 |
 |
 |
| |
Multimorbidity and risk of death differs by gender in people living with HIV in the Netherlands - the ATHENA cohort study
|
| |
| |
Reported by Jules Levin
Glasgow Oct 28-31 2018
Ferdinand Wit1,2, Marc van der Valk2, Jet Gisolf3, Wouter Bierman4,
Peter Reiss1,2 on behalf of the ATHENA HIV observational cohort study
1. Stichting HIV Monitoring, Amsterdam
2. Academic Medical Center, Amsterdam
3. Rijnstate Hospital, Arnhem
4. University Medical Center Groningen, Groningen
The Netherlands
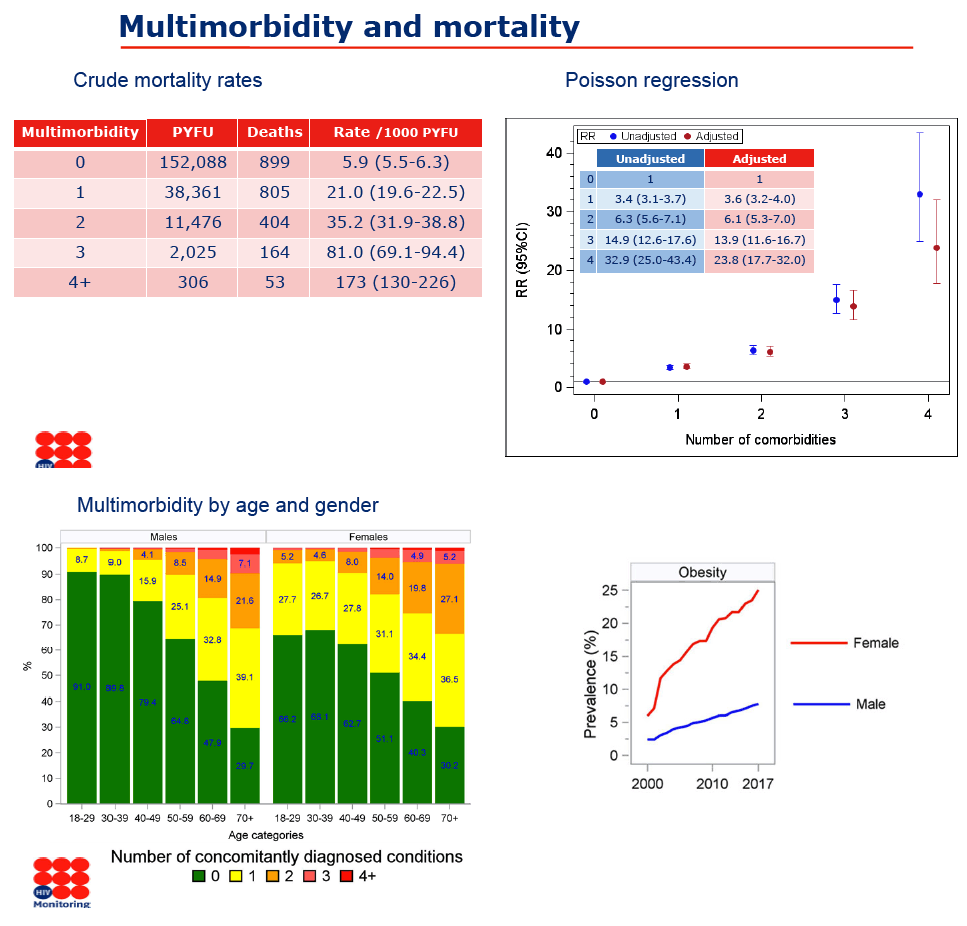
Authors conclude: MULTI-MORBIDITY is strongly & independently associated with mortality"
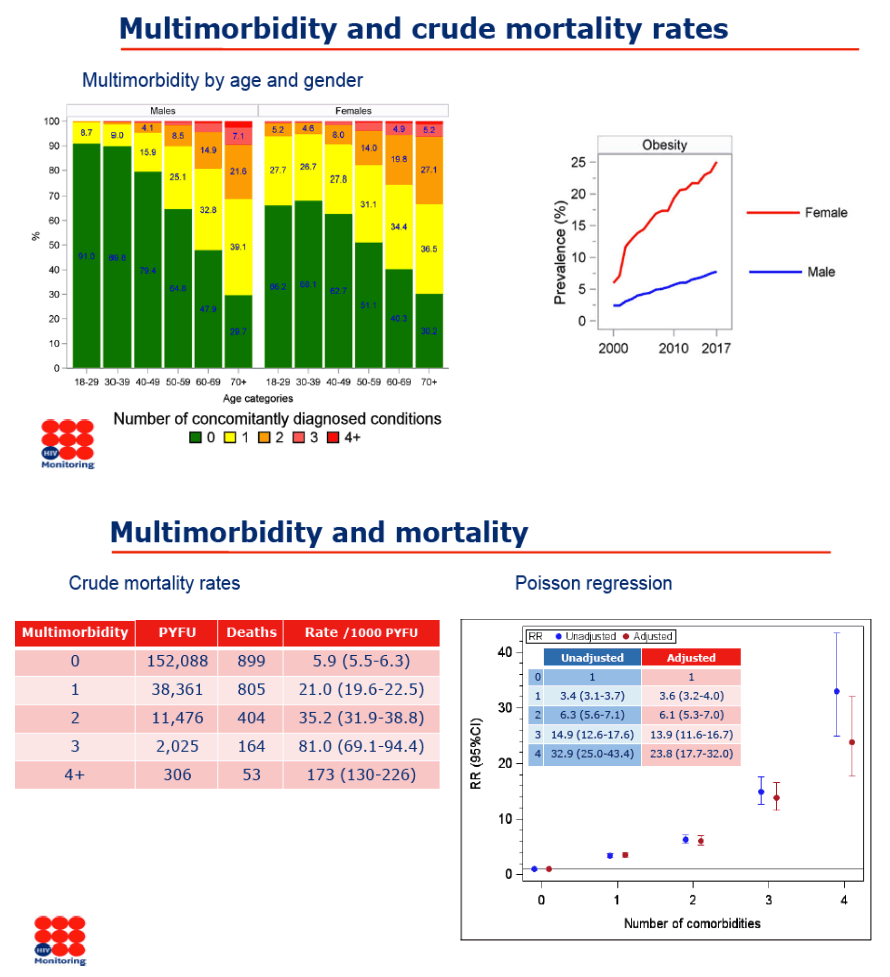
take note of these 3 slides: the 1st shows 23.8 fold INCREASED risk for death after adjustment so 32.9 fold increased risk before adjustment with 4 comorbidities. with 3 comorbidities death risk increased 13.9 fold, with 2 comorbidities death risk increased 6.1 fold, and with only 1 death risk increased 3.6 fold. Death rate was 5.9/1000 patient years followup with zero comorbdities, increasing to 21.0, 35.2, 81.0, and 173 when there were 1, 2, 3, and 4+ comorbidities present, so death rates increased with each additional comorbidity.
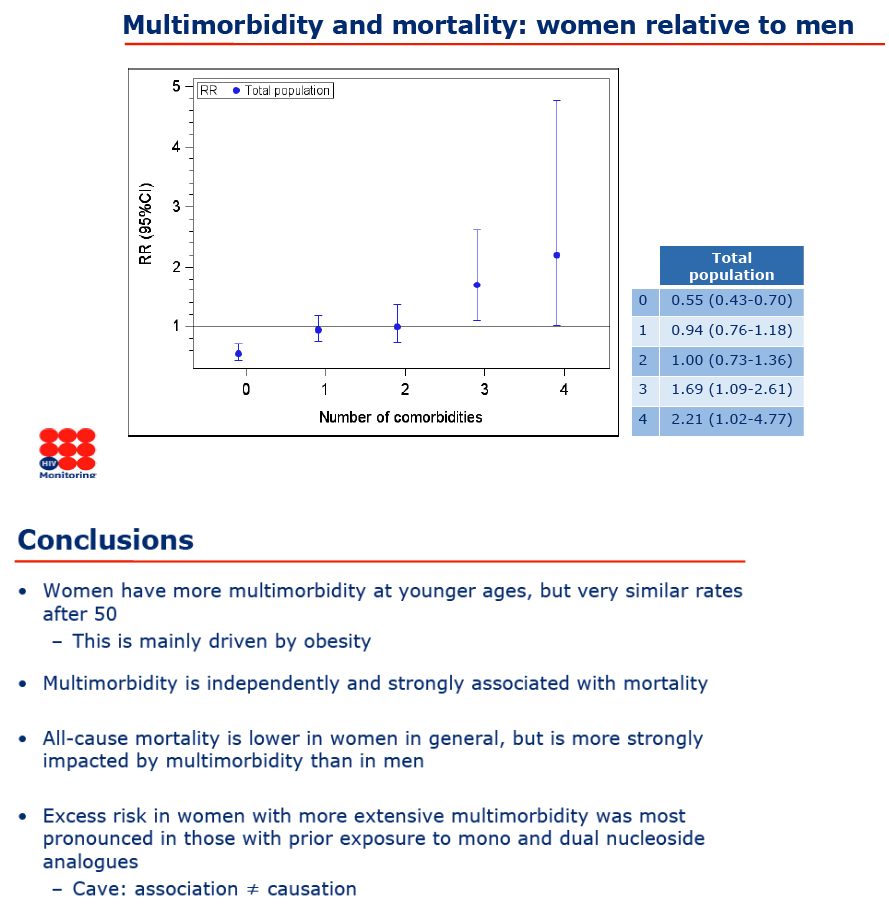
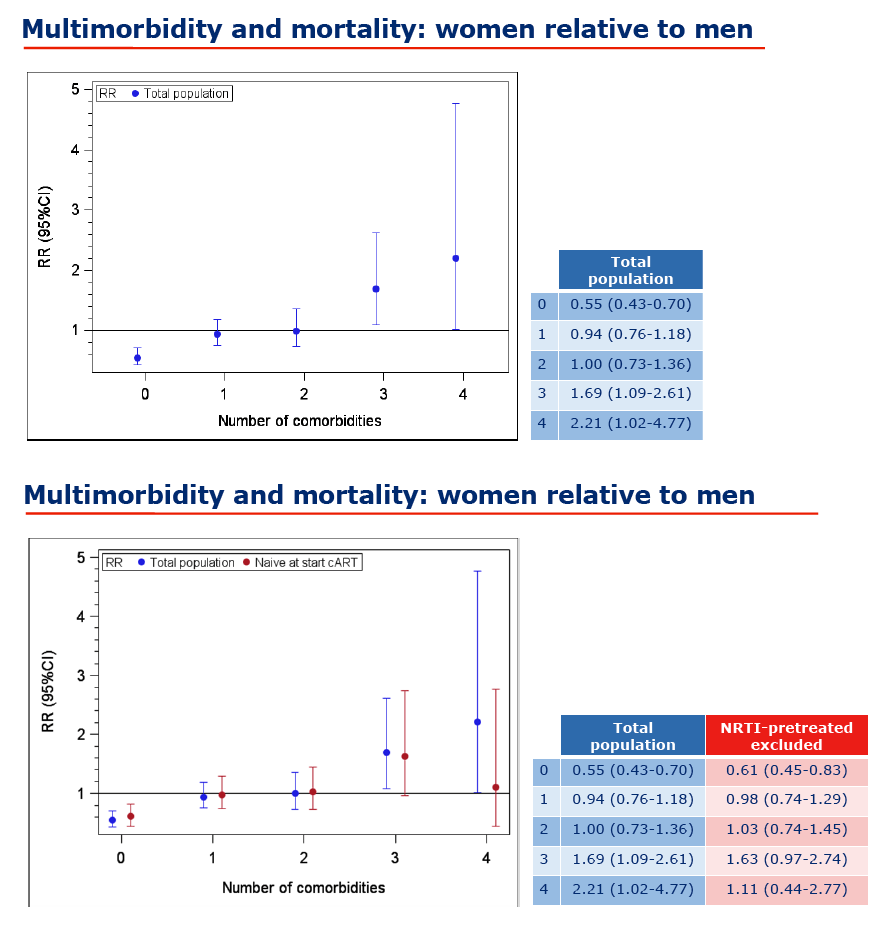
In the 2nd slide just below more women from 18-69 ages than men had 1, 2, 3, or 4 comorbidities. In the 3rd slide just below you see women 3 or 4 comorbidities had 69% and 121% greater death rates compared to men.

program abstract
Multimorbidity and risk of death differs by gender in people living with HIV in the Netherlands: the ATHENA cohort study
F Wit1; M van der Valk2; J Gisolf3; W Bierman4 and P Reiss2 1Stichting HIV Monitoring, Academic Medical Center, Amsterdam, Netherlands. 2Department of Internal Medicine, Academic Medical Center, Amsterdam, Netherlands. 3Department of Internal Medicine, Rijnstate Ziekenhuis, Arnhem, Netherlands. 4Department of Internal Medicine - Infectious Diseases, University Medical Center Groningen, Groningen, Netherlands
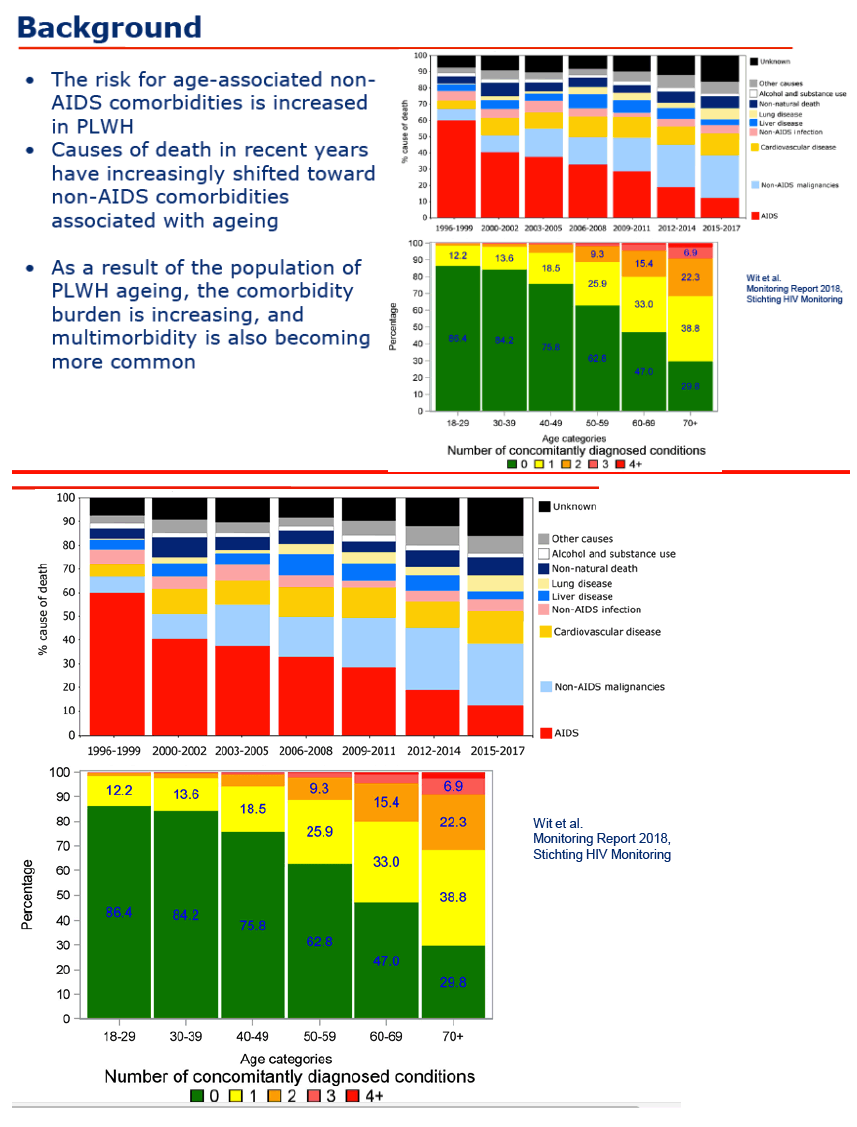
Background: PLWHIV on cART are living longer and because of aging are experiencing more non-AIDS comorbidities, which have become the most common cause of death in PLWHIV on cART. We investigated if multimorbidity predicts mortality in PLWHIV on cART and whether this differs by gender. Materials and methods: We used data from PLWHIV from the ATHENA cohort collected from 2000 to 2016. Comorbidities identified were: cardiovascular disease; stroke; non-AIDS malignancies, excluding non-melanoma skin cancers and pre-malignant cervical/anal lesions; moderate-severe chronic kidney disease (eGFR <30 mL/min
≥6 months, Grade ≥G3b); diabetes mellitus; hypertension (use of antihypertensives or blood pressure ≥160/100 mmHg); obesity (BMI >30). Poisson regression compared mortality between genders adjusting for demographics, traditional risk factors and HIV-related parameters.
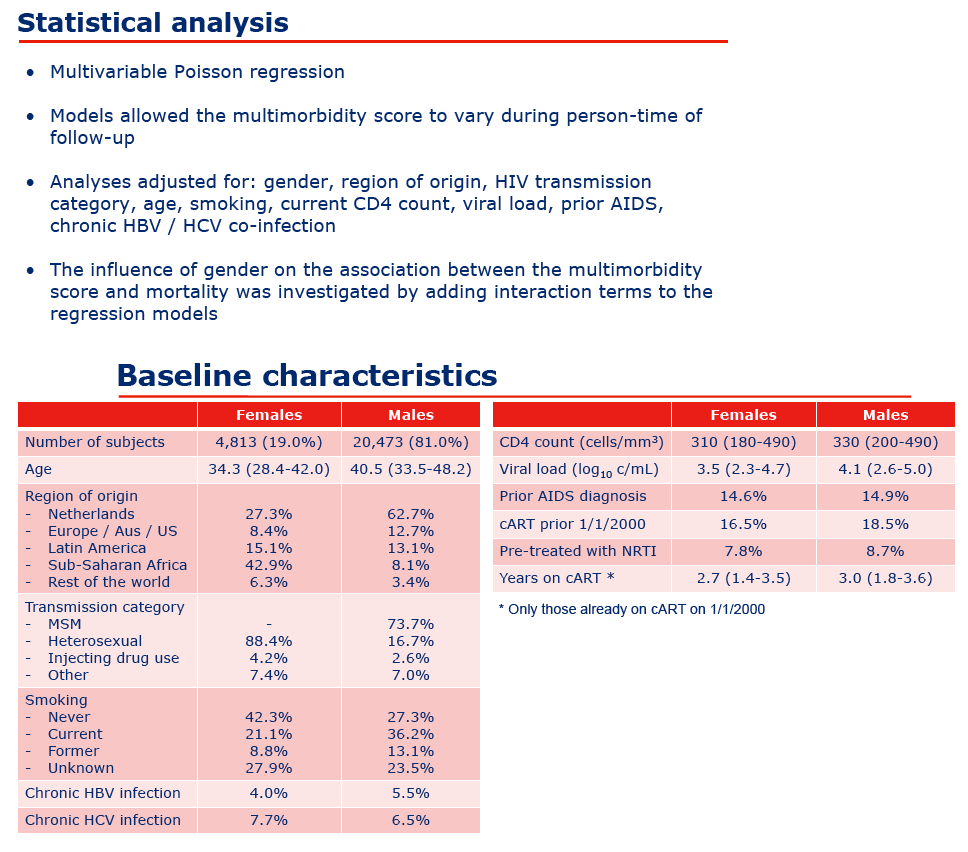
Results: Data from 24,383 PLWHIV (19.2% females) were included (see Table 1). At cART initiation the mean number of non-AIDS comorbidities in males (0.26) and females (0.25) were similar (p = 0.34). At last available follow-up in 2016 the mean number of comorbidities had increased in both males (0.59) and females (0.59), p = 0.18. Mortality risk increased with number of comorbidities, from 6.83 deaths per 1000 person-years in PLWHIV with zero comorbidities, to 13.8, 28.2, 65.6 and 139 per 1000 person-years with 1, 2, 3, ≥4 comorbidities, respectively. Poisson regression confirmed the relationship between multimorbidity and mortality: risk ratio (RR) 2.66 (2.54 to 2.79) per additional comorbidity. Overall mortality risk, adjusted for the number of comorbidities, was significantly lower in women than men (RR 0.78 [0.67 to 0.91], p = 0.002). However, there was a significant interaction between gender, number of comorbidities and mortality (p < 0.0001) with the RR for women compared to men, ranging from 0.57 (0.45 to 0.74), to 0.75 (0.59 to 0.95), to 1.00 (0.74 to 1.38), to 1.52 (1.00 to 2.32), and 1.77 (0.83 to 3.78) for those with 0, 1, 2, 3, ≥4 comorbidities. Every individual comorbidity, except non- AIDS malignancies, carried excess mortality risk for women. Excess mortality in women with more extensive multimorbidity was driven partly by exposure to mono- and dual nucleoside analogues before the cART era, as the increased risk attenuated and lost statistical significance after excluding PLWHIV pre-treated with nucleoside analogues before start of cART: RR for women compared to men at three and four comorbidities were 1.39 (0.87 to 2.23) and 1.17 (0.47 to 2.91), respectively.
Conclusions: Multimorbidity was a strong independent predictor of mortality in adult PLWHIV. Although women in general and especially women with less than three comorbidities had lower mortality than men, their risk was reversed and increased compared to men when experiencing three or more comorbidities.


|
| |
|
 |
 |
|
|