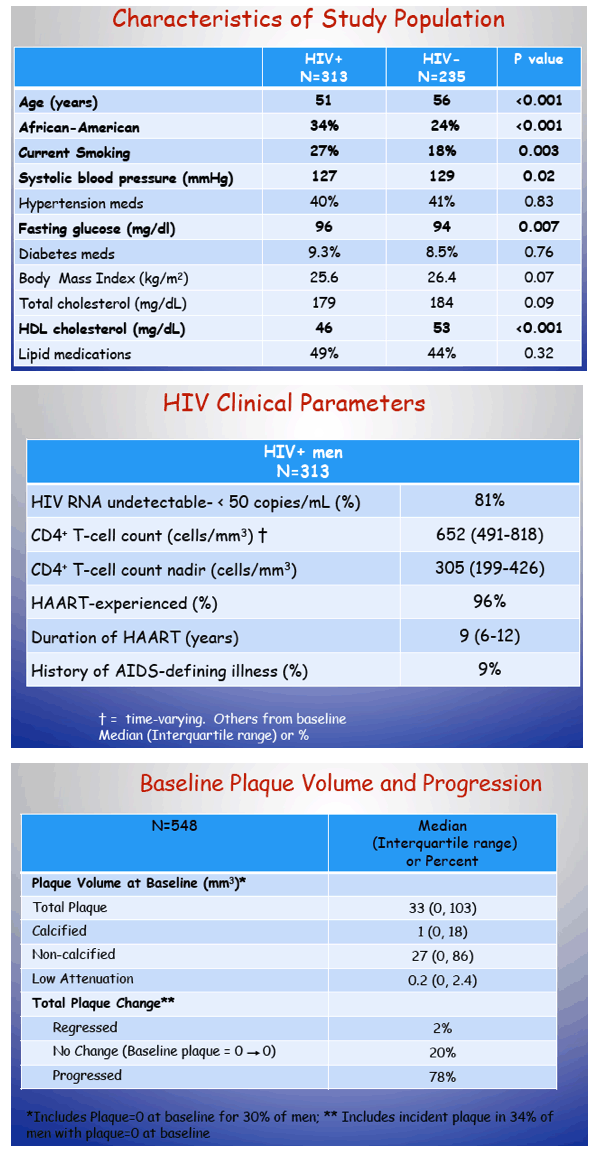
Compared with HIV-negative men, the HIV group was younger (median 51 versus 56, P < 0.001), had a higher proportion of blacks (34% versus 24%, P < 0.001), and had a higher proportion of current smokers (27% versus 18%, P = 0.003). Men with HIV had lower systolic blood pressure, higher fasting glucose, and lower "good" high-density lipoprotein cholesterol (46 versus 53 mg/dL, P < 0.001). Men with HIV had taken antiretroviral therapy for a median of 9 years, and 81% had a viral load below 50 copies.
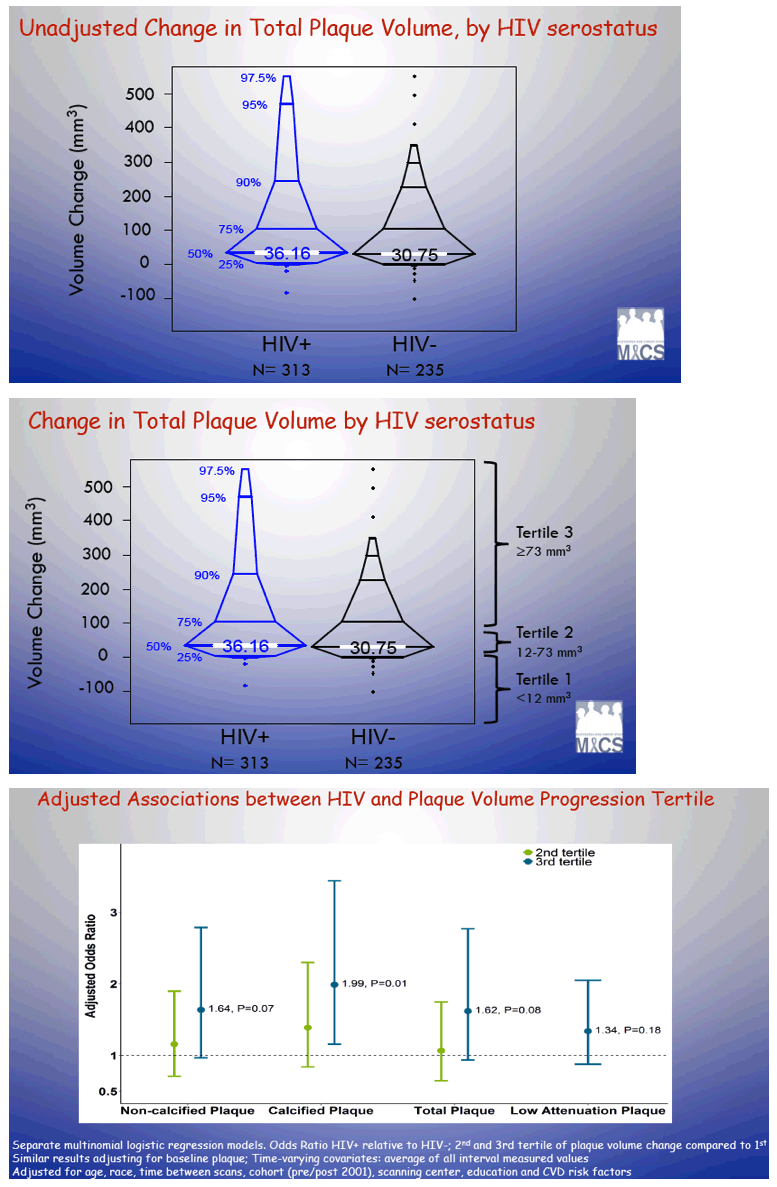
All men had two coronary artery CTs. Median plaque volume at the baseline assessment was 33 mm(3) for all plaques and 27 mm(3) for dangerous noncalcified plaque. During a median follow-up of 4.5 years, plaque volume progressed in 78% of plaques, did not change in 20%, and regressed in 2%. Through follow-up median plaque volume rose 36.16 mm(3) in men with HIV and 30.75 mm(3) in men without HIV.
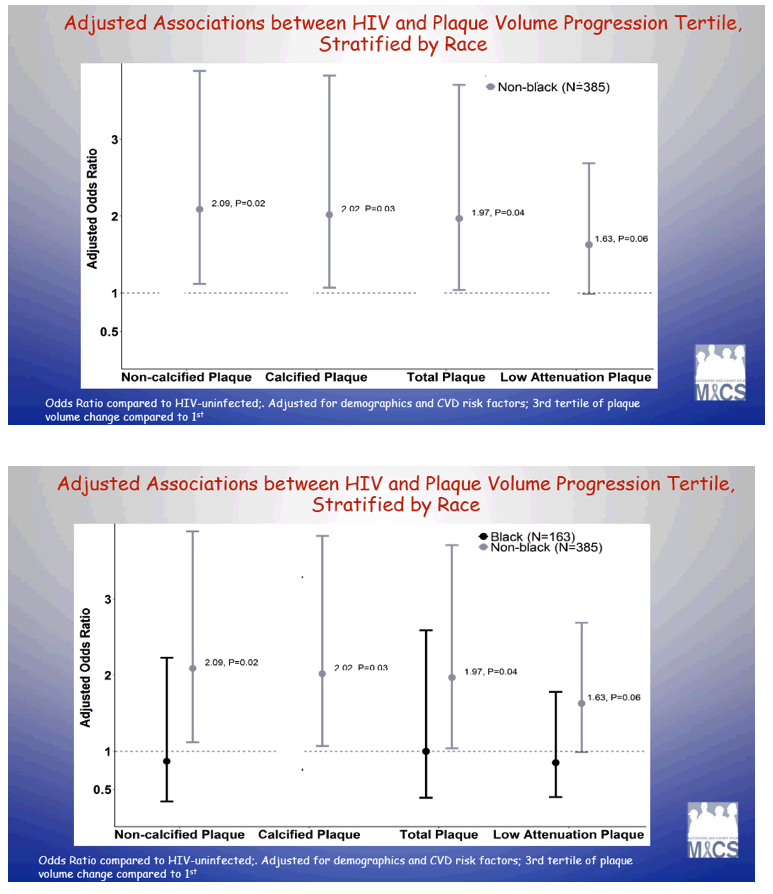
Comparing the third (highest) tertile of plaque progression with the first (lowest) tertile, adjusted analysis indicated doubled odds of plaque volume progression in men with calcified plaque (OR 1.99, P = 0.01). The association was smaller and nearly significant for noncalcified plaque (OR 1.64, P = 0.07) and total plaque (OR 1.62, P = 0.08).
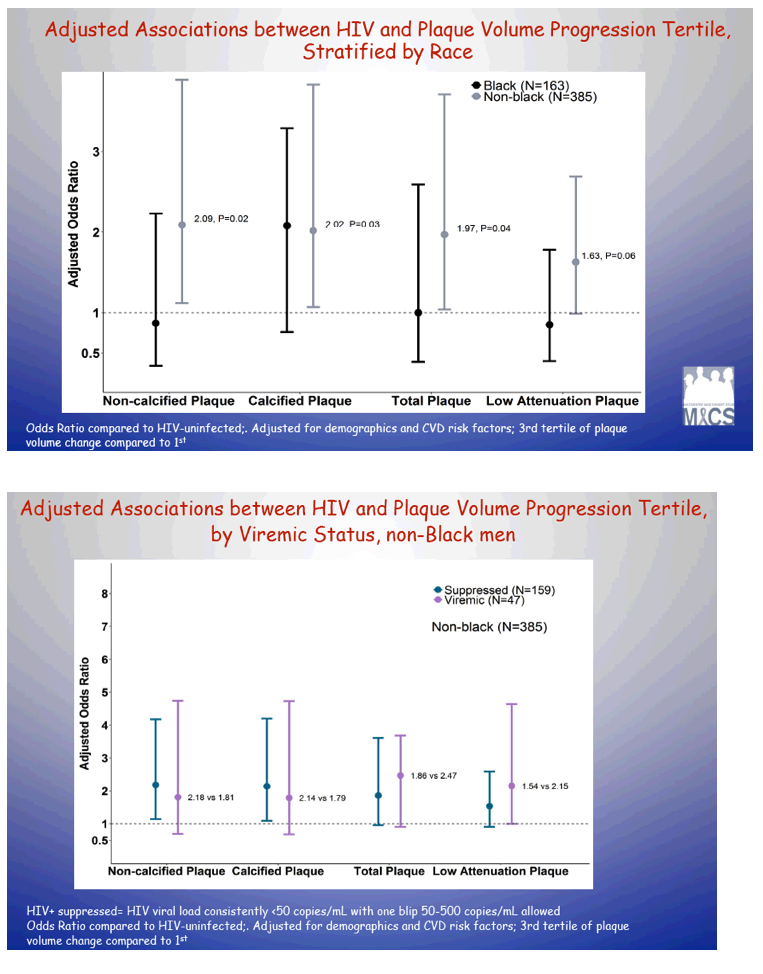
Adjusted analysis limited to nonblack men linked HIV to a near doubling of total plaque progression (odds ratio [OR] 1.97, P = 0.04). The association between HIV status and greater odds of progression was similar for noncalcified plaque (OR 2.09, P = 0.02) and calcified plaque (OR 2.02, P = 0.03), but weaker for low-attenuation plaque (OR 1.63, P = 0.06). None of these associations held true in black men. Among nonblack men, plaque progression was similar in men with and without HIV suppression. CD4-cell nadir and time on ART did not predict plaque progression.
Post and MACS colleagues concluded that coronary atherosclerotic plaque volume progression is greater in men with HIV than in sociodemographically similar men without HIV. The finding held true for both calcified plaque and noncalcified plaque in this largest study of plaque progression with HIV to date. The investigators suggested that the racial difference seen (plaque progression risk in nonblacks but not blacks) could reflect environmental and lifestyle factors, biologic differences, or genetic susceptibilities.
The MACS team cautioned that "predictors of subclinical coronary artery plaque progression may differ from predictors of myocardial infarction and other cardiovascular events." They called for additional studies to confirm these findings in women with HIV and other groups.
References
1. Post W, Haberlen S, Zhang L, et al. HIV infection is associated with progression of high risk coronary plaque in the MACS. 25th Conference on Retroviruses and Opportunistic Infections (CROI). March 4-7, 2018. Boston. Abstract 77.
2. Post WS, Budoff M, Kingsley L, et al. Associations between HIV infection and subclinical coronary atherosclerosis. Ann Intern Med. 2014;160:458-467. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4143766/




|
| |
|
 |
 |
|
|