 |
 |
 |
| |
Summary from EASL 2018 for Hepatitis C (HCV)
HCV in 2018: Success stories and remaining challenges?
|
| |
| |
Jürgen K. Rockstroh M.D., Professor of Medicine
University of Bonn, Germany
Edited by Jules Levin
Correspondence:
Prof. Dr. J.K. Rockstroh
Department of Medicine I
University of Bonn
Sigmund-Freud-Str. 25
53105 Bonn
Germany
Introduction
The International Liver Congress™ (ILC) (the 53rd Annual International Liver Congress) of the European Association for the Study of the Liver (EASL)) was held in April from 11-15th, 2018 in Paris, France. Over 10.000 delegates documented the persistent interest in the area of liver disease. Although, no new HCV drugs are entering the HCV treatment arena, there was a considerable amount of new data from studies in the hepatitis field showing that there is still a lot to learn and discuss. Once again, issues around HCV screening, linkage to care, fine-tuning HCV treatment including a tremendous amount of real-life data from various cohorts and affected patient populations, treated with different DAA-combinations throughout the world were presented. Moreover, with increasing HCV cohorts in place and extended follow-up, a better understanding of hepatitis C as a disease is taking place. Indeed new insights into which comorbidities might all benefit from cure of HCV after successful DAA therapy were presented. In addition, the newly revised EASL practice guidelines for HCV management were released for the first time and the corresponding publication is now downloadable from the EASL website (http://www.journal-of-hepatology.eu/article/S0168-8278(18)31968-8/fulltext). Finally, increasing reports of microelimination are encouraging, maybe less because for example treating all around 1000 estimated HCV-infected individuals from Iceland is not really a challenge, but because the associated reduction in new HCV infections convincingly shows that high treatment uptake really has an impact on future infections and HCV epidemiology (1). Nevertheless, inequalities in access to HCV therapy worldwide persist, particularly in high burden countries underlining that the path to achieving WHO HCV elimination targets is still long and stony.
Feedback from the real world
With the more recent introduction of the pangenotypic regimens sofosbuvir/velpatasvir and glecaprevir/pibrentasvir, two new fix dose combinations have become available which may even overcome the need for baseline HCV genotype assessment. Larger data sets however, from real-life cohorts still are missing but this gap has been filled at this year EASL. First real-world data on safety and effectiveness of glecaprevir/pibrentasvir (G/P) for the treatment of patients with chronic HCV infection was presented from Germany within the German Hepatitis C-Registry (DHC-R) (2). The DHC-R is an ongoing, non-interventional, multicenter, prospective registry study. Data were collected between July 28, 2017 and February 9, 2018 from 104 sites in Germany. All patients included into the study were treated with G/P for 8, 12, or 16 weeks according to the local label. Primary study end-point was SVR12 (HCV RNA < LLOQ 12 weeks post-treatment) assessed in the "Total Effectiveness Population", and in the "Per Protocol population" (excludes non-virologic failures). Overall, 866 subjects were enrolled into the study. Patients with advanced cirrhosis were excluded. The patient disposition is summarized in figure 1.
Figure 1: Patient disposition
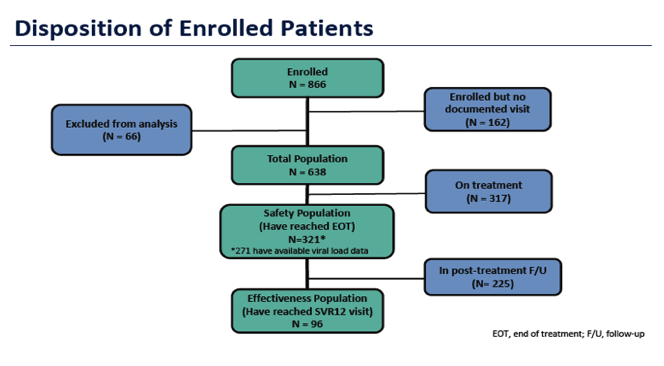
Of note, only 96 subjects had yet a full data set available for SVR12 analysis. The baseline characteristics for all 638 patients who entered the study and received G/P therapy are listed in table 1 and 2.
Table 1: Baseline characteristics
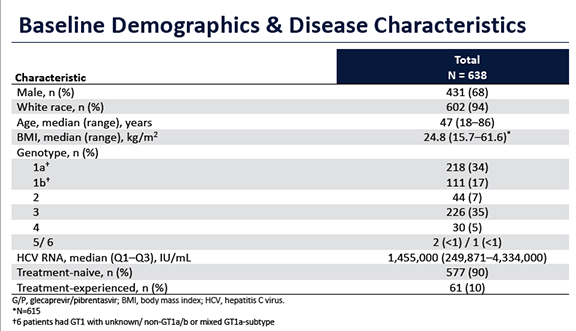
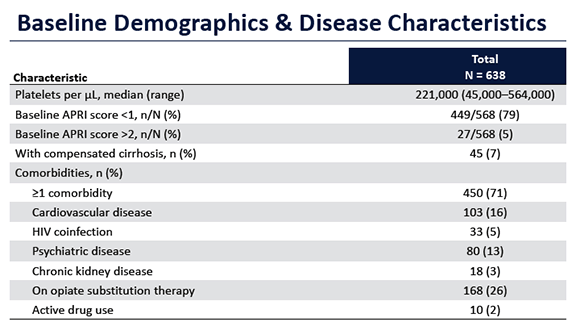
In principle all HCV genotypes were included but only very few GT 5 and 6 patients entered the study. Only 7% of patients already had cirrhosis and only 10% were HCV treatment-experienced. Overall, in this relatively less advanced patient population for liver disease, excellent SVR12 rates were obtained for the 96 patients who already had SVR12 follow-up data available. Indeed SVR12 was achieved in 93/96 patients (97%). Of the 3 non-responders, one was lost to follow-up already early at treatment week 1. 2 patients discontinued therapy early because of adverse events (1 patient with irritable bowel disease, cardiovascular insufficiency, and thyroid dysfunction discontinued at TW4 due to diarrhea and 1 patient with psychiatric disease, drug abuse, HIV/HCV coinfection, and chronic respiratory disease discontinued at TW1 due to nausea). Figure 2 and 3 summarize the outcome of the treated patients in the per protocol analysis treated so far.
Figure 2: Effectiveness of G/P, SVR12 (per protocol population) Figure 3: Treatment duration
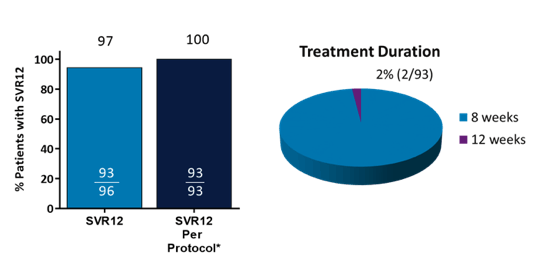
No virological failure has been documented to date underlining the excellent efficacy of G/P in this real world cohort. Overall safety was good with less than 1% discontinuing because of adverse events.
FIRST REAL-WORLD DATA ON SAFETY AND EFFECTIVENESS OF GLECAPREVIR/PIBRENTASVIR FOR THE TREATMENT OF PATIENTS WITH CHRONIC HEPATITIS C VIRUS INFECTION: DATA FROM THE GERMAN HEPATITIS C-REGISTRY - (04/13/18)
Further real-life data from G/P fix-dose HCV therapy was presented from Italy. The NAVIGATOR-II study investigated the effectiveness and safety of G/P in an Italian real-life setting (3). 723 HCV Italians consecutively treated with G/P within the Lombardy web-based Navigator-II Network were analyzed. G/P was administered according to drug label (8, 12 or 16 weeks). Fibrosis was determined histologically or non-invasively, through liver stiffness measurement (LSM). Sustained Virological Response 4 (SVR4) was defined as undetectable HCV-RNA 4weeks after the end of treatment (EOT). The baseline characteristics as well as baseline features by treatment duration are depicted below in table 3 and 4.
Table 3: Baseline characteristics of the NAVIGATOR-II study
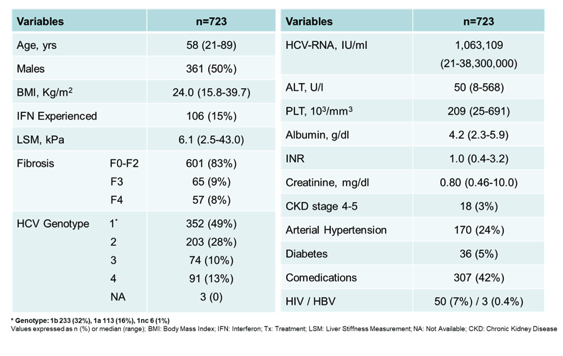
Table 4: Baseline Features According to Treatment Duration
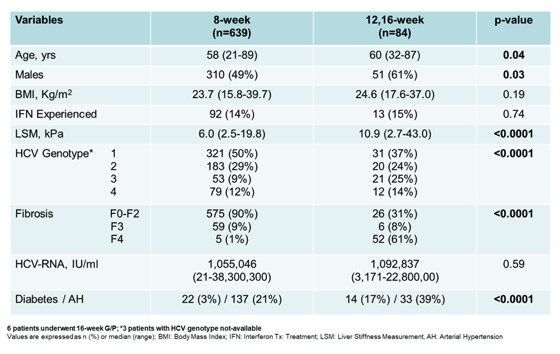
Of note, patients with longer treatment durations were more likely to have more advanced liver disease and revealed more concomitant comorbidities. The per-protocol analysis of SVR4 and 12 for the different treatment duration groups are summarized in figure 4.
Figure 4: Virological Response rates (Interim Analysis, Per Protocol)
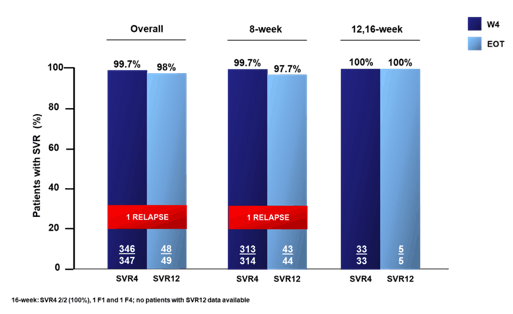
So far, only one relapse has been noted in the entire patient population thereby emphasizing the excellent efficacy with the G/P combination in this real-life cohort. The relapse was a GT3 patient with FO fibrosis at baseline and an Y93H NS5A variant at baseline (at relapse Y93H and L31I). Adverse events were mostly mild and only reported in 49 (7%) patients. Four (0.5%) patients discontinued HCV therapy due to AEs. Three (0.4%) patients died of drug-unrelated causes. In conclusion, in a large real-life cohort of HCV Italian patients, G/P combination administered for 8 or 12-16 weeks confirmed excellent effectiveness and safety.
Real-Life Effectiveness and Safety of Glecaprevir/Pibrentasvir Among 723 Patients with Chronic Hepatitis C: The NAVIGATOR-II Study - Interim Analysis - (04/16/18)
Interesting real-life data was reported from Scotland on treatment with sofosbuvir/velpatasvir for only 8 weeks in genotype 3 patients (4). Twelve weeks of sofosbuvir/velpatasvir (SOF/ VEL) have been demonstrated to be highly effective at treating HCV genotype 3. A previous phase 2 trial reported high SVR rates in treatment-naïve non-cirrhotic patients, treated with 8 weeks of SOF/ VEL (SVR 98% (52/53)). In order to maximize the number of patients potentially cured with in a fixed treatment budget, the Scottish HCV care providers elected to treat non-cirrhotic GT3 patients eligible for treatment (F2/3) with 8 weeks of SOF/VEL (4). DAAs in this study were dispensed from community pharmacies in line with patients' opiate substitution therapy (OST). Those still injecting or in early stages of recovery were prescribed methadone (and DAAs) as daily observed therapy (DOT), with more stable patients dispensed 2-3 x weekly or weekly. Patients not on OST were dispensed at 2 weekly intervals. Overall, the treatment outcome results were presented for 90 patients. Table 5 summarizes the main baseline characteristics. 82/90 (91.1%) were on OST treatment. 55% of study participants had self-reported ongoing drug use or positive urine screening.
Table 5: Baseline characteristics

At end of treatment (week 8) 59 subjects (65.6%) were HCV RNA undetectable, 16 (17.8%) were <12 IU/ml but still positive and 7 (7.8%) even had low levels of quantifiable HCV RNA between 12-41 IU/ml. For 8 subjects no EOT results were available. The SVR12 rates for the entire study cohort are shown below in figure 5.
Figure 5: SVR12 rates
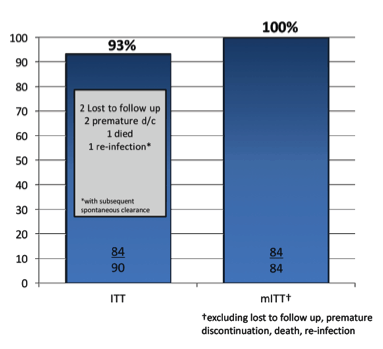
To date in the mITT analysis all patients achieved SVR12. This is an impressive result and underlines once again even in the setting of a real-life IVDU cohort with high rates of ongoing substance abuse that HCV cure is achievable. In patient groups with adherence challenges 8 weeks regimens appear particularly attractive. Of interest, is also that a considerable amount of patients still had a positive HCV-PCR at EOT emphasizing that a positive signal in the PCR or even low level viremia at end of treatment does not preclude subsequent treatment success. In summary, patients on daily-supervised OST have excellent SVR rates when given DAAs along with OST. Widespread adoption of 8 weeks treatment could reduce drug acquisition costs, and increase clinic treatment capacity, without sacrificing SVR. In settings with limited resources, such a strategy may help to achieve the HCV elimination goals.
8 weeks sofosbuvir/velpatasvir in genotype 3 patients with significant fibrosis: Highly effective amongst an OST cohort - (04/13/18)
New data from randomized clinical trials with already registered DAA combinations
There is still considerable interest in new data from clinical trials with already registered DAA compounds, which either looks at new patient populations that have been understudied before or investigates new treatment durations. In consideration of the high price associated with DAA rollout, possibilities to reduce treatment duration promise cheaper therapy and are obviously welcomed in particular in countries with high disease burden. At EASL, data was presented on a trial evaluating a shorter treatment duration of elbasvir/grazoprevir (EBR/GZR) for 8 weeks in non-cirrhotic treatment-naïve genotype 4 patients (5). Recent EASL guidelines already recommend EBR/GZR for 8 weeks in HCV GT1b patients who are TN and have F0-F2 fibrosis. In a pooled analysis of clinical trial data, a 12-week regimen of EBR/GZR was highly effective among TN participants with HCV GT4 infection, thereby prompting the question whether shorter treatment durations may also be feasible in this patient group (6). Treatment-naive participants with mild to moderate fibrosis (METAVIR stage F0-F2 determined by Fibroscan) were randomized to EBR/GZR (50 mg / 100 mg) for 8 or 12 weeks accordingly. Randomization was stratified by baseline viral load ≤ vs > 800,000 IU/mL. The primary efficacy end-point was SVR12 (HCV RNA <15 IU/mL at follow-up week 12). The study design is depicted below in figure 6.
Figure 6: Study design
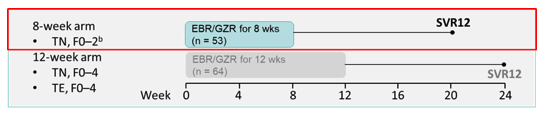
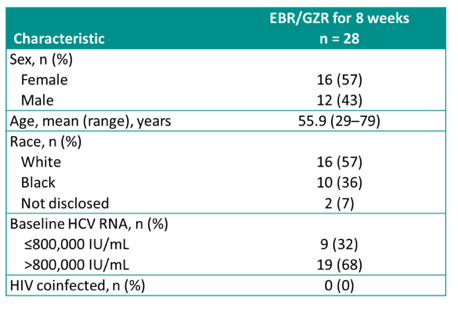
This is an ongoing trial with 53 participants enrolled in the 8-week arm. So far, 47 have completed 8 weeks of treatment and 28 were evaluable for SVR12. The baseline characteristics of those 28 patients are shown below in Table 6. Of note, two thirds of the patients had a HCV viral load above 800.000 IU/ml.
Table 6: Baseline characteristics
Most of the study subjects had a GT 4a infection (39%), followed by 4d and 4f with 14%, respectively. The preliminary response rates are shown below in figure 7.
Figure 7: Treatment outcome results
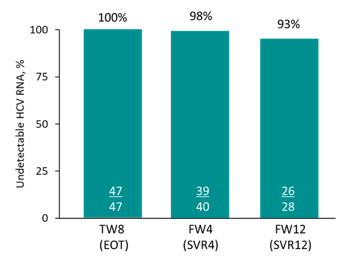
Of those patients, which already had SVR12 follow-up available, 93% achieved SVR12. Two patients developed a relapse one with HCV GT 4a and one 4d, respectively. One patient who developed relapse had no RAS at baseline or upon failure, the other had the NS5A RAS T58P at baseline, the result from the genotype at virological failure is still pending.
In summary, in this ongoing study investigating a novel 8-week treatment regimen of EBR/GZR in participants with HCV GT4 infection high rates of SVR among treatment-naive participants with mild to moderate (F0-F2) fibrosis who have completed FW12 were reported. 2 participants developed a relapse. The EBR/GZR combination showed an excellent safety profile with no serious AEs or discontinuations. Final results from the 8-week arm plus outcomes in participants treated for 12 weeks will provide further information regarding the effective use of EBR/GZR in participants with HCV GT4 infection.
Efficacy and safety of 8 weeks of elbasvir/grazoprevir in HCV GT4-infected treatment-naive participants - (04/12/18)
One remaining important question is around the value of ribavirin as an add-on to sofosbuvir/Velpatasvir therapy in HCV genotype 3 patients. In cirrhotic patients, lower SVR12 rates have been reported for SOF/VEL, particularly if baseline RAS were present. Indeed, within the newly released EASL HCV clinical practice guidelines the combination of sofosbuvir and velpatasvir is not recommended in treatment-naïve and treatment-experienced
patients infected with HCV genotype 3 with compensated (Child-Pugh A) cirrhosis, because suboptimal results have been reported with this combination. Maria Buti presented data from a randomized trial, which evaluated SOF/VEL ± RBV for 12 weeks in patients with chronic HCV GT 3 infection and compensated cirrhosis (7). This randomized, open-label study in GT 3 patients with compensated cirrhosis was conducted at 29 sites in Spain. The study included treatment naïve and treatment experienced patients, including patients with NS3/4 PI or NS5B inhibitor treatment experience. Patients with HIV coinfection were eligible. The study design is shown below in figure 8.
Figure 8: Study design
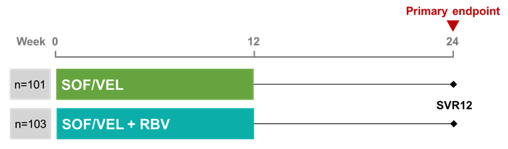
The baseline characteristics of the 204 included patients are listed in table 7.
Table 7: Baseline characteristics
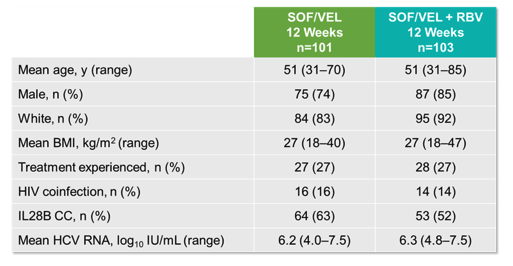
Of note, 27% of patients included were treatment experienced, 15% were HIV coinfected. Overall, 92/101 patients in the SOF/VEL arm (91%) versus 99/103 in the SOF/VEL+RBV arm (96%) achieved SVR12. The SVR 12 rates by treatment experience are shown below in figure 9.
Figure 9:Results: SVR12 by Prior Treatment
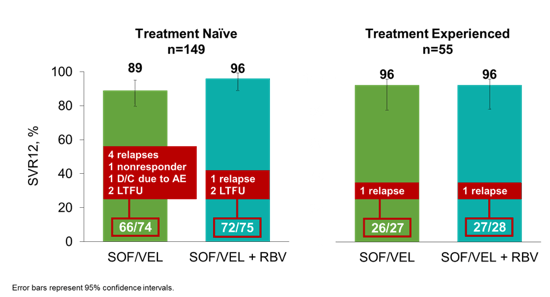
In patients with Y93H at baseline 2 of 4 patients achieved SVR12 in the SOF/VEL arm versus
8 of 9 patients achieving SVR12 in the SOF/VEL + RBV. The SVR 12 rates by baseline NS5A RAS is shown below in figure 10.
Figure 10: SVR12 rates by baseline NS5A RAS
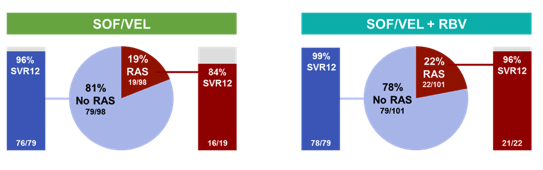
The virology analysis was performed on patients with known virologic outcome; RASs were analyzed using a 15% cut off.
Overall efficacy was very good for all GT3 patients independent whether RBV was added or not. In the presence of Y93H in cirrhotic GT3 patients however, the addition of RBV can reduce relapse risk. Therefore, in GT3 potentially the performance of a genotypic resistance test to either rule out or confirm the presence of an Y93H may be helpful to decide whether additional ribavirin should be added or not. With regard to safety, SOF/VEL was well tolerated with hardly any discontinuations because of adverse events. Of note, more lab abnormalities in particular changes in hemoglobin levels were noted in the study participants who were receiving add-on ribavirin. The safety results are summarized in table 8.
Table 8: Safety results
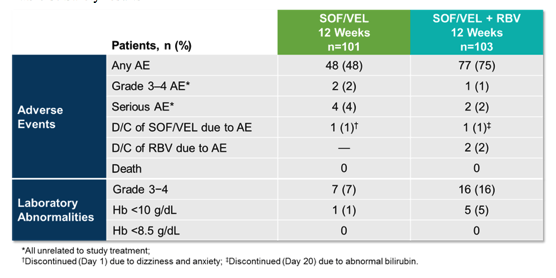
Safety and Efficacy of Sofosbuvir/Velpatasvir with and without Ribavirin in Genotype 3 HCV-Infected Patients with Cirrhosis - (04/13/18)
GT 5 and 6 are rare HCV genotypes and frequently underrepresented in clinical trial development of HCV DAAs. GT5 has an estimated global prevalence of <1% and can be found primarily in Chile and southern and eastern sub-Saharan Africa. GT6 has a 5% global prevalence and is primarily located in Southeast Asia and southern China. ENDURANCE-5,6 is an ongoing phase 3b, non-randomized, open-label, multicenter study conducted in 84 adults with chronic HCV GT 5 or 6 infection without cirrhosis (8 weeks) or with compensated cirrhosis (12 weeks) (8). The study design is shown below in figure 11.
Figure 11: Study design: ENDURANCE-5,6
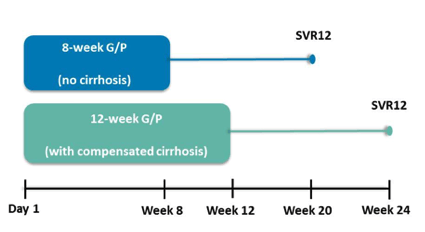
The baseline characteristics of the study population are summarized in table 9.
Table 9: Baseline characteristics of the ENDURANCE 5,6 trial.
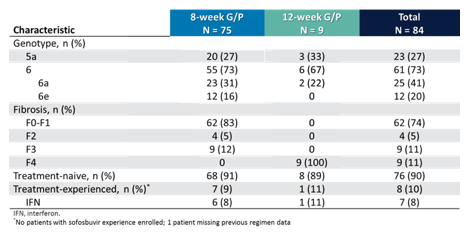
The majority of patients were treatment naïve. The various genotype 6 subtypes included are shown in more detail in figure 12. Most patients had a GT6a subtype. The great diversity in subtypes however, underlines the necessity for collecting data on all different subtypes as treatment outcomes may differ by subtype.
Figure 12: Baseline Demographics: Genotype 6 Subtype Diversity
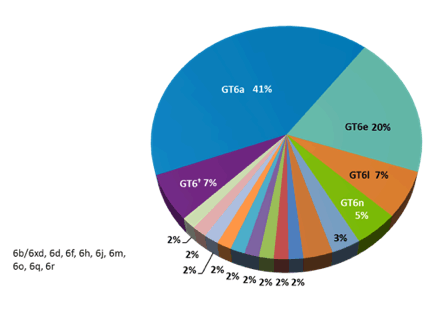
In this interim analysis, 70 patients have reached PTW12. 14 patients have yet to reach PTW12 but all (14/14) had viral suppression at end of treatment. The SVR12 rates for the 70 patients with complete follow-up are shown in figure 13.
Figure 13: SVR12 rates
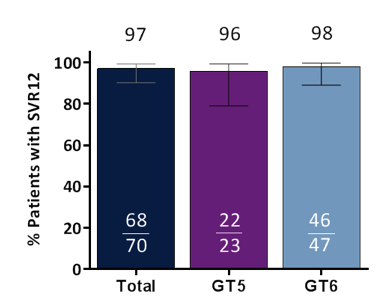
Overall, excellent cure rates have been obtained in the GT5,6 patients. One treatment-naïve, non-cirrhotic GT5 patient relapsed and one treatment-naïve GT6f patient with cirrhosis developed on treatment failure. G/P maintained a favorable safety profile: no discontinuations, no serious adverse events attributed to G/P, and no grade 3 or higher ALT elevations. In summary, G/P achieved high SVR12 rates in genotype 5 or 6 infection.
EFFICACY AND SAFETY OF GLECAPREVIR/PIBRENTASVIR IN PATIENTS WITH HCV GENOTYPE 5 OR 6 INFECTION: THE ENDURANCE-5, 6 STUDY - (04/13/18)
Direct-acting antivirals (DAAs) have not been prospectively studied or well-utilized in sub-Saharan Africa (SSA). At EASL results from an ongoing prospective study of ledipasvir/sofosbuvir (LDV/SOF) in Rwanda for adults with chronic hepatitis C virus (HCV) genotype (GT) 1 and GT4 infection was reported (9). The "Simplifying Hepatitis C Antiviral Therapy in Rwanda for Elsewhere in the Developing World" (SHARED) study is a prospective trial in Rwanda evaluating the safety and efficacy of LDV/SOF (90 mg/400 mg once daily) for 12 weeks in 300 adults with HCV GT1 and/or GT4. Exclusion criteria include decompensated cirrhosis, HBV coinfection, uncontrolled HIV infection, and hepatocellular carcinoma. Sustained virologic response 12 weeks after completion of therapy (SVR12) is the primary efficacy outcome. Among the 300 enrolled participants, median age is 64 (IQR 55, 72) and 62% are women. 30 (10.0%) participants are co-infected with HIV. Baseline median HCV viral load is 6.0 log10 IU/ml [IQR 5.6, 6.4]. 249 (80.3%) are reported to have GT4 only, 4 (1.3%) with GT1 only, and 47 (15.7%) with "mixed" GT1/4. The SVR12 results are shown below in figure 14.
Figure 14: SVR12 rates by genotype
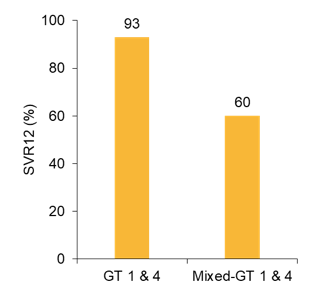
259/298 (87%) achieved SVR12 (ITT analysis; 2 VLs pending). 32 (11%) developed a relapse, and 5 (2%) patients developed on-treatment virological failure. One
(0.3%) death occurred during the study. Mixed GT 1 + 4 was predictive of VL failure (HR = 4.6; p<0.001). Further GT subtyping and deep sequencing for resistance
mutations is ongoing. Overall, no drug-related AEs or laboratory abnormalities
resulting in treatment discontinuation or study termination were recorded throughout the study. LDV/SOF was well tolerated and effective in a predominant GT 4 population in Rwanda. Deeper understanding of GT 4 heterogeneity and resistance in this region
is needed and could impact guidelines for DAA selection. Study results are very encouraging for DAA introduction and scale-up in Rwanda and other limited resource settings.
DIRECT-ACTING ANTIVIRAL TREATMENT IN SUB-SAHARAN AFRICA: A PROSPECTIVE TRIAL OF LEDIPASVIR/SOFOSBUVIRFOR CHRONIC HEPATITIS C INFECTION IN RWANDA (THE SHAREDSTUDY) - (04/20/18)
New data from key populations
People who inject drugs (PWID) are most affected by HCV infection. To reach the WHO goal of HCV eradication by 2030, DAA therapy has to be scaled up particularly in PWID. Unfortunately, many barriers still exist when it comes to HCV therapy in this patient group despite reports of high SVR rates in patients with and without opoid substitution therapy (OST). A potential concern is a higher proportion of lost patients in OST und non-OST with previous drug history. A German study at EASL investigated the role of alcohol and cannabis consumption on sustained virological response (SVR) rates and proportion of lost to follow up (LTFU) (10). All patients analyzed derived from the DHC-R which is a German national multicenter non-interventional real-world registry study. Overall, N=7,747 chronic HCV patients started DAA therapy: n=739 OST (patients with Opioid Substitution Therapy), n= 1,500 non-OST/DU (patients with former/current Drug Use without Opioid Substitution Therapy) and n=5,508 non-OST/NDU (patients without a history of drug use (Non Drug Use). The final data set included N=528 OST and n=5,582 non-OST (DU and NDU) who all had therapy completed and at least one follow-up documentation (Intention-to-treat (ITT) population). The patient disposition is pictured in figure 15.
Figure 15: Patient disposition
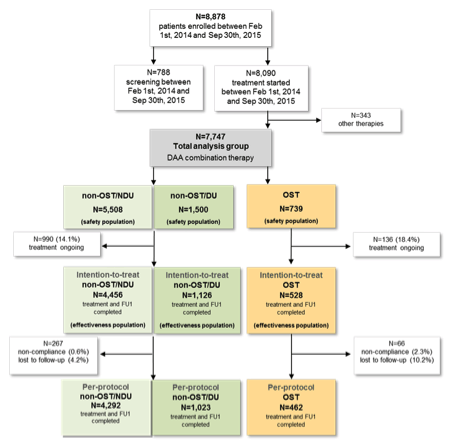
OST: patients with Opioid Substitution Therapy; non-OST/DU: patients with former/current Drug Use without Opioid Substitution Therapy; non-OST/NDU: patients without a history of drug use (Non Drug Use)
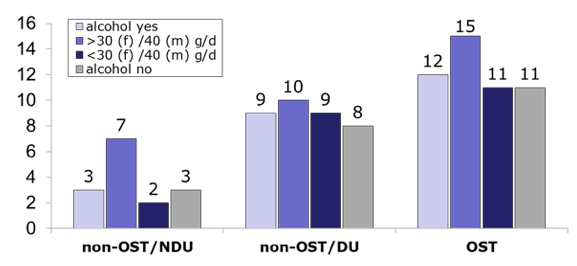
Alcohol consumption was reported in 17.9% (128/714) of OST, in 17.1% (256/1,462) of non-OST/DU and in 11.6% (631/5,421) of non-OST/NDU patients. Among OST patients, 25% consumed high amounts (>40 g alcohol/d (men)/>30 g/d (women)) of alcohol. In non-OST/DU, high amounts of alcohol were consumed in 22.2%. In non-OST/NDU, significantly less patients (13.9%) consumed high amounts of alcohol when compared to OST patients (p < 0.05). Similarly, cannabis consumption was significantly higher in OST patients (19.2%, 139/725), than in non-OST/DU (9.6%,141/1,474, p < 0.05) and non-OST/NDU patients (1.2%, 66/5,448, p < 0.05). In alcohol and in non-alcohol consuming patients proportion of LTFU did not differ significantly within each group but was significantly higher in OST compared to non-OST/NDU. LTFU occurred mainly after end of therapy (EOT) (see figure 16).
Figure 16: Results: Lost to follow up (LTFU) according to alcohol consumption
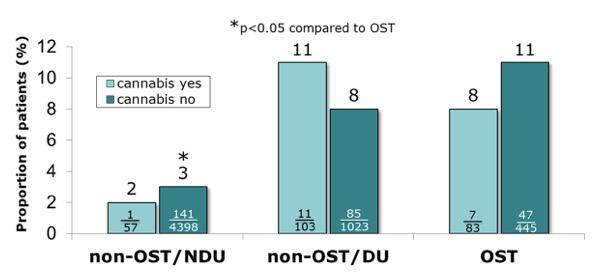
In contrast, consumption of cannabis was not a risk factor for LTFU. Indeed, in cannabis consuming patients the proportion of lost-to-follow-up did not differ significantly between groups (see figure 17).
Figure 17: Results: Lost to follow up (LTFU) according to cannabis consumption
Except for patients with a high alcohol intake, SVR 12/24 rate (ITT) was significantly higher in non-OST/NDU compared to OST patients, mainly driven by less loss-to-folow-up (see figure 18). Cannabis consumption however, did not influence SVR12/24 (ITT) significantly.
Figure 18: Results: SVR 12/24 rates (ITT) according to alcohol consumption
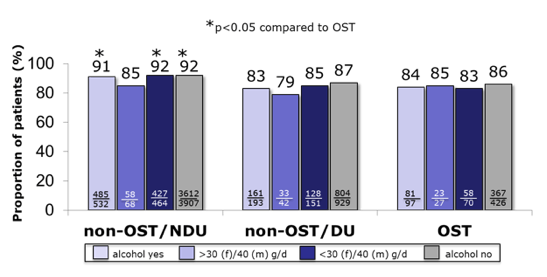
In summary, High SVR rates can be achieved in both OST and non-OST patients. Alcohol or cannabis consumption do not diminish cure rates in PP analysis. However, LTFU is more likely in patients with current or former drug use than in patients without drug history or with a high alcohol consumption but occurred mainly after EOT, leaving a high chance for HCV elimination in these patients.
Scaling up HCV-DAA treatment in patients on opioid substitution therapy - does alcohol or cannabis consumption diminish cure rates? Data from the German Hepatitis C Registry (DHC-R) - (04/16/18)
Re-treatment in DAA failures
Although virological failure under all oral DAA combination therapy is rare, around 1-5% of patients may have failed modern HCV therapy. Retreatment, in particular after development of resistance-associated substitutions, may be challenging. At EASL, several studies addressing retreatment after DAA failure were presented. Patients, who had virological failure in the G/P Phase II or III clinical trials, across all genotypes, were offered enrollment into a retreatment study, MAGELLAN-3. MAGELLAN-3 is an ongoing open-label, phase 3b trial to determine the efficacy and safety of G/P (300/120 mg once daily) + sofosbuvir (SOF; 400 mg once daily) + ribavirin (RBV; 1,000-1,200 mg daily, divided into two doses) in patients who had virologic failure on G/P treatment in an AbbVie-sponsored clinical trial. Patients who had non-GT 3 infection, without cirrhosis, and were naïve to NS3/4A protease and NS5A inhibitors prior to failure with G/P, received 12 weeks of treatment; all others received 16 weeks. The study design of the MAGELLAN-3 study is shown below in figure 19.
Figure 19: Study design of the MEGALLAN-3 study
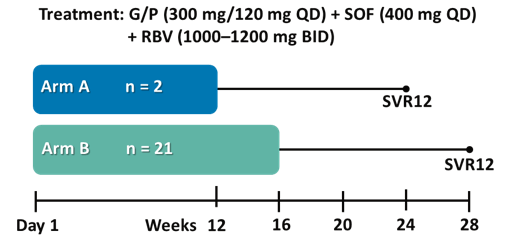
The baseline characteristics of the patients included into the study are summarized in table 10 and 11.
Table 10: Baseline demographics and clinical characteristics
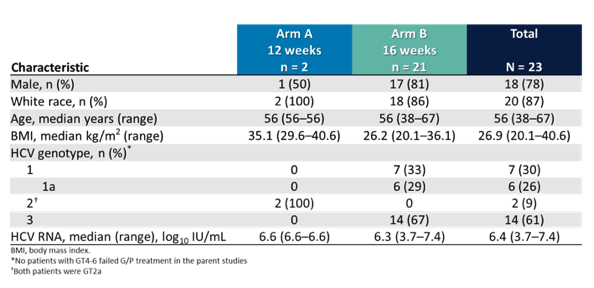
Table 11: Baseline demographics and clinical characteristics
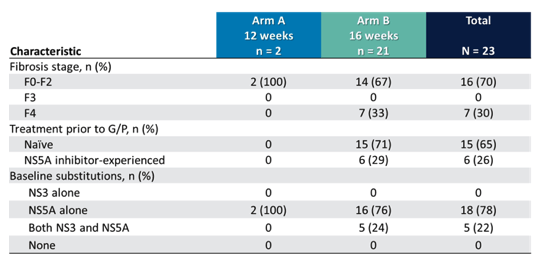
Most patients had GT1 infection, with one third showing compensated cirrhosis. All patients had relevant RASs from prior DAA treatment and subsequent virological failure. Figure 20 shows SVR12 rates for all patients by treatment arm and genotype.
Figure 20: SVR12 rates
Overall, only one relapse occurred in a GT1a patient with compensated cirrhosis who had failed SOF/LDV prior to G/P. In conclusion, preliminary data from this study show that HCV-infected patients who experienced virological failure following G/P treatment can achieve high SVR12 rates with G/P + SOF + RBV. Overall, the combination of G/P + SOF + RBV was well tolerated. Indeed, it looks as if 3-drug class therapy (NS5A+NSA+Sof) is a great option for salvage therapy. Similar good responses have been described for the licensed 3-drug fix dose combination of Velpatasvir/sofosbuvir/voxilaprevir (12).
RETREATMENT OF HEPATITIS C VIRUS INFECTION IN PATIENTS WHO FAILED GLECAPREVIR/PIBRENTASVIR - (04/12/18)
The fixed dose combination of once daily 300 mg glecaprevir and 120mg pibrentasvir (GP) was FDA approved for the treatment of chronic HCV infection, including genotype 1 (GT1) patients who failed a prior NS5A-containing regimen without prior exposure to a PI. The aim of this retreatment study was to add further evidence in GT1 NS5Ai/SOF ±RBV failures utilizing the FDA label-consistent GP regimen given for 16 weeks and in addition to explore a shorter 12-week duration of GP in non-cirrhotic subjects and compensated cirrhotics (RBV added) (13). The study design is shown below in figure 21.
Figure 21: Study design
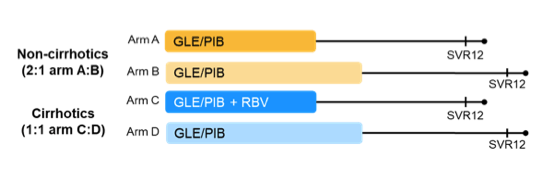
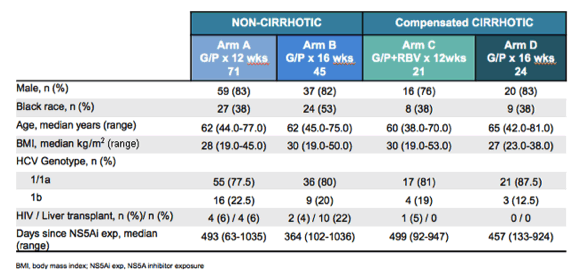
The baseline characteristics of the patient population are listed below in table 12.
Table 12: Baseline demographics and clinical characteristics
The baseline RAS (15% threshold) are listed below in table 13.
Table 13: Baseline polymorphisms
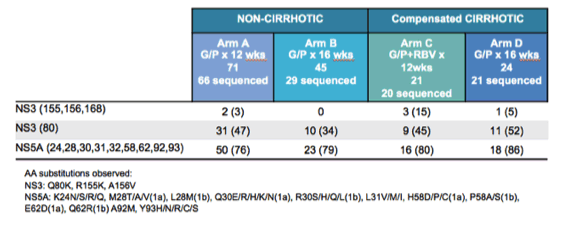
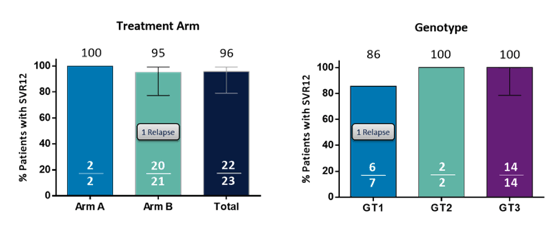
Indeed, the majority of patients had baseline NS5A RAS present. The preliminary outcomes being SVR4 rates for all treatment arms are shown below in figure 22.
Figure 22: SVR4 rates
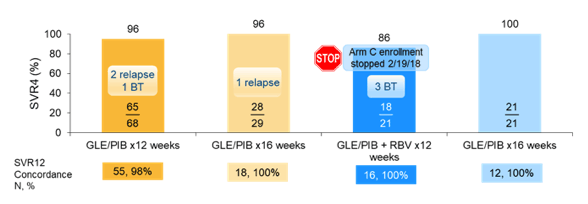
7 treatment failures were observed: 2 relapses and one breakthrough (BT) in the non-cirrhotic 12 week treatment arm, one relapse in the non-cirrhotic 16 week treatment arm and 3 breakthroughs in the compensated cirrhosis 12 week + RBV arm, leading to suspension of this particular study arm. All virological failures where observed in GT1a patients. None of the patient with virological failure had a NS3A RAS at baseline but 4/6 did show NS3A RAS upon failure. All 6 patients with genotype data available with failure had NS5A RAS at baseline.
In conclusion, preliminary data from this trial shows that patients with HCV GT1 infection who experienced virologic failure following NS5A+ SOF +/- RBV therapy achieved an overall high SVR4 rate of 95% with GP retreatment despite high rates of baseline NS5A RAS. Lower efficacy and tolerability was observed for the combination of G/P plus RBV given for 12 weeks in compensated cirrhotics (SVR4 rate 86%).
Phase 3b, Multi-Center, Randomized, Open-Label, Pragmatic Study of Glecaprevir/Pibrentasvir (G/P) +/- Ribavirin for GT1 Subjects with Chronic Hepatitis C Previously Treated with an NS5A Inhibitor + Sofosbuvir Therapy - (04/16/18)
Implications of SVR following DAA therapy: what are the clinical benefits?
Various studies presented at EASL dealt with changes in the natural course of liver disease but also other disease entities or comorbidities following successful HCV therapy. Long-term virological and clinical outcomes in patients with cirrhosis who achieve SVR after DAA treatment are being evaluated in the DALTON cirrhosis registry study (14). Overall, 1245 patients with decompensated and compensated cirrhosis who achieved SVR following treatment with a SOF-based regimen were assessed. Table 14 summarizes the main demographics of the study population.
Table 14: Demographics

The liver complications after SVR are shown by CTP score in table 15. In this study, HCC was uncommon and occurred more often in patients with decompensated cirrhosis. Overall, 99.9% of patients maintained SVR with only one incidence of virologic failure observed.
Table 15: Liver complications after SVR

Figure 23 shows the changes in FibroScan after SVR for the different CTP stages over time. Impressively, most patients show an improvement in FibroScan score which is maintained over time.
Figure 23: FibroScan scores over time
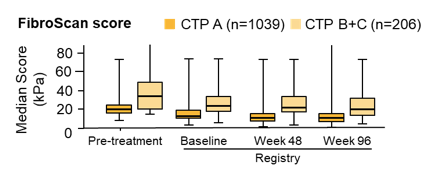
Changes in CTP and MELD scores for patients with decompensated cirrhosis are shown in figure 24.
Figure 24: CTP Class and MELD Score Shifts in Decompensated Patients
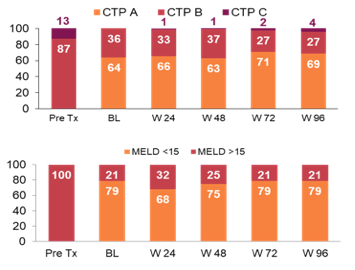
The majority of patients maintained or improved their CTP category relative to pre-treatment up to week 96. This data nicely underlines the clinical benefit, which comes with achieving SVR in patients with already relevant liver disease at baseline.
Long-Term Follow-up of Patients with Chronic HCV Infection and Compensated or Decompensated Cirrhosis Following Treatment with Sofosbuvir-Based Regimens - (04/16/18)
One important remaining research area in the area of HCV is cohort research which allows to study the long-term outcome of liver disease after successful DAA therapy and to study the separate effects on hepatic and non-hepatic causes of death. Clearly one important question is whether obtaining SVR will also affect other relevant diseases such as cardiovascular disease. Lipid profiles have been noticed to change after SVR and also changes in inflammation associated with chronic viral infection can be expected. At EASL data from the prospective RESIST-HCV cohort were presented which evaluated 5,166 patients who started DAAs treatment in 22 Sicilian Centers between March 2015 and December 2016 (15). 499 patients with previous HCC or OLTX were excluded from further analysis. All patients were followed after SVR to register liver-related and unrelated outcomes. The primary endpoint was the evaluation of survival since starting DAAs. Cox regression analysis was used to assess the predictors of liver-related and unrelated death. Patients were observed for a mean of 72 weeks. The baseline characteristics of the cohort are shown below in table 16.
Table 16: Baseline clinical features of 4668 patients included in RESIST-HCV cohort
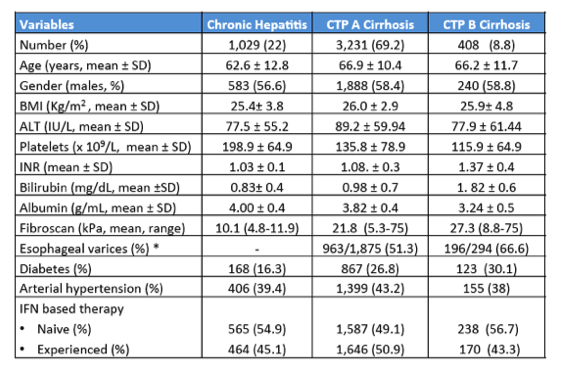
Of note, the majority of patients (over 75%) were cirrhotic with a relatively high mean age (above 62) clearly indicating that this was a patient population which a high risk for clinical events. Table 17 summarizes the main virological features of the study population at baseline.
Table 17: Baseline virological features
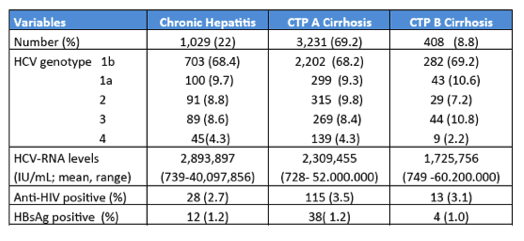
Most Patients had a HCV GT1b infection, only very few had concomitant HIV infection. SVR was achieved under DAA therapy in 90.7% of all patients, with only 0.3% of drop-outs due to adverse events. 63 patients (1.4%) died during the follow-up of 72 weeks +/- 32 weeks. The main death causes are listed in table 18.
Table 18: Death causes
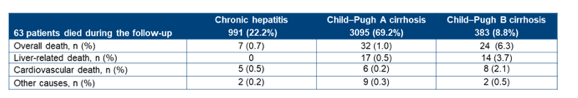
Risk for liver-related death was highest in patients with Child B cirrhosis. In multivariate cox-regression analysis albumin <3.5 g/dl (HR 6.01; 95% CI 2.30-15.73) and non-SVR (HR 18.50; 95% CI 6.75-50.70) emerged as significant risk factors for liver death in Child A cirrhosis patients. The liver mortality in 3095 patients with Child A cirrhosis is shown below in figure 25.
Figure 25: Liver mortality in Child A cirrhosis patients according to viral response.
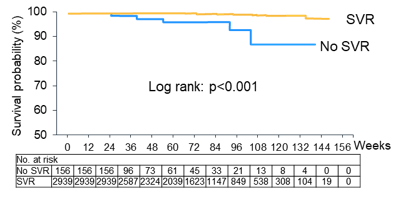
The cardiovascular mortality observed within the cohort of 4468 individuals is shown below in figure 26.
Figure 26: cardiovascular mortality related to viral response
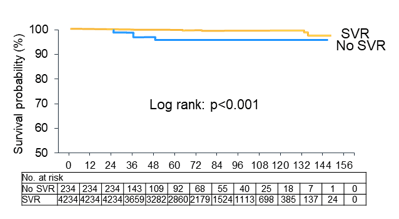
Overall, patients with SVR were significantly less likely to die from cardiovascular disease. Risk factors for cardiovascular mortality were further evaluated by cox multivariate model. Only diabetes (HR 4.11; 95% CI 1.30-12.98, p=0.011) and non-SVR (HR 10.56; 95% CI 3.43-32.46, p<0.001) were significantly associated with an increased risk for cardiovascular death.
In conclusion, patients with SVR to a DAA regimen have a better survival outcome than non-responders at all stages of liver disease. Eradication of HCV in patients with CHILD A cirrhosis reduces the risk of liver events and increases survival in comparison to non-SVR. Subjects with Child B cirrhosis retain a significant risk of HCC, hepatic decompensation and death after HCV eradication. Deaths linked to cardiovascular disease are reduced after viral eradication regardless of the stage of liver fibrosis.
DISEASE OUTCOMES AFTER DAA-INDUCED SVR: DATA FROM THE RESIST-HCV COHORT - (04/17/18)
Hepatitis C virus (HCV) infection has been associated with extrahepatic co-morbidities. Prior to the introduction of direct-acting antiviral (DAA) agents, HCV therapy involved interferon (IFN), which has been reported to have anti-tumor effects, but has substantial side effects and has low sustained virologic response (SVR) rates. In contrast, DAAs are well-tolerated and have SVR rates >90%. To characterize the long-term effects of DAA-based therapy a study at EASL examined the risk of total non-hepatic cancer associated with DAA treatment, vs IFN treatment in the pre-DAA era (16). This is a very new research question and of great interest as HCV previously has been associated with an increased risk for certain tumors. Overall, 367,156 adults with chronic HCV infection were enrolled between January 2006 and March 2017 in a U.S. administrative claims database. 22,894 were identified as have being exposed to DAAs (follow-up through March 2017), and 10,989 who had been exposed to IFN prior to May 2011 (introduction of boceprevir, follow-up through November 2013). All patients had ≥12 months of prior enrolment and no evidence of prior cancer at baseline. Absolute rates per 100 person-years (PY) of cancer events (identified by diagnostic claims, excluding liver cancer) were calculated, along with exact 95% Poisson confidence intervals (CIs). Hazard ratios (HRs) estimating cancer risk associated with DAA vs pre-DAA IFN were estimated using Cox proportional hazards methods, after adjustment for covariates and incorporation of weighting based on treatment propensity scores. Table 19 shows the unadjusted and adjusted event rates. The absolute rate of total non-hepatic cancer following DAA exposure was slightly higher than that following IFN exposure: 6.07 per 100 PY (95%CI: 5.78-6.38) vs 5.52 per 100 PY (95% CI: 5.26-5.79). However, after adjustment for covariates including age, gender, and baseline comorbidities and medication use, as well as propensity score weighting, DAA exposure was associated with a significantly reduced risk relative to IFN exposure (HR: 0.86, 95%CI: 0.80-0.93).
Table 19: Hazard ratios for non-hepatic cancer
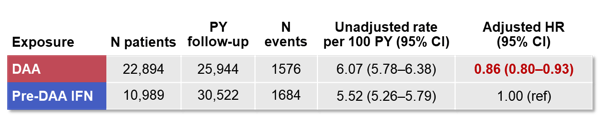
Figure 27 shows the Adjusted Total Non-Hepatic Cancer-Free Survival and demonstrates a significant reduction in risk of total non-hepatic cancer in the DAA era.
Figure 27: Adjusted Total Non-Hepatic Cancer-Free Survival
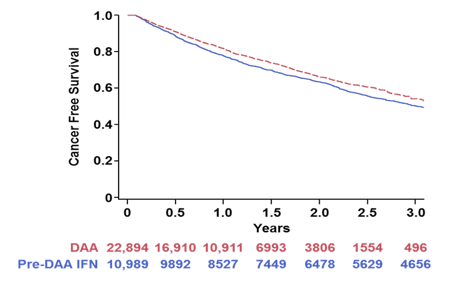
In conclusion, there is a reduction in the adjusted risk of total non-hepatic cancer in the DAA era. Adjusted HR is 0.86 in DAA-era vs 1.00 in the Pre-DAA era.
Risk of Total Non-hepatic Cancer Following Treatment for HCV Infection with Direct-acting Antiviral Agents - (04/16/18)
At this year EASL new data was also presented around SVR after DAA therapy and the risk for HCC occurrence or recurrence. Indeed, the real benefit of viral eradication after DAAs on disease progression, including HCC development, are still limited and controversial. The prospective study presented from Italy aimed to evaluate the HCC risk of DAA-treated cirrhotic patients in a large prospective cohort of DAA-treated HCV-cirrhotic patients (17). The main baseline demographics are listed below in table 20.
Table 20: Baseline demopgraphics by hstory of previous HCC
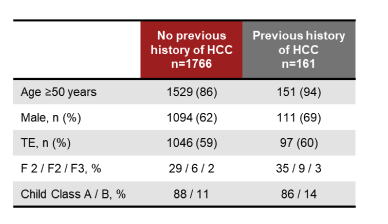
1,927 patients were included; 161 patients had a previous history of HCC. Most patients were in Child Pugh class A (88% without history of HCC and 86% of patients with previously treated HCC), and the mean MELD score was 8 in both groups. 1,832 patients (95%) achieved SVR. No difference in SVR rates was observed regardless the history of HCC. Of the 161 patients with past HCC, 38 developed tumor recurrence during the follow-up (incidence person-year 24.8%). 50/1,766 patients (2.8%) without a previous HCC history developed HCC during the follow-up (cumulative incidence p-year, 2.4%). SVR was confirmed as the strongest predictor of HCC incidence from the multivariate (HR 4.85; 95%CI: 2.25-4.69; p<0.0001) and varices (HR 2.41; 95%CI: 1.23-4.69; p<0.01). Figure 28 a and b shows in a Kaplan-meier curve the occurrence and recurrence incidence for HCC, respectively.
Figure 28a: Occurrance
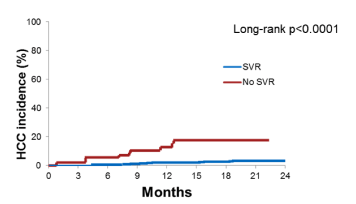
Figure 28b: Recurrance
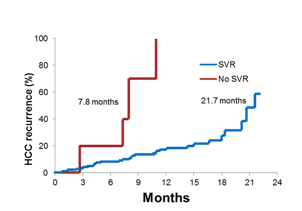
Figure 29 shows the HCC occurrence rate by SVR response and presence of varices. The presence of varices was associated with a higher HCC risk maybe as a reflection of more advanced liver disease stages.
Figure 29: HCC occurance per 100-years by SVR and varices status.
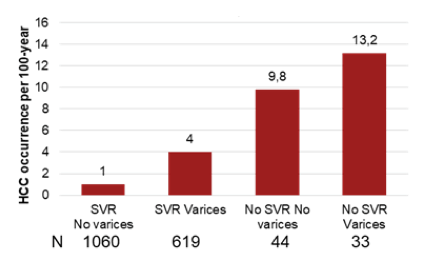
In summary, SVR was associated with a significant decrease of recurrent or de novo HCC in cirrhotic patients treated with DAA. 50/1,766 patients (2.8%) without a previous HCC history developed HCC during the follow-up (cumulative incidence p-year, 2.4%). SVR was confirmed as the strongest predictor of HCC incidence from the multivariate (HR 4.85; 95%CI: 2.25-4.69; p<0.0001) and varices (HR 2.41; 95%CI: 1.23-4.69; p<0.01).
SVR IS THE STRONGEST PREDICTOR OF OCCURRENCE AND RECURRENCE OF HEPATOCELLULAR CARCINOMA IN HCV CIRRHOTIC PATIENTS AFTER TREATMENT WITH DIRECT ACTING ANTIVIRALS: A PROSPECTIVE MULTICENTER ITALIAN STUDY. - (04/17/18)
Micro to macro-elimination: More good news to share....
Various sessions and presentations at EASL addressed issues around micro-elimination. In particular, well-identified patient groups such as hemophiliacs or HIV/HCV coinfected patients are ideal cohorts for attempting HCV elimination. In addition, countries with low disease burden and small population numbers are low hanging fruits for HCV elimination. At this year EASL an update was provided on the HCV elimination project from Iceland. It has been estimated that there are around 800-1000 HCV-infected individuals in Iceland out of a total population from 330.000. Overall, 80% of individuals with HCV have already been diagnosed. A Nationwide treatment program has been initiated in January 2016, aiming for elimination of HCV infection as a public health threat (Treatment as prevention TraPHepC). Vogur Addiction Hospital, a key sentinel site where most PWID in Iceland seek treatment provides an excellent opportunity to monitor trends in HCV prevalence among PWID. Treatment was initially with sofosbuvir/ledipasvir +/- ribavirin and more recently since end of 2016 sofosbuvir/velpatasvir. HCV cure rates have been high as 90% and even 94% for those individuals who completed their HCV therapy. Figure 30 shows the decline in number of HCV positive PWIDS from Vogur Addiction Hospital after increased roll-out of DAA therapy. Indeed the HCV prevalence among PWID, which was 42.6% in 2015 for those individuals admitted for addiction treatment prior to TraP HepC, dropped to 11.6% in 2017, thereby representing a 73% reduction (p<0.001).
Figure 30: Number of HCV positive patients at Vogur Hospital over time.
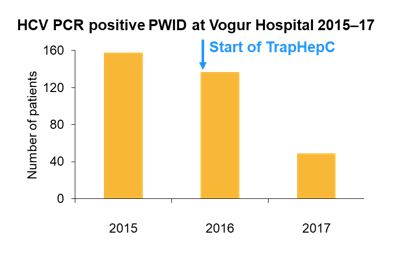
In summary, a major scale-up in HCV treatment for all patient groups has been successfully initiated in Iceland, which has already translated into a significant reduction in HCV prevalence among PWIDs.
Marked reduction in prevalence of hepatitis C viremia among people who inject drugs (PWID) during 2nd year of the Treatment as Prevention (TraPHepC) program in Iceland - (04/24/18)
An update on the much larger national HCV elimination program from Georgia was also presented in Paris. Georgia has an estimated population of 3.7 million with an estimated number of HCV-infected and HCV-RNA positive individuals of around 150.000 which leads to an overall HCV prevalence of 5.4% which is obviously quite high. The special situation in Georgia is the extreme political will also from Government side to achieve HCV elimination and the partnering with Gilead who have agreed to supply HCV drugs for free to the country for achieving HCV elimination. In order to develop a successful elimination plan, which includes increased testing and improving linkage to care, Georgian doctors and politicians have teamed up with many other international partners under the leadership of the American CDC to make their dream of HCV elimination become reality. The overall goal is to reduce the HCV prevalence by 90% (to 0.5%) by 2020 in Georgia. In Paris data from the hepatitis C care cascade were presented 3 years after starting the national Georgian hepatitis C elimination program. The cascade of care as of 31st March 2018 is shown in figure 31.
Figure 31: HCV Cascade of care in Georgia 03/2018
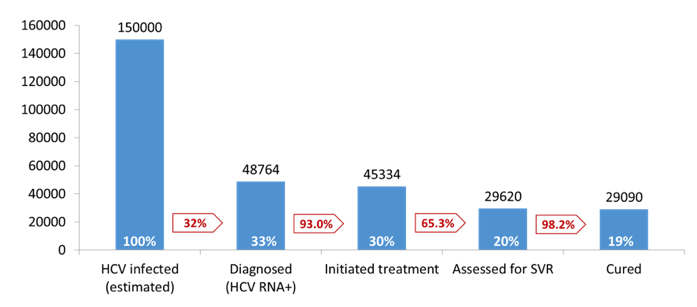
It is amazing to see how well linkage of care works for those diagnosed for HCV, with 93% overall initiating HCV therapy after diagnosis. Also, HCV cure rates are impressive with over 98%. From April 2015 until March 2016 IFN-containing and IFN-free SOF regimens were recommended based on various clinical scenarios (genotype, cirrhosis, previous treatment experience). From April 2016 onwards sofosbuvir/ledipasvir was used for treatment of all genotypes. In Georgia 34% of HCV infections are with genotype 3. In Europe however, sofosbuvir/ledipasvir is not recommended for GT3 treatment. Most interestingly, however cure rates in GT3 patients were highest with the LDV/SOF/RBV combination. Treatment outcome by regimen for GT3 is depicted in figure 32.
Figure 32: Treatment outcomes of SOF and LDV/SOF in Genotype 3 Patients with Complete SVR Data, Apr 2015 - Mar 2018.
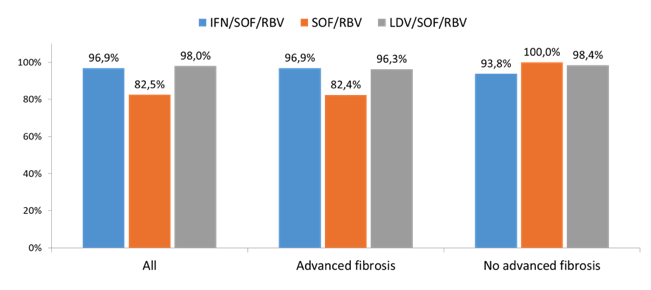
In summary, the Georgian hepatitis C treatment model ensures high cure rates already exceeding national elimination target for treatment with LDV/SOF, even without newer generation DAAs. Indeed, LDV/SOF proved to be highly effective in genotypes 2 and 3. Scaling-up testing and diagnosis, along with effective linkage to treatment services are however needed, to achieve the goal of elimination.
Hepatitis C Care Cascade in the Country of Georgia After 3 years of Starting National Hepatitis C Elimination Program - (04/24/18)
Indeed, in many countries despite unlimited access to modern DAA therapy, the main challenge remains the diagnosis of people living with HCV who are unaware of their diagnosis. In order to monitor changes in patient populations and patient characteristics it appears appealing similar to HIV to evaluate whether changes in the amount of patients with late presentation occurs. In order to evaluate the extent and reasons of late presentation and implement strategies to face it in the context of viral hepatitis, two consensus definitions of late stage and advanced liver disease had been developed recently by a group of viral hepatitis experts (20). To determine whether the widespread usage of direct acting antivirals (DAAs) has led already to a reduction in HCV infected patients presenting with advanced liver disease at the time of treatment initiation in Germany, data derived from the German Hepatitis C Cohort (GECCO) was analyzed (21). Treatment naive HCV infected patients initiating DAA-based treatment between January 2014 and September 2017 were included. Advanced liver disease was defined by APRI-Score ≥1.5, METAVIR ≥ F3 or FibroScan ≥ 9.5kPa. Late presentation over time was analyzed for each year. Risk factors for late presentation were evaluated. The number of treatment-naïve patients initiating DAA-based treatment by year is shown below in figure 33.
Figure 33: Treatment-naïve patients initiating DAA-based treatment within the German GECCO Cohort.
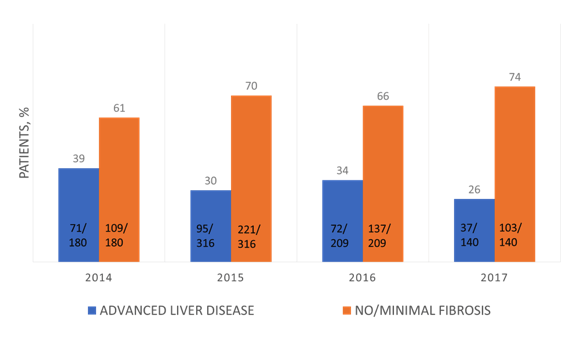
653 HCV monoinfected and 210 HIV/HCV coinfected patients were included. 65.5% were male; mean age was 48.6 ± 12.7 years. Overall, 32.5% (275/845) of patients had advanced liver disease with 15.4% (130/845) having liver cirrhosis. In 2014 39.4% (71/180) of patients presented with advanced liver disease, decreasing to 30.1% (95/316), 34.4% (72/209) and 26.4% (37/140) in the years 2015, 2016 and 2017 (p= 0.057). These results clearly indicate that so far no significant change in the number of late presenters has occurred suggesting that still many patients have remained undiagnosed in Germany even with late disease stages. Of note, patients with and without advanced liver disease differed in age (p< 0.0001), genotype (p= 0.005), transmission route (p= 0.047), CD4 cell count (p= 0.027) and time from diagnosis to treatment initiation (p= 0.007). In the multivariable logistic regression analysis GT 3 remained an independent risk factor for presentation with advanced liver disease (p= 0.042). A decrease in HIV coinfection was observed among patients with advanced liver disease initiating DAA-based treatment comparing the years 2014-2017 (p≤0.0001). The proportion of patients being infected with GT3 and intravenous drug users presenting with advanced liver disease increased significantly over time. This suggests that treatment uptake in the coinfected patients has been particularly high which makes sense as their HCV status is well known and that more recently increasingly IVDUs with GT3 are being treated potentially also because more broadly active DAA combinations have become available particularly for GT3 patients. In summary, the proportion of HCV infected patients starting DAA treatment with advanced liver disease remained high during the observation period, highlighting the need for broader screening and prevention measures.
Has increased rollout of direct acting antiviral therapy decreased the burden of late presentation and advanced liver disease in patients starting Hepatitis C Virus therapy in Germany? - (05/04/18)
Summary
• A high SVR12 rate of 97% with no virologic failures to date was reported in patients with HCV GT1-6 infection treated with G/P in a large German real-world cohort.
• Eight weeks of SOF/VEL is highly effective in GT3 infected patients with significant (F2/3) fibrosis. Patients on daily supervised OST have excellent SVR rates when given DAAs along with OST.
• An 8-week treatment regimen of EBR/GZR in participants with HCV GT4 infection showed high rates of SVR (93%) among treatment-naive participants with mild to moderate (F0-F2) fibrosis. 2 participants however, developed relapse. Final results from the 8-week arm plus outcomes in participants treated for 12 weeks will provide further information regarding the effective use of EBR/GZR in participants with HCV GT4 infection.
• GT3 HCV-infected patients with cirrhosis have high overall rates of SVR12 after treatment with SOF/VEL with or without RBV. Among those with baseline NS5A RASs and cirrhosis, the addition of RBV to 12weeks of SOF/VEL led to numerically higher SVR rates.
" G/P achieves high SVR12 rates in genotype 5 or 6 infection.
• LDV/SOF was well tolerated and effective in a predominant GT 4 population in Rwanda. Study results are very encouraging for DAA introduction and scale-up in Rwanda and other limited resource settings.
• High SVR rates could be achieved in both OST and non-OST patients. Alcohol or cannabis consumption did not diminish cure rates in PP analysis. However, LTFU is more likely in patients with a high alcohol consumption or current or former drug use than in patients without drug history.
• Preliminary data from this study show that HCV-infected patients who experienced virological failure following G/P treatment can achieve high SVR12 rates with G/P + SOF + RBV. Overall, the combination of G/P + SOF + RBV was well tolerated.
• Patients with HCV GT1 infection who experienced virologic failure following NS5A+ SOF +/- RBV therapy achieved an overall high SVR4 rate of 95% with GP retreatment despite high rates of baseline NS5A RAS. Lower efficacy and tolerability was observed for the combination of G/P plus RBV given for 12 weeks in compensated cirrhotics (SVR4 rate 86%).
• Patients with SVR to a DAA regimen have a better survival outcome than non-responders at all stages of liver disease. Eradication of HCV in patients with CHILD A cirrhosis reduces the risk of liver events and increases survival in comparison to non-SVR.
• Subjects with Child B cirrhosis retain a significant risk of HCC, hepatic decompensation and death after HCV eradication.
• Deaths linked to cardiovascular disease are reduced after viral eradication regardless of the stage of liver fibrosis.
• There is a reduction in the adjusted risk of total non-hepatic cancer in the DAA era. Adjusted HR is 0.86 in DAA-era vs 1.00 in the Pre-DAA era.
• SVR is associated with a significant decrease of recurrent or de novo HCC in cirrhotic patients treated with DAA.
• a major scale-up in HCV treatment for all patient groups has been successfully initiated in Iceland, which has already translated into a significant reduction in HCV prevalence among PWIDs.
• The Georgian hepatitis C treatment model ensures high cure rates already exceeding national elimination target for treatment with LDV/SOF, even without newer generation DAAs. Scaling-up testing and diagnosis, along with effective linkage to treatment services are however needed to achieve the goal of elimination.
• In Germany the proportion of HCV infected patients starting DAA treatment with advanced liver disease remained high between 2014-2017, highlighting the need for broader screening and prevention measures.
References
1. Runarsdottir V et al. Marked reduction in the prevalence of hepatitis C viremia among people who inject drugs (PWID) during 2nd year of the Treatment as Prevention (TraP HepC) program in Iceland. 53rd EASL; Paris, France; April 11-15, 2018. Abstract PS-095
2. Berg T, et al. First real-world data on safety and effectiveness of glecaprevir/pibrentasvir for the treatment of patients with chronic hepatitis C virus infection: data from the German Hepatitis C-Registry. 53rd EASL; Paris, France; April 11-15, 2018. Abstract GS-007
3. D'Ambrosio R et al. Real-Life Effectiveness and Safety of Glecaprevir/Pibrentasvir Among 723 Patients with Chronic Hepatitis C: The NAVIGATOR-II Study - Interim Analysis. 53rd EASL; Paris, France; April 11-15, 2018. Abstract GS-013
4. Boyle A, et al. 8 weeks sofosbuvir/velpatasvir in genotype 3 patients with significant fibrosis: Highly effective amongst an OST cohort. 53rd EASL; Paris, France; April 11-15, 2018. Abstract PS-034
5. Asselah T, et al. Efficacy and safety of 8 weeks of elbasvir/grazoprevir in HCV GT4-infected treatment-naïve participants. 53rd EASL; Paris, France; April 11-15, 2018. Abstract GS-006
6. Asselah T, et al. Efficacy of elbasvir and grazoprevir in participants with hepatitis C virus genotype 4 infection: A pooled analysis. Liver Int. 2018 Feb 20. doi: 10.1111/liv.13727. [Epub ahead of print]
7. Buti M, et al. Safety and Efficacy of Sofosbuvir/Velpatasvir with and without Ribavirin in Genotype 3 HCV-Infected Patients with Cirrhosis. 53rd EASL; Paris, France; April 11-15, 2018. Abstract PS-035
8. Asselah T, et al. Efficacy and Safety of Glecaprevir/Pibrentasvir in Patients with HCV Genotype 5 or 6 Infection: The ENDURANCE-5,6 Study 53rd EASL; Paris, France; April 11-15, 2018. Abstract GS-012
9. Gupta N, et al. Direct-acting antiviral treatment in sub-Saharan Africa: A prospective trial of Ledipasvir/Sofosbuvir for chronic Hepatitis C infection in Rwanda (the SHARED study). 53rd EASL; Paris, France; April 11-15, 2018. Abstract PS-090
10. Christiansen S, et al. Scaling up HCV-DAA treatment in patients on opioid substitution therapy - does alcohol or cannabis consumption diminish cure rates? Data from the German Hepatitis C Registry (DHC-R). 53rd EASL; Paris, France; April 11-15, 2018. Abstract PS-036
11. Wyles D, et al. Retreatment of patients who failed glecaprevir/pibrentasvir treatment for hepatitis C virus infection. 53rd EASL; Paris, France; April 11-15, 2018. Abstract PS-040
12. Bourlière M, et al.: POLARIS-1 and POLARIS-4 Investigators. Sofosbuvir, Velpatasvir, and Voxilaprevir for Previously Treated HCV Infection. N Engl J Med. 2017;376:2134-2146.
13. Lok A, et al. A phase 3b, open-label, randomized, pragmatic study of glecaprevir/pibrentasvir +/- ribavirin (RBV) for HCV genotype 1 subjects who previously failed an NS5A Inhibitor + sofosbuvir (SOF) therapy. 53rd EASL; Paris, France; April 11-15, 2018. Abstract LBO-008
14. Mangia A, et al. Long-term follow-up of patients with chronic HCV infection and compensated or decompensated cirrhosis following treatment with sofosbuvir-based regimens. 53rd EASL; Paris, France; April 11-15, 2018. Abstract GS-018
15. Calvaruso V, et al. Disease outcomes after DAA-induced SVR: data from the resist-HCV cohort. 53rd EASL; Paris, France; April 11-15, 2018. Abstract PS-149
16. Chokkalingam A, et al. Risk of total non-hepatic cancer following treatment for HCV infection with direct-acting antiviral agents. 53rd EASL; Paris, France; April 11-15, 2018. Abstract PS-155
17. Lleo A, et al. SVR is the strongest predictor of occurrence and recurrence of hepatocellular carcinoma in HCV cirrhotic patients after treatment with DAAs: a prospective multi-centric Italian study. 53rd EASL; Paris, France; April 11-15, 2018. Abstract PS-154
18. Tyrfingsson T, et al. Marked reduction in prevalence of hepatitis C viremia among people who inject drugs (PWID) during 2nd year of the Treatment as Prevention (TraPHepC) program in Iceland. 53rd EASL; Paris, France; April 11-15, 2018. Abstract PS-095
19. Tsertsvadze T, et al. Hepatitis C Care Cascade in the Country of Georgia After 3 years of Starting National Hepatitis C Elimination Program. 53rd EASL; Paris, France; April 11-15, 2018. Abstract PS-096
20. Mauss S, et al. Late presentation of chronic viral hepatitis for medical care: a consensus definition. BMC medicine. 2017;15:92
21. Rockstroh J, et al. Has increased rollout of direct acting antiviral therapy decreased the burden of late presentation and advanced liver disease in patients starting Hepatitis C Virus therapy in Germany? 53rd EASL; Paris, France; April 11-15, 2018. Abstract THU-432
|
| |
|
 |
 |
|
|