 |
 |
 |
| |
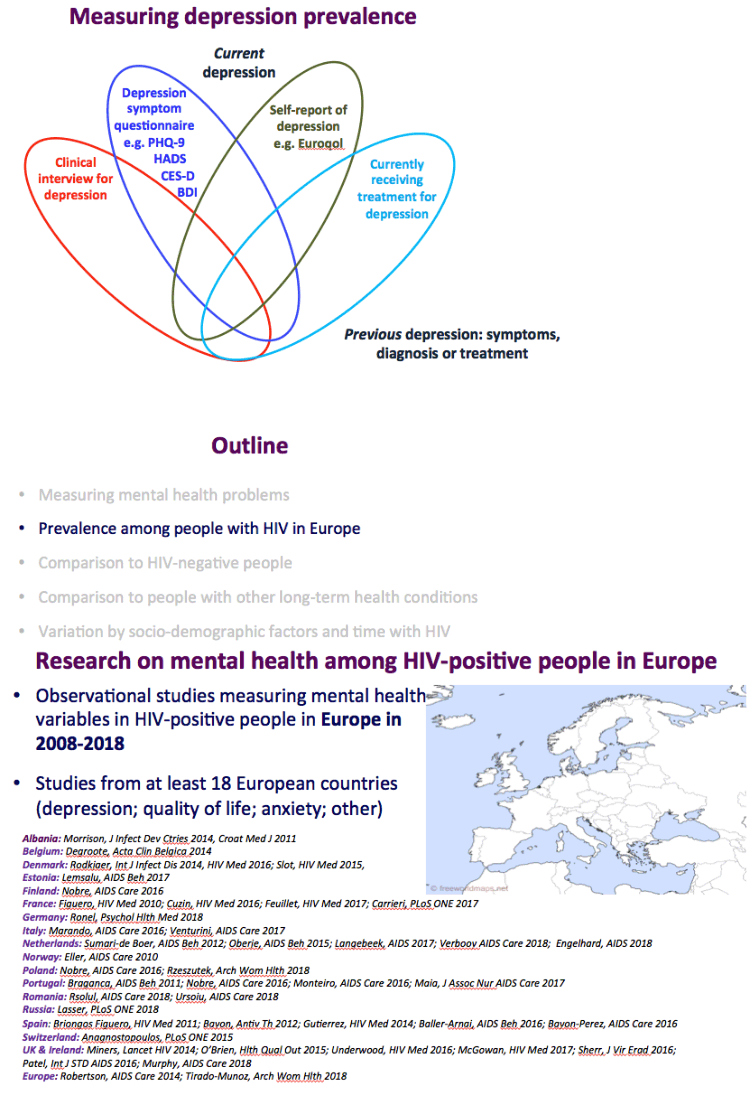
Prevalence of mental health problems
among people living with HIV:
|
| |
| |
Reported by Jules Levin
HIV Drug Therapy, Glasgow 2018, October 28-31, 2018, Glasgow
Fiona Lampe
Institute for Global Health, University College London
Pdf talk attached
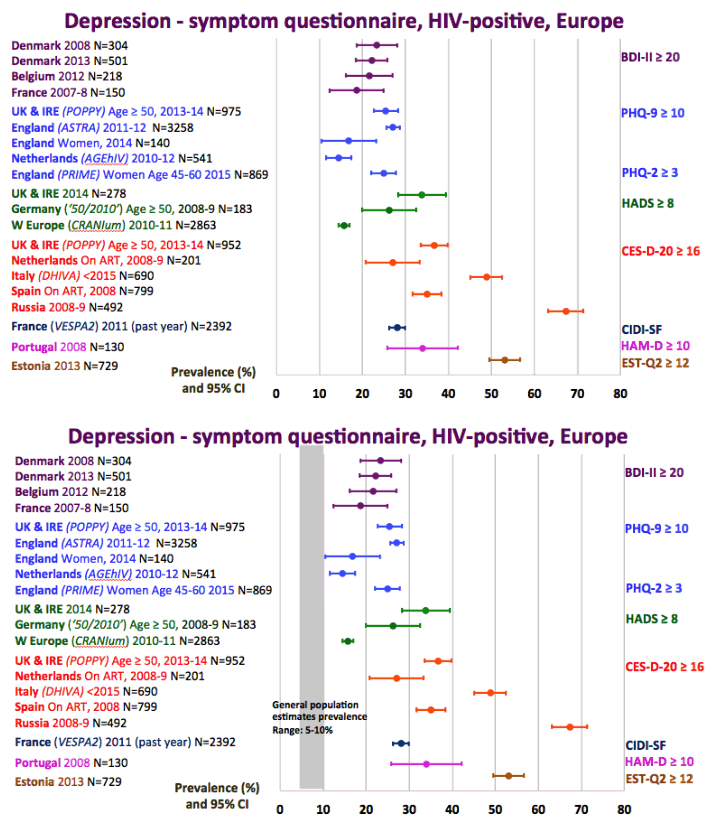
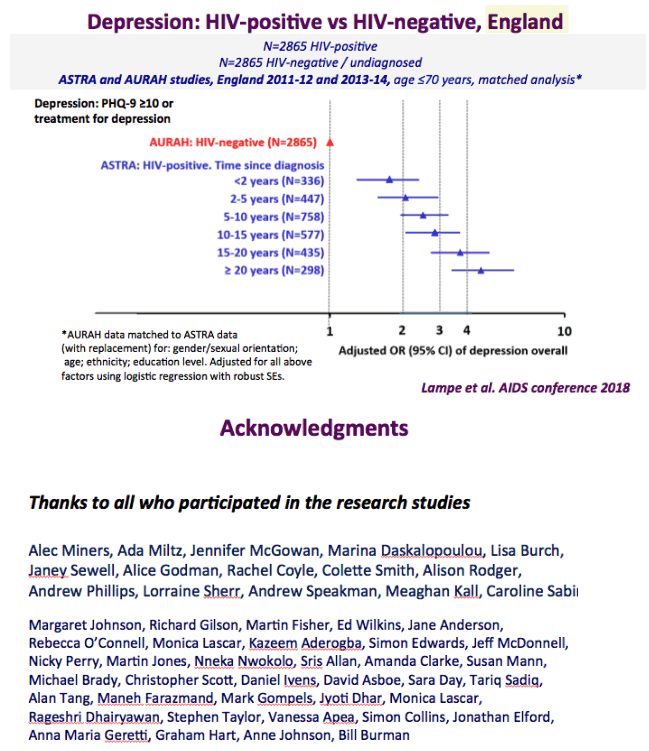
4 Times Higher Rates of Depression among HIV+ compared to General Population.....in this graph
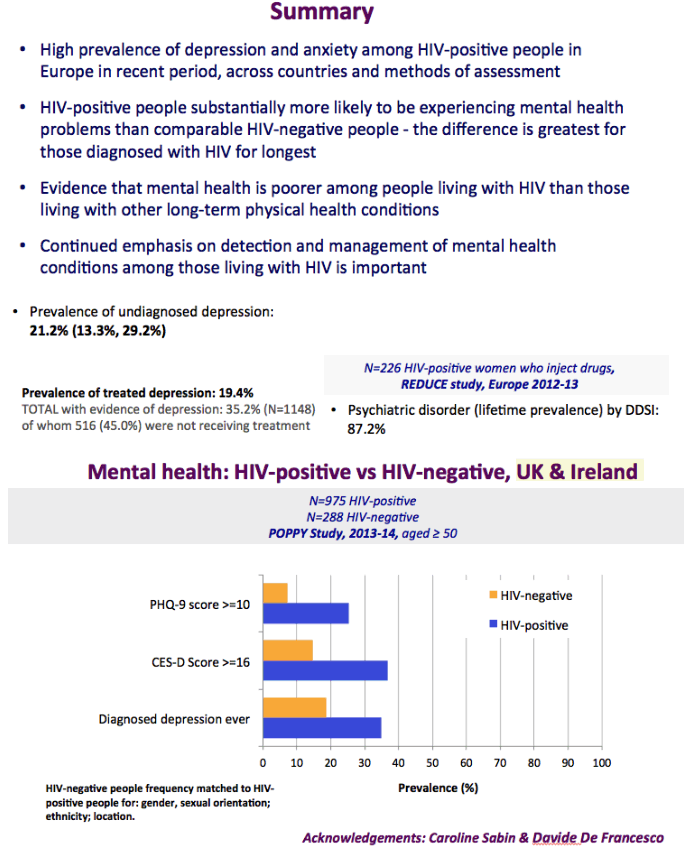
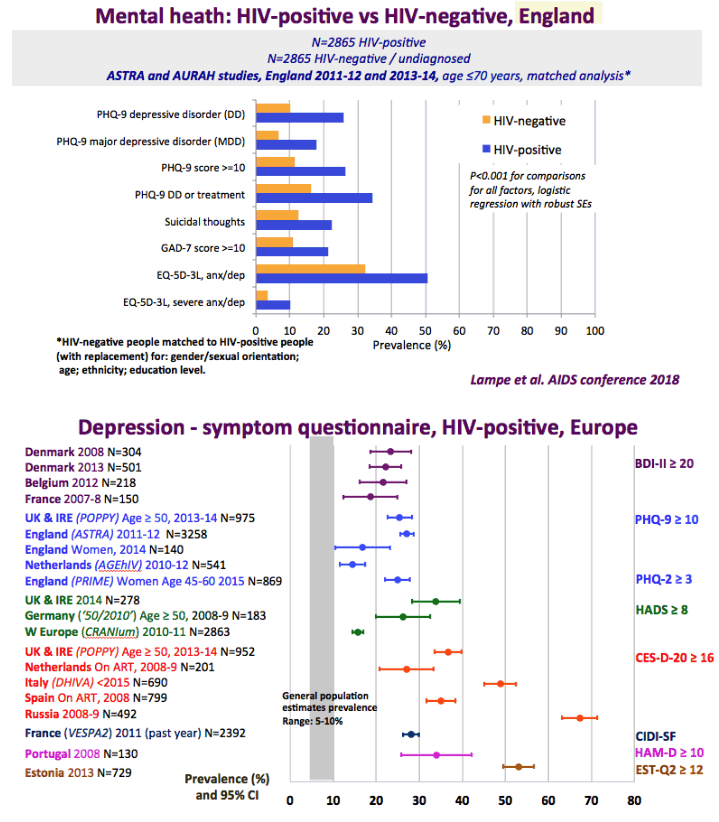
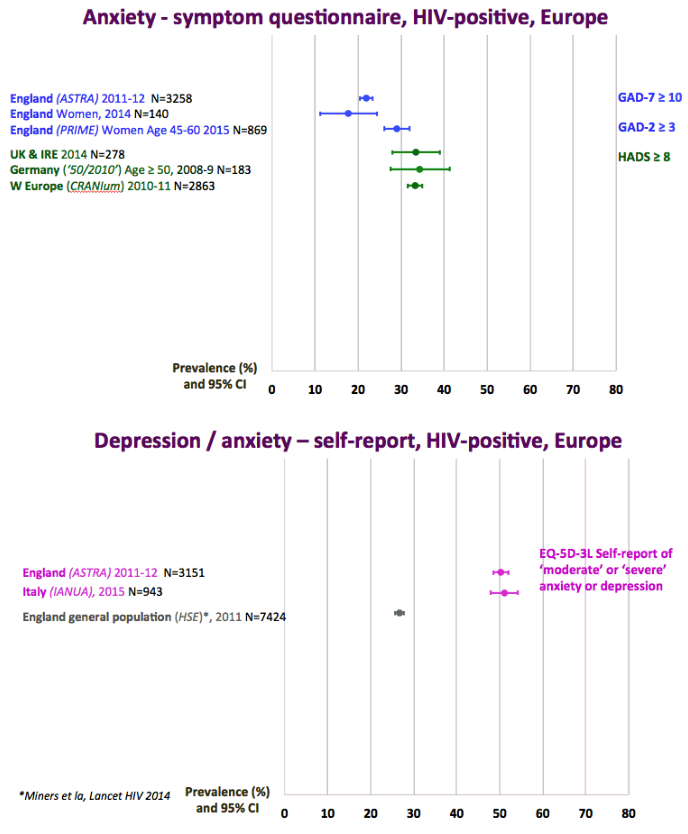
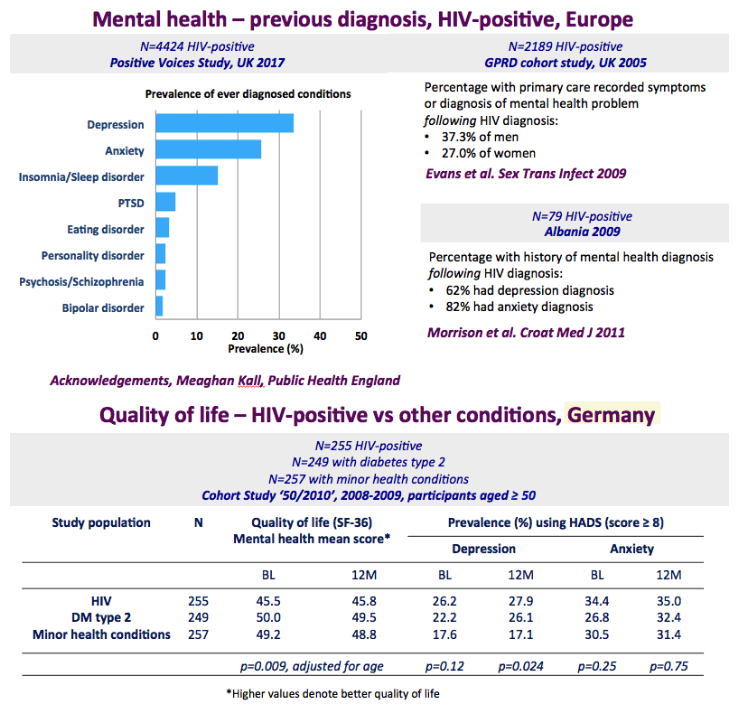
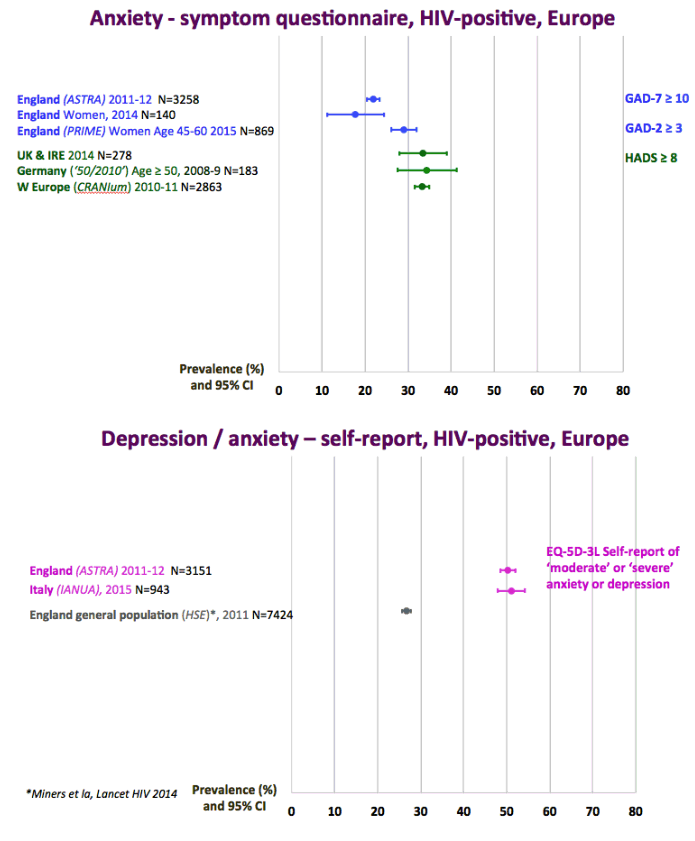
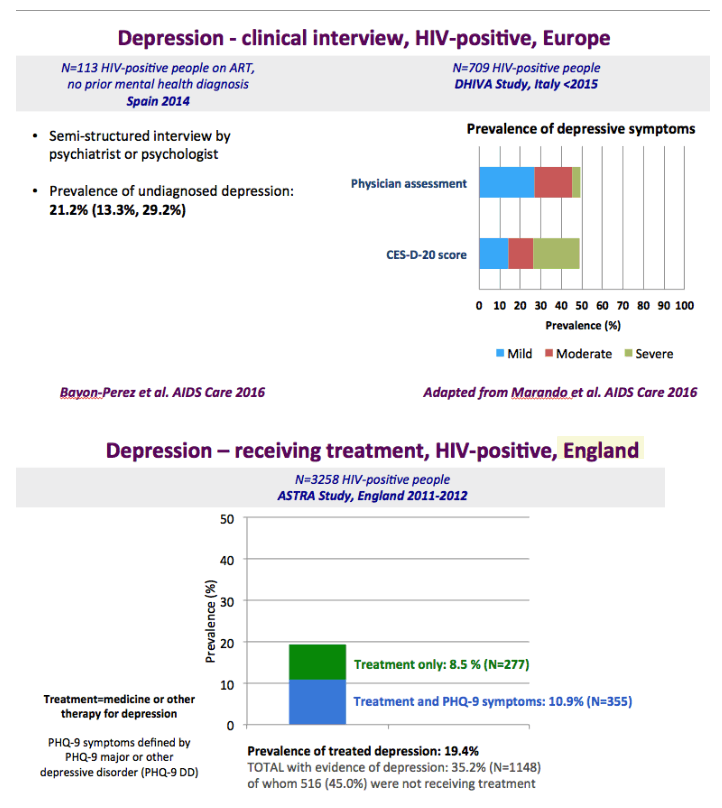
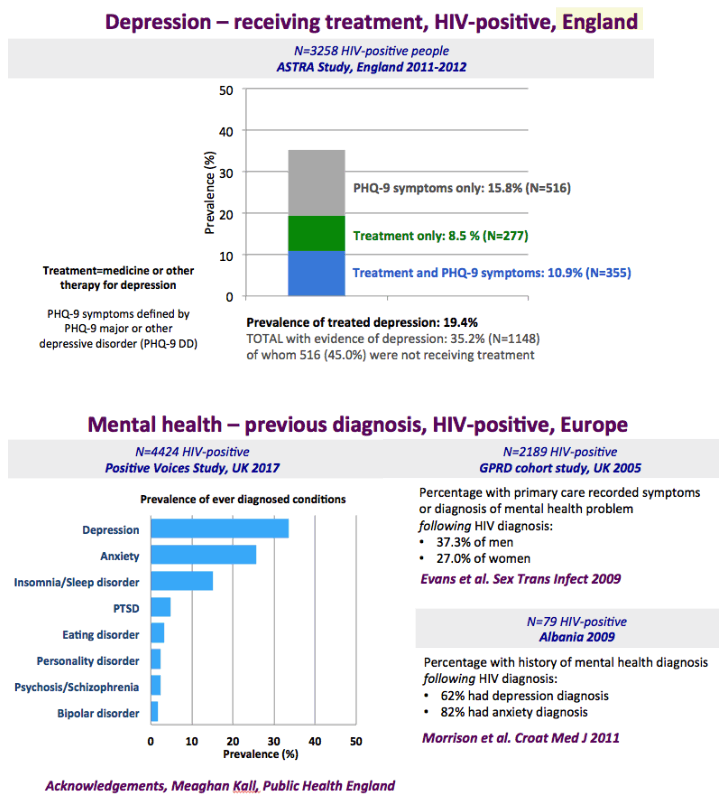
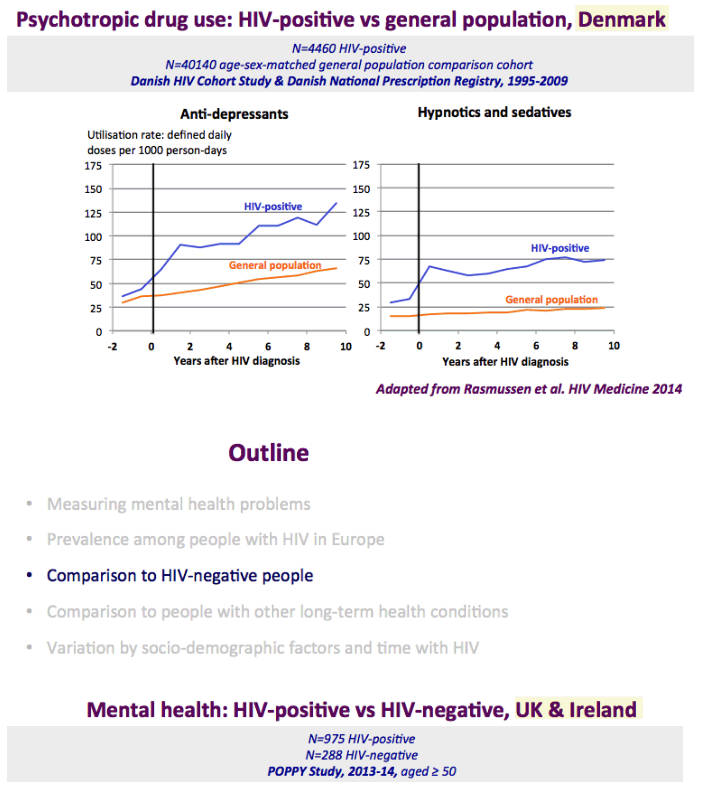
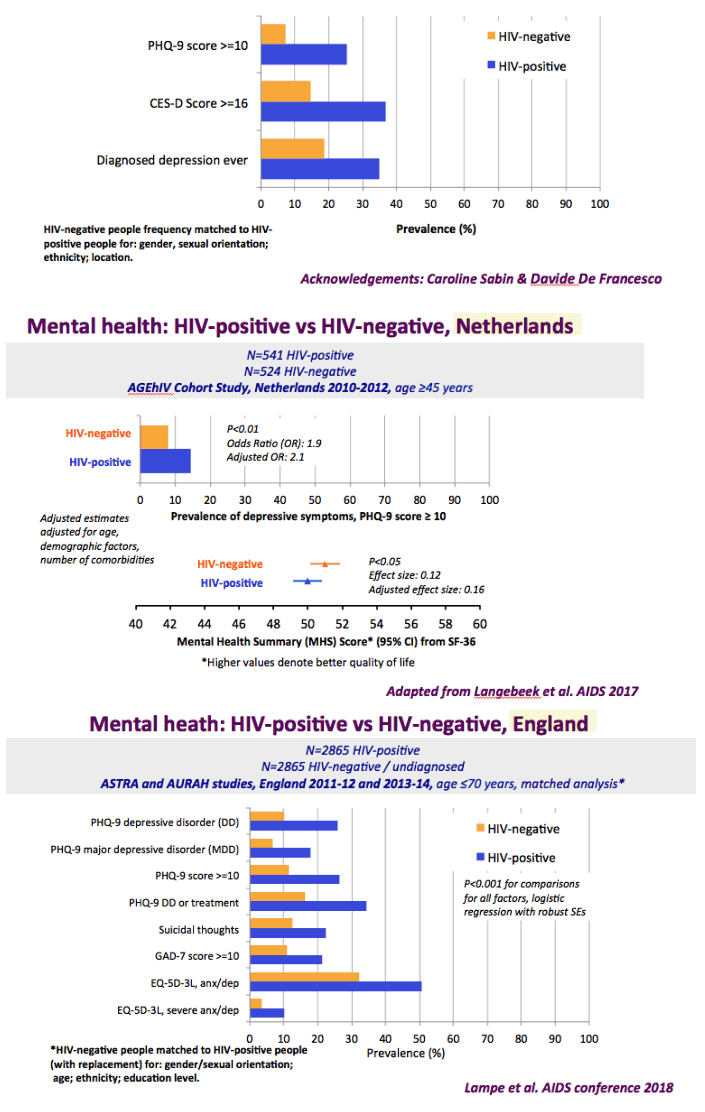
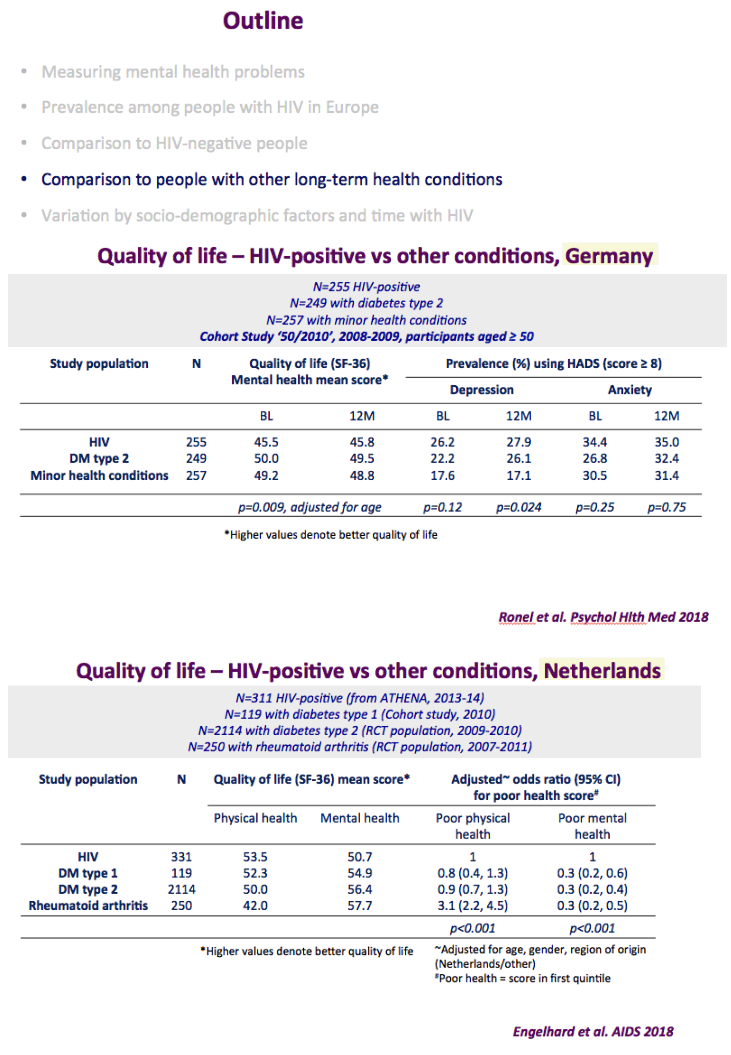
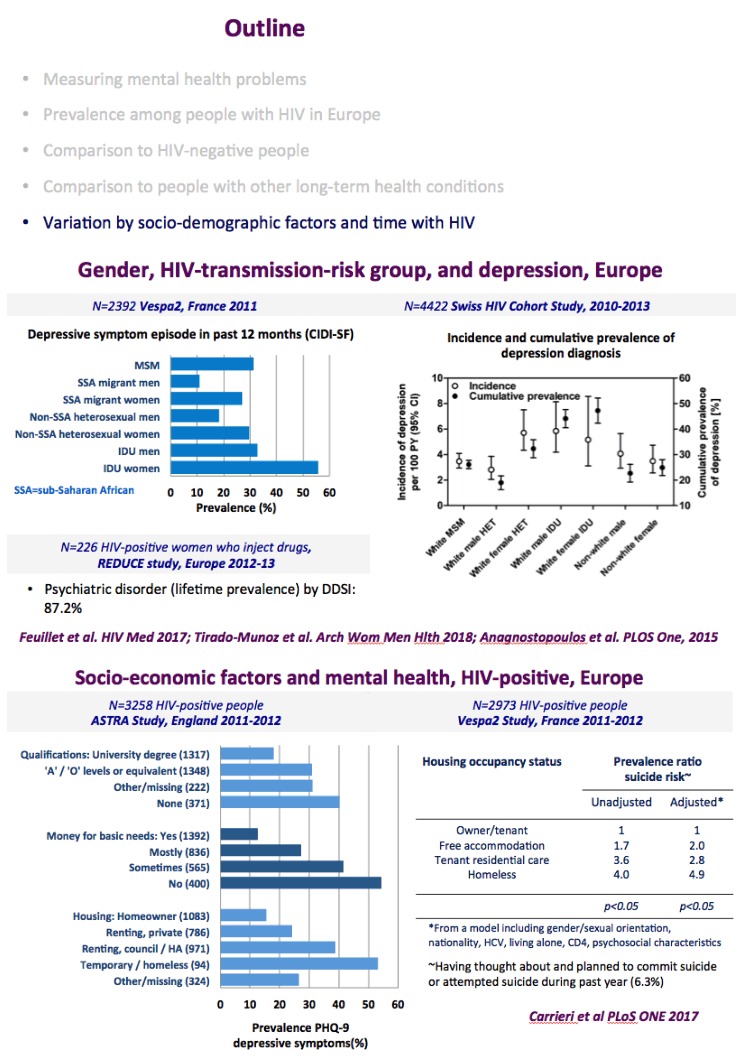
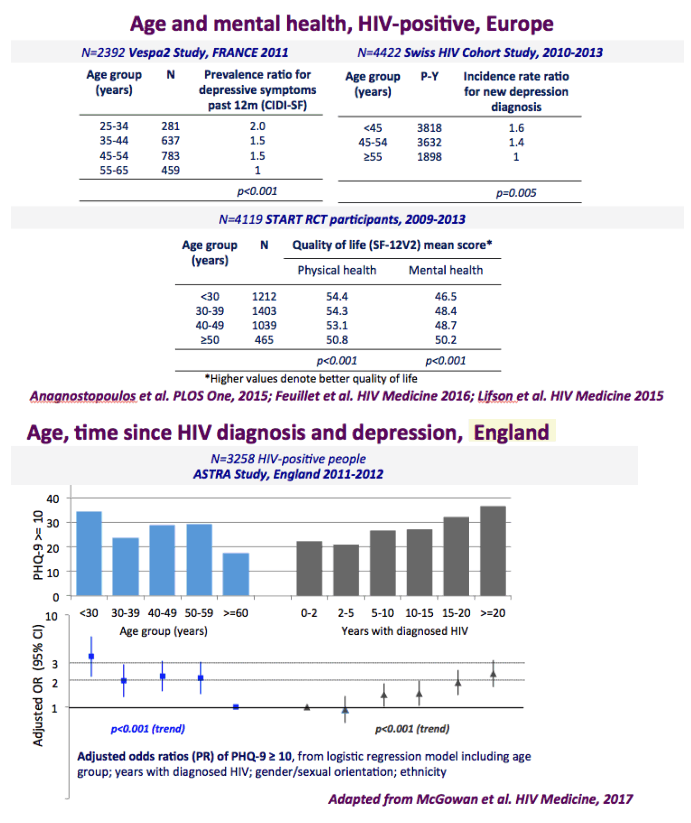
The graph just below shows depression rates by questionnaire among HIV+ at 20% to 50% and remember this is self-reported meaning many may have cognitive impairment & not realize it. Graph immediately below up to 35% have anxiety. 50% with HIV reported "moderate" or "severe" depression/anxiety compared to 25% in the 3rd graph just below. In graph just below: in the UK HIV+ 35% had "ever diagnosed" depression, 25% anxiety, 37% of HIV+ men had primary care recorded symptoms or diagnosis of mental health problem. In Albania 62% had depression and 82% anxiety. Graph lower down in this report from Denmark shows psychtropic drug use 3-6 times greater among HIV+ than the general population. A study below showed 19% reported depressed were treated & 45% remained untreated. But in the published literature these drugs can be associated with cognitive impairment which can increase risk for falls and fractures, and in the general population for those at greater risk who are elderly they recommend to consider NOT using these medications, not so in the HIV+ population, so they may be overused. From the POPPY Study mental health issues & depression are much greater among HIV+ than the general population, 2-3 times greater, up to 35% depression rates in HIV+. Comparing HIV+ to those with people who have other health conditions but not HIV this below you can see table quality of life was worse among HIV+ and depression was worse too compared to people who had diabetes or other minor conditions. In a separate presentation today at Glasgow Chloe Orkin, MD, of Royal London Hospital and chair of the British HIV Association (BHIVA), suggested that in addition to the well-known 90-90-90 AIDS targets, a new "90" needed to be added: 90% good health-related quality of life. "Often, we see the physical and psychological as distinct, but we need to be aware of people's mental health".... "As physicians, we need to become stigma-aware."..... "It's really important as healthcare professionals to be part of the solution rather than exacerbating the problem." The studies show below that often high rates depression & anxiety start after a person was diagnosed with HIV. The affect of stigma likely plays a big role in contributing to depression, as worsening stigma occurs with older age in HIV+ as self-stigma gets much worse along with suffering the consequences iof the affects of aging after 65 years old. Below is a slide depicting depression differences between patient groups and IDU women have high depression rates with slides saying 87% have a lifetime histrory of depression which is not very surprising but bear this in mind translating to the USA where so many HIV_ women & men too have an IDU history and how that will emerge in the aging older HIV+ population. In graph slide below: depression & suicide risk is much greater who have financial issues & is related to home ownership. Renters have higher suicide risk compared to homeowners. Finally duration of time with HIV is associated with greater depression rates - see slide below, there is a doubling of depression rates to 35% for those HIV+ for 20 years or more versus those infected with HIV for 0-2 years. here is study also at Glasgow, the first study to quantify the death rate will increase for every additional comorbidities an HIV+ person gets .Jules
GLASGOW: Multimorbidity and risk of death differs by gender in people living with HIV in the Netherlands - the ATHENA cohort study - (10/29/18)


|
| |
|
 |
 |
|
|