 |
 |
 |
| |
Successful HCV treatment does not affect rate of
heart disease or non-AIDS cancer
|
| |
| |
Conference on Retroviruses and Opportunistic Infections (CROI), March 4-7, 2019, Seattle
Mark Mascolini
Despite concern that "bad" LDL cholesterol rises after HCV cure, analysis of 18,736 people with HCV/HIV coinfection found no evidence linking HCV status or treatment to new (incident) cardiovascular disease [1]. Neither did this EuroSIDA study tie HCV status or treatment to development of non-AIDS cancers. But successful HCV therapy cut incidence of end-stage liver disease and liver cancer.
HCV cure with direct-acting antivirals (DAAs) brought many changes. Halting ongoing inflammation due to chronic HCV infection lowered rates of liver disease and offered the prospect of reining in inflammation-driven nonliver disease. At the same time, EuroSIDA investigators noted, HCV infection lowered LDL levels and HCV cure boosted LDL. At the 2018 CROI, a 237-person study in Spain determined that curing HCV in people with HIV inflated 10-year cardiovascular risk [2].
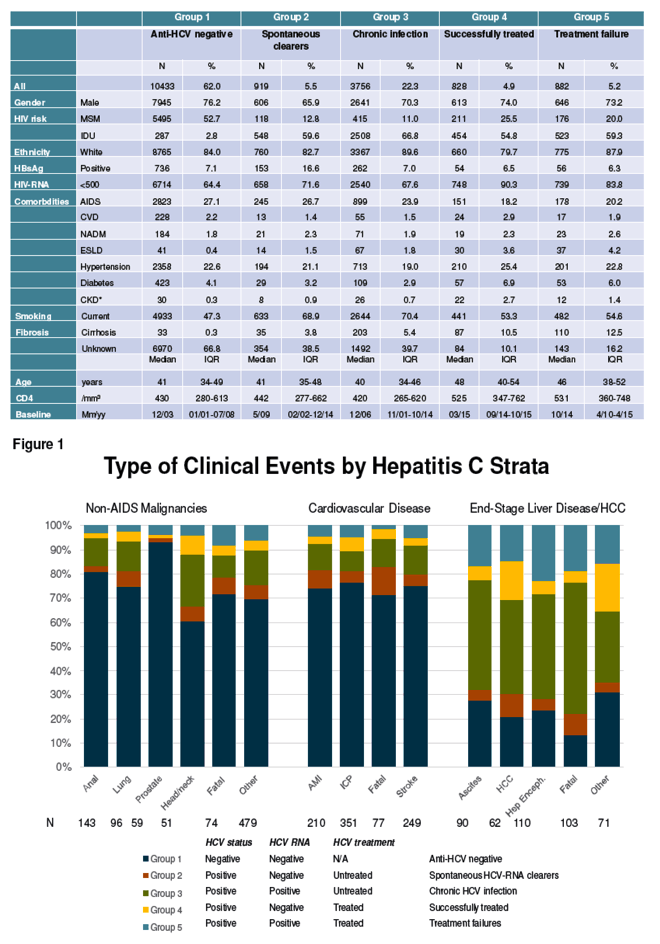
To determine whether this impact on cardiovascular risk has clinical consequences--and to chart the impact of HCV status and treatment on rates of non-AIDS cancer and liver disease--a EuroSIDA team divided cohort members into 5 groups: (1) anti-HCV negative people, (2) spontaneous clearers of HCV RNA, (3) people with untreated chronic HCV infection, (4) people successfully treated for HCV, and (5) HCV treatment failures. Then they tracked incidence of end-stage liver disease (including hepatocellular carcinoma), non-AIDS cancer (excluding hepatocellular carcinoma), and cardiovascular disease. They used Poisson regression to compare incidence of these endpoints in the 5 HCV groups.
Of the 18,736 cohort members with known HCV status, most (62%) were anti-HCV-negative, 6% spontaneous clearers, 22% chronically infected, 5% successfully treated, and 5% treatment failures. In the whole group, 74% were men, 85% were white, and 84% had ever taken antiretroviral therapy. Median age stood at 41 and median CD4 count at 438.
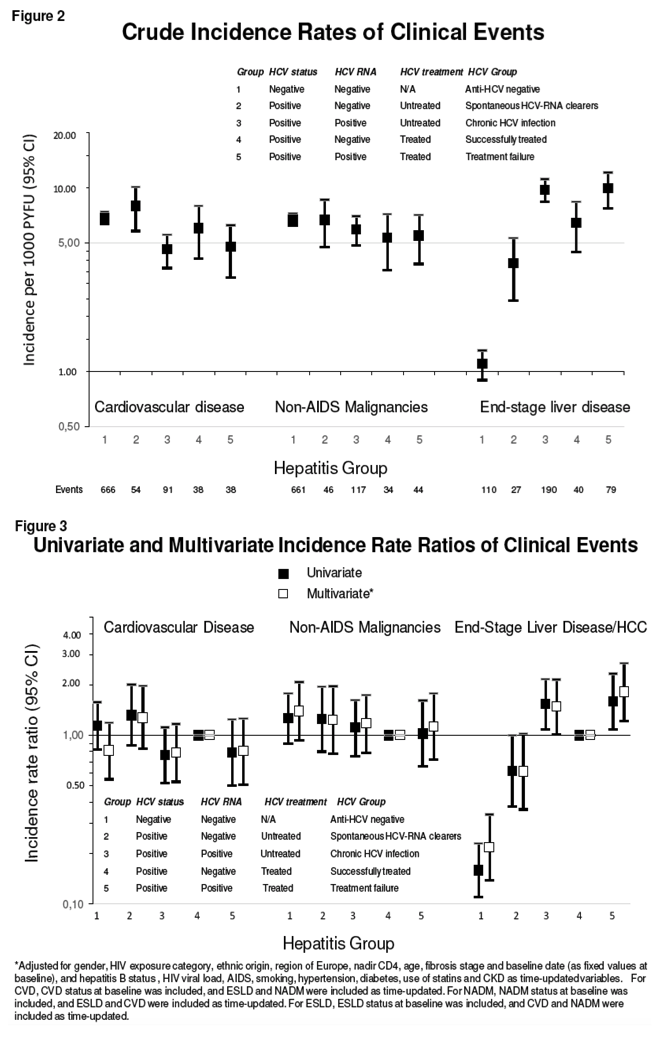
Through a median 8.3 years of follow-up, the researchers counted 887 new cardiovascular events, 902 new cases of non-AIDS cancer, and 436 new cases of end-stage liver disease. In adjusted analyses, compared with people successfully treated for HCV infection (Group 4), two groups had higher incidence of end-stage liver disease at the following adjusted incidence rate ratios (aIRR) and 95% confidence intervals (CI):
-- Group 3, chronic infection: aIRR 1.47, 95% CI 1.02 to 2.13, P = 0.041
-- Group 5, treatment failure: aIRR 1.80, 95% CI 1.22 to 2.66, P = 0.0033
Group 2, spontaneous clearers, had a marginally lower incidence of end-stage liver disease than successfully treated people (aIRR 0.61, 95% CI 0.36 to 1.02, P = 0.058).
EuroSIDA investigators found no statistically significantly differences between HCV groups in incidence of cardiovascular disease or non-AIDS cancers. Excluding people from Central East Europe and Eastern Europe, who tend to be younger, did not substantially change these findings. Separate analysis of myocardial infarctions or strokes alone did not differ across the 5 HCV groups. And incidence of the three overall conditions did not differ by age above versus below 50 across the 5 HCV groups.
A study of more than 60,000 US veterans with HCV but not HIV, reviewed separately by NATAP, tied DAA therapy to lower risk of incident cardiovascular disease at all fibrosis stages [3].
The EuroSIDA researchers concluded that they found "no evidence of any impact of HCV infection status or HCV treatment on incidence of both non-AIDS defining malignancies and cardiovascular disease in HIV coinfected persons." Higher incidence of end-stage liver disease and liver cancer in chronically HCV-infected people, they added, "underline[s] the importance of early and effective HCV treatment for reducing liver-related complications in HIV/HCV infected persons."
References
1. Peters L, Lundgren J, Rockstroh J, et al. Clinical outcomes in persons coinfected with HIV and HCV: impact of HCV treatment. Conference on Retroviruses and Opportunistic Infections (CROI). March 4-7, 2019. Seattle. Abstract 565.
2. Carrero A, Berenguer J, Hontanon V, Navarro J. Eradication of HCV: effects on cardiovascular risk and preclinical atherosclerosis. Conference on Retroviruses and Opportunistic Infections (CROI). March 2018. Boston. Abstract 631. http://www.croiconference.org/sessions/eradication-hcv-effects-cardiovascular-risk-and-preclinical-atherosclerosis
3. Butt AA, Yan P, Aslam S, et al. Effect of liver fibrosis stage and DAA treatment on risk of CVD events in ERCHIVES. Conference on Retroviruses and Opportunistic Infections (CROI). March 4-7, 2019. Seattle. Abstract 570.
------------------------------
Clinical Outcomes in Persons Coinfected with HIV and HCV: Impact of HCV Treatment
L Peters1, J Lundgren1, J Rockstroh2, J Gerstoft3, LD Rasmussen4, S Bhagani5, I Aho6, C Pradier7, J Bogner8, C Mussini9, A Castagna10, F Maltez11, M Laguno12, G Wandeler13, K Falconer14, T Trofimora15, E Borodulina16, D Jevtovic17, E Bakowska18, K Kase19, G Kyselyova20, A Mocroft21 on behalf of the EuroSIDA Study
1CHIP, Rigshospitalet, Copenhagen, Denmark. 2University of Bonn, Bonn, Germany. 3Rigshospitalet, Copenhagen, Denmark. 4Odense University Hospital, Odense, Denmark. 5Royal Free Hospital, London, UK. 6Helsinki University Hospital, Helsinki, Finland. 7Centre Hospitalier Universitaire de Nice, Nice, France.8Ludwig Maximilians University of
Munich, Munich, Germany. 9University of Modena and Reggio Emilia, Modena, Italy. 10San Raffaele Scientific Institute, Milano, Italy. 11Hospital de Curry Cabral, Lisbon, Portugal. 12Hospital Clinic, Barcelona, Spain. 13Bern University Hospital, Bern, Switzerland. 14Karolinska University Hospital, Stockholm, Sweden. 15Novgorod Centre for AIDS prevention and control, Novgorod the Great, Russia. 16Samara State Medical University, Samara, Russia. 17Infectious & Tropical Diseases Hospital, Belgrade, Serbia. 18Wojewodzki Szpital Zakazny, Warsaw, Poland. 19West-Tallin Central Hospital, Tallinn, Estonia. 20Crimean Republican AIDS centre, Simferopol. 21UCL, London, UK

Abstract Body:
Previous studies have found changes in lipids and inflammatory biomarkers after HCV cure, but there is little data on clinical endpoints in HIV/HCV coinfected persons. We investigated the impact of HCV coinfection status and clearance of HCV-RNA following treatment on the risk of non-AIDS malignancies (NADM), cardiovascular disease (CVD) and end-stage liver disease (ESLD) in HIV/HCV infected persons in the EuroSIDA study.
All HIV positive persons with known HCV status after January 2001 were included and stratified into five groups based on time-updated HCV-RNA and use of HCV treatment: 1) HCV-uninfected, 2) spontaneously resolved HCV infection, 3) Chronic untreated HCV infection, 4) Successfully treated HCV infection, 5) HCV-RNA positive despite previous HCV treatment. Separate analyses were performed with each clinical event (fatal and non-fatal) ESLD (including hepatocellular carcinoma, HCC), NADM (excluding HCC) and CVD (myocardial infarction, stroke, angioplasty, coronary bypass, carotid endarterectomy). Poisson regression was used to compare incidence rates between HCV groups.
A total of 15,524 HIV positive persons were included. The majority were male (74%), White (87%), on cART (85%) and current smokers (55%) with a median (IQR) age of 41 (35-49) years and CD4 cell count of 446 (290-641) cells/µl. During a median of 6.6 (IQR 2.3–12.6) person years of follow up (PYFU), a total of 694 CVD, 710 NADM and 375 ESLD events occurred; crude incidence rates/1000 PYFU (95% CI) were 6.1 (5.7–6.6) for CVD, 6.2 (5.8–6.7) for NADM and 3.2 (2.9–3.6) for ESLD. In univariable and multivariable analysis, there were no differences in incidence of both NADM and CVD between those who were untreated, had cleared HCV-RNA after HCV treatment and those with chronic infection (figure). In contrast, the incidence of ESLD was significantly lower among persons who had cleared HCV-RNA after treatment compared to those with chronic infection, and similar to those with spontaneous HCV-RNA clearance.
Although HCV cure has been shown to perturb levels of lipid and inflammatory biomarkers, studies of HIV/HCV coinfected persons have lacked power to focus on clinical events. We found no evidence of any impact of HCV infection status or HCV treatment on incidence of both NADM and CVD in coinfected persons while successful HCV treatment significantly lowered the incidence of ESLD to what was observed for those with spontaneous HCV-RNA clearance.



|
| |
|
 |
 |
|
|